US Pharm. 2012;37(3):HS-2-HS-5.
Male circumcision is a common surgical procedure performed in neonates, generally for religious or cultural reasons. The 1999 Circumcision Policy Statement of the American Academy of Pediatrics (AAP) does not recommend routine neonatal circumcision because of insufficient evidence regarding possible medical benefits. Controversy concerning the suggested medical benefits of circumcision has led to debate in recent decades.1-3 Over the past few decades, the circumcision rate in the United States has dropped. Even given this decline, circumcision is one of the most commonly performed medical procedures in the U.S. There are several different devices available for performing circumcision, and all circumcision procedures require effective local anesthesia and pain management. Complications from the procedure, such as bleeding and infection, are rare.
Background
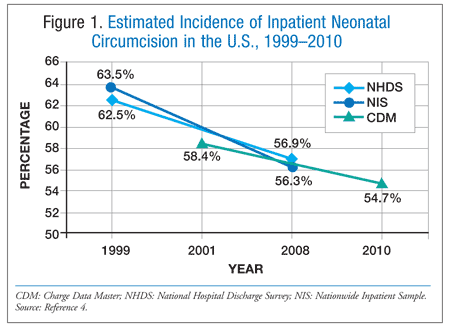
In the U.S., the overall incidence of neonatal circumcision from 1999 to 2010 was approximately 55% to 59%, which is a slight decline from the previous decade (FIGURE 1); however, the actual incidence is likely higher, since these estimates do not include circumcisions performed in the community.4 The reduced incidence could be due to several factors, including—but not limited to—the AAP policy statement, population shifts, and changes in Medicaid coverage. AAP’s stance against routine circumcision may discourage some parents from circumcising their sons. As immigration changes the makeup of the U.S. population, circumcision rates could fluctuate, since circumcision is primarily a religious or cultural decision. As of 2009, neonatal circumcision is covered by Medicaid in 33 states (two additional states provide coverage depending upon the enrollment plan).4 Therefore, circumcision rates could continue to decline if more states elect not to provide coverage for the procedure.
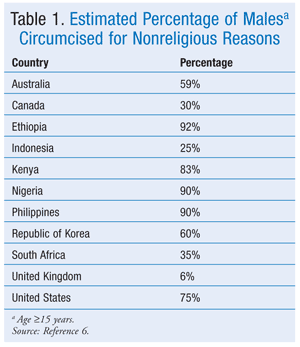
Circumcision is most commonly performed among Jews and Muslims based on religious tradition, and whether or not the child’s father was circumcised is frequently a determining factor for culturally based decisions.1,5,6 In the U.S., an estimated 75% of males aged 15 years and older have been circumcised for nonreligious reasons. The prevalence of males circumcised for nonreligious reasons varies substantially among countries, as shown in TABLE 1.6
Some advocates of circumcision encourage the procedure for its potential medical benefits. There is evidence that uncircumcised infants are more prone to urinary tract infections (UTIs), which may be attributed to higher bacterial colonization on the glans of the penis.7,8 Schoen et al reported a 9.1-fold reduction in UTI incidence in circumcised males during the first year of life.8 Additionally, circumcision may offer protective benefits against sexually transmitted diseases (STDs) such as gonorrhea, syphilis, and HIV, as infectious bacteria that cause STDs are thought to colonize the area underneath the foreskin.2,5,9-11 HIV binds to CD4 and CCR5 receptors on Langerhans cells found on the inner surface of the foreskin, which can lead to an increased risk of HIV transmission during sexual intercourse.9 Research is ongoing regarding the potential medical benefits of circumcision, with the possible reduction of HIV transmission being of great interest worldwide. Furthermore, circumcision may offer protective benefits against penile cancer. Maden et al found that the risk of penile cancer was 3.2 times greater in uncircumcised men than in those who were circumcised; however, the authors also emphasized the importance of considering sexual history and other medical conditions when assessing penile cancer risk.12
The Procedure
The Gomco clamp, the Mogen clamp, and the PlastiBell device are the most commonly used circumcision instruments in the U.S. The Gomco and Mogen clamps protect the glans of the penis while the foreskin is removed by means of a crush injury.5,13,14 In randomized trials, the Gomco clamp was determined to be more painful and took 2.5 times longer to complete the procedure compared with the Mogen clamp; the Mogen clamp was almost twice as fast as the PlastiBell device, with no significant differences in pain scores throughout the procedure.14,15 While the Mogen clamp enables the shortest procedure time, it is thought to remove the least amount of foreskin.5,14,15 The PlastiBell device involves the placement of a plastic protective shield over the glans and under the foreskin. A suture is then placed over the foreskin, compressing it and resulting in tissue necrosis. The foreskin and the plastic shield usually fall off within a week.5,14 The instrument used to perform a circumcision depends primarily upon the provider’s education, training, and overall preference.3,5 Circumcision is contraindicated in premature neonates, those with bleeding disorders or a family history of bleeding disorders, and those with penile abnormalities for which the foreskin may be needed for reconstructive surgery.2,5
Anesthesia and Analgesia
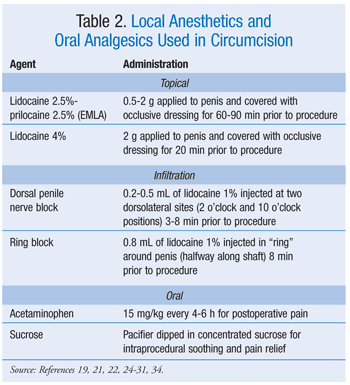
The AAP recommends that adequate analgesia be provided during circumcision, since the procedure is known to be painful.1,3,5 In addition to crying, facial grimacing, and behavioral changes, neonates manifest pain through physiologic markers such as increased heart rate and blood pressure and reduced oxygen saturation.16 No single agent has been proven to provide complete pain relief for all neonates undergoing circumcision; therefore, combination therapy is likely the most effective option.17,18 See TABLE 2 for selected anesthetic and analgesic agents.
Topical Anesthetics: Some providers may prefer topical anesthetics since they are relatively noninvasive and are proven to be safe, with minimal risk of methemoglobinemia or systemic toxicities. Mild erythema, usually occurring within 24 hours, has been reported in some neonates.19-22 Topical lidocaine-prilocaine cream (lidocaine 2.5% and prilocaine 2.5%) is a commonly used eutectic mixture of local anesthetics (EMLA). Through randomized, placebo-controlled trials, lidocaine-prilocaine cream (0.5-2 g under an occlusive dressing) has been shown to be significantly more effective than placebo for reducing pain during circumcision, as measured by behavioral and physiologic changes.19-21,23 Lidocaine-prilocaine cream (1 g) applied to the penis for 60 to 80 minutes prior to circumcision was found to be safe and effective for neonates. Neonates who received lidocaine-prilocaine cream spent less time crying, displayed less facial activity, and experienced smaller increases in heart rate and blood pressure compared with those receiving placebo. However, pain relief was diminished during circumcision phases involving substantial tissue damage.20 Benini et al found similar efficacy using lidocaine-prilocaine 0.5 g cream applied under an occlusive dressing for 45 to 60 minutes prior to circumcision.19
Compared with lidocaine 30% cream (1 g), lidocaine-prilocaine cream (1 g) more effectively reduced crying time and suppressed heart rate and blood pressure increases in neonates undergoing circumcision.21 Topical lidocaine 30% cream (0.5 g) applied to the penis 20 minutes before circumcision did not have an overwhelmingly significant advantage over placebo in terms of physiologic changes; newborns in the placebo group, however, experienced more crying (and at a higher intensity) and leg and arm flailing than the lidocaine group. Lidocaine cream was concluded to be a safe option in newborns since no significant systemic absorption of lidocaine was reported.24
Dorsal Penile Nerve Block (DPNB): Although more invasive than lidocaine-prilocaine cream, DPNB is a more effective method of providing local anesthesia to infants undergoing circumcision.22,25-27 DPNB is administered by injecting lidocaine 1% (0.2-0.5 mL) in two dorsolateral sites (the 2 o’clock and 10 o’clock positions at the base of the penis) 3 to 8 minutes prior to circumcision.14,22,25,26,28 Epinephrine should never be added to the lidocaine because of its vasoconstrictive properties and the risk of ischemia and necrosis.17 To minimize the risk of adverse reactions such as bruising or hematoma formation, proper administration is essential.22 Compared with lidocaine-prilocaine cream, DPNB results in better pain reduction in terms of behavioral changes, pain scale scores, and/or physiologic alterations.22,24,26 Two studies that used Neonatal Infant Pain Scale (NIPS) scores as endpoints concluded that NIPS scores were significantly lower in neonates receiving DPNB versus lidocaine-prilocaine, indicating greater pain reduction.22,26 Additionally, Butler-O’Hara et al reported that infants receiving lidocaine-prilocaine cream (0.5 g applied 60 minutes prior) experienced an escalation in heart rate more than fivefold greater than in infants receiving DPNB.22
Subcutaneous Ring Block: As with DPNB, ring block is more invasive than lidocaine-prilocaine cream and should be administered by a trained clinician; however, the pain of injection is less than that of circumcision. Ring block was determined to be superior to DPNB (0.4 mL of lidocaine 1% at two dorsolateral injection sites), lidocaine-prilocaine cream (2 g applied 90 minutes prior), and placebo in newborns undergoing circumcision. The ring block was administered by injecting 0.8 mL of lidocaine 1% in a “ring” around the penis (halfway along the shaft) approximately 8 minutes prior to the procedure. Ring block more effectively reduced pain during foreskin separation and incision, as evidenced by less crying and lower heart rate. DPNB was the second most effective anesthetic, followed by lidocaine-prilocaine cream. About one-half of newborns in the ring block and DPNB groups experienced minor bruising following the procedure. As with DPNB, epinephrine should not be added to the lidocaine.23
Acetaminophen: Acetaminophen is commonly used to relieve discomfort or pain in infants, but it is not recommended as the sole analgesic to reduce circumcision-related pain. In a double-blind, placebo-controlled trial, infants were randomized to receive either placebo or acetaminophen 15 mg/kg every 6 hours for 24 hours, beginning 2 hours before the procedure. Crying time and physiologic changes (heart and respiratory rates) were monitored throughout the procedure, and a standardized comfort score was used to determine postoperative pain. No significant differences were apparent between the two groups during the intraoperative period and the immediate postoperative period. Infants receiving acetaminophen showed statistically significant improvements in comfort scores 6 hours postoperatively, which implies that acetaminophen may be beneficial after the initial postoperative period.27
Sucrose: The use of sucrose-dipped pacifiers in neonates has been shown to be superior to the use of water-dipped pacifiers for reducing crying during painful procedures (circumcision and heel sticks).18,29,30 Sucrose is less effective than lidocaine-prilocaine cream or DPNB for reducing pain, as determined by changes in heart rate, oxygen saturation, and blood pressure.18,31 However, the combination of sucrose and lidocaine-prilocaine cream has been shown to be more effective than either agent alone for relieving neonatal pain associated with circumcision.18
Complications
The complication rate for circumcision reported in the literature varies, but is generally between 2% and 5%. The most common complication is bleeding, with a reported incidence of around 1%. Direct pressure to the site is sufficient to control bleeding in most patients.32 Occasionally, the use of thrombin, epinephrine, or sutures may be required. Infection may occur, but with less frequency than bleeding, and can be successfully treated with oral antibiotics and local wound care. The most serious long-term complication is the inability to retract the remaining foreskin, which results in phimosis. This may be treated with topical steroids; however, surgical revision is usually required. Less common complications include skin bridges, inclusion cysts, fistulas, glans injury, and penile-sensation deficits.33
Conclusion
Ultimately, the decision regarding neonatal circumcision is to be made by the child’s parents. The benefits and risks of the procedure should be explained to the parents in an unbiased fashion, thereby allowing them the opportunity to make the best decision for their child. If circumcision is performed, combination analgesic therapy should be provided for the most effective pain relief. Ring block and DPNB are superior to lidocaine-prilocaine cream and lidocaine cream for reducing pain during the procedure. In addition to an anesthetic, a sucrose-dipped pacifier can help soothe the neonate during circumcision, and acetaminophen has shown benefit for relieving postoperative pain.
REFERENCES
1. American Academy of Pediatrics Task Force on Circumcision. Circumcision policy statement. Pediatrics. 1999;103:686-693.
2. Lerman SE, Liao JC. Neonatal circumcision. Pediatr Clin North Am. 2001;48:1539-1557.
3. Howard CR, Howard FM, Garfunkel LC, et al. Neonatal circumcision and pain relief: current training practices. Pediatrics. 1998;101:423-428.
4. CDC. Trends in in-hospital newborn male circumcision—United States, 1999-2010. MMWR Morb Mortal Wkly Rep. 2011;60:1167-1168.
5. Alanis MC, Lucidi RS. Neonatal circumcision: a review of the world’s oldest and most controversial operation. Obstet Gynecol Surv. 2004;59:379-395.
6. World Health Organization (WHO) and Joint United Nations Programme on HIV/AIDS. Male Circumcision: Global Trends and Determinants of Prevalence, Safety and Acceptability. Geneva, Switzerland: WHO; 2007.
7. Ginsburg CM, McCracken GH Jr. Urinary tract infections in young infants. Pediatrics. 1982;69:409-412.
8. Schoen EJ, Colby CJ, Ray GT. Newborn circumcision decreases
incidence and costs of urinary tract infections during the first year of
life. Pediatrics. 2000;105:789-793.
9. Szabo R, Short RV. How does male circumcision protect against HIV infection? BMJ. 2000;320:1592-1594.
10. Moses S, Plummer FA, Bradley JE, et al. The association between
lack of male circumcision and risk for HIV infection: a review of the
epidemiological data. Sex Transm Dis. 1994;21:201-210.
11. Cook LS, Koutsky LA, Holmes KK. Circumcision and sexually transmitted diseases. Am J Public Health. 1994;84:197-201.
12. Maden C, Sherman KJ, Beckmann AM, et al. History of circumcision,
medical conditions, and sexual activity and risk of penile cancer. J Natl Cancer Inst. 1993;85:19-24.
13. Wan J. GOMCO circumcision clamp: an enduring and unexpected success. Urology. 2002;59:790-794.
14. Kurtis PS, DeSilva HN, Bernstein BA, et al. A comparison of the
Mogen and Gomco clamps in combination with dorsal penile nerve block in
minimizing the pain of neonatal circumcision. Pediatrics. 1999;103:e23.
15. Taeusch HW, Martinez AM, Partridge JC, et al. Pain during Mogen or PlastiBell circumcision. J Perinatol. 2002;22:214-218.
16. American Academy of Pediatrics, Canadian Paediatric Society. Prevention and management of pain and stress in the neonate. Pediatrics. 2000;105:454-461.
17. Taddio A. Pain management for neonatal circumcision. Paediatr Drugs. 2001;3:101-111.
18. Mohan CG, Risucci DA, Casimir M, et al. Comparison of analgesics in ameliorating the pain of circumcision. J Perinatol. 1998;18:13-19.
19. Benini F, Johnson CC, Faucher D, Aranda JV. Topical anesthesia during circumcision in newborn infants. JAMA. 1993;270:850-853.
20. Taddio A, Stevens B, Craig K, et al. Efficacy and safety of lidocaine-prilocaine cream for pain during circumcision. N Engl J Med. 1997;336:1197-1201.
21. Woodman PJ. Topical lidocaine-prilocaine versus lidocaine for neonatal circumcision: a randomized controlled trial. Obstet Gynecol. 1999;93:775-779.
22. Butler-O’Hara M, LeMoine C, Guillet R. Analgesia for neonatal
circumcision: a randomized controlled trial of EMLA cream versus dorsal
penile nerve block. Pediatrics. 1998;101:e5.
23. Lander J, Brady-Fryer B, Metcalfe JB, et al. Comparison of ring
block, dorsal penile nerve block, and topical anesthesia for neonatal
circumcision: a randomized controlled trial. JAMA. 1997;278:2157-2162.
24. Weatherstone KB, Rasmussen LB, Erenberg A, et al. Safety and efficacy of a topical anesthetic for neonatal circumcision. Pediatrics. 1993;92:710-714.
25. Williamson PS, Williamson ML. Physiologic stress reduction by a local anesthetic during newborn circumcision. Pediatrics. 1983;71:36-40.
26. Garry DJ, Swoboda E, Elimian A, Figueroa R. A video study of pain relief during newborn male circumcision. J Perinatol. 2006;26:106-110.
27. Howard CR, Howard FM, Weitzman ML. Acetaminophen analgesia in neonatal circumcision: the effect on pain. Pediatrics. 1994;93:641-646.
28. Kirya C, Werthmann MW Jr. Neonatal circumcision and penile dorsal nerve block—a painless procedure. J Pediatr. 1978;92:998-1000.
29. Blass EM, Hoffmeyer LB. Sucrose as an analgesic for newborn infants. Pediatrics. 1991;87:215-218.
30. Kaufman GE, Cimo S, Miller LW, Blass EM. An evaluation of the
effects of sucrose on neonatal pain with 2 commonly used circumcision
methods. Am J Obstet Gynecol. 2002;186:564-568.
31. Herschel M, Khoshnood, Ellman C, et al. Neonatal circumcision. Randomized trial of a sucrose pacifier for pain control. Arch Pediatr Adolesc Med. 1998;152:279-284.
32. Weiss HA, Larke N, Halperin D, Schenker I. Complications of
circumcision in male neonates, infants and children: a systematic
review. BMC Urol. 2010;10:2.
33. Malone P, Steinbrecher H. Medical aspects of male circumcision. BMJ. 2007;335:1206-1209.
34. Lehr VT, Cepeda E, Frattarelli DA, et al. Lidocaine 4% cream
compared with lidocaine 2.5% and prilocaine 2.5% or dorsal penile block
for circumcision. Am J Perinatol. 2005;22:231-237.
To comment on this article, contact rdavidson@uspharmacist.com.





