US Pharm. 2010;35(2):24-29.
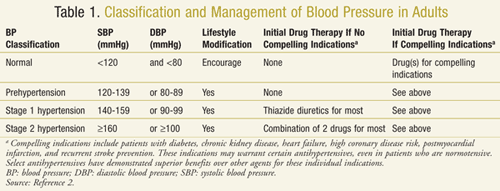
Nearly 72 million people in the United States have hypertension (HTN), and one out of three American adults has HTN. In addition, one-third of people with HTN are unaware they even have high blood pressure (BP), which is why HTN is often referred to as “the silent killer.”1 Hypertension is defined as a BP >140/90 millimeters of mercury (mmHg). As BP rises, risk increases for heart failure, myocardial infarction, kidney disease, and stroke. For each 20 mmHg increase in systolic blood pressure (SBP) or 10 mmHg increase in diastolic blood pressure (DBP) above 115/75 mmHg, the risk of cardiovascular disease doubles.2 A recent study conducted in nondiabetic patients supports treating to a target SBP <130 mmHg versus a target SBP <140 mmHg. The group achieving the lower SBP experienced significantly less development of left ventricular hypertrophy and cardiovascular events than the group treated to the usual SBP goal.3 Current Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7) classification and treatment of BP for adults is given in TABLE 1.
Various lifestyle risk factors have been identified that elevate blood pressure and lead to HTN. Many of these risk factors have been well documented in the literature, and according to recent trials or new research awaiting publication, others have recently been postulated to affect BP (TABLE 2). A healthy lifestyle is essential to preventing HTN and managing it successfully. Lifestyle modifications should be incorporated into every treatment regimen for prehypertension and HTN (TABLE 3). Implementation of a healthy lifestyle decreases BP, reduces cardiovascular disease risk, and increases the efficacy of antihypertensive medications.2
Conventional Risk Factors for Developing Hypertension
Hypertension can develop because of a person’s lifestyle, medication regimen, underlying health conditions, genetic history, or a combination of these factors. Nonmodifiable risk factors include advancing age, race, family history of HTN or premature heart disease, and other concurrent health conditions. Some of these health conditions include adrenal tumors, chronic kidney disease, congenital heart defects, diabetes, thyroid disorders, pheochromocytoma, and pregnancy. Hypertension is more common in African Americans and appears to develop at an earlier age in this race. Medications that may cause HTN include caffeine, chronic steroid therapy, oral contraceptives, nonsteroidal anti-inflammatory drugs (NSAIDs), cyclooxygenase-2 (COX-2) inhibitors, amphetamines and other stimulant drugs, cocaine, decongestants, weight loss drugs, cyclosporine and other immunosuppressants, erythropoietin, and OTC supplements (e.g., ephedra, licorice, ma huang).2
Established Lifestyle Risk Factors for Developing Hypertension
There are many modifiable risk factors for HTN, and the list seems to be growing steadily with ongoing research. Cigarette smoking is the single most common avoidable cause of cardiovascular death in the world.4 Data from the CDC show that 21% of adults (18 years of age and older) in the U.S. currently smoke cigarettes.5 Those who smoke 15 or more cigarettes per day have a higher incidence of HTN. Smoking immediately raises BP and heart rate transiently through increasing sympathetic nerve activity and myocardial oxygen consumption. Chronically, tobacco chemicals damage the lining of the arterial walls of the heart, resulting in artery stiffness and narrowing that can last for 10 years after smoking cessation. Smoking also increases the progression of renal insufficiency and risk of other cardiovascular complications.4,6

Obesity is estimated to be the leading cause of preventable illness in the U.S. Greater than two-thirds of HTN prevalence can be attributed to obesity.7 The National Heart, Lung, and Blood Institute (NHLBI) defines obesity as having a body mass index (BMI) ³30 kg/m2.2 Results from the National Health and Nutrition Examination Survey (NHANES, 2005-2006) indicate that 34.3% of the U.S. adult population is obese.8 Obesity is most pronounced in the southeast region of the country. Overweight prevalence among children and adolescents also remains high in the U.S., with 10% of U.S. children classified as overweight or obese.7,8 Abdominal adiposity, in particular, is linked to congestive heart failure, coronary artery disease, diabetes, sleep apnea, and stroke. Being overweight requires that more blood be supplied to oxygenate heart tissues, and as the circulated blood volume increases through the blood vessels, the pressure increases on the artery walls.6,7
Besides obesity, a lack of physical activity and sedentary lifestyle produce an increase in heart rate. An increased heart rate requires that the heart work harder with each contraction, and it exerts a stronger force on the arteries, thereby raising BP. Physical inactivity has also been linked to more health care office visits, hospitalizations, diabetes, and increased medication burden.6,9
Multiple dietary factors increase the risk for HTN. It is well known that excessive sodium intake leads to HTN. A diet high in salt causes the body to retain fluid, and increased water movement raises the pressure within the vessel walls.6 The majority of the sodium in Western-style diets is derived from processed foods. High-salt diets decrease the effectiveness of antihypertensives in patients with resistant HTN. Resistant HTN is defined as having a BP above one’s goal despite using three or more antihypertensive medications concurrently.10 A high-salt diet can also increase the need for potassium. Potassium balances the amount of sodium within cells. If not enough potassium is consumed or retained, sodium accumulates in the blood. A diet low in potassium (<40 mEq/day) produces sodium accumulation through decreased sodium excretion, thereby leading to HTN. Potassium deficiency also increases the risk for stroke.6,11
Excessive alcohol consumption consisting of greater than two drinks per day for men or greater than one drink per day for women leads to sustained BP elevations.2 Alcohol interferes with blood flow by moving nutrient-rich blood away from the heart.12 Alcohol can also reduce the effectiveness of antihypertensives. Binge drinking, or having at least four drinks consecutively, may cause significant and rapid increases in BP.13 Debate exists on whether low-to-moderate alcohol consumption raises or lowers BP.
Emerging Risk Factors for Developing Hypertension
A diet high in sugar, fructose in particular, raises BP in men, according to a recent study presented at the American Heart Association’s (AHA) 2009 High Blood Pressure Research Conference.14 High fructose consumption has also been linked to an increased risk of obesity. Fructose is a dietary sugar that is used in corn syrup and accounts for one-half of the sugar molecules in table sugar. High-fructose corn syrup is often utilized in packaged sweetened products and drinks due to its long shelf life and low cost. In this study, men consuming a high-fructose diet for just 2 weeks experienced an increased incidence of HTN and metabolic syndrome.14
Vitamin D deficiency (<80 nmol/L) may increase the risk of developing systolic HTN in premenopausal women years later, according to a study conducted in Caucasian women in Michigan.15 In this study, presented at the AHA’s High Blood Pressure Research Conference, researchers compared BP and vitamin D levels drawn in 1993 to those drawn 15 years later in 2007. Premenopausal women (average age of 38 years) with vitamin D deficiency in 1993 were three times more likely to have HTN in 2007 than those with normal vitamin D levels in 1993.15
Sleep deprivation raises SBP and DBP and may lead to HTN. In the recent Coronary Artery Risk Development in Young Adults (CARDIA) sleep study, sleep maintenance and sleep duration were measured in a group of adults aged 35 to 45 years and then repeated 5 years later on the same study population.16 According to this study, shorter sleep duration and poor sleep quality increase BP levels and lead to HTN. Sleep deprivation may produce an increase in heart rate and sympathetic activity, evolving into HTN.16
A connection has been found between HTN and road traffic noise. An Environmental Health study published in 2009 measured loudness of road noise in decibels at the home address in a large number of adults and their incidence of self-reported HTN. A significant association was found for incidence of HTN and residing near a noisy road. Interestingly, a less prominent effect on BP was noted in the elderly when compared to younger adults. Possible explanations offered by the authors include that noise may be harder to detect in the elderly and may be less of an annoyance in the older population than in younger individuals. The study authors speculate that long-term exposure to noise causes endocrine and a sympathetic stress response on a middle-aged adult’s vascular system, resulting in HTN and an elevated cardiovascular risk profile.17
A questionnaire completed by deployed American servicemen and servicewomen revealed that those reporting multiple exposures to combat had a significantly higher incidence of HTN than those reporting no combat. The elevation in BP is thought to arise from the high stress situation of combat exposure. Combat stress can result in significant physical and psychosocial stress to those deployed.18
Lifestyle Modifications for Treatment of Hypertension
Cigarette smoking is a modifiable cardiovascular risk factor that can have profound effects. Smoking cessation can result in immediate improvement in BP and heart rate after just 1 week.19 A linear relationship has been discovered in improvement in arterial wall stiffness and duration of smoking cessation in ex-smokers. Achievement of a decade of smoking cessation results in remodeling to nonsignificant levels of arterial stiffness.20 In addition to lowering BP, smoking cessation results in an overall cardiovascular risk reduction and reduction in mortality. Rigorous measures should be utilized to assist individuals in achieving smoking cessation.2 Smoking cessation should be assessed and discussed at every available opportunity, whether it be inpatient, outpatient, or at the pharmacy. Studies have shown that when patients are told their lung age, they are more likely to quit smoking.21 Pharmacists possess an enormous opportunity to assist patients in achieving smoking cessation by teaching patients about the various smoking cessation pharmacotherapy options. An explanation of how to properly use the medications (OTC and prescription), differences between them, and what to expect from the medications can improve adherence and the desired outcome of successful smoking cessation.
Weight reduction can have the most profound effect of all lifestyle modifications on lowering BP, leading to an approximate drop in SBP of 5 to 20 mmHg per 10 kg weight loss. The JNC 7 guidelines recommend weight reduction to maintain a normal body weight defined as a BMI between 18.5 and 24.9 kg/m2.2 The Surgeon General’s recommendations published by the U.S. Department of Health and Human Services advise determining a person’s BMI and having him or her lose at least 10% of body weight if overweight or obese. It is also recommended to lose weight gradually at a pace of one-half to two pounds per week.22
Along with weight reduction, regular aerobic physical activity for 30 minutes or more per day most days of the week is recommended and results in an SBP improvement of 4 to 9 mmHg.2 It is recommended that children be physically active for 60 minutes most days of the week. The Surgeon General recommends limiting television viewing to below 2 hours per day.22
The JNC 7 guidelines recommend multiple dietary modifications. The most notable and effective is adoption of the Dietary Approaches to Stop Hypertension (DASH) eating plan, which can lower SBP by 8 to 14 mmHg. 2 The DASH eating plan is equally efficacious to adding on a single antihypertensive medication. This diet plan includes a significant consumption of fruits and vegetables rich in potassium, which assists in maintaining optimal sodium to potassium ratio. The DASH eating plan is low in saturated fat and consists of low-fat dairy products. Sodium restriction is an important component of the DASH diet and also recommended independently in the JNC 7 guidelines. A reduction in sodium intake to £100 mmol/day (6 g NaCl or 2.4 g sodium) can drop SBP by 2 to 8 mmHg. The DASH diet also provides details on how to check labels for sodium content and how to estimate sodium amounts in foods based on how they are cooked or prepared when eating in restaurants.2,23 The Surgeon General also recommends selecting sensible portions.22
Limiting alcohol consumption to two drinks or less for most men and one drink per day or less for women is recommended by the JNC 7 guidelines. The equivalency of two drinks is defined as 24 oz of beer, 1 oz of ethanol (e.g., vodka, gin), 3 oz of 80-proof whiskey, or 10 oz of wine. A decrease in alcohol intake can lower SBP by 2 to 4 mmHg.2
Plausible Lifestyle Modifications for Treatment of Hypertension
Lowering fructose intake through limiting consumption of sweetened products could prevent rises in BP and development of metabolic syndrome. Reducing intake of sweetened drinks or processed foods that contain high-fructose corn syrup and lessening use of regular table sugar will lower intake of fructose.14
Vitamin D deficiency is widespread among women. It is speculated by some researchers that many women do not receive adequate sun exposure, obtain enough vitamin D in their diet, or supplement with enough vitamin D. The current recommended intake of vitamin D for this population is 400 to 600 IUs per day, though some researchers suggest a higher intake of daily vitamin D. Knowing one’s vitamin D level and obtaining adequate vitamin D through diet and/or supplementation may prevent HTN.15
A randomized, controlled trial published in 2007 demonstrated that regular consumption of a small amount of dark chocolate has been shown to mildly reduce BP (-2.9 mmHg systolic and -1.9 mmHg diastolic average) in people with stage 1 HTN or prehypertension. The study population did not have other cardiovascular risk factors and were not taking antihypertensive medications. This study compared daily intake (30 kcal, or the equivalent of a Hershey’s Kiss) of dark chocolate and white chocolate for 18 weeks. The group receiving white chocolate had no improvement in BP. It is suspected that the polyphenols in the dark chocolate lower BP.24
A recent study explored the effects of various milk and cheese products on developing HTN in adults aged 55 years and older living in the Netherlands. It was discovered after 6 years that higher dairy intake was associated with lower rates of HTN. The authors concluded that consumption of low-fat dairy products may prevent HTN in older individuals.25 Another study conducted in U.S. women aged 45 years and older showed similar results with intake of low-fat dairy products, but not with supplements of calcium or vitamin D.26
Lastly, various studies have shown that ownership of a dog or cat lowers a person’s BP. Whether this is accomplished through increased exercise or the psychological effects of a human-animal connection is yet to be fully established. Health benefits of pet ownership include BP reductions, a reduction in triglyceride levels, improved exercise habits, decreased feelings of loneliness, and decreased stress levels.27,28
Conclusion
A person’s way of life can have substantial effects on his or her health, including the risk of developing HTN. Numerous lifestyle risk factors have been implicated in the development of HTN; likewise, several lifestyle modifications effectively lower BP. Alterations in lifestyle are essential to prevention and treatment of HTN and can decrease the need for one or more prescription medications. Lifestyle changes to lower BP can additionally correct obesity, lower cardiovascular risk, decrease insulin resistance, improve drug efficacy, and enhance antihypertensive effect. Greater BP reductions are achieved if two or more lifestyle adjustments are made concurrently. Assisting and motivating patients to make lifestyle changes to lower their BP to goal levels is recommended by the JNC 7 guidelines yet is often underutilized by health care clinicians. It is imperative that pharmacists be knowledgeable in risk factors and treatments for HTN and express interest in having patients reach their BP goals. Studies have proven that involvement of a pharmacist in the treatment of hypertensive patients can result in improved BP control through adoption of lifestyle modifications, proper antihypertensive selection, and better adherence to medications.2,29
REFERENCES
1. High blood pressure fact sheet. Centers for Disease Control and Prevention. www.cdc.gov/DHDSP/library/fs_bloodpressure.htm. Accessed October 10, 2009.
2. JNC 7 Express. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. NIH Publication No. 03-5233. December 2003. www.nhlbi.nih.gov/guidelines/hypertension/express.pdf. Accessed October 10, 2009.
3. Verdecchia P, Staessen JA, Angeli F, et al. Usual versus tight control of systolic blood pressure in non-diabetic patients with hypertension (Cardio-Sis): an open-label randomised trial. Lancet. 2009;374:525-533.
4. Kaplan NM. Smoking and hypertension. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate; 2009.
5. FastStats on smoking. Centers for Disease Control and Prevention. www.cdc.gov/nchs/fastats/smoking.htm. Accessed October 10, 2009.
6. High blood pressure (hypertension). Risk factors. Mayo Clinic. www.mayoclinic.com/health/high-blood-pressure/DS00100/DSECTION=risk-factors. Accessed October 10, 2009.
7. Narkiewicz K. Obesity and hypertension—the issue is more complex than we thought. Nephrol Dial Transplant. 2006;21:264-267.
8. Overweight and obesity. Data and statistics. Centers for Disease Control and Prevention. www.cdc.gov/obesity/data/index.html. Accessed October 10, 2009.
9. In brief: your guide to physical activity and your heart. National Heart, Lung, and Blood Institute. NIH Publication No. 06-5847. Reprinted January 2008. www.nhlbi.nih.gov/health/public/heart/obesity/phy_active_brief.pdf. Accessed October 10, 2009.
10. Pimenta E, Gaddam KK, Oparil S, et al. Effects of dietary sodium reduction on blood pressure in subjects with resistant hypertension: results from a randomized trial. Hypertension. 2009;54:475-481.
11. Kaplan NM, Rose BD. Potassium and hypertension. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate; 2009.
12. Saunders E. High blood pressure: tips to stop the silent killer. University of Maryland Medical Center. www.umm.edu/features/blood_pressure.htm. Accessed October 31, 2009.
13. Ten ways to control blood pressure without medication. Mayo Clinic. www.mayoclinic.com/health/high-blood-pressure/HI00027. Accessed October 31, 2009.
14. Johnson R, Perez-Pozo S, Schold J, Lillo JL. High-sugar diet increases men’s blood pressure; gout drug protective. Abstract P127. American Heart Association. September 23, 2009. http://americanheart.mediaroom.com/index.php?s=43&item=829. Accessed October 31, 2009.
15. Griffin FC, Sowers MR, Gadegbeku CA. Vitamin D deficiency in younger women is associated with increased risk of high blood pressure in mid-life. Abstract P253. American Heart Association. September 24, 2009. http://americanheart.mediaroom.com/index.php?s=43&item=823. Accessed October 31, 2009.
16. Knutson KL, Van Cauter E, Rathouz PJ, et al. Association between sleep and blood pressure in midlife: the CARDIA sleep study. Arch Intern Med. 2009;169:1055-1061.
17. Bodin T, Albin M, Ardo J, et al. Road traffic noise and hypertension: results from a cross-sectional public health survey in southern Sweden. Environ Health. 2009;8:38.
18. Granado NS, Smith TC, Swanson GM, et al. Newly reported hypertension after military combat deployment in a large population-based study. Hypertension. 2009;54:966-973.
19. Minami J, Ishimitsu T, Matsuoka H. Effects of smoking cessation on blood pressure and heart rate variability in habitual smokers. Hypertension. 1999;33:586-690.
20. Jatoi NA, Jerrard-Dunne P, Freely J, Mahmud A. Impact of smoking and smoking cessation on arterial stiffness and aortic wave reflection in hypertension. Hypertension. 2007;49:981-985.
21. Parkes G, Greenhalgh T, Griffin M, Dent R. Effect of smoking quit rate of telling patients their lung age: the Step2quit randomized controlled trial. BMJ. 2008;336:598-600.
22. Surgeon General’s healthy weight advice for customers. U.S. Department of the Health and Human Services Office of the Surgeon General. www.surgeongeneral.gov/topics/obesity/calltoaction/fact_advice.htm. Accessed November 1, 2009.
23. Your guide to lowering your blood pressure with DASH. U.S. Department of Health and Human Services. NIH Publication No. 06-4082. Revised April 2006. www.nhlbi.nih.gov/health/public/heart/hbp/dash/new_dash.pdf. Accessed November 1, 2009.
24. Taubert D, Roesen R, Lehmann C, et al. Effects of low habitual cocoa intake on blood pressure and bioactive nitric oxide. JAMA. 2007;298:49-60.
25. Engberink MF, Hendriksen MA, Schouten EG, et al. Inverse association between dairy intake and hypertension: the Rotterdam Study. Am J Clin Nutr. 2009;89:1877-1883.
26. Wang L, Manson JE, Buring JE, et al. Dietary intake of dairy products, calcium, and vitamin D, and the risk of hypertension in middle-aged and older women. Hypertension. 2008;51:1073-1079.
27. Jackson K. A pet in your life keeps the doctor away. Medical News Today. September 30, 2009. www.medicalnewstoday.com/articles/165580.php. Accessed November 6, 2009.
28. Health benefits of pets. Centers for Disease Control and Prevention. www.cdc.gov/Healthypets/health_benefits.htm. Accessed November 6, 2009.
29. Sookaneknun P, Richards R, Sanguansermsri J, Teerasut C. Pharmacist involvement in primary care improves hypertensive patient clinical outcomes. Ann Pharmacother. 2004;38:2023-2028.
To comment on this article, contact rdavidson@uspharmacist.com.






