US Pharm. 2009;34(7):14-19.
Sunlight has been thought to be beneficial in recent decades, a time in which widespread tanning has become the norm. However, some patients’ quest for the perfect tan may lead them to permanent disfigurement and early death due to the damaging effects of ultraviolet (UV) radiation.
Ultraviolet Radiation
Sunlight consists of 45% UV radiation, 5% visible radiation, and 50% infrared radiation. The UV region (100-400 nm) is further divided based on wavelengths into long wave UVA (315-400 nm), medium wave UVB (280-315 nm) and short wave UVC (100-280 nm). The ozone layer absorbs all of the UVC and 95% of the UVB. However, the UVA is not absorbed and thus constitutes more than 95% of the solar radiation that reaches us.1-3
Benefits of UV Radiation
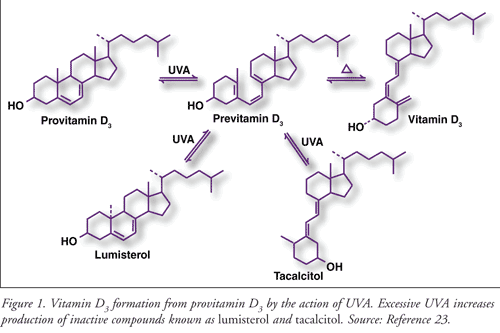
UV radiation has a few beneficial health effects, most notably being integral in the formation of vitamin D. Upon exposure to UVA radiation (290-300 nm), provitamin D3 (7-dehydrocholesterol) is converted rapidly to previtamin D3.4 Previtamin D3 undergoes slow thermal conversion to vitamin D3, as well as the biologically inactive compounds lumisterol and tacalcitol (FIGURE 1). A brief 10-minute exposure of uncovered hands and face is all that is needed to ensure adequate supplies of vitamin D3.5 It is uncommon for patients to experience inadequate photoconversion to vitamin D3. Those most at risk are patients residing in northern latitudes during winter, patients with more highly pigmented skin, or elderly people who routinely use clothing or sunscreens to reduce their sun exposure.
Excessive UV Radiation
Excessive UV exposure increases production of the inactive compounds lumisterol and tacalcitol, which can be converted back to previtamin D3. Vitamin D2 (ergocalciferol) is also formed in a similar fashion from provitamin D2 (ergosterol). Excessive UV exposure provides no added benefit in forming additional vitamin D. However, it results in profound and permanent damage to underlying skin through two mechanisms.
UV radiation is directly absorbed by cellular chromophores, causing damaging chemical reactions. UV also causes photosensitization. In these cases, UV is absorbed by endogenous or exogenous sensitizers that become electrically excited; the resultant reactions form reactive oxygen species (ROS). ROS produce oxidative damage to DNA, proteins, fatty acids, and saccharides, leading to disrupted cell metabolism, morphological and structural changes in cells, attacks upon regulation pathways, and alterations in the differentiation, proliferation, and apoptosis of skin cells. These processes initially lead to sunburn, wherein the skin is red, painful, and hot to the touch. Sunburn usually appears within a few hours after sun exposure and may take from several days to several weeks to fade. Excessive exposure to UV radiation also increases the risk of photoaging, solar elastosis, actinic keratoses, basal and squamous cell carcinomas, and melanoma.1-3,6
Photoaging
Photoaging, also known as dermatoheliosis, is a set of UV-induced, disfiguring changes in the uppermost layer of skin, the epidermis.7-9 Unfortunately, these changes are not apparent until several decades of excessive exposure have occurred, causing a false sense of security in chronic tanners. The degree of photoaging one experiences is partly determined by the underlying skin color. Those most prone to suffer are light-skinned white patients, while those most protected are dark-skinned patients.7,10
The epidermal changes of photoaging include wrinkles, coarseness, scaling, looseness, dryness, bruising, and telangiectasias (visible veins).7,10-13 Various areas of mottled hyperpigmentation appear, referred to in lay terms as age spots, liver spots, and medically as solar lentigines.7 Sun-exposed areas may also exhibit hypopigmentation (i.e., small, white, scarlike lesions). Many patients deny strenuously that these aging skin changes are due to irresponsible sun exposure in youth. To counter this argument and educate patients, physicians suggest asking them to compare the skin of their arms and face to the skin of their buttocks.7 All areas of the patients’ skin are identically aged chronologically. The damage to the exposed areas reflects the additive exogenous factors that damaged skin beyond its normal intrinsically aged appearance. Thus, the exposed areas would have been as smooth and undamaged as the buttocks if the patient had exercised restraint in sun exposure and/or tanning.
Solar Elastosis
Solar elastosis is another form of dermatoheliosis, and is the term used for sun damage in the dermal layer of skin underlying the epidermis. Dermal tissues are composed mainly of elastic fibers and collagen fibers. Elastic fibers give skin elasticity while collagen fibers give it strength.14 Excessive sun exposure causes elastic fibers to mutate into a thick mass of tangled fibers that lose elasticity and cause the dermis to thicken abnormally.14 Collagen fibers degenerate and dermal strength is compromised. The net effect of these changes is development of deep wrinkles and furrows on the face and exposed areas, yellowish discolorations of the forehead and back of the neck, and general sagging and drooping of areas that do not have strong underlying bony support (dermatochalasis).7,15 Thus, the upper arms sag loosely, the skin beneath and behind the chin forms “chicken neck,” the lower lip droops, and the ear lobes lengthen.13
Actinic Keratoses
Actinic (solar) keratoses are potentially premalignant sun-induced lesions usually found on sun-exposed areas.7,16 They are more common as patients age, appearing as pink-red, dry, scaly lesions that average 1 to 3 mm in diameter. Experts estimate that 1% to 16% of actinic keratoses eventually become squamous cell carcinoma.7 They occur most often in patients with fair skin who have a history of chronic sun exposure, such as those in outdoor occupations.
Basal and Squamous Cell Carcinomas
DNA damage caused by sun exposure is well established as being causally responsible for basal and squamous cell carcinomas.7,17-19 Persons at highest risk are those with mothers of Celtic, Scandinavian, or English origin; patients with blue or hazel eyes, red or blond hair, light skin, or freckles; and those who are not able to tan.7
Melanoma
Melanoma incidence is steadily increasing.7,20 A history of blistering sunburns in youth greatly increases risk, leading pharmacists to recommend taking sun precautions at all times. Those at greatest risk are the same as ones at risk for basal and squamous cell carcinomas. Patients should be taught to constantly scan their bodies for lesions that change in size, color, symptoms, or any other relevant parameter.7
Sun Protection
One of the most productive public health education topics the pharmacist can engage in is proper instruction about sun protection. This encompasses teaching patients about skin types, sunscreens, and other sun avoidance strategies.
Patients may be taught the concept of skin types, in order to help them assess their own risk for serious problems due to the sun. The lighter the skin, the greater the bearer’s propensity to develop serious problems from UV radiation. Lighter skin types also need sunscreens with a higher sun protection factor (SPF).7
The foremost method used by people to protect themselves from the sun remains sunscreens. However, to gain maximal protection, it is imperative to use these products correctly.7 First, patients should choose the highest SPF sunscreen that they can locate (e.g., SPF30+). Second, patients must apply sunscreen 30 minutes before entering the sun. This allows body heat to warm the product so that it will spread well to cover all parts of the skin surface before the UV radiation can damage the skin. The patient should then reapply the sunscreen just before entering the sun to ensure that any missed section is covered.
Patients should use an adequate amount of sunscreen. This is approximately 1 oz. for an adult application (e.g., 2.5-5.0 mL for the face and neck, 5.0-7.5 mL for the arms and shoulders, 5.0-7.5 mL for the torso, and 10-12.5 mL for the legs and tops of the feet). They should apply it with the fingertips rather than the palms to obtain better coverage. Sunscreen should be reapplied frequently while outdoors to replace whatever amount was accidentally toweled away, washed off, or sweated from the body. Patients should choose a product labeled “very water resistant” to help ensure that it will remain on the body during the calculated exposure time. It is also important to remember the lips. Numerous lip balms are available with sunscreens in the formulation.
Pharmacists may also teach patients to cover themselves as much as possible when in the sun. They may point out the advantages of purchasing special sun-protective articles of clothing that are rated with SPF 30+ protection, such as the Solumbra line from Sun Precautions.21

Proposed FDA Sunscreen Labeling
In August 2007, the FDA announced its intent to upgrade sunscreen labeling.22 The agency’s purpose is to provide enhanced warning about UVA radiation. If the proposal becomes a final rule, manufacturers would be required to use a star system to give consumers an easy method to determine the degree of UVA protection. A product would carry only one star if it conferred low UVA protection, two stars for medium protection, three stars for high protection, and four stars to denote the highest UVA protection available in a nonprescription sunscreen. A product not rating at least one star would prominently display a label stating it provides no UVA protection.
The FDA also proposed adding a label advising consumers that sunscreen is only one option available to them, and that limiting time in the sun and wearing protective clothing would also be critical. Finally, the FDA proposed allowing manufacturers to go beyond the SPF limit of 30+ to allow products to advertise protection at SPF 50+ (although there are already some products on the market labeled beyond this).

Among U.S. citizens there is the widespread belief that prolonged exposure to the sun is healthy, and that tanning is a good way to improve health and attractiveness. Unfortunately, this belief is wrong and may lead to epidemics of skin damage, premature aging, and various skin cancers.
What Does the Sun Do?
Being in the sun and tanning booth exposes you to ultraviolet (UV) radiation. UV radiation causes less serious problems, such as skin changes that make you look older than your years and also drooping or sagging of parts of the body such as the chin, upper arm, and lip. The sun also causes such serious problems as solar keratoses, squamous and basal cell cancers, and melanoma. These can cause skin disfigurement if they need to be removed, and can also spread to other areas if not caught early enough, causing a needless and early death.
The Myths of Tanning
America’s tanning craze will cause a skin cancer epidemic in a few years. To avoid this, people must stop using tanning booths. One myth is that tanning makes one more desirable. The reality is that while you may look good for a little while, in later years you may be scarred from wrinkles and numerous cancer surgeries. Another myth is that tanning booths only give you a “healthy” tan. However, there is no such thing as a healthy tan. Every tan is damaging, and tanned skin is skin that will eventually look far worse than it should. You must avoid tanning salons and any situation where you have unprotected exposure to the sun for more than a few minutes.
Using Sunscreens
You should use sunscreen or sunblock at every opportunity when you anticipate sun exposure for more than a few minutes. Some people are confused about how to choose sunscreens. You should first have an idea of how long you can stay in the sun before developing a slight redness. This is your minimal erythema dose (MED). Perhaps your MED is 10 minutes. Sunscreens and sunblocks have a number on the bottle called the SPF or sun protection factor. This number, through a simple multiplication, gives you a way to figure how long you can stay in the sun if you use that product. For example, if your MED is 10 minutes, using a product with SPF 6 allows you to stay out six times longer, for a total of 60 minutes to get only slight redness. If you wish to stay out longer, choose a product with a higher SPF and multiply by your 10-minute MED. If you stay out beyond the sunscreen protection time, you will burn and thus increase your risk of skin cancers and possibly other deadly problems. In general, individuals with fair skin burn more easily and should use a sunscreen with SPF 30+.
Sun Avoidance
There are other strategies to avoid the sun, such as staying inside during the peak burn time of 10 am to 4 pm. Cloudy days do not protect you, as UV rays penetrate clouds. Wear long sleeves, long pants, and a hat with a brim that is several inches wide all around. Sunless tanning products (self-tanners) that contain dihydroxyacetone (DHA) are FDA approved and provide an alternative to suntanning without risking UV exposure.
Remember, if you have questions, Consult Your Pharmacist.
REFERENCES
1. Hussein MR. Ultraviolet radiation and skin cancer: molecular mechanisms. J Cutan Pathol. 2005;32:191-205.
2. Clydesdale GJ, Dandie GW, Muller HK. Ultraviolet light induced injury: immunological and inflammatory effects. Immunol Cell Biol. 2001;79:547-568.
3. Duthie MS, Kimber I, Norval M. The effects of ultraviolet radiation on the human immune system. Br J Dermatol. 1999;140:995-1009.
4. Bikle DD. A bright future for the sunshine hormone. Sci Med. 1995;2:58-67.
5. DeLuca HF. Vitamin D. Nutr Today. 1993;28:6-11.
6. Melnikova VO, Ananthaswamy HN. Cellular and molecular events leading to the development of skin cancer. Mutat Res. 2005;571:91-106.
7. Pray WS. Nonprescription Product Therapeutics. 2nd ed. Baltimore, MD: Lippincott Williams & Wilkins; 2006.
8. Rostan EF. Laser treatment of photodamaged skin. Facial Plast Surg. 2005;21:99-109.
9. Rabello-Fonseca RM, Azulay DR, Luiz RR, et al. Oral isotretinoin in photoaging: clinical and histopathological evidence of efficacy in an off-label indication. J Eur Acad Dermatol Venereol. 2009;23:115-123.
10. Sjerobabski Masnec I, Poduje S. Photoaging. Coll Antropol. 2008;32(suppl 2):177-180.
11. Laga AC, Murphy GF. The translational basis of human cutaneous photoaging: on models, methods, and meanings. Am J Pathol. 2009;174:357-360.
12. Ho SG, Chan HH. The Asian dermatologic patient: review of common pigmentary disorders and cutaneous diseases. Am J Clin Dermatol. 2009;10:153-168.
13. Jackson R. Elderly and sun-affected skin. Can Fam Physician. 2001;47:1236-1243.
14. Knott A, Reuschlein K, Lucius R, et al. Deregulation of versican and elastin binding protein in solar elastosis. Biogerontology. 2009;10:181-190.
15. Ditre C, Wu J, Baumann LS, Rigel D. Innovations in natural antioxidants and their role in dermatology. Cutis. 2008;82(suppl 6):2-16.
16. Resnick L, Rabinovitz H, Binninger D, et al. Topical sulindac combined with hydrogen peroxide in the treatment of actinic keratoses. J Drugs Dermatol. 2009;8:29-32.
17. Garcia C, Poletti E, Crowson AN. Basosquamous carcinoma. J Am Acad Dermatol. 2009;60:137-143.
18. MacFarlane DF, Alonso CA. Occurrence of nonmelanoma skin cancers on the hands after UV nail light exposure. Arch Dermatol. 2009;145:447-449.
19. Hachiya A, Sriwiriyanont P, Fujimura T, et al. Mechanistic effects of long-term ultraviolet UV irradiation induce epidermal and dermal changes in human skin xerografts. Am J Pathol. 2009;174:401-413.
20. Wolff T, Tai E, Miller T. Screening for skin cancer: an update of the evidence for the U.S. Preventive Services Task Force. Ann Intern Med. 2009;150:194-198.
21. Solumbra. Sun Precautions, Inc. www.sunprecautions.com. Accessed April 30, 2009.
22. FDA aims to upgrade sunscreen labeling. www.fda.gov/consumer/updates/
23. Ortega GR, Deimling MJ, Delgado JA. Vitamins and related compounds. In: Block JH, Beale JM Jr, eds. Wilson and Gisvold’s Textbook of Organic Medicinal and Pharmaceutical Chemistry. 11th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004:866-903.






