US Pharm. 2012;37(5):39-42.
With over 2 million occurrences in the United States every year, ocular trauma is a prevalent condition managed by health care providers, including pharmacists.1 The pain associated with ocular trauma can be particularly debilitating. As a result, it is common for patients to consult pharmacists about OTC or home remedies in an attempt to self-medicate before they are able or willing to seek further medical attention from a physician or eye care specialist. Pharmacists play a key role in helping patients quickly and effectively manage their pain while avoiding adverse effects. They routinely answer questions about the use of ophthalmic pain medications, so it is important to be aware of the practitioner’s rationale behind prescribing them.
Patients who have experienced trauma may not be completely aware of the severity of the situation or the full extent of the damage. Conditions that seem rather benign can be sight threatening. It is always important to ask questions regarding the origin of the injury in order to determine the urgency of the situation and give appropriate recommendations regarding pain management. A knowledgeable pharmacist can recognize serious conditions that require immediate medical attention and ensure that the patient receives the eye care necessary to preserve his or her sight.
Types of Ocular Trauma
Pain management and treatment options usually depend on the underlying condition. The most common ocular trauma is a superficial injury to the anterior portion of the eye, such as a corneal abrasion (FIGURE 1) or conjunctival laceration.1 Not only are these injuries extremely painful, but they may not heal without intervention. An infection may ensue if not treated promptly. Therefore, it is important to refer the patient to a physician or eye care specialist in a timely fashion. Until the patient can get medical attention, nonpreserved artificial tears, gels, and ointments assist in hydrating and lubricating the eye. They also provide comfort by cushioning sensitive nerves that have been damaged. Eye patches known as pressure patches immobilize the eyelid and relieve pain caused by mechanical irritation of the eyelid when the patient blinks. Pressure patches can be used on a temporary basis for patients with corneal abrasions. However, patches must be used cautiously because they can be associated with infection and delayed healing. They should never be used in patients with contact lens–related abrasions, penetrating injuries, corneal ulcers, or chemical burns.2 Pressure patches are not used as often due to the emergence of more effective options such as bandage contact lenses, which are discussed in detail below.
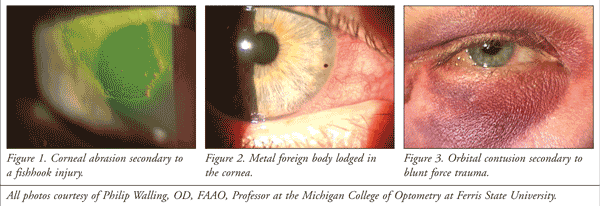
Foreign bodies, usually lodged in the cornea or conjunctiva, are the second most prevalent ophthalmic injury (FIGURE 2).1 Sterile eyewash or irrigating solution relieves pain in the sense that it assists in removing debris or particles in and around the eye. Foreign bodies can penetrate the eye and result in serious complications. An open globe injury, or ruptured globe, is considered an emergency. If a patient has a foreign body, be sure to determine the circumstances surrounding the incident. If a penetrating injury resulting in a ruptured globe is suspected, a protective shield should be placed over the eye, and the patient should be treated immediately. Because many chemicals have the ability to deeply penetrate ocular tissues, chemical injuries are extremely sight threatening. Advise the patient to immediately begin flushing the eye with saline solution and seek eye care right away.3
Contusions to the eye and areas surrounding it are usually a result of blunt force trauma (FIGURE 3). Blunt force trauma to the eye can be particularly harmful because the traumatic forces disrupt the eye’s normal anatomical structure. Thus, patients are at risk of damage to the bones surrounding the eye and the structures located in the back of the eye. Patients are also at risk of conditions such as orbital blowout fractures, retinal detachments, or vitreoretinal hemorrhages.4 Ask the patient about symptoms of vision loss, double vision, flashes of light, or floaters. These symptoms indicate the need for prompt medical attention. Until then, cold ice packs and acetaminophen will quell periorbital inflammation and reduce pain. It is advisable to refrain from nonsteroidal anti-inflammatory drugs (NSAIDs) or aspirin in the event that the patient has an internal hemorrhage.3
Pharmacologic Treatment Options
Once the patient receives eye care, there are various prescription medications available for the management of ocular pain and discomfort. TABLE 1 lists acute and long-term treatment strategies for the most common injuries. Because ocular pain is frequently caused by an acute condition related to the anterior structures of the eye, topical therapeutics play an important role in the management of pain. They are a noninvasive, easily administered method of drug delivery. Topical agents target the anterior structures of the eye with minimal systemic absorption. They are frequently prescribed in conjunction with oral peripheral-acting agents such as acetaminophen or centrally-acting opioid analgesics such as hydrocodone.5

A major source of pain from ocular trauma is inflammation. Inflammatory mediators, particularly prostaglandins, play an important role in lowering the pain threshold and regulating the eye’s inflammatory response. The level of pain perceived by the central nervous system is intensified by chemical mediators such as substance P, bradykinin, and histamine.5 The ocular inflammatory response results in blood vessel dilation, increased blood flow, blood plasma leakage, and a breakdown of the blood-ocular barrier. This often enhances photophobia and gives the eye a red and swollen appearance. Pupillary miosis, discharge, and a decreased palpebral aperture often accompany inflammation and pain.6 Ocular trauma is frequently associated with anterior uveitis. This condition results in inflammation of the iris and ciliary body as well as the release of protein and white blood cells into the anterior chamber. Patients with anterior uveitis commonly experience a deep, aching pain and extreme light sensitivity associated with ciliary body and iris muscle spasms.7
Topical Ophthalmic NSAIDs: Ophthalmic NSAIDs block the cyclooxygenase pathway and inhibit the formation of inflammatory mediators that inevitably cause pain. They are routinely used to ameliorate pain and inflammation after cataract surgeries and corneal refractive surgeries such as LASIK (laser-assisted in situ keratomileusis). Although this is an off-label use of the medication, the analgesic properties of NSAIDs have been utilized to effectively manage pain and discomfort due to ocular surface trauma. They have been found to be particularly helpful for alleviating pain secondary to corneal abrasions. A study by Weaver and Terrell revealed that patients prescribed topical NSAIDs for corneal abrasions spend less time away from work and require fewer oral analgesics to manage their pain. The medication was generally prescribed four times a day for 1 to 5 days or until the cornea reepithelialized.8
The two most recently released topical ophthalmic NSAIDs are Bromday (bromfenac 0.09%) and Nevanac (nepafenac 0.1%). To date, Bromday is the only medication of its kind approved for once-daily dosing.9 The decreased dosing regimen aids in patient compliance in administering the medication as directed. Nevanac is the first prodrug in its class. Typically prescribed three times per day, it is said to reach higher intraocular concentrations when nepafenac hydrolyzes into amfenac in the anterior chamber of the eye.5 Another recent addition, Acuvail (ketorolac 0.45%), is unique in that it is supplied in a unit-dose preservative-free formula.9 This can be very helpful for patients with corneal injuries or for patients with known hypersensitivities to the preservatives in most topically applied ophthalmic medications.
Topical NSAIDs are relatively safe, with few local or systemic side effects. Stinging upon instillation as well as transient conjunctival hyperemia is not uncommon. Caution should be used when topical NSAIDs are used in conjunction with prostaglandin analogues for intraocular pressure (IOP) reduction, as this usage may lead to a subsequent rise in IOP.5 The development of corneal stromal ulcers, also known as corneal melting, was associated with generic diclofenac 0.1% ophthalmic solution in a small number of patients. Investigators suspect that the corneal melting was due to the solubilizer/preservative used in that particular formulation. It has since been withdrawn from the marketplace.10
Ophthalmic Corticosteroids: Ophthalmic corticosteroids are more effective than ophthalmic NSAIDs at suppressing inflammatory mediators that cause pain, especially when the patient exhibits uveitis. By reducing inflammation, corticosteroids can hasten the eye’s healing response and prevent tissue scarring. This is important in cases where corneal scarring can result in permanent vision loss. Corticosteroids are also available in combination with antibiotics to treat bacterial infections and/or to provide additional coverage against opportunistic pathogens.9
Corticosteroids must be prescribed with caution because they have significant side effects including cataracts, increased susceptibility to infections, and delayed healing due to their effect on collagen synthesis.5,11 Because they severely exacerbate the condition, corticosteroids should be completely avoided in patients with herpes simplex keratitis. As many as 30% of patients will experience a marked increase in intraocular pressure when using a corticosteroid.7 Therefore, patients taking topical corticosteroids should be monitored frequently, and these agents should be used conservatively in patients with ocular hypertension and glaucoma. Corticosteroids are generally not intended for the long-term treatment of chronic ocular conditions.5 Doses are ordinarily tapered to prevent an inflammatory relapse.5,7
Alrex (loteprednol etabonate 0.2%) and Lotemax (lotepred-nol etabonate 0.5%) are “soft steroids” designed with a decreased propensity for some of the harmful side effects related to ophthalmic corticosteroid use. The likelihood of toxicity is reduced because the chemical structure of the drug transforms into an inactive metabolite after it has exerted its pharmacologic effects. One particular benefit of soft steroids is the diminished probability of both IOP increases and cataract formation. These agents are frequently prescribed for the patient using corticosteroids on a long-term basis or if the patient has experienced a marked increase in IOP while using a traditional ophthalmic corticosteroid.5,11
Cholinergic Antagonists (Cycloplegics): Patients who have ocular trauma experience a deep, aching pain and severe photophobia from ciliary body and iris muscle inflammation. Cholinergic antagonists such as atropine sulfate 1% or homatropine hydrobromide 1% inhibit muscarinic receptors located in the iris sphincter and ciliary body. As a result, cycloplegics both dilate the pupil and prevent the eye’s ability to focus on near objects for 1 to 12 days. By fixing the pupil and rendering the involved muscles inactive, cycloplegics provide a substantial amount of pain relief.5,7 Cycloplegics are also beneficial because they inhibit the leakage of additional inflammatory proteins by stabilizing the blood-aqueous barrier. Additionally, they prevent the formation of harmful adhesions between the iris and the lens or cornea.7
Because its effect can last up to 12 days, atropine sulfate 1% is usually reserved for severe cases when a long-lasting, constant cycloplegic effect is needed. Intermediate-acting agents such as homatropine hydrobromide 1% are preferred in a majority of cases. Short-acting agents, such as cyclopentolate hydrochloride 1%, have a much weaker and shorter cycloplegic effect. They are usually reserved only for patients with very mild levels of uveitis.7,12
Cholinergic antagonists have known ocular and systemic side effects and should be used judiciously in certain patient populations. Ocular effects include conjunctival hyperemia, allergic blepharoconjunctivitis, and increased lacrimation. Cycloplegics have been known to raise IOP in patients with open-angle glaucoma. They can cause acute angle-closure glaucoma in patients predisposed to the condition. Known systemic side effects include diffuse cutaneous flushing, decreased salivation and sweating, convulsions, seizures, and psychotropic responses. Because of the increased risk of toxicity and central nervous system disturbances, cholinergic antagonists should be used cautiously in young children, elderly individuals, those with spastic paralysis or brain damage, and patients with motor or mental retardation.5
Topical Anesthetics: The cornea, conjunctiva, sclera, and iris are all highly innervated with extremely sensitive nerve endings from the ophthalmic division of the trigeminal nerve.6,13 When patients have superficial injuries to the surface of their eye, they feel severe pain caused by the shear forces of the eyelids as they blink. This situation is particularly common in corneal abrasions, lacerations, and foreign bodies. Topical anesthetics temporarily alleviate the pain for 5 to 20 minutes by effectively blocking peripheral nerve conduction and inhibiting the excitation of pain-sensitive nerve endings. They are used during an examination to aid in the visualization of ocular structures, measure IOP, or remove a foreign body.5 Because anesthetics are so effective at eliminating pain, albeit for a very short duration, patients often ask for a prescription. The off-label use of topical anesthetics in this manner is contraindicated because of serious complications such as delayed wound healing, keratitis, corneal ulceration, and vision loss.5
Contact Lenses: A viable pain management strategy is the therapeutic use of silicone hydrogel, or bandage, contact lenses. Bandage contact lenses cushion exposed corneal nerves and are extremely effective at managing pain from corneal abrasions or lacerations or after the removal of a foreign body. They protect the cornea from mechanical irritation and facilitate wound healing. The use of topical medications (antibiotics or NSAIDs) over a contact lens can be helpful in the management of pain and the treatment of the condition. Because contact lenses are absorptive in nature, they have been known to prolong the length of time that the ocular surface is exposed to the medication. This not only exposes the eye to higher drug concentrations but also increases permeation and absorption.14
Bandage contact lenses must always be fitted and frequently evaluated by an eye care practitioner. The primary risk involved with prescribing bandage contact lenses is the possibility of a bacterial infection. Topical antibiotics are regularly prescribed in conjunction with bandage contact lens use. Patients should be monitored for complications such as corneal toxicity secondary to preservatives in topical medications.14 Pharmacists can advise patients wearing bandage contact lenses to be cognizant of the signs of such complications. This includes increased discharge, redness, swelling, pain, or decreased vision. If such signs occur, the patient should contact an eye care practitioner immediately.14

Conclusion
Ocular trauma is a common occurrence associated with a significant amount of pain. In an attempt to alleviate the pain quickly, pharmacists are often the first health care professional that patients consult. It is always important to ask detailed questions about the origin of the injury so as to determine the urgency of the situation and provide the proper instructions regarding pain management. Depending on the situation, certain OTC products may be helpful in controlling pain on a short-term basis. Ultimately, it is important to receive medical attention from an eye care professional even if the injury seems benign.
Topical ophthalmic medications are used in conjunction with peripheral- and centrally-acting oral analgesics for the management of pain. Corticosteroids, NSAIDs, and cycloplegics are helpful in reducing pain secondary to inflammation. Nonpreserved artificial tears, gels, ointments, and bandage contact lenses cushion exposed nerve endings and prevent pain secondary to the mechanical forces of the eyelids. It is useful to understand the rationale behind the use of ophthalmic pain medications because pharmacists play a key role in counseling the patients who use them.
The authors would like to acknowledge H. Stephen Lee, PharmD, Associate Professor at Ferris State University College of Pharmacy, for his professional guidance and support.
REFERENCES
1. McGwin G, Hall TA, Xie A, Owsley C. Trends in eye injury in the United States, 1992-2001. Invest Ophthalmol Vis Sci. 2006;47(2):521-527.
2. Sage NL, Verrault R, Rochette L. Efficacy of patching for traumatic corneal abrasions: a controlled clinical trial. Ann Emerg Med. 2001;38(2):129-134.
3. Kunimoto DY, Kunal DK, Makar MS. The Wills Eye Manual. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004.
4. Kiel J, Chen S. Contusion injuries and their ocular effects. Clin Exp Optom. 2001;84(1):19-25.
5. Bartlett J, Jaanus S. Clinical Ocular Pharmacology. 5th ed. Oxford, UK: Butterworth-Heinemann; 2008.
6. Belmonte C, Garcia-Hirschfeld J, Gallar J. Neurobiology of ocular pain. Prog Retin Eye Res. 1997;16(1):117-156.
7. Skorin L, Lea A. Addressing anterior uveitis. Optom Manage. 2002;37(11):36-41.
8. Weaver CS, Terrell KM. Update: do ophthalmic
nonsteroidal anti-inflammatory drugs reduce the pain associated with
simple corneal abrasion without delaying healing? Ann Emerg Med. 2003;41(1):134-140.
9. Melton R, Thomas R. Clinical guide to ophthalmic drugs. Rev Optom. 2011;148(suppl 5):1A-47A.
10. Abelson MB, Lilyestrom L. Melting away the myths of NSAIDs. Rev Ophthalmol. 2007;14(11):124-128.
11. Pavesio C, DeCory H. Treatment of ocular inflammatory conditions with loteprednol etabonate. Br J Ophthalmol. 2008;92(4):455-459.
12. Dodds E. Treatment strategies in patients with anterior uveitis. Ann Emerg Med. 2003;41(1):55-68.
13. Remington L. Clinical Anatomy of the Visual System. Boston, MA: Butterworth-Heinemann; 1998.
14. Veys J, Meyler J, Davies I. Essential contact lens practice: contact lenses for therapeutic use. Optician. 2001;235(6137):28-37.
15. Flach AJ. The importance of eyelid closure and
nasolacrimal occlusion following the ocular instillation of topical
glaucoma medications, and the need for the universal inclusion of one of
these techniques in all patient treatments and clinical studies. Trans Am Ophthalmol Soc. 2008;106:138-148.
To comment on this article, contact rdavidson@uspharmacist.com.






