US Pharm. 2010;35(9):50-58.
Iron deficiency anemia (IDA) is the most common nutritional deficiency in the world.1 IDA, which is caused by decreased total body iron content, is characterized by hypochromic, microcytic red blood cells, which are often associated with blood loss.1 Iron intake in the United States is estimated at less than 60% of recommended amounts in toddlers, premenopausal women, and pregnant women. This inadequate intake is sufficient to cause health risks.2
The Healthy People 2010 nutrition and weight status objectives projected a 3% to 4% reduction of IDA in children, women of childbearing potential, and pregnant women.3 The overall goals for reducing IDA in these populations were not met by 2010, so this objective was retained in Healthy People 2020.1,3 IDA is preventable and reversible by increasing iron supplementation or reducing iron loss. Toddlers, premenopausal women, and adolescent girls are at greatest risk for IDA in the U.S. and other developed nations; this may be due to dietary concerns and inadequate prevention strategies and therapeutic approaches.1,4,5
A diagnosis of iron deficiency should be considered when a patient has a history of chronic fatigue or blood loss. After diagnosis, the underlying cause should be assessed and a treatment plan should be developed that includes replacement of iron stores or blood.
Physiology
Iron is distributed in active metabolic and storage pools. Compared with men, women have smaller total body iron stores (2.5 g vs. 3 g) owing to smaller body size, lower androgen levels, and chronic iron loss through menses, pregnancy, and lactation. Two-thirds of total body iron is found circulating in heme, mostly in erythrocyte hemoglobin (Hb); the remaining third is stored in tissues and other cells as ferritin and hemosiderin.5
The body absorbs heme iron (found in meat) more efficiently than nonheme iron (found in plant sources). Dietary nonheme iron must be reduced to the ferrous state and released from food by acidic gastric secretions. Co-ingestion of some foods, such as vegetable fiber, bran, and tea, significantly reduces total absorption of nonheme iron; however, ascorbic acid and citrus juice enhance absorption.5
Adults consuming a typical U.S. diet containing 15 mg of dietary iron absorb only 1 mg of iron. Premenopausal women and adolescent girls have higher daily replacement needs because of menstrual blood loss. Iron absorption increases during periods of depletion, although absorption rarely increases to more than 6 mg/day unless supplemental iron is added.5
Diagnosis
IDA is suspected in patients who have microcytic anemia. The normal serum iron level for women is 60 mcg/dL to 140 mcg/dL. Total iron-binding capacity is 250 mcg/dL to 450 mcg/dL. Patients taking oral iron may have normal serum iron despite a total body iron deficiency; in such circumstances, a valid test requires cessation of iron therapy for 24 to 48 hours before serum values are measured.6
Serum ferritin concentration closely correlates with total body iron stores. The range of normal ferritin in most laboratories is 30 ng/mL to 300 ng/mL, and the mean is 49 ng/mL in women. The National Health and Nutrition Examination Survey describes iron deficiency in women as a low concentration of ferritin (<12 ng/mL).1
Diagnosis prompts consideration of the cause of IDA (usually, bleeding). Women with obvious blood loss--menses--may require no further testing. Postmenopausal women without obvious blood loss should have the gastrointestinal (GI) tract evaluated because anemia may be the only indication of an occult GI cancer.6
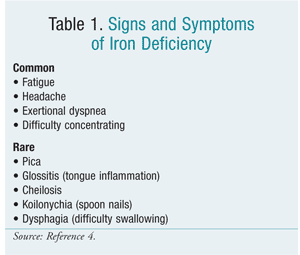
Patients with IDA may not exhibit symptoms until their iron stores are severely depleted. Anemia patients may complain of fatigue upon limited exertion, headaches, shortness of breath, or difficulty concentrating.6 See TABLE 1 for a list of signs and symptoms.
Causes of Iron Deficiency
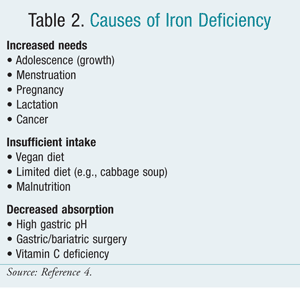
The daily iron requirement for adolescent girls and premenopausal women is approximately 20 mg elemental iron. However, this amount often is not attained because absorption from dietary sources is limited by the absorptive capacity of the intestine. Iron deficiency occurs readily owing to regular iron losses, increased requirements, or decreased intake. In premenopausal women, cumulative menstrual blood loss is a common cause. Vitamin C deficiency can contribute to IDA by producing capillary fragility, hemolysis, and bleeding.7 TABLE 2 lists causes of iron deficiency.
Vegan Diet: Women who do not consume animal protein are thought to be at greater risk for IDA owing to the ingestion of solely nonheme dietary iron and the increased intake of iron-absorption inhibitors (phytates, tannins, fiber). Main dietary sources of iron for vegans are cereals, dried beans, vegetables, and dried fruits. Haddad and colleagues studied a small group of established vegans and nonvegetarians and their intakes of various nutrients and measured hematologic and other biochemical markers for differences.7 Iron intake from food and supplements was similar between the groups. Vegan women had a higher intake of ascorbic acid, which enhances iron absorption. Vegan and nonvegetarian women did not differ in any hematologic markers, including Hb, hematocrit, and ferritin. A similar number of women in both groups had ferritin levels below 12 mcg/L, suggesting that supplementation may be necessary regardless of diet. The German Vegan Study suggests that vegan women ingest iron in sufficient quantities, but it found that women younger than 50 years had low serum ferritin concentrations (14 ng/mL) compared with older women (28 ng/mL).8 The authors suggest an iron supplement for younger vegan women to increase iron exposure and to offset diminished absorption and increased loss.8
Bariatric Surgery: Iron deficiency with or without anemia is higher in patients undergoing bariatric surgery (30%-40%), especially when the patient is premenopausal.9 Diminished erythropoietic response from inflammation, blood loss from surgery, reduced intake of meat, and postoperative iron and B12 malabsorption may further increase the risk of IDA in bariatric surgery patients. Assessment and treatment of reduced iron stores optimally should occur prior to surgery. Oral iron supplementation should be administered for a sufficient duration and dosage to replenish body stores to normal levels. Owing to the diminished erythropoietic response and diminished GI absorption in some chronically obese patients, erythropoiesis-stimulating agents may be administered if oral iron given over several weeks fails to increase Hb or other hematopoietic markers.10 IV iron replacement has been reported to be effective for raising Hb in postoperative bariatric surgery patients with reduced iron stores.9,11,12 Mechanick and colleagues recommend a daily intake of 40 mg to 65 mg elemental iron with vitamin C for patients with malabsorptive or combination-type bariatric procedures, followed by continued monitoring of iron and ferritin levels to allow for adjustment of dose or route.12
Drug Interactions: The use of proton pump inhibitors (PPIs) has increased in recent years, especially since they are available without a prescription.13 Hydrochloric acid in the stomach dissociates nonheme iron salts from food; the solubilized iron salts are then reduced to the ferrous form, which is more easily absorbed. Long-term use of PPIs may decrease available iron in the diet, owing to changes in stomach acidity. Prolonged omeprazole treatment has not been shown to reduce iron stores in patients with a normal diet.13 There is some controversy as to the malabsorption of oral iron replacement with PPI use in cases of existing iron deficiency.13,14 Sharma and colleagues reported on two women with IDA with diminished response to oral iron-replacement therapy, both of whom responded to oral iron replacement after omeprazole was discontinued.14
Concurrent use of dairy products, cholestyramine, or antacids containing calcium, aluminum or magnesium decreases iron absorption. Patients should take iron supplements at least 2 hours before or after consuming these products.11
Adolescence: Girls aged 15 to 18 years need additional iron for increasing lean tissue, increasing blood volume, and replacing menstrual blood loss. Their iron requirement may be twice as much as that of an adult woman.15 In adolescence, obesity may be related to increased iron deficiency. Pinhas-Hamiel and colleagues observed that 39% of obese (body-mass index [BMI] >97th percentile) children aged 10 to 18 years and 12% of overweight children (BMI 85th-97th percentile) had iron deficiency, as measured by lower serum iron levels, compared with their healthy-weight counterparts (4.4%).16
Pregnancy: In pregnancy, red blood cell volume increases by 30% and peaks in the mid third trimester. The developing fetus requires iron for growth and blood production, and these extra iron needs may increase to as much as 1,000 mg elemental iron daily during the pregnancy. The consequences of IDA during pregnancy include diminished intellectual and productive capacity and increased susceptibility to infection. A Cochrane Review of iron supplementation during pregnancy suggests that second- and third-trimester Hb levels below 95 g/L may be associated with inadequate pregnancy weight gain, low birthweight (LBW), and premature delivery.17 If anemia is present, the recommended daily dose of elemental iron ranges from 30 mg to 120 mg. Some newer findings suggest that weekly administration of iron may be sufficient to improve iron utilization, increase compliance, and reduce the side effects of daily dosing.18 There is insufficient evidence to promote provision of routine iron supplementation for nonanemic pregnant women.17
Soares and colleagues compared iron stores and prevalence of IDA in nulliparous adolescent girls (n = 61) and adult (n = 122) women during pregnancy and postpartum.18 All participants received iron supplementation of 40 mg/day with folic acid. Transferrin saturation index and mean ferritin levels were lower in adolescents (aged 10-19 years) in late pregnancy and prior to delivery, compared with adults. Iron deficiency was less frequent in adults. This may be due to reduced iron stores prior to pregnancy in the adolescent population.
Lactation: The amount of iron excreted in breast milk is not thought to be dependent on the iron status of the mother. Women are encouraged to continue prenatal vitamins with iron while breastfeeding. Preterm infants, LBW infants, infants with hematologic disorders, and those with inadequate iron stores at birth generally require iron supplementation before 6 months of age. Term breastfed infants with no underlying conditions should be given iron-supplemented foods starting at 6 months of age.19
Maintaining Healthy Iron Stores
A varied diet adequate in iron is recommended for everyone. Individuals who do not consume animal protein should be encouraged to eat foods with a higher iron content--dark leafy vegetables; dried beans; nuts; prunes, raisins, and dried figs; enriched cereals; whole grains--in combination with citrus juice or other ascorbic acid-rich foods to enhance absorption. Iron absorption is reduced with concurrent intake of tea, fiber, and calcium-rich foods.8
Replacing Iron Stores
Oral: If diet alone is insufficient to maintain iron stores and the patient is exhibiting signs and laboratory values consistent with iron deficiency with or without anemia, an oral iron supplement may be recommended. If the iron deficiency is caused by an underlying disease or GI bleeding, the cause should be addressed.16,18
Oral iron supplements are available as ferrous salts--fumarate, gluconate, glutamate, lactate, succinate, and sulfate--in tablet or liquid form. These different types of iron salts are absorbed in a similar manner. Dosing should be conveyed as milligrams of elemental iron to reduce confusion between salt forms. To deliver 18 mg of iron per day across the intestinal wall (at 10% absorption), a typical replacement dose for a person with IDA would be 60 mg elemental iron three times a day. A 325-mg tablet of ferrous sulfate contains 65 mg elemental iron; a 300-mg tablet of ferrous gluconate contains 36 mg of elemental iron, requiring twice the number of tablets to equal the same dose.4,5
Tablet formulations of iron are nonenteric-coated or enteric-coated and immediate-release or extended-release. Enteric-coated and extended-release tablets are better tolerated and should be released in the duodenum to be absorbed effectively. Iron released in the stomach is not tolerated as well. If iron is released below the duodenum, there is less absorption and treatment will be ineffective. Trying a nonenteric-coated product and retesting for serum iron markers would be the next step if enteric-coated, extended-release tablets do not raise iron stores sufficiently.4
Parenteral: Parenteral iron may be given when oral iron therapy has failed because of malabsorption or severe intolerance to oral products. Currently available parenteral iron products in the U.S. include iron dextran, sodium ferric gluconate, and iron sucrose. These products differ in molecular size, bioavailability, side-effect profile, and cost. The main concerns with parenteral iron are its potential to overload the body's iron-binding capacity and the potential for free iron reactions leading to systemic immune dysfunction.9
Patients should be monitored 5 to 10 days after iron replacement is initiated to observe response to any supplement. After response is documented, iron status should be monitored to ensure compliance with the therapy regimen and to determine whether normal iron values have been restored. Iron therapy needs to be continued until total body stores are replenished.9
Potential Side Effects of Iron Therapy
Oral iron in doses prescribed to treat IDA has been associated with GI side effects such as nausea, vomiting, constipation, diarrhea, dark-colored stools, and abdominal distress. Liquid iron preparations may stain the teeth.20
Parenteral iron administration may cause blood-pressure changes, flushing, headache, peripheral edema, nausea, muscle cramps, staining of the skin at an intramuscular injection site, or dyspnea.20
Conclusion
IDA in adolescent girls and premenopausal women is associated with the loss of iron via menses, pregnancy, and lactation. Dietary habits or bariatric surgery may place some women at high risk for IDA. Postmenopausal women usually have the same risk as similarly aged men.
Patients should be reminded that an acidic gastric environment is optimal for absorption. Absorption will be inhibited with concomitant use of antacids, histamine-2 blockers, PPIs, dairy products, and cholestyramine. Some products with minerals--calcium, magnesium, phosphate--also may decrease iron absorption. Iron supplements should be taken between meals or at bedtime with citrus juice to enhance absorption.
REFERENCES
1. Looker AC, Cogswell ME, Gunther EW. Iron deficiency--United States, 1999-2000. MMWR Weekly. 2002;51:897-899.
2. Kennedy E, Meyers L. Dietary Reference Intakes: development and uses for assessment of micronutrient status of women--a global perspective. Am J Clin Nutr. 2005;81:1194S-1197S.
3. Health and Human Services. Healthy People 2020: nutrition and weight status. NWS HP2020-3 and -4.
www.healthypeople.gov/hp2020/
4. Alleyne M, Horne MK, Miller JL. Individualized treatment for iron-deficiency anemia in adults. Am J Med. 2008;121:943-948.
5. Zimmermann MB, Hurrell RF. Nutritional iron deficiency. Lancet. 2007;370:511-520.
6. Tefferi A. Anemia in adults: a contemporary approach to diagnosis. Mayo Clin Proc. 2003;78:1274-1280.
7. Haddad EH, Berk LS, Kettering JD, et al. Dietary intake and biochemical, hematologic, and immune status of vegans compared with nonvegetarians. Am J Clin Nutr. 1999;70:586S-593S.
8. Waldmann A, Koschizke JW, Leitzmann C, Hahn A. Dietary iron intake and iron status of German female vegans: results of the German Vegan Study. Ann Nutr Metab. 2004;48:103-108.
9. Muñoz M, Botella-Romero F, Gómez-Ramírez S, et al. Iron deficiency and anaemia in bariatric surgical patients: causes, diagnosis and proper management. Nutr Hosp. 2009;24:640-654.
10. Péneau S, Dauchet L, Vergnaud AC, et al. Relationship between iron status and dietary fruit and vegetables based on their vitamin C and fiber content. Am J Clin Nutr. 2008;87:1298-1305.
11. Zhu A, Kaneshiro M, Kaunitz JD. Evaluation and treatment of iron deficiency anemia: a gastroenterological perspective. Dig Dis Sci. 2010;55:548-559.
12. Mechanick JI, Kushner RF, Sugerman HJ, et al. American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & Bariatric Surgery medical guidelines for clinical practice for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric patient. Endocr Pract. 2008;14(suppl 1):1-83.
13. Jensen RT. Consequences of long-term proton pump blockade: insights for studies of patients with gastrinomas. Basic Clin Pharmacol Toxicol. 2006;98:4-19.
14. Sharma VR, Brannon MA, Carloss EA. Effect of omeprazole on oral iron replacement in patients with iron deficiency anemia. South Med J. 2004;97:887-889.
15. Beard JL. Iron requirements in adolescent females. J Nutr. 2000;130:440S-442S.
16. Pinhas-Hamiel O, Newfield RS, Koren I, et al. Greater prevalence of iron deficiency in overweight and obese children and adolescents. Int J Obes Relat Metab Disord. 2003;27:416-418.
17. Peña-Rosas JP, Viteri FE. Effects and safety of preventive oral iron or iron+folic acid supplementation for women during pregnancy. Cochrane Database Syst Rev. 2009;(4):CD004736.
18. Soares NN, Mattar R, Camano L, Torloni MR. Iron deficiency anemia and iron stores in adult and adolescent women in pregnancy. Acta Obstet Gynecol Scand. 2010;89:343-349.
19. Gartner LM, Morton J, Lawrence RA, et al. Breastfeeding and the use of human milk. Pediatrics. 2005;115:496-506.
20. Lexi-Drugs Online [subscription required].
http://online.lexi.com/crlsql/
To comment on this article, contact
rdavidson@uspharmacist.com.





