US Pharm. 2011;36(11):58-63.
Obsessive-compulsive disorder (OCD) is an extremely disabling disease that causes significant distress and compromised quality of life.1 The features of OCD are recurrent obsessions and/or compulsions that consume a large amount of time (>1 hour/day).2 OCD has been described as one of the 10 most disabling disorders.3 Most patients experience a waxing and waning of symptoms, with exacerbations occurring during times of stress.2
An obsession is a persistent and intrusive thought, idea, image, or impulse that results in marked anxiety or distress, such as wondering whether the stove was left on or being preoccupied with cleanliness.4 TABLE 1 lists some common obsessions.1

A compulsion is a repetitive behavior or mental act that is carried out in response to an obsession.4 A compulsion is performed to alleviate the anxiety caused by an obsession.1 Examples include counting and repetitive handwashing. A compulsion does not bring pleasure to the patient.4 Often, the patient experiences shame and tries to keep this condition a secret because he or she knows that these thoughts or actions are excessive or unreasonable.1 TABLE 1 lists some common compulsions.1
Epidemiology
The National Comorbidity Survey Replication determined the lifetime prevalence of OCD to be 2.3%, with a 12-month prevalence of 1.2%. Approximately half of survey respondents who reported having had OCD at some time in their life also reported suffering from symptoms within the last 12 months. The estimated amount of time per day that respondents were plagued by obsessions was 5.9 hours, and 4.6 hours per day were spent engaging in compulsions.5
The onset of OCD usually occurs during adolescence or early adulthood, and there do not seem to be any gender-related differences; males and females are equally afflicted.2 There is a strong genetic component to OCD, and familial and environmental factors may influence the development of the disorder.6
Diagnosis
The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), considers OCD to be an anxiety disorder.7 The differential diagnosis of OCD includes depressive ruminations, generalized anxiety disorder, posttraumatic stress disorder, and schizophrenic and manic delusions.8
OCD may be difficult to diagnose because of the patient’s reluctance to reveal information about his or her thoughts or behaviors. Morgan and Kirkwood provide three screening questions: 1) Do you have repetitive thoughts that make you anxious and that you cannot get rid of regardless of how hard you try? 2) Do you keep things extremely clean or wash your hands frequently? 3) Do you check things excessively?4 Fenske and Schwenke suggest asking: Do you ever find it necessary to do certain things that don’t make sense or that you don’t want to do?1
Although it is not a diagnostic tool, the Yale-Brown Obsessive Compulsive Scale (Y-BOCS) is used to determine the severity of a patient’s OCD symptoms. By focusing on the characteristics of obsessions and compulsions, rather than on the content, this scale can reliably assess the efficacy of the treatment a patient is receiving.9 The Y-BOCS evaluates symptoms based on how much of the patient’s time they occupy, the degree to which they interfere with normal functioning, the level of distress they cause, how much the patient resists them, and how much control the patient has over them.8,9 An example of the Y-BOCS is found at
www.stlocd.org/handouts/YBOC-
Subtypes
Various subtypes of OCD exist. These include the early-onset, hoarding, “just right,” primary obsessional, scrupulosity, tic-related, and pediatric autoimmune neuropsychiatric disorders associated with streptococcus (PANDAS) OCD subtypes.
Early-onset OCD develops before puberty, and there is a high likelihood that this form will go into remission before adulthood. Early-onset OCD is more likely to be associated with tics and other comorbidities (e.g., attention-deficit/
Hoarding is often associated with more severe symptoms and higher rates of psychiatric comorbidities (social phobia, in particular). Quality of life is more severely impaired with hoarding than with other subtypes.1 Hoarding tends to be resistant to treatment, including medication and psychotherapy.8 Consideration is being given to classifying hoarding as an independent syndrome, often with comorbid OCD.10
Patients suffering from the “just right” subtype need to have things a certain way or under control. This need results in repetitive actions to relieve anxiety. While “just not right” feelings occur in all subtypes, this is the primary manifestation of “just right” OCD.1
Approximately 25% of OCD patients do not experience compulsions; however, they may have mental rituals (e.g., counting, praying). The obsessions commonly have themes of violence, sex, or religion.1 This is the primary obsessional subtype.
Patients with the scrupulosity subtype are concerned with morality or religion. For people with strong religious beliefs, this form of OCD can be extremely devastating. Obsessions may include blasphemous thoughts or a focus on whether the patient has committed a sin; compulsions may involve excessive prayer or confession or seeking reassurance from clergy.1
Tic-related OCD tends to have an early onset (10%-40% of all cases are diagnosed before adulthood), and there is a strong chance of remission later in the patient’s life.7 This form of OCD may be associated with Tourette’s syndrome.1 A high incidence of psychiatric comorbidities, such as ADHD, body dysmorphic disorder, trichotillomania, social anxiety, and mood disorders, accompanies tic-related OCD. Some common obsessions include hoarding and those involving the body, as well as those related to symmetry and appearance.1,7 Often, selective serotonin reuptake inhibitors (SSRIs) alone are not effective, and an adjunctive atypical antipsychotic is needed.1 Although no specific genes have been isolated, there is a strong familial component.7
When OCD and tic disorders develop after an infection with Group A beta-hemolytic streptococcus, PANDAS is suspected. There is a waxing and waning of symptoms with this form of OCD. PANDAS is theorized to be caused by an autoimmune process. Some experts doubt the existence of PANDAS, while other clinicians use prophylactic antibiotic treatment to prevent it.7
There are also some miscellaneous types of OCD. Some patients develop OCD following an acute brain injury. The use of atypical antipsychotics to treat patients with schizophrenia has resulted in OCD symptoms. It is unclear whether OCD following treatment is an adverse effect of the atypical antipsychotic or the unmasking of comorbid OCD that was not apparent while the schizophrenia went untreated.10
Certain OCD subtypes that occur prior to puberty are being considered as independent syndromes for the upcoming DSM-V. These include tic-related OCD, early-onset OCD, and PANDAS.7
Psychiatric Comorbidities
Almost 90% of patients with OCD suffer from another psychiatric disorder.5,10 These conditions include other anxiety disorders, major depressive disorder, eating disorders, and personality disorders.2 Alcohol or substance abuse may occur in OCD patients.8 In children with OCD, learning disorders and behavioral disorders are common.2
Major depressive disorder is the most common comorbidity, with approximately two-thirds of patients experiencing it at some point in their lives.1 Sometimes comorbid depression is associated with a poorer treatment outcome.8 Suicidal ideation occurs in more than 50% of patients, and 15% have made suicide attempts. Thoughts of suicide strongly correlate with comorbid depression.1
Many conditions fall under the umbrella of “obsessive-compulsive spectrum” conditions and have symptoms that overlap those of OCD. These generally fall into one of three categories: neurologic-motoric conditions (e.g., Tourette’s syndrome), impulse-control disorders (e.g., trichotillomania, skin picking, pathologic gambling), or conditions involving bodily preoccupation (e.g., body dysmorphic disorder, eating disorders, hypochondriasis).11 There is no consensus as to whether any of these are distinct disorders or whether they are varying manifestations of an overall obsessive-compulsive spectrum.10
Treatment
Because it can be difficult to diagnose, OCD is often undertreated.1 The average lag time of diagnosis is 17 years.3 Treatment rarely resolves all symptoms, and improvement occurs slowly. Despite this, even partial symptom resolution can be beneficial for the patient.1,4 The goals of treatment are primarily focused on decreasing symptoms and improving the patient’s functioning and quality of life.8 Patient and family education can be helpful for enhancing adherence to treatment. Attendance at self-help groups, which may be located through the International OCD Foundation ( www.ocfoundation.org), may be of great benefit to the patient.8 Treatment for OCD consists of psychotherapy (particularly cognitive-behavioral therapy [CBT]) and medication.1,4
In CBT, the patient is exposed to the focus of his or her obsession, either literally (touching items in a public bathroom) or figuratively (thinking about the obsession), and then learns to postpone the compulsive response.1 This form of CBT is called exposure and response prevention (ERP).3 ERP may be used as first-line treatment in patients wishing to avoid or postpone medication therapy.8
Medication Therapy
The neurobiology of OCD is complex, and it is thought that several neurotransmitters are involved. Because OCD responds well to serotonin reuptake inhibitors (SRIs), there is a consensus that serotonin imbalance is the primary mechanism for the disorder; however, 50% to 60% of patients treated with SRI monotherapy have an inadequate response.12 The SRIs used for OCD are clomipramine and SSRIs. Fluoxetine, paroxetine, fluvoxamine, and sertraline are approved for OCD treatment, but other SSRIs are used off-label.1,4 There is some evidence that clomipramine has superior efficacy over SSRIs, but because of better tolerability, SSRIs are the first-line agent of choice.8 In a meta-analysis by Soomro et al, patients taking an SSRI were twice as likely as those given placebo to have at least a 25% reduction in symptoms.13
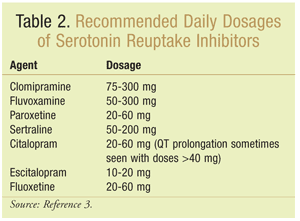
Medication dosages for OCD are greater than those for major depression.1,4,8 The recommended daily dosages are as follows: clomipramine 75-300 mg; fluvoxamine 50-300 mg; paroxetine 20-60 mg; sertraline 50-200 mg; citalopram 20-60 mg (QT prolongation sometimes occurs with doses >40 mg); escitalopram 10-20 mg; and fluoxetine 20-60 mg (TABLE 2).3 The patient should be monitored for serotonin syndrome (anxiety, tremor, tachycardia, and sweating).8 Especially in the elderly, the drug must be slowly titrated up to the maximum tolerated dosage. Before it is concluded that the patient’s response is inadequate, the medication should be taken for at least 8 to 12 weeks, with 4 to 6 weeks at the maximum tolerated dosage.8 The pharmacist should warn the patient that it may take weeks or months for the medication to work; adherence to the medication regimen should be encouraged, and the pharmacist should be available to offer support.1
In the event that the response to initial SSRI therapy is inadequate, there are several alternatives. Switching the SRI to a different one may be useful.3 Unfortunately, there are no data to suggest which agent works best. The addition of CBT may be an option.8 If the initial agent is an SSRI, augmentation with clomipramine may be feasible; however, plasma concentrations of clomipramine and desmethylclomipramine should be determined 2 to 3 weeks after a daily dosage of 50 mg is reached. Total plasma concentrations should be kept below 500 ng/mL to avoid cardiac and central nervous system toxicity.8 The addition of a dopamine receptor antagonist has shown promise in clinical trials.3,8
In a systematic review by Komossa et al, quetiapine and risperidone showed some efficacy as adjunctive medications; however, the efficacy of olanzapine was inconclusive.14 Atypical antipsychotics may be useful in patients with tics, but sometimes adverse effects limit their use.14
Neuroimaging studies have suggested that glutamate (an excitatory neurotransmitter) may play a role in the pathophysiology of OCD.15-17 Some promising evidence suggests that agents active in glutamatergic neurotransmission have shown efficacy in the treatment of OCD. Memantine has been studied and shown benefit as an adjunctive agent for refractory OCD.15,16 Amantadine has been reported to ameliorate OCD symptoms in patients who do not respond adequately to SSRI monotherapy.17
Another agent being studied for adjunctive therapy is ondansetron. Ondansetron, a 5-HT3 antagonist, is used as an antiemetic. Taken concurrently with an SSRI, the drug has shown increased efficacy without a worsening of adverse effects in some studies.18,19
Drug therapy should be continued for at least 1 to 2 years.1,4 When medication therapy is being discontinued, the drug should be tapered in decrements of 10% to 25% every 1 to 2 months, and OCD symptoms should be monitored throughout the process.8 The relapse rate is high, and long-term treatment is warranted by two to four severe relapses or three to four moderate relapses.1,4 Some patients require lifelong medication.1
Conclusion
OCD is an extremely debilitating condition that causes the patient distress and a reduction in quality of life. It often responds poorly to medication therapy. SRIs, in particular SSRIs, are the cornerstone of treatment. ERP therapy used in conjunction with medication often results in a greater response.3 The job of the pharmacist is to reassure patients and make them aware of the resources available to them, such as the International OCD Foundation.
REFERENCES
1. Fenske JN, Schwenk TL. Obsessive compulsive disorder: diagnosis and management. Am Fam Physician. 2009;80:239-245.
2. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
3. Stein DJ, Denys D, Gloster AT, et al. Obsessive-compulsive disorder: diagnostic and treatment issues. Psychiatr Clin N Am. 2009;32:665-685.
4. Morgan LA, Kirkwood CK. Anxiety disorders. In: Linn WD, Wofford MR, O’Keefe ME, Posey LM, eds. Pharmacotherapy in Primary Care. New York, NY: McGraw Hill Medical; 2009:255-261.
5. Ruscio AM, Stein DJ, Chiu WT, Kessler RC. The epidemiology of obsessive-compulsive disorder in the National Comorbidity Survey Replication. Mol Psychiatry. 2010;15:53-63.
6. Pauls DL. The genetics of obsessive-compulsive disorder: a review. Dialogues Clin Neurosci. 2010;12:149-163.
7. Leckman JF, Denys D, Simpson HB, et al. Obsessive-compulsive disorder: a review of the diagnostic criteria and possible subtypes and dimensional specifiers for DSM-V. Depress Anxiety. 2010;27:507-527.
8. Koran LM, Hanna GL, Hollander E, et al. Practice guideline for the treatment of patients with obsessive-compulsive disorder. Am J Psychiatry. 2007;164(7 suppl):5-53.
9. Goodman WK, Price LH, Rasmussen SA, et al. The Yale-Brown Obsessive Compulsive Scale. I. Development, use, and reliability. Arch Gen Psychiatry. 1989;46:1006-1011.
10. Murphy DL, Timpano KR, Wheaton MG, et al. Obsessive-compulsive disorder and its related disorders: a reappraisal of obsessive-compulsive spectrum concepts. Dialogues Clin Neurosci. 2010;12:131-148.
11. Wetterneck CT, Teng EJ, Stanley MA. Current issues in the treatment of OC-spectrum conditions. Bull Menninger Clin. 2010;74:141-166.
12. Koo MS, Kim EJ, Roh D, Kim CH. Role of dopamine in the pathology and treatment of obsessive-compulsive disorder. Expert Rev Neurother. 2010;10:275-290.
13. Soomro GM, Altman D, Rajagopal S, Oakley-Browne M. Selective serotonin re-uptake inhibitors (SSRIs) versus placebo for obsessive compulsive disorder (OCD). Cochrane Database Syst Rev. 2008;(1):CD001765.
14. Komossa K, Depping AM, Meyer M, et al. Second-generation antipsychotics for obsessive compulsive disorder. Cochrane Database Syst Rev. 2010;(12):CD008141.
15. Aboujaoude E, Barry JJ, Gamel N. Memantine augmentation in treatment-resistant obsessive-compulsive disorder: an open-label trial. J Clin Psychopharmacol. 2009;29:51-55.
16. Stewart SE, Jenike EA, Hezel DM, et al. A single-blinded case-control study of memantine in severe obsessive-compulsive disorder. J Clin Psychopharmacol. 2010;30:34-39.
17. Pasquini M, Berardelli I, Biondi M. Amantadine augmentation for refractory obsessive-compulsive disorder: a case report. J Clin Psychopharmacol. 2010;30:85-86.
18. Soltani F, Sayyah M, Feizy F, et al. A double-blind, placebo-controlled pilot study of ondansetron for patients with obsessive-compulsive disorder. Hum Psychpharmacol. 2010;25:509-513.
19. Pallanti S, Bernardi S, Antonini S, et al. Ondansetron augmentation in treatment-resistant obsessive-compulsive disorder: a preliminary, single-blind, prospective study. CNS Drugs. 2009;23:1047-1055.
To comment on this article, contact rdavidson@uspharmacist.com.






