US Pharm. 2011;36(4):29-34.
Conjunctivitis, or inflammation of the conjunctiva, is commonly referred to as “pink eye” or “red eye.”1,2 Although the actual incidence is unknown, the condition is one of the most frequent causes of patient self-referral.3
The conjunctiva is a thin tissue extending from the limbus of the eye to the eyelid margin. The three parts of the conjunctiva are the bulbar conjunctiva (covering the anterior portion of the sclera), the palpebral, or tarsal, conjunctiva (lining the inner surface of the eyelid), and the conjunctival sac (space bounded by the bulbar and tarsal conjunctivae). The conjunctiva contains mast cells (MCs) and other inflammatory cells.4
Conjunctivitis may be caused by one or more of several factors. Allergens, irritants, mechanical abrasions, bacteria, and viruses all can cause inflammation of the conjunctiva; for appropriate treatment, it is important that the etiologic agent be identified.1,5 Most cases of conjunctivitis are self-limited, and the condition rarely causes permanent vision loss or structural damage.3 This article will discuss three common classes of conjunctivitis: allergic, viral, and bacterial.
ALLERGIC CONJUNCTIVITIS
About 40% of the general population experiences allergic conjunctivitis (AC), and 80% of these patients have concurrent allergic rhinitis.4,6 AC is associated with type 1 hypersensitivity reactions, and there are generally four types: seasonal and perennial AC (SAC, PAC), vernal conjunctivitis, atopic conjunctivitis, and giant papillary conjunctivitis (GPC).3,7
SAC and PAC
SAC and PAC constitute the majority of AC cases, with SAC comprising more than half.4,7 SAC, which is recurrent, is caused by exposure to ragweed, pollen, or other seasonal allergens.2,4 Patients with PAC exhibit symptoms year round, and the most common triggers are mold spores, animal dander, dust mites, and feathers.4 SAC tends to be worse in warm, dry weather and to lessen with rain and cool temperatures.4 SAC and PAC usually have bilateral involvement (the severity of each eye may differ) and result in little to no sequelae.3,4
Signs and symptoms include watery discharge, chemosis (edema of the conjunctiva), conjunctival injection (dilation of the conjunctival vessels), hyperemia, pruritus, eyelid edema, and ropy mucous discharge.2-4,8 The patient may also experience photophobia.4,7 “Allergic shiners” (dark circles under the eyes) may be present.4 Commonly, the patient has concurrent signs and symptoms of asthma and/or rhinitis.4,7 The absence of itching rules out AC.7
Treatment involves palliative measures and medication therapy. Nonpharmacologic measures include saline irrigation, cold compresses, avoiding allergens, avoiding eye rubbing, and using preservative-free artificial tear solution.3,7-9 The patient should be instructed to keep the artificial tear solution in the refrigerator, because the use of cold product causes vasoconstriction. Artificial tears have a dual function: They flush and dilute allergens, and also form a barrier to prevent allergens from coming in contact with the conjunctiva.9 SAC patients should stay indoors with the windows closed when the pollen count is high; they should not cut grass on windy days and when the pollen count is high. Pets should be kept out of the bedroom, and the bathroom should be kept clean and dry to inhibit mold growth.9
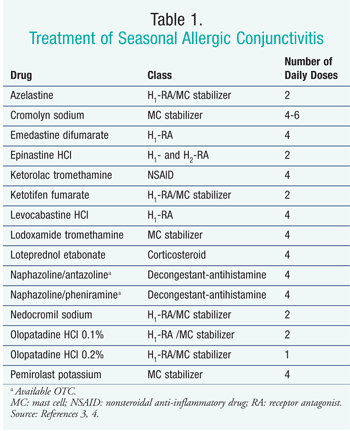
There are several pharmacologic agents for the treatment of AC. For mild SAC or PAC, topical OTC antihistamine-vasoconstrictor combination agents may be used; however, second-generation topical H1-receptor antagonists are more effective. With persistent or recurrent conditions, an MC stabilizer may be used. A topical low-potency corticosteroid may be used for 1 to 2 weeks if symptoms remain uncontrolled with use of an antihistamine and an MC stabilizer.3 Corticosteroid use increases the risk of the development of cataracts or glaucoma. Patients using corticosteroids should be closely monitored.7 There is an FDA-approved topical formulation of ketorolac for pruritus. An oral antihistamine may be used in conjunction with topical agents.3 TABLE 1 lists the agents used to treat AC.3,4
Antihistamines: Antihistamines block the H1 receptor. Systemic use may only partially relieve allergic symptoms. Topical antihistamine/decongestant combination ophthalmic solution is more efficacious for relieving ocular symptoms.6 Second-generation oral antihistamines (e.g., cetirizine) cause less sedation. The antihistamine is effective for acute onset and reduces pruritus, while the decongestant reduces chemosis, eyelid edema, and redness via vasoconstriction.9
MC Stabilizers: MC stabilizers prevent the degranulation of MCs. They are unsuitable for an acute reaction because they have no effect on the histamine that has already been released.9 They may be used for prophylaxis and maintenance of mild-to-moderate symptoms.4,9 MC stabilizers also provide relief of nasal symptoms because of drainage from the nasal passages into the lacrimal duct.4
Ketorolac Tromethamine: Topical ketorolac is a nonsteroidal anti-inflammatory drug used for relief of pruritus.4 Appropriate for the acute phase of AC, ketorolac does not mask ocular infections or cause increased intraocular pressure and cataract formation.9 Ketorolac may sting or burn when initially instilled, but this may be alleviated by refrigerating the solution before use.4,9
Corticosteroids: Corticosteroids are reserved only for severe symptoms, as they can cause increased intraocular pressure, cataract formation, and corneal infection.4 Suitable for the acute and late phases, corticosteroids are used for hyperacute onset, for severe symptoms, or when the condition is refractory to other medications. Pulse dosing of a topical solution may be employed, followed by maintenance with an MC stabilizer.9 Corticosteroids should not be used for longer than 1 to 2 weeks, and the patient should be medically monitored, preferably by an ophthalmologist. Patients should never be given unlimited refills.4
Two commonly used topical ophthalmologic corticosteroid solutions are fluorometholone and loteprednol. Fluorometholone is highly effective in AC. It penetrates the cornea, but is inactivated in the anterior chamber; therefore, it is less likely to cause increased intraocular pressure and cataract formation.4 Likewise, loteprednol is less likely to increase intraocular pressure or cause cataracts; it primarily targets the late phase of the inflammatory process.4,9 It is a safe agent to use when MC stabilizers are inadequate.4
Vernal Conjunctivitis: Vernal conjunctivitis is a serious condition that may result in vision loss. The mechanism is more complex than merely a type 1 hypersensitivity reaction, and it involves other immune mediators also.10 This chronic disease most commonly affects males under 20 years of age, with onset usually occurring in childhood.2,3 Vernal conjunctivitis is characterized by acute exacerbations in the spring and summer.3 Exacerbations gradually decrease over time, with most patients outgrowing the disorder by age 30 years.2,3 The average duration of vernal conjunctivitis is 4 years.2 One-third of patients have multiple atopic conditions, such as asthma or eczema.10
The bulbar and/or tarsal conjunctivae are involved in vernal conjunctivitis, which presents bilaterally. Clinical signs and symptoms include eyelid thickening, ptosis (upper-eyelid paralysis resulting in drooping), conjunctival scarring, corneal neovascularization, ulceration, conjunctival thinning, infection, vision loss, limbal Trantas’ dots (small white dots of degenerating eosinophils and epithelial cell debris), watery and mucous discharge, and keratoconus (conical protrusion of the cornea).2,3,10 The patient may experience foreign-body sensation, pain, and photophobia in the case of corneal involvement.10
Palliative measures may be employed. Nonspecific triggers such as sun, wind, and salt water should be avoided.9 Pharmacologic treatment includes systemic and/or topical antihistamines. Often, a course of pulse dosing of a topical steroid is needed. Severe cases require the addition of an MC stabilizer to the topical steroid. Topical cyclosporine may be substituted for the steroid unless there is corneal involvement.3,7,9 In patients aged 2 years and older, pimecrolimus cream or topical tacrolimus ointment may be applied to the eyelid skin. The patient should take care not to get the medication on the conjunctiva, cornea, or tear film.3
Atopic Conjunctivitis
Atopic conjunctivitis is quite similar to vernal conjunctivitis. The typical patient is male and aged 30 to 50 years.7 Atopic conjunctivitis is a chronic condition with a childhood onset; the patient typically has atopic dermatitis or eczema during childhood and develops ocular symptoms later in life.2,3,7 Like vernal conjunctivitis, this condition presents bilaterally with a similar clinical picture.3,7,9
Mild cases usually respond to palliative measures plus antiallergy medications. Acute cases, no matter how mild, require pulse topical steroid dosing.9 Moderate-to-severe cases require prophylactic antibiotics and topical steroids.3,9 As with vernal conjunctivitis, pimecrolimus cream or tacrolimus ointment may be used. Topical cyclosporine may be used instead of a topical steroid (except in the case of corneal involvement).3,7 Severe cases that are unresponsive to topical therapy may require systemic immunosuppression.3
GPC
GPC is not a true allergic condition; it is chronic inflammation caused by irritation of the tarsal conjunctiva.7,9 Typical causes include contact lens wear (most common), exposed sutures, and ocular prosthesis.2,3 GPC has been associated with the use of hard, soft, and rigid gas permeable contacts.2 The two components of GPC are mechanical irritation and immune hypersensitivity reaction mediated by MCs, eosinophils, and T lymphocytes.9
GPC may present unilaterally or bilaterally, depending on the causative agent. There may be itching, tearing, burning, mucous discharge, giant papillae on the superior tarsal conjunctiva, and conjunctival injection.9 Severe cases may result in eyelid swelling and ptosis.3 Corneal erosion and superficial punctate keratitis may also occur.9 When GPC is associated with contact lens use, there may be increased lens movement with blurry vision upon blinking.2,9
Treatment consists primarily of modifying the causative agent.3,9 For contact lenses, one strategy is to switch from conventional to daily-wear or disposable lenses or from extended overnight-wear to daily-wear lenses.9 Other measures include more frequent lens replacement, decreased lens-wearing time, and use of enzymatic treatments and preservative-free lens care systems. For moderate-to-severe GPC, contact lens use should be discontinued for several weeks to months.3 If pharmacologic therapy is indicated, antihistamines and MC stabilizers may be used. Severe cases may require an MC stabilizer and a topical steroid (loteprednol).3,9 Nedocromil is appropriate for long-term maintenance.9
VIRAL CONJUNCTIVITIS
This is the most common form of conjunctivitis.11 It is far more common than bacterial conjunctivitis.5 The three main viral types are adenovirus, herpes simplex virus (HSV), and herpes zoster (HZ) (varicella-zoster virus).3
Adenoviral Conjunctivitis
This is the most common type of viral conjunctivitis.8 It is self-limited, and improvement usually occurs within 5 to 14 days; however, contagion is possible for up to 14 days after the appearance of symptoms.3,12 Adenoviral conjunctivitis is highly contagious and is spread through direct contact with contaminated hands, medical equipment, pool water, or personal items.12 Patients must take appropriate measures to reduce the risk of spread.3
Adenoviral conjunctivitis may present unilaterally or bilaterally with an acute onset (often sequentially bilateral).3 Frequently, the patient suffers from a concomitant upper respiratory infection. Symptoms include red, itchy eyes with a watery or mucous discharge.13 Severe cases may involve conjunctival scarring, symblepharon (adhesion of eyelids to the eyeball), and subepithelial corneal infiltrates.3,12
Because it is difficult to differentiate adenoviral conjunctivitis from bacterial conjunctivitis, antibiotics are frequently prescribed.5,12 There may also be an opportunistic bacterial infection warranting antibiotic use.5 No antiviral solutions are effective against adenoviruses.1,3 Artificial tears, topical antihistamines, and cold compresses may alleviate symptoms.3,12 Topical corticosteroids may be beneficial, but the patient must be monitored closely.3 If symptoms do not resolve on their own or if there is corneal involvement, the patient should be referred to an ophthalmologist.12
HSV Conjunctivitis
HSV occurs in neonates of infected mothers 1 to 2 weeks after birth; it also may occur in sexual partners of infected individuals.11 Triggers include stress, trauma, infection with another virus, and ultraviolet exposure.3 HSV is the most common cause of blindness from corneal disease in the U.S.2,11 The disease presents unilaterally with bulbar conjunctival injection, watery discharge, epithelial keratitis of the cornea or conjunctiva, stromal keratitis, neovascularization, scarring, thinning, perforation, uveitis, trabeculitis, and vesicular rash or ulceration of the eyelids.3
HSV usually does not require treatment. Symptoms resolve within 4 to 7 days, unless there are complications. To prevent corneal infection, oral or topical antivirals should be used. Trifluridine 1% solution 5 to 8 times daily or oral acyclovir 200 mg to 400 mg 5 times daily may be used; oral valacyclovir 500 mg 2 to 3 times daily or famciclovir 250 mg twice daily are effective also. Vidarabine 3% ointment is another topical antiviral.1 Use of topical antivirals for longer than 2 weeks may result in toxicity. Topical steroids are contraindicated.3
HZ Conjunctivitis
Patients with chickenpox (or people exposed to it) may develop HZ conjunctivitis. The condition is usually self-limited, with symptom resolution within a few days.3
HZ may present unilaterally or bilaterally. Symptoms include bulbar conjunctival injection and watery discharge. Punctate keratitis may result in primary infection. Limbal vesicles may form, especially with primary disease. Vesicle formation may result in necrosis and scarring on the eyelid margins, conjunctiva, and corneal stroma.3
Topical antibiotics are sometimes used to prevent secondary bacterial infections. There are no effective topical antivirals, but immunocompromised patients may be given acyclovir 800 mg 5 times daily for 7 days, valacyclovir 1,000 mg every 8 hours for 7 days, or famciclovir 500 mg 3 times daily for 7 days.3
BACTERIAL CONJUNCTIVITIS
Bacterial conjunctivitis often presents similarly to the viral form. The best way to distinguish between them is by the discharge. Bacterial infection causes a more mucopurulent discharge, and when the patient awakens in the morning, the eyes are often “glued” shut.8,12,13 For neonates, prevention strategies include prophylactic use of erythromycin 0.5% or tetracycline 1%.3
There are three classifications of bacterial conjunctivitis: hyperacute, acute, and chronic.12 Hyperacute infection is often caused by Neisseria gonorrhoeae in sexually active adults.12 There are many pathogens that can cause an acute infection, whereas Chlamydia trachomatis most often causes the chronic condition.13
Gonococcal Conjunctivitis
Gonococcal conjunctivitis can occur in adults and neonates. Symptoms in neonates typically occur before those of chlamydial conjunctivitis (1-7 days after birth), but may be delayed if prophylactic antibiotics have been used.3 Often associated with systemic disease, the condition progresses quickly to a severe purulent infection that may result in eye pain, corneal infection, scarring and/or perforation, septicemia with arthritis, and meningitis, and can lead to blindness.3,11,12 Immediate referral to an ophthalmologist is warranted.12 One or both eyes may be affected.3
Often, patients have systemic disease (sometimes without symptoms); therefore, systemic and topical antibiotics are indicated.3,13
Nongonococcal Conjunctivitis
Nongonococcal conjunctivitis, an acute infection, is the most common form of bacterial conjunctivitis seen in primary care. There are many natural defenses against conjunctival infection, but sometimes bacteria overcome them.2 Staphylococcus aureus is a common pathogen in adults, whereas Streptococcus pneumoniae and Haemophilus influenzae are more common in children.12 Moraxella lacunata may also cause infection.1,2 In infants and children, bacterial otitis media, pharyngitis, or sinusitis may lead to bacterial conjunctivitis, which without treatment may progress to severe infection.3 Direct contact with contaminated hands is the most common means of transmission.12
Infection is often mild and self-limited in adults, but may progress to complications in children. One or both eyes may be affected, with the most common symptoms being bulbar conjunctival injection and mucopurulent discharge. Rarely will mild infection progress to corneal infection and preseptal cellulitis (infection of the eyelid and periorbital tissues).3 When symptoms persist beyond 4 weeks (often with frequent relapses), the condition is considered chronic and the patient must be referred to an ophthalmologist.2,12 S aureus is often the causative agent.2
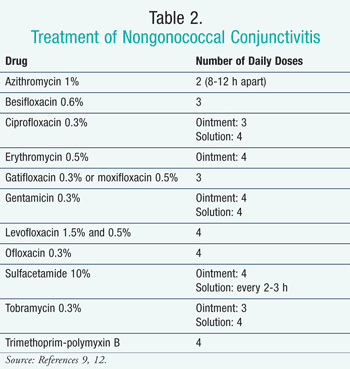
Treatment is empirical, with a topical broad-spectrum antibiotic for 5 to 7 days.1,3 TABLE 2 lists topical antibiotics used for nongonococcal conjunctivitis.9,12
Chlamydial Conjunctivitis
Chlamydial conjunctivitis can affect adults and neonates.3,11 The most common cause of infectious neonatal conjunctivitis, chlamydial conjunctivitis is transmitted from the mother’s genital tract.11 Half of infants are infected at other sites, such as the nasopharynx, genital tract, or lungs.3 In neonates, symptoms appear 5 to 19 days after birth (or earlier, if the placenta ruptures). Untreated, the condition can persist for 3 to 12 months.3
One or both eyes may be affected. Neonatal symptoms include eyelid edema, bulbar conjunctival injection, discharge (purulent or mucopurulent), and lack of follicles. Adults exhibit bulbar conjunctival injection, mucopurulent discharge, corneal pannus (vascularization), punctate epithelial keratitis, preauricular lymphadenopathy, and bulbar conjunctival follicles.3
Since infection is usually systemic, treatment includes both systemic and topical antibiotics.3,13 Erythromycin ophthalmic ointment, along with a single 1-g dose of azithromycin or doxycycline 100 mg twice daily for 14 days, is efficacious.12
CONCLUSION
Conjunctivitis is quite common, and the pharmacist will see many afflicted patients throughout his or her career. The pharmacist is often the first health care professional the patient seeks out, and can be a valuable resource.
Questions about contact lens use, recent upper respiratory infections, exposure to others with conjunctivitis, and use of new eye cosmetics may shed light on the etiology of the condition; however, all conjunctivitis patients should be referred to a physician for treatment.4,11
The pharmacist can facilitate the selection of preservative-free artificial tear solutions, OTC topical antihistamine-decongestant products, contact lens cleaning solutions, and oral OTC antihistamines. The pharmacist also can counsel the patient on palliative measures, refrigerating topical solutions, and modifying contact lens use during treatment.
REFERENCES
1. Henderer JD, Rapuano CJ. Ocular pharmacology. In: Brunton LL, Lazo JS, Parker KL. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 11th ed. New York, NY: McGraw-Hill Medical; 2006:1707-1738.
2. American Optometric Association. Care of the Patient with Conjunctivitis. 2nd ed. St. Louis, MO: American Optometric Association; 2002.
www.aoa.org/documents/CPG-11.
3. American Academy of Ophthalmology. Preferred Practice Pattern. Conjunctivitis. San Francisco, CA: American Academy of Ophthalmology; 2008.
http://one.aao.org/CE/
4. Bielory L, Friedlaender MH. Allergic conjunctivitis. Immunol Allergy Clin N Am. 2008;28:43-58.
5. Visscher KL, Hutnik CM, Thomas M. Evidence-based treatment of acute infective conjunctivitis: breaking the cycle of antibiotic prescribing. Can Fam Physician. 2009;55:1071-1075.
6. Bielory L. Allergic conjunctivitis and the impact of allergic rhinitis. Curr Allergy Asthma Rep. 2010;10:122-134.
7. Ono SJ, Abelson MB. Allergic conjunctivitis: update on pathophysiology and prospects for future treatment. J Allergy Clin Immunol. 2005;115:118-122.
8. Horton JC. Disorders of the eye. In: Fauci AS, Braunwald E, Kasper DL, et al, eds. Harrison’s Principles of Internal Medicine. 17th ed. New York, NY: McGraw-Hill Medical; 2008:180-195.
9. Chigbu DI. The management of allergic eye diseases in primary eye care. Cont Lens Anterior Eye. 2009;32:260-272.
10. Kumar S. Vernal keratoconjunctivitis: a major review. Acta Ophthalmol. 2009;87:133-147.
11. Sethuraman U, Kamat D. The red eye: evaluation and management. Clin Pediatr (Phila). 2009;48:588-600.
12. Cronau H, Kankanala RR, Mauger T. Diagnosis and management of red eye in primary care. Am Fam Physician. 2010;81:137-144.
13. Tarabishy AB, Jeng BH. Bacterial conjunctivitis: a review for internists. Cleve Clin J Med. 2008;75:507-512.
To comment on this article, contact rdavidson@uspharmacist.com.






