US Pharm. 2011;36(6):46-54.
The challenge of developing guidelines for the diagnosis, management, treatment, and prevention of urinary tract infections (UTIs) is a daunting one. The condition runs through diverse populations of the elderly, from the walking well to the chronically ill. Each population has unique characteristics and requires a tailored approach to diagnosis and treatment.
In this article, the discussion of UTIs has been structured according to walking-well, chronically ill, and institutionalized elderly patients in order to better elucidate the issues associated with each population.
Introduction
Generally, a UTI requires treatment if significant amounts of one or more organisms are present in the urine.1 In geriatrics, bacteriuria alone frequently is insufficient to diagnose a UTI and does not always require antimicrobial treatment.2 While in the past an absolute colony count exceeding 100,000 has been diagnostic of infection and lower colony counts have been considered evidence of contamination or colonization, recent studies indicate that lower counts also may indicate infection.3
Factors that predispose the elderly to bacteriuria include hormonal changes, such as estrogen deficiency resulting in vaginal atrophy, or a reduction in colonizing lactobacilli causing an increase in vaginal pH, leading to subsequent colonization with pathogenic bacteria.4
Other medical conditions may predispose elderly patients to urinary retention and, consequently, bacteriuria. These include neurologic disease (i.e., stroke), fecal impaction, and cystocele (in women). In men, benign prostatic hyperplasia (BPH) causes urinary retention or incomplete voiding, promoting bacterial growth in the urine. Fecal soiling and poor perineal hygiene also may predispose patients to bacteriuria.5,6 Medications also may predispose elderly patients to bacteriuria. Drugs such as anticholinergics used to treat Parkinson’s disease, antihistamines, psychotropics, and pain medications can lead to decreased parasympathetic tone and reduced motility and urinary flow.
UTIs in the Walking Well
Urethritis: The primary symptoms of this condition, which results from urethral inflammation and/or infection, are dysuria (painful or difficult urination) and purulent discharge. The incidence of urethritis secondary to sexually transmitted disease (STD) caused by Chlamydia or Gonococcus has been increasing in this population, according to the CDC. The reason for this is a decrease in condom use, which would prevent STDs.7 Other pathogens include adenovirus, Escherichia coli, herpes simplex, Mycoplasma, and Trichomonas (Bradshaw urethritis).8
Prostatitis: This condition is an inflammation or infection of the prostate gland. See TABLE 1 for the prostatitis classification system used by the National Institute of Diabetes and Digestive and Kidney Diseases.9
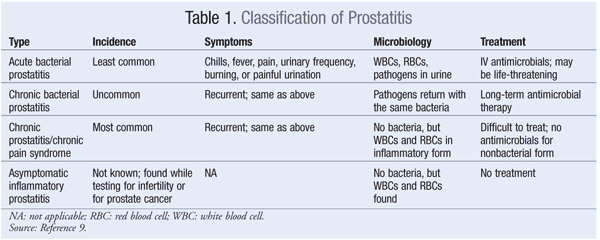
Bacterial Prostatitis: These infections, which may be acute or chronic, are characterized by local and systemic symptoms such as dysuria; urinary frequency; suprapubic, pelvic, and perineal pain; fever; chills; and overall malaise. Bacterial prostatitis generally responds to prolonged use of antimicrobials. Acute prostatitis becomes chronic if symptoms persist for more than 3 months.10 However, even in acute cases, the recurrence rate is greater than 50% in the elderly. Risk factors for acute prostatitis include urethral stricture, lower UTI (cystitis or urethritis), BPH, instrumentation of the lower urinary tract, and prostatic biopsy. Risk factors for chronic prostatitis include anatomical or physiologic lower urinary tract obstruction (i.e., neurologic etiology), voiding dysfunction, pelvic floor muscle dysfunction, intraprostatic reflux of urate and creatinine, BPH, and lower UTI.11 Bacteriology studies in prostatitis commonly implicate E coli, Proteus, Klebsiella, Streptococcus, Staphylococcus aureus, and Enterococcus.12
Cystitis: Cystitis, an inflammation or infection of the urinary bladder, is seen more often in females in this population. One of the more common causes is poor hygiene resulting in urethral contamination with fecal bacteria that then pass directly into the bladder. In males, cystitis most commonly results from urinary tract obstruction; it usually is secondary to BPH and urinary retention, but it may be secondary to bladder enervation resulting from spinal-cord injury or multiple sclerosis. Diabetes is frequently associated with cystitis since glycosuria provides an ideal environment for infection. In dementia, infection is usually caused by poor hygiene, as noted above. Patients who have received radiation therapy to the perineum (including rectum) also are prone to cystitis.13
Other conditions predisposing to cystitis include pelvic-relaxation syndromes from birth trauma, obesity, and advanced age, which in women cause the ligaments and muscles supporting the pelvic organs and the pelvic floor to stretch. Pelvic-relaxation syndromes may cause uterine and vaginal prolapse and conditions such as cystocele, urethrocele, enterocele, and ectocele.14
Interstitial Cystitis: Also known as painful bladder syndrome, interstitial cystitis involves pelvic pain, urinary urgency, and frequency in the absence of bacteriuria. Recent findings show that this condition may affect as many as 20% of women and impact quality of life significantly.15 The many causes of this condition include hormonal changes in women that alter the lining of the bladder, leading to discomfort.16 Interstitial cystitis may be caused by certain medications or by exposure to radiation therapy for tumors in the pelvic region, such as prostate or colon cancer.17
Honeymoon Cystitis: In women, this condition is diagnosed when symptoms of UTI develop following sexual intercourse. Vaginal intercourse promotes the entry of bacteria through the urethra and into the bladder. Some women contract honeymoon cystitis when pressure exerted on the bladder during vigorous sexual activity causes mucosal irritation and disruption, rendering the bladder more prone to the bacteria and causing symptoms.18
UTIs Secondary to Chronic Disease
Diabetes Mellitus: UTIs affect millions of people each year and are responsible for billions of dollars in health care spending. Elderly people with diabetes are thought to be at increased risk for UTIs, presumably secondary to immunologic, neurologic, or anatomical abnormalities.19 In the geriatric population, there is a fivefold increase in a diabetic patient’s susceptibility to UTI complications. Risk factors include duration of diabetes, high glycosylated hemoglobin level, glycosuria, and pyuria.20
A critical step in the infection process is the adhesion of pathogenic bacteria to the bladder mucosa. The high prevalence of gram-negative pathogens such as E coli and Klebsiella may be due to the pathogens’ ability to adhere to the urinary tract mucosa.21 This increased adherence in the presence of glycosuria and decreased functionality of neutrophils in diabetic patients results in an increased incidence of UTI. The low urinary pH caused by bacterial metabolism does not inhibit bacterial growth in this population.
Asymptomatic bacteriuria in the diabetic patient requires special assessment. Women with type 2 diabetes and asymptomatic bacteriuria have been found to have an increased risk of developing a UTI during 18-month follow-up (27% of those with diabetes vs. 17% of those without).22
Pyelonephritis: The most prevalent upper UTI, pyelonephritis is an ascending infection that involves the renal pelvis and is often secondary to chronic disease or a previous UTI ascending from the lower tract. It may present with fever, chills, nausea and vomiting, abdominal pain radiating to the back, and tenderness in the flank (costovertebral angle [CVA]) or bladder area. The presence of nitrite and leukocytes in the urine, as well as leukocytosis with a left shift, is generally sufficient for diagnosis. As many as 20% of women presenting with pyelonephritis demonstrate positive blood cultures; however, clinical outcomes do not differ from those in women without positive cultures.23
The frequency of pyelonephritis is approximately 250,000 cases per year, with 40% of cases leading to hospitalization.24 Urine cultures are positive in 90% of these cases. Pyelonephritis usually responds to oral or IV antimicrobial therapy. Treatment failure may be caused by resistant organisms or comorbid conditions such as obstructive abnormalities or immunocompromization. Renal impairment is always considered a sequela and must be followed.
Renal Calculi: The relationship between UTIs and renal calculi is one of cause and effect. The urinary obstruction that a stone may cause enables urine to pool above a blockage. This can be a reservoir of infection and over the long term may cause hydronephrosis. In addition, a UTI can cause the formation of struvite (magnesium, ammonium, and phosphate) stones (also known as infection stones), which develop only in infected urine.25
Mucosal trauma from the calculi can cause inflammation and create a site for the development of bacterial seeding and infection. This can be chronic in the case of renal pelvis stones (staghorn calculi), whereas other conditions, such as hyperuricemia and hypercalcemia, cause the repeated development of renal calculi.26
UTIs in Institutionalized Elderly Patients
Published infection rates of UTIs in the institutionalized geriatric population range from 12% to 30%.27 The anatomical and functional changes occurring in this population are usually complicated by underlying or chronic disease. In addition to the changes seen in the walking well, the kidneys may be less able to excrete acid and urea and may fail to maintain normal osmolality. The consequences are increased perineal colonization, vaginitis, and bacterial colonization in the bladder. In addition, male patients show a tendency toward prostatic enlargement, resulting in urinary outflow obstruction and leading to urinary stasis and further colonization.28
Decreased cognition has been identified as a contributing factor to urge incontinence. In long-term care facilities, concerns over bedwetting or soiling, skin breakdown, and secondary infection and patient hygiene associated with urinary incontinence may lead to placement of a permanent urinary catheter.29 This situation increases the risk of urosepsis (defined as bacteremia with systemic infection and potential vascular collapse). Urosepsis is potentially fatal, with approximately 4% of deaths due directly to the infection; in an additional 5%, mortality is secondary to hospital complications or complications related to underlying conditions.30
The diagnostic dilemma in this population is the paucity or absence of symptoms. Urinary frequency, urgency, or dysuria may or may not occur or may not be reported because of the underlying functional status of the patient. Geriatric patients with bacteriuria and bacteremia may not have fever or exhibit other signs of general infection. It is important to compare minor changes in the individual patient’s baseline and then begin the workup to rule out common causes of these alterations.31
One of the most challenging problems in the clinical management of this population is asymptomatic bacteriuria, which is defined as the presence of more than 100,000 colony-forming units of bacteria without symptoms or signs. This condition may be present in up to 30% of ambulatory elderly and up to 50% of institutionalized elderly.32 It also is found in nearly all catheterized patients.
Because the presence of bacteriuria does not predict mortality in the aged, screening for asymptomatic bacteriuria is not recommended unless the patient is scheduled to undergo a genitourinary procedure. Treatment does not prevent recolonization in these patients and does not reduce the risk of development of a clinically significant UTI. In fact, aggressive treatment of this condition may contribute to unnecessary antimicrobial use, with its risks of adverse events, superinfection, and development of bacterial resistance.33
UTI Diagnosis in the Geriatric Population
Symptoms in the elderly may differ from those in the general population. General criteria for diagnosing a UTI are presented in TABLES 2 and 3.34-37 Also important for diagnosis is a history of recent or multiple sexual contacts or ethanol or drug abuse resulting in syncope and poor hygiene.7,14


Physical Characteristics: A patient with clinically significant UTI appears ill and in distress. Physical findings, while variable, generally include fever (body-temperature change may be small and dependent on individualized baselines). Abdominal examination usually demonstrates tenderness over the suprapubic area, usually without rebound tenderness. Further evaluation may reveal CVA tenderness, which may be considered a hallmark of pyelonephritis or stones. Both males and females may present with urethral discharge. Females may demonstrate evidence of organ prolapse upon gynecologic examination, while in males examination may reveal an enlarged, tender prostate with discharge upon massage and manipulation.37
Laboratory Findings: Laboratory findings in clinically significant UTI will vary depending on the area of the system that is involved. Typically, urinalysis shows proteinuria and red blood cells (from inflammation and injury), and tests are nitrite positive (because bacteria that colonize in the urine convert nitrates to nitrites). White blood cells (WBCs) are present, but indicate clinical infection only in excess of 10 per high-power field.31 CBC may show leukocytosis, often with a larger-than-normal number of immature WBCs present (left shift).38
The most common organisms found on culture are E coli, Klebsiella, Gonococcus, and Chlamydia.39 When a chronic indwelling catheter is present, other organisms must be considered, including Proteus, Staphylococcus, Streptococcus, Enterococcus, and Candida.
Treatment of UTIs
When treating uncomplicated, acute cystitis in the walking-well geriatric population, the use of first-line antibiotics, such as sulfa drugs (sulfamethoxazole/
Pyelonephritis carries a higher risk of systemic complications and requires immediate assessment and initiation of treatment. In the nonhospitalized patient, initial empiric treatment can be a first-line antibiotic with adjustment within 48 hours based on urine culture and sensitivity results. Outpatient treatment should be continued for 10 to 14 days. If the patient’s condition worsens, further studies, including renal ultrasound to rule out structural abnormalities, or hospitalization with use of IV antibiotics must be considered.41
Acute prostatitis requires empiric treatment with quinolones or sulfa agents for 4 to 6 weeks. A recurrence of symptoms shortly after treatment may indicate chronic prostatitis. This requires prostatic massage with culture and sensitivity of the prostatic fluid and initiation of empiric treatment with sulfas and quinolones as above with adjustment based on laboratory findings. Antimicrobial therapy must be continued for 3 months.10
In general, quinolones have replaced sulfas as the primary antibiotic for UTIs over the last decade, although studies have shown that sulfa drugs provide adequate coverage as first-line treatment in uncomplicated UTIs.14 Attention must be paid to resistance patterns with quinolones as their usage continues to increase.38
In the treatment of suspected UTIs in institutionalized geriatric patients with indwelling catheters, it is recommended that the Loeb criteria be followed as a guide to therapy initiation and adverse outcomes.34,42 In patients without catheters, the presence of fever and other symptoms warrants initiation of therapy.
No treatment is recommended for asymptomatic patients with bacteriuria or funguria. Empiric treatment and prophylaxis are ineffective and counterproductive and could lead to increased antibiotic resistance and other complications associated with prolonged antibiotic use. In patients scheduled to undergo lower urinary tract manipulation with insertion of a Foley catheter, it is advisable to use a prophylactic course of a single 500-mg dose of levofloxacin or two doses of sulfamethoxazole/trimethoprim.
In geriatric patients presenting with urethritis in which the causative agent is identified as Gonococcus or Chlamydia, empiric treatment as per current public recommendations is advised. The use of ceftriaxone or doxycycline is commonly prescribed. Levofloxacin may also be effective in these cases. Other organisms to be considered in the sexually active geriatric population include adenoviruses, Mycoplasma, Ureaplasma, and Gardnerella vaginalis.44 Treatments for these organisms are dictated by culture and sensitivity results.
Conclusion
Various geriatric populations, from the walking well to those with chronic disease to the institutionalized, are affected by UTIs. Each of these populations is impacted in different ways and requires a different treatment approach. It is important to remember that comorbidities can affect the site and seriousness of the infection; this must be kept in mind in the diagnosis and treatment of an individual patient’s UTI.
Symptoms of UTI in elderly patients may differ from those seen in the general population. In a patient with a suspected infection, diagnosis should be made based on the individual patient’s presenting symptoms, physical examination, and laboratory findings. Various treatments are available for UTI, and therapy should be based on the causative agent as well as on the pathophysiology and underlying comorbidities present.
UTIs are found throughout the geriatric population, with variable presentations. The treatment must be based on the patient’s overall health, underlying chronic conditions, and ability to care for himself or herself. Each patient’s care must be individualized to obtain the best possible outcome.
REFERENCES
1. Midthun SJ. Criteria for urinary tract infection in the elderly: variables that challenge nursing assessment. Urol Nurs. 2004;24:157-162,166-169,186.
2. Nicolle LE. Urinary tract infection: traditional pharmacologic therapies. Dis Mon. 2003;49:111-128.
3. Strand CL, Bryant JK, Sutton KH. Septicemia secondary to urinary tract infection with colony counts less than 105 CFU/mL. Am J Clin Pathol.1985;83:619-622.
4. Samsioe G. Urogenital aging—a hidden problem. Am J Obstet Gynecol. 1998;178:S245-S249.
5. Gomolin IH, McCue JD. Urinary Tract Infection in the Elderly Patient. Darien, CT: Cliggott Publishing; 2000.
6. Shortliffe LM, McCue JD. Urinary tract infection at the age extremes: pediatrics and geriatrics. Am J Med. 2002;113(suppl 1A):55S-66S.
7. Ginsberg TB. Aging and sexuality. Med Clin North Am. 2006;90:1025-1036.
8. Bradshaw CS, Denham IM, Fairley CK. Characteristics of adenovirus associated urethritis. Sex Transm Infect. 2002;78:445-447.
9. Krieger JN, Nyberg L, Nickel JC. NIH consensus definition and classification of prostatitis. JAMA. 1999;282:236-237.
10. Ramakrishnan K, Salinas R. Prostatitis: acute and chronic. Prim Care. 2010;37:547-563.
11. Lobel B, Rodriguez A. Chronic prostatitis: what we know, what we do not know, and what we should do! World J Urol. 2003;21:57-63.
12. Millán-Rodríguez F, Palou J, Bujons-Tur A, et al. Acute bacterial prostatitis: two different sub-categories according to a previous manipulation of the lower urinary tract. World J Urol. 2006;24:45-50.
13. Rahn D. Urinary tract infections: contemporary management. Urol Nurs. 2008;28:333-341.
14. Liang SY, Mackowiak PA. Infections in the elderly. Clin Geriatr Med. 2007;24:441-456.
15. Sairanen J, Leppilahti M, Tammela TL, et al. Evaluation of health-related quality of life in patients with painful bladder syndrome/interstitial cystitis and the impact of four treatments on it. Scand J Urol Nephrol. 2009;43:212-219.
16. Erickson D, Propert K. Pregnancy and interstitial cystitis/painful bladder syndrome. Urol Clin N Am. 2007;34:61-69.
17. Wu EQ, Birnbaum H, Mareva M, et al. Interstitial cystitis: cost, treatment and co-morbidities in an employed population. Pharmacoeconomics. 2006;24:55-65.
18. Chew L, Fihn S. Recurrent cystitis in non-pregnant women. West J Med. 1999;170:274-277.
19. Stapleton A. Urinary tract infections in patients with diabetes. Am J Med. 2002;113(suppl 1A):80S-84S.
20. Turan H, Serefhanoglu K, Torun AN, et al. Frequency, risk factors, and responsible pathogenic microorganisms of asymptomatic bacteriuria in patients with type 2 diabetes mellitus. Jpn J Infect Dis. 2008;61:236-238.
21. Hoepelman AI, Meiland R, Geerlings SE. Pathogenesis and management of bacterial urinary tract infections in adult patients with diabetes mellitus. Int J Antimicrob Agents. 2003;22:S35-S43.
22. Geerlings SE, Brouwer EC, Gaastra W, et al. Effect of glucose and pH on uropathogenic and non-uropathogenic Escherichia coli: studies with urine from diabetic and non-diabetic individuals. J Med Microbiol. 1999;48:535-539.
23. Nicolle L. Uncomplicated urinary tract infection in adults including uncomplicated pyelonephritis. Urol Clin N Am. 2008;35:1-12.
24. Ramakrishnan K, Scheid DC. Diagnosis and management of acute pyelonephritis in adults. Am Fam Physician. 2005;71:933-942.
25. Johri N, Cooper B, Robertson W, et al. An update and practical guide to renal stone management. Nephron Clin Pract. 2010;116:C159-C171.
26. Akagashi K, Tanda H, Kato S, et al. Characteristics of patients with staghorn calculi in our experience. Int J Urol. 2004;11:276-281.
27. O’Donnell JA, Hofmann MT. Urinary tract infections: how to manage nursing home patients with or without chronic catheterization. Geriatrics. 2002;57:45-58.
28. Grover ML, Bracamonte JD, Kanodia AK, et al. Urinary tract infection in women over the age of 65: is age alone a marker of complication? J Am Board Fam Med. 2009;22:266-271.
29. Griffiths D. Clinical studies of cerebral and urinary tract function in elderly people with urinary incontinence. Behav Brain Res. 1998;92:151-155.
30. Armitage KB, Salata RA, Landefeld CS. Urosepsis in the elderly: clinical and microbiological characteristics. Infect Dis Clin Pract. 1993;2:260-266.
31. Juthani-Mehta M, Drickamer MA, Towle V, et al. Nursing home practitioner survey of diagnostic criteria for urinary tract infections. J Am Geriatr Soc. 2005;53:1986-1990.
32. Juthani-Mehta M. Asymptomatic bacteriuria and urinary tract infection in older adults. Clin Geriatr Med. 2007;23:585-594.
33. Nicolle L. Asymptomatic bacteriuria: review and discussion of the IDSA guidelines. Int J Antimicrob Agents. 2006;28S:S42-S48.
34. Loeb M, Bentley DW, Bradley S, et al. Development of minimum criteria for the initiation of antibiotics in residents of long-term-care facilities: results of a consensus conference. Infect Control Hosp Epidemiol. 2001;22:120-124.
35. McGeer A, Campbell B, Emori TG, et al. Definitions of infection for surveillance in long-term care facilities. Am J Infect Control. 1991;19:1-7.
36. Jackson MM, Fierer J, Barrett-Connor E, et al. Intensive surveillance for infections in a three-year study of nursing home patients. Am J Epidemiol. 1992;135:695-696.
37. Schmiemann G, Kniehl E, Gebhardt K, et al. The diagnosis of urinary tract infection: a systematic review. Dtsch Arztebl Int. 2010;107:361-367.
38. Grover ML, Bracamonte JD, Kanodia AK, et al. Assessing adherence to evidence-based guidelines for the diagnosis and management of uncomplicated urinary tract infection. Mayo Clin Proc. 2007;82:181-185.
39. Caterino JM, Weed SG, Espinola JA, Camargo CA Jr. National trends in emergency department antibiotic prescribing for elders with urinary tract infection, 1996–2005. Acad Emerg Med. 2009;16:500-507.
40. McEwen L, Farjo R, Foxman B. Antibiotic prescribing for cystitis: how well does it match published guidelines? Ann Epidemiol. 2003;13:479-483.
41. Warren J, Abrutyn E, Hebel JR, et al. Guidelines for antimicrobial treatment of uncomplicated acute bacterial cystitis and acute pyelonephritis in women. Infectious Diseases Society of America (ISDA). Clin Infect Dis. 1999;29:745-758.
42. Gindle AA, Rhee SH, Katz ED. Predictors of outcome in geriatric patients with urinary tract infections. J Emerg Med. 2004;27:101-108.
43. Wolf JS, Bennett CJ, Dmochowski RR, et al. Best practice policy statement on urologic surgery antimicrobial prophylaxis. J Urol. 2008;179:1379-1390.
44. Bradshaw CS, Tabrizi SN, Read TR, et al. Etiologies of nongonococcal urethritis: bacteria, viruses, and the association with orogenital exposure. J Infect Dis. 2006;193:336-345.
To comment on this article, contact rdavidson@uspharmacist.com.





