US Pharm. 2010;35(7):31-37.
It is predicted that by 2020, chronic obstructive pulmonary disease (COPD) will become the third most common cause of death in the world.1 Yet currently, there are only a number of treatment modalities that have demonstrated long-term improvement of lung function.2 These include smoking cessation, oxygen supplementation in hypoxic patients, and lung volume reduction surgery in emphysemic patients. Inhaled bronchodilators and corticosteroids are the mainstay of COPD treatment; however, their efficacy is limited to preventing exacerbations and alleviating symptoms. Considering the current trajectory of COPD mortality and morbidity, it is imperative that we seek pharmacologic options that may play a role in reducing the burden of COPD. Presently, the data in regard to improving outcomes are especially encouraging with combination therapies.
This article will examine the evidence supporting the use of combination therapy of beta agonists with muscarinic antagonists and/or corticosteroids. The data supporting the use of tiotropium as the muscarinic agent of choice will also be highlighted, although no commercially made tiotropium/beta agonist fixed-combination product is available. This is due to the shorter duration of activity of currently available beta agonists, which are dosed every 4 to 12 hours, whereas tiotropium is dosed once daily.2
Pharmacologic Rationale for Combination Therapy
The use of combination products that contain agents with different mechanisms of action allows targeting of more than one pathophysiologic pathway. According to the Global Initiative for Chronic Obstructive Lung Diseases (GOLD) guidelines, the definition of COPD is “a preventable and treatable disease with some extrapulmonary effects that may contribute to the severity in individual patients. Its pulmonary component is characterized by airflow limitation that is not fully reversible. The airflow limitation is usually progressive and associated with an abnormal inflammatory response of the lung to noxious particles or gases.”2 Two key pathophysiologic targets to note from the definition are airflow limitation and inflammation, which can be treated with bronchodilators and corticosteroids, respectively.
Airway contractility depends on both the parasympathetic and sympathetic nervous systems. Specific inhalers have been produced to target these systems, including short-acting beta agonists (SABAs; albuterol and salbutamol) and long-acting beta agonists (LABAs; salmeterol and formoterol) to act on adrenergic receptors; and short-acting muscarinic antagonists (SAMAs; ipratropium) and long-acting muscarinic antagonists (LAMAs; tiotropium) to block cholinergic receptors. The activation of various muscarinic receptors by acetylcholine causes airway constriction via the parasympathetic system. Conversely, activation of sympathetic beta2 receptors will lead to airway relaxation, allowing both muscarinic inhibition and beta agonists to be targets of COPD treatment. A significant amount of animal data support cross-activity of acetylcholine on the sympathetic system and adrenergic catecholamines on the parasympathetic (acetylcholine neurotransmission) system. Therefore, it has been hypothesized that combination therapy may be a way of optimizing both muscarinic and adrenergic targets versus using only individual agents.3
Besides adrenergic and muscarinic targets, inflammation also plays a role in the pathology of COPD. Patients with COPD have infiltration of T cells, macrophages, and neutrophils within the airway mucosa and lung parenchyma. Unfortunately, the effects of corticosteroids on the inflammatory pathway of COPD are minimal. Studies using corticosteroid therapy alone have shown that they have little effect on inflammatory markers in the sputum.4 However, in combination, corticosteroids may increase the number of beta2 adrenoceptors, while beta2 agonists may induce glucocorticoid receptor (GR) nuclear translocation.5 Therefore, corticosteroid combination therapy may exhibit synergistic pharmacologic properties that anticholinergic beta-agonist combination therapies demonstrate.
Lastly, there are a number of differences in properties within the drug classes to be noted when selecting agents. The most clinically relevant difference is the affinity to target receptors. The higher the affinity, the longer the duration; therefore, there is a decreased need for multiple doses. For example, tiotropium (a LAMA) has a much higher affinity for and slower dissociation time from muscarinic receptors than ipratropium (a SAMA), and thus may be dosed once a day. Of note, ipratropium is not recommended for use with tiotropium, whereas SABAs and LABAs may be used concomitantly. Another example of differences within classes is seen with formoterol and salmeterol (both LABAs). Formoterol has a faster onset of action and a greater peak bronchodilatory effect than salmeterol. This may be a result of formoterol’s higher selectivity for the beta2 receptor and lower lipophilicity.6 Whether these pharmacologic differences of LABAs translate into clinical outcomes has yet to be seen.

Current GOLD Guidelines
Updated in 2009, the GOLD guidelines recommend a stepwise approach (TABLE 1) to treat patients based on severity of symptoms and airflow limitation as measured by forced expiratory volume in one second (FEV1).2 (Spirometry values are further explained in FIGURE 1.7) Patients who fall into stage I (mild) should first be advised to quit smoking, which is the most clinically effective and cost-effective intervention to reduce the rates of COPD and halt its progression.2 In addition to advising smoking cessation, the clinician should also educate patients on the importance of reducing occupational exposure to indoor and outdoor air pollution and other environment irritants, which may exacerbate symptoms and worsen the disease state. Lastly, patients should receive annual influenza vaccinations, as they have been demonstrated to reduce morbidity and mortality by as much as 50%.2 Patients 65 years of age or older should also receive the pneumococcal polysaccharide vaccine, although the data regarding the utility of pneumococcal vaccination have been conflicting.2
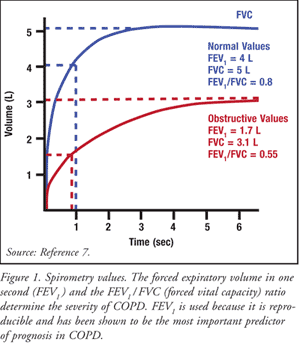
As the disease progresses, it is inevitable that patients will require more than one agent to control their symptoms. In all stages of COPD, the patient begins the stepwise treatment with a short-acting bronchodilator (i.e., albuterol). Then as lung function declines, longer-acting agents like formoterol or tiotropium are added. Once the patient’s FEV1 falls below 50%, an inhaled corticosteroid can be introduced.2 The following section will delve deeper into the specific combinations that are used in stages II (moderate) and III (severe).
Efficacy Studies of Combination Pharmacologic Management
Numerous studies have tried to establish the efficacy of combination therapy in COPD. Unfortunately, many of the studies do not maintain rigorous trial design, lack congruity in study design, have differing definitions of outcomes, or provide conflicting results. Another common issue is the difficulty in assessing mortality in studies that may last for only a matter of months. Therefore, the data to support pharmacologic management are currently limited to decreasing exacerbations and improving symptoms and quality of life. Now a number of these studies will be presented to see how data have built upon each other to arrive at current practices. TABLE 2 contains combination products that are FDA approved for use in COPD.2
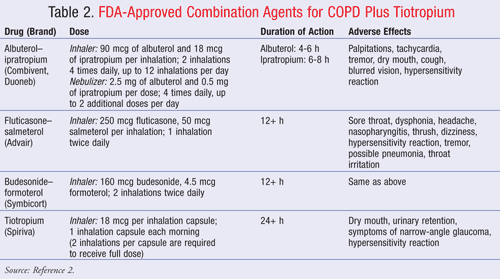
Combination Therapy of Short-Acting Bronchodilators (SABAs and SAMAs): SABAs like albuterol are used for symptomatic relief across all stages of COPD, but short-acting agents do not provide optimal lung function improvement as monotherapy. Based on the pharmacologic rationale described above, the combination of albuterol with ipratropium (available as Combivent or Duoneb; see TABLE 2) has been studied against albuterol monotherapy and ipratropium monotherapy. Multiple studies have shown that in combination, the two short-acting bronchodilators, as metered-dose inhaler (MDI) or nebulizer, were better at improving FEV1 and decreasing exacerbations than each of the monotherapies separately.6,8-11
Combination Therapy of LABAs With SAMAs: When LABAs were introduced to the market, they offered prescribers therapeutic drugs that allowed for 12-hour dosing as opposed to 4- to 6-hour dosing (i.e., albuterol). Decreasing the number of administered doses alleviates the patient’s burden and increases the treatment’s efficiency.3,12 A 12-week study comparing salmeterol 50 mcg twice daily plus ipratropium 40 mcg four times daily to salmeterol alone, found that the combination was much more effective in improving FEV1 and airway conductance.13 Another study confirmed the improvement of FEV1 when adding salmeterol to existing SAMA therapy.14
The addition of salbutamol (a SABA), 200 mcg four times a day, was compared to the addition of formoterol (a LABA), 12 mcg daily, to ipratropium (a SAMA), 40 mcg four times a day.15 Adding formoterol was found to be more effective than adding salbutamol in terms of lung function, measured by peak expiratory flow rate, FEV1, forced vital capacity (FVC), and symptom scores. Therefore, adding a LABA demonstrates improved outcomes over either not using any LABAs at all or a SABA alone.
Combination Therapy of SABAs or LABAs With Tiotropium: In the same way that LABAs demonstrated better outcomes over SABAs, tiotropium (a LAMA) has also demonstrated more convenience and significantly greater bronchodilation and improvements in symptoms over its shorter-acting counterpart, ipratropium, which must be taken 3 to 4 times daily.16,17
To assess the hypothesis of better outcomes being associated with longer activity, LABAs with tiotropium have also been studied. Current GOLD guidelines advise that one or more long-acting bronchodilators may be added at moderate-to-severe stages.2 Several studies examined the LABA plus tiotropium combination ranging from acute postbronchodilator effects to studies lasting more than one year. In a 12-week study comparing formoterol 12 mcg twice daily plus tiotropium 18 mcg once daily to tiotropium monotherapy, the combination significantly increased the FEV1 AUC0-4h compared with tiotropium at all time points (P <.001).18 At the end of the study, increases from baseline in trough FEV1 and FVC were significantly greater with the combination treatment than with tiotropium alone. These outcomes were again found in a longer study lasting 6 months using similar treatment arms.19 This study also found that the combination treatment arm had fewer exacerbations, although not reaching statistical significance. Lastly, another study comparing salmeterol-tiotropium versus tiotropium found that the combination improved quality of life scores but did not improve FEV1 or decrease number of exacerbations over tiotropium alone.20 Overall, the outcomes of these studies demonstrate there are a number of added benefits in using combinations over tiotropium alone.
Combination Therapy of Beta Agonists With Inhaled Corticosteroids (ICS): Unlike with asthma, the data regarding ICS have not been as robust with COPD patients. A number of studies have demonstrated no benefit in lung function or mortality, and one meta-analysis showed increased risk of pneumonia with ICS treatment.21-23 Despite the lack of positive data supporting the use of ICS, these same studies also revealed that daily ICS can decrease the number of exacerbations and slow the decline of quality-of-life scores in patients with severe COPD. With this impact being seen with patients with severe COPD (FEV1 <50%), the GOLD guidelines recommend adding ICS in patients with more severe COPD prone to exacerbations.2 Patients with COPD should never be treated with ICS alone.
A number of studies reinforce the benefits of using ICS in combination with a LAMA. These benefits include improvement in FEV1 and quality-of-life scores.24 More recently, the Towards a Revolution in COPD Health (TORCH) study included patients with moderate-to-severe COPD.25 During TORCH, treatment with fluticasone propionate for 3 years was found to reduce the rate of decrease in FEV1 compared with placebo (P <.003).26 There was a 25% reduction in exacerbations with combination therapy compared to placebo, which was also significantly more of a reduction compared to salmeterol alone. The quality-of-life scores were statistically higher in the combination arm. In addition, combination therapy demonstrated a trend towards decreased mortality, but this end point did not reach statistical significance.26
Triple Therapy: Finally, building on all of the previously noted studies, it appears that using a LABA, tiotropium, and ICS may provide the optimal synergistic combination to maximize clinical outcomes. Studies conducted have shown that triple therapy, using LABA-ICS combinations with tiotropium, improves lung function, symptoms, and health status, and reduces the risk of hospitalizations compared with tiotropium alone in patients with moderate-to-severe COPD.27-29
The Canadian Thoracic Society/Canadian Respiratory Clinical Research Consortium conducted a randomized, double-blind, placebo-controlled trial with 449 patients with moderate-to-severe COPD.20 The treatment arms included tiotropium 18 mcg plus placebo, tiotropium 18 mcg plus salmeterol, and tiotropium 18 mcg plus fluticasone-salmeterol (500 mcg/50 mcg). It was found that there was not a significant difference in the percentage of patients experiencing exacerbations, but the combination tiotropium plus fluticasone-salmeterol (Advair) was associated with significant improvement of lung function, quality of life, and reduced number of hospitalizations, compared with tiotropium plus placebo.
Discussion
The burst of new research in the area of COPD over the past several years is warranted, considering it is projected to become the third leading cause of death in the world. There are a number of new agents in the pipeline, including LABAs dosed once daily and other fixed-combination products, that may hold the promise of broader outcomes to include mortality benefits.12 As time passes and more information surfaces, it will become clearer which agents, new or old, in which combination may benefit COPD patients optimally.
Based on the current evidence, there are a number of treatment options that appear to be more efficacious than others. The strongest evidence points to always including smoking cessation information and immunizations when treating patients. The end point in regard to mortality has not yet been met, but the evidence upholds the current GOLD guidelines. Patients should be treated in a stepwise approach and, when agents are added, they should be from a different class of drugs in order to optimize pathophysiologic targets.
REFERENCES
1. Rabe KF, Hurd S, Anzueto A, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med. 2007;176:532-555.
2. Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. Updated December 2009. www.goldcopd.com. Accessed April 16, 2010.
3. Cazzola M, Molimard M. The scientific rationale for combining long-acting beta2-agonists and muscarinic antagonists in COPD. Pulm Pharmacol Ther. 2010;23:257-267.
4. Hattotuwa KL, Gizycki MJ, Ansari TW, et al. The effects of inhaled fluticasone on airway inflammation in chronic obstructive pulmonary disease: a double-blind, placebo-controlled biopsy study. Am J Respir Crit Care Med. 2002;165:1592-1596.
5. Roth M, Johnson PR, Rudiger JJ, et al. Interaction between glucocorticoids and beta2 agonists on bronchial airway smooth muscle cells through synchronised cellular signaling. Lancet. 2002;360:1293-1299.
6. Restrepo RD. A stepwise approach to management of stable COPD with inhaled pharmacotherapy: a review. Respir Care. 2009;54:1058-1081.
7. Thomason MJ, Strachan DP. Which spirometric indices best predict death from chronic obstructive pulmonary disease? Thorax. 2000;55:785-788.
8. Dorinsky PM, Reisner C, Ferguson GT, et al. The combination of ipratropium and albuterol optimizes pulmonary function reversibility testing in patients with COPD. Chest. 1999;115:966-971.
9. COMBIVENT Inhalation Aerosol Study Group. In chronic obstructive pulmonary disease, a combination of ipratropium and albuterol is more effective than either agent alone. An 85-day multicenter trial. Chest. 1994;105:1411-1419.
10. Levin DC, Little KS, Laughlin KR, et al. Addition of anticholinergic solution prolongs bronchodilator effect of beta 2 agonists in patients with chronic obstructive pulmonary disease. Am J Med. 1996;100:40S-48S.
11. Friedman M, Serby CW, Menjoge SS, et al. Pharmacoeconomic evaluation of a combination of ipratropium plus albuterol compared with ipratropium alone and albuterol alone in COPD. Chest. 1999;115:635-641.
12. Welte T. Optimising treatment for COPD—new strategies for combination therapy. Int J Clin Pract. 2009;63:1136-1149.
13. van Noord JA, de Munck DR, Bantje TA, et al. Long-term treatment of chronic obstructive pulmonary disease with salmeterol and the additive effect of ipratropium. Eur Respir J. 2000;15:878-885.
14. Chapman KR, Arvidsson P, Chuchalin AG, et al. The addition of salmeterol 50 mg bid to anticholinergic treatment in patients with COPD: a randomized, placebo controlled trial. Can Respir J. 2002;9:178-185.
15. D’Urzo AD, De Salvo MC, Ramirez-Rivera A, et al. In patients with COPD, treatment with a combination of formoterol and ipratropium is more effective than a combination of salbutamol and ipratropium: a 3-week, randomized, double-blind, within-patient, multicenter study. Chest. 2001;119:1347-1356.
16. Casaburi R, Conoscenti CS. Lung function improvements with once-daily tiotropium in chronic obstructive pulmonary disease. Am J Med. 2004;117(suppl 1):33S-40S.
17. Vincken W, van Noord JA, Greefhorst AP, et al. Improved health outcomes in patients with COPD during 1 yr’s treatment with tiotropium. Eur Respir J. 2002;19:209-216.
18. Tashkin D, Pearle J, Iezzoni D, Varghese ST. Formoterol and tiotropium compared with tiotropium alone for treatment of COPD. COPD. 2009;6:17-25.
19. Vogelmeier C, Kardos P, Harari S, et al. Formoterol mono- and combination therapy with tiotropium in patients with COPD: a 6-month study. Respir Med. 2008;102:1511-1520.
20. Aaron SD, Vandemheen KL, Fergusson D, et al; Canadian Thoracic Society/Canadian Respiratory Clinical Research Consortium. Tiotropium in combination with placebo, salmeterol, or fluticasone-salmeterol for treatment of chronic obstructive pulmonary disease: a randomized trial. Ann Intern Med. 2007;146:545-555.
21. COMBIVENT Inhalation Solution Study Group. Routine nebulized ipratropium and albuterol together are better than either alone in COPD. Chest. 1997;112:1514-1521.
22. Pauwels RA, Lofdahl CG, Laitinen LA, et al. Long-term treatment with inhaled budesonide in persons with mild chronic obstructive pulmonary disease who continue smoking. European Respiratory Society Study on Chronic Obstructive Pulmonary Disease. N Engl J Med. 1999;340:1948-1953.
23. Burge PS, Calverley PM, Jones PW, et al. Randomised, double blind, placebo controlled study of fluticasone propionate in patients with moderate to severe chronic obstructive pulmonary disease: the ISOLDE trial. BMJ. 2000;320:1297-1303.
24. Chung KF, Caramori G, Adcock IM. Inhaled corticosteroids as combination therapy with beta-adrenergic agonists in airways disease: present and future. Eur J Clin Pharmacol. 2009;65:853-871.
25. Calverley PM, Anderson JA, Celli B, et al; TORCH Investigators. Salmeterol and fluticasone propionate and survival in chronic obstructive pulmonary disease. N Engl J Med. 2007;356:775-789.
26. Celli BR, Thomas NE, Anderson JA, et al. Effect of pharmacotherapy on rate of decline of lung function in chronic obstructive pulmonary disease: results from the TORCH study. Am J Respir Crit Care Med. 2008;178:332-338.
27. Singh D, Brooks J, Hagan G, et al. Superiority of “triple” therapy with salmeterol/fluticasone propionate and tiotropium bromide versus individual components in moderate to severe COPD. Thorax. 2008;63:592-598.
28. Cazzola M, Andò F, Santus P, et al. A pilot study to assess the effects of combining fluticasone propionate/salmeterol and tiotropium on the airflow obstruction of patients with severe-to-very severe COPD. Pulm Pharmacol Ther. 2007;20:556-561.
29. Welte T, Miravitlles M, Hernandez P, et al. Efficacy and tolerability of budesonide/formoterol added to tiotropium in COPD patients. Am J Respir Crit Care Med. 2009;180:741-750.
To comment on this article, contact rdavidson@uspharmacist.com.






