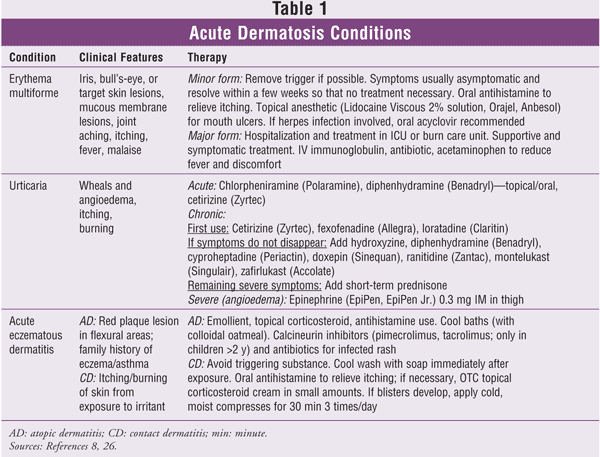
Dermatosis is defined as a disorder involving lesions or eruptions of the skin that are acute (lasting days to weeks) or chronic (lasting months to years). Acute lesions are relatively common and exhibit a wide range of clinical conditions. Usually, these conditions are triggered by local or systemic immunologic factors (e.g., allergic reaction); however, the exact etiology remains unclear. Acute inflammatory dermatosis conditions include erythema multiforme (EM), pruritus (urticaria), and eczema (TABLE 1). Treatment options differ for acute and chronic lesions.1 This article reviews the conditions and treatment of common acute dermatosis lesions.
Erythema Multiforme
EM is classified into two forms: a mild or minor form (about 80% of cases) and a major form (rarer and severe). The minor form is usually a self-limiting, quick-onset condition, and the major form has high morbidity and death.2 EM is classified as a type III or type IV hypersensitivity reaction to certain drugs or to infections (TABLE 2) including herpes, tuberculosis, Mycoplasma pneumoniae, and histoplasmosis.3-7 Lesions may affect only the skin or the skin and mucous membranes in the mouth, nose, or genital areas.2 Usually, an individual will start with a fever, sore throat, and malaise for about a week, after which a rash appears. EM commonly occurs in young adults (between 20 and 40 years of age) and affects men more than women.8 About one-third of patients experience disease recurrence.8,9

Clinically, there is a distinctive distribution of fixed red papules, macules, or bullae, hence the name multiforme.10 Plaques are small, circumscribed lesions less than 1 cm in diameter that are elevated or protrude above the surface of normal surrounding tissue. Macules are flat lesions that have a different color from the surrounding tissue (e.g., freckles). Bullae are circumscribed, elevated lesions that are more than 5 mm in diameter and contain serous fluid; they look like blisters.11
Over time, these primary lesions typically grow larger and produce well-demarcated plaques that undergo variable concentric changes; some have central blisters with a necrotic blister roof, while others have areas of central epidermal necrosis without circumscribed blister formation.10,12 Skin lesions frequently have a characteristic bull's-eye, iris, or target lesion that consists of concentric rings of erythema alternating with normal skin color, with the darkest color at the center of the lesion. Oral lesions usually present as ulcers and are commonly found on the lateral borders of the tongue. Crusted and bleeding lips are frequently seen in these patients.9,13
First described in 1922, Stevens-Johnson syndrome (SJS)--sometimes referred to as EM major--is life-threatening.10,12,14 It is generally agreed that SJS and toxic epidermal necrolysis are different manifestations of the same disease.15 Both the skin and mucous membranes are affected, and the lips are crusted with blood. Mucosal lesions are found on the mucosa of the eyes, nose, mouth, and genitals; they are more widespread and severe than in the minor form, and it is painful for the patient to eat and urinate.16 SJS is usually due to a reaction to medications rather than an infection; however, mycoplasma infection is considered to be a possible etiology.17 Possible sequelae to SJS are organ damage and blindness.
Diagnosis and Prognosis: Diagnosis of EM is made on clinical findings with the exclusion of other diseases. Histologic features are not specific, so biopsy is necessary. For the minor form of EM, healing usually takes about 2 to 4 weeks; the most severe major form (SJS) may last for a prolonged period of time and has a mortality rate of about 5%.12,16 The increased mortality is due to a higher rate of bacterial superinfection and sepsis. EM must be distinguished from many conditions, including urticaria, which usually heals within 24 hours and does not form blisters.18 Some other confounding conditions are lupus erythematosus, pityriasis rosea, viral exanthem, autoimmune bullous diseases (e.g., pemphigoid), vasculitis, and Kawasaki disease.4,11
Treatment: If the systemic cause of EM can be identified, treatment should be initiated to treat the cause. For instance, if the patient has been diagnosed with M pneumoniae-associated EM, a macrolide or tetracycline should be administered.16,18 If herpes-associated EM is diagnosed, acyclovir should be administered as early as possible. If a drug is the etiologic factor, it should be discontinued immediately.16,18 Since mild cases of EM are self-limiting, most signs and symptoms (although the patient usually is asymptomatic) will dissipate soon after removal of the triggering cause; however, adjunctive palliative treatment (e.g., antihistamines) or topical corticosteroids (e.g., fluocinonide or betamethasone) may be necessary to alleviate symptoms.18,19 Antibiotics are used to control secondary skin infections. Mouth ulcers can be quite painful and interfere with eating, drinking, and talking. Topical anesthetics containing lidocaine or benzocaine are helpful. The use of systemic corticosteroids is controversial and usually not necessary.18,20 Recurrent cases due to herpes simplex virus infection can be prevented with continuous oral acyclovir and monitored by a dermatologist.18 Many other drugs have been used successfully for the management of recurrent EM, including dapsone (100-150 mg/day), hydroxychloroquine (200 mg/day), and azathioprine (100-150 mg/day).8,21
Rapid desensitization is a form of therapy that allows patients to be treated with medications to which they previously had a hypersensitivity reaction.22 This method achieves temporary tolerization to full therapeutic doses by slow administration of incremental doses of the drug that induced the hypersensitivity reaction.
Treatment of SJS is more involved and complicated, and there are no set guidelines to follow. All triggering medications should be discontinued. Some patients are best treated in a hospital-based burn unit. Most treatment is symptomatic (e.g., topical oral analgesics) and supportive. The use of systemic corticosteroids for their anti-inflammatory and immunosuppressive properties is controversial.20 Early administration of these agents has been documented in some cases, but their use is discouraged because of reports of increased morbidity and mortality due to sepsis.23 Other agents, such as cyclosporine and cyclophosphamide, have been used, but without a high success rate.24,25 Intravenous immunoglobulins are used anecdotally to help stop the progression. Antibiotics are given for secondary bacterial skin infections.
Urticaria
Urticaria, or hives, is a common (25% of the U.S. population) skin condition that is characterized by localized mast-cell degranulation resulting in dermal hyperpermeability and pruritic edematous plaque lesions.26 Lesions develop quickly after exposure to the allergen or antigen, with a central area of swelling, redness, and blanching. The pruritic, plaquelike lesions may coalesce, forming annular, linear, or arciform configurations, and they may itch or burn. A common site for lesions is the skin, especially areas exposed to pressure, such as the trunk, ears, and distal extremities. Lesions can spread by scratching, forming large red patches.
The swelling, or edema, is caused by plasma leaking out of the small blood vessels in the connective tissue; this is an inflammatory response to the foreign antigen. The center of the lesion is pale because of the edema. The swellings can be either superficial in the dermis (referred to as wheals) or deeper in the lower dermis or subcutaneous fat (known as angioedema). Areas of angioedema usually involve the face, mouth (lips), buttocks, genitals, abdominal organs, and larynx.26 Histamine, which also leaks out of the blood vessels, is responsible for the itching.
Urticaria can be acute or chronic and spontaneous, physical, or another form. Acute urticaria usually persists for less than 6 weeks; wheals last no more than 24 hours and heal without complications.27 Chronic episodes of urticaria, which are not as common, may occur for longer periods of time, at least twice a week for at least 6 weeks; they can last up to months or years and may be associated with angioedema.28
Chronic urticaria is divided into two classifications: 40% to 50% of patients with the condition have chronic autoimmune urticaria (CAU), and 50% to 60% have chronic idiopathic urticaria.29,30 CAU is commonly caused by an immunoglobulin (Ig) G antibody to the alpha subunit of the IgE receptor usually reactive with unoccupied IgE receptors, or by IgG antibody to IgE (5%-10%).30 CAU also may be associated with antithyroid antibodies (27%); diseases such as vasculitis and hepatitis; and viral (e.g., cytomegalovirus, Epstein-Barr), bacterial, or fungal infections.30
Etiology: Spontaneous acute urticaria is caused by many triggers: foods, medications, insect bites, contact allergies, and viral upper respiratory tract infections, especially in children. Foods containing high amounts of histamine, such as strawberries, tomatoes, shrimp, lobster, cheese, spinach, and eggplant, also can trigger a response.26 The release of histamine from cutaneous mast cells and basophils in response to the allergen initiates the IgE immune process. Urticaria and angioedema are the result of the IgE antibody-mediated reaction.30
Causes of chronic urticaria are more difficult to determine and may be idiopathic without any identifiable etiology.26 Physical urticaria is caused by sun exposure, cold, exercise, heat, water, pressure (e.g., carrying something heavy against the body), scratching, or vibration.30After exposure, the individual may experience wheezing, flushing, and wheals.30
Diagnosis: The diagnosis of urticaria is relatively uncomplicated because it is based on a physical examination and a thorough medical history. Blood testing and biopsy are not necessary. Many physical and contact urticarias can be confirmed by a challenge of the triggering agent, or by a skin test or radioallergosorbent test for atopy.29
More severe cases of urticaria, which represent only 5% to 10% of occurrences, are usually associated with a systemic disease such as lupus erythematosus or Sjögren's syndrome. In these cases, CBC, erythrocyte sedimentation rates, and urinalysis can be ordered.31 Laryngeal angioedema is a medical emergency requiring prompt assessment.26
Treatment: Treatment of acute urticaria is based on removal or avoidance of the triggering agent.32 The mainstay of therapy is an oral antihistamine such as chlorpheniramine or diphenhydramine or a nonsedating H1-receptor antagonist such as loratadine, cetirizine, or fexofenadine, which are adequate in mild cases (TABLE 1). If symptoms do not disappear, other medications should be added. For example, cyproheptadine is the drug of choice for cold-induced urticaria, and ranitidine may be useful in combination with an H1-blocker, although it can exacerbate urticaria. Also, since doxepin is both an H1- and an H2-blocker, it is helpful when an H1 alone is not enough.26,31 Calamine lotion and cool baths with or without colloidal oatmeal are soothing and relieve the itching.
The treatment of chronic urticaria follows specific guidelines. It is recommended to start with a nonsedating H1-receptor antagonist such as cetirizine, fexofenadine, or loratadine. If symptoms do not disappear, add hydroxyzine, diphenhydramine, cyproheptadine, doxepin, ranitidine, montelukast, or zafirlukast. If symptoms remain severe, the judicious addition of short-term prednisone may be considered.30 Additionally, a sunscreen should be added for solar urticaria.
In a more severe angioedema case involving anaphylaxis, epinephrine at a dose of 0.3 mL to 0.5 mL 1:1,000 solution intramuscularly (IM) every 15 minutes is administered to adults; a 1:2,000 solution at a dose of 0.3 mL (0.15 mg) IM (maximum 0.3 mL) is administered to children.
Acute Eczematous Dermatitis
The terms eczema, dermatitis, and eczematous dermatitis frequently are used interchangeably and very often are used nonspecifically, resulting in confusion for both clinician and patient. Many dermatologists avoid the term eczema altogether because of its ambiguity.33 Eczema, whose literal translation is "to boil over," is a broad category including many pruritic inflammatory disorders, but the two most common reasons for an eczematous reaction are atopic dermatitis (AD) and allergic contact dermatitis (ACD).1 Although AD and ACD are completely different in nature and pathogenetically unrelated, in the acute stage both disorders share common morphologic features, especially vesicle formation, which ultimately causes a disruption of the epidermal barrier. The loss of this protective shield allows additional external noxious agents of microbial, chemical, or physical origin to enter the skin, thereby aggravating and perpetuating the disease. For this reason, vesicle formation and subsequent loss of the epidermal barrier are key events in acute eczematous reactions.34
Eczema can be acute, chronic, or both. Acute lesions appear quickly as red rashes, which may become blisters (vesicles) that form in the epidermis and ooze and then crust over.1 Chronic lesions are generally dry and scaly, with thickenings and skin markings (lichenification) and altered pigmentation.35
AD and ACD
AD, the most common cause of eczematous rash in children, usually first appears in infants aged 2 to 6 months. The prevalence rate is 10% to 12% in children and 0.9% in adults.36 In infants and children, the rash appears on the shoulders, chest, abdomen, and back, but also occurs on the face or scalp and around the ears. This condition resolves spontaneously by puberty in most patients, but it sometimes recurs in times of stress or for unknown reasons. In adults, the rash may appear as recalcitrant hand eczema or as a localized or generalized dermatitis.36
Patients with AD nearly always have a family history of dermatitis or asthma.36 The classic triad of atopy consists of asthma, allergic rhinitis, and atopic dermatitis. Atopic skin is particularly susceptible to bacterial and viral infections, which may become widespread. Some common causes of AD are dry weather, frequent bathing, and wool or synthetic clothing; aeroallergens such as dust mites, animal dander, and mold may exacerbate the condition.37
Histologically, AD is a hypersensitivity reaction involving the binding of IgE to mast cells; degranulation of the mast cells occurs upon exposure to the antigen, and histamine is released.38 Children afflicted with AD may lose sleep because of the constant itching.37
Treatment of the acute, weeping stages of AD (TABLE 3) involves the application of wet dressings (description follows) and topical corticosteroids that can be applied underneath the wet dressing twice daily.39 Only low-potency corticosteroids such as hydrocortisone and desonide should be applied to the facial area. The topical immunomodulators and calcineurin inhibitors pimecrolimus and tacrolimus have been shown to be very effective for AD, with fewer side effects than topical steroids.35 Calcineurin inhibitors are not approved for children under 2 years.35

The most common local effects of exposure to the irritant are skin burning and irritation, so patients must be counseled regarding appropriate sun protection.37 An emollient cream should be applied immediately after bathing and at least twice daily to prevent dryness.37 The use of sedating and nonsedating antihistamines to treat pruritus associated with AD has been shown to be ineffective when compared with placebo, except in association with an allergy.40
Antibiotics may be need to be administered if infection occurs. If improvement is not seen, culturing may be necessary to determine the resistant bacterium. Infection usually is due to Staphylococcus aureus or Streptococcus pyogenes.
A wet dressing consists of a wet (warm water and wrung out) pair of long underwear or pajamas worn with a dry pair over it.36 The dressing is changed every 4 to 6 hours.36 A wet dressing enables the skin to be in an environment of 100% humidity with the moisture allowed to evaporate to 60%, which relieves the pruritus. Optimum results are seen if this treatment is administered throughout the day rather than just at night.
ACD results from contact with certain substances, including dental materials.41 Repeated exposure to the antigen causes an allergic sensitization. After the initial exposure, clinical signs may not appear for up to 7 to 10 days. After repeated exposures, lesions will appear within 12 hours. Both ACD and AD are characterized by a lymphocyte infiltration and spongiosis, or marked intercellular edema, of the stratum spinosum layer of the epidermis.1
Treatment for ACD consists of oral antihistamines, topical corticosteroids, and wet dressings. The suspected trigger should be avoided. The area should be washed with soap and cool water. Application of calamine lotion or use of colloidal oatmeal baths may help relieve the itching. Dermatitis is often a long-term problem. Patients should be counseled to moisturize their skin and carefully avoid the use of soap when they notice their skin getting dry; if the itchy rash returns, they should use both the moisturizer and the steroid cream or ointment.
Conclusion
Acute inflammatory dermatoses are relatively common afflictions that have a myriad of causes. The pharmacist can help patients discern possible triggering agents of the skin condition and suggest preventive and treatment strategies, including referral to a dermatologist.
REFERENCES
1. Murphy GF, Mihm MC Jr. The skin. In: Cotran RS, Kumar V, Collins T, eds. Robbins Pathologic Basis of Disease. 6th ed. Philadelphia, PA: WB Saunders Co.; 1999:1170-1213.
2. Farthing P, Bagan JV, Scully C. Mucosal disease series. Number IV. Erythema multiforme. Oral Dis. 2005;11:261-267.
3. Raksha MP, Marfatia YS. Clinical study of cutaneous drug eruptions in 200 patients. Indian J Dermatol Venereol Leprol. 2008;74:80.
4. Locharernkul C, Loplumlert J, Limotai C, et al. Carbamazepine and phenytoin induced Stevens-Johnson syndrome is associated with HLA-B*1502 allele in Thai population. Epilepsia. 2008;49:2087-2091.
5. Borrás-Blasco J, Navarro-Ruiz A, Borrás C, Casterá E. Adverse cutaneous reactions associated with the newest antiretroviral drugs in patients with immunodeficiency virus infection. J Antimicrob Chemother. 2008;62:879-888.
6. Hofbauer GF, Burg G, Nestle FO. Cocaine-related Stevens-Johnson syndrome. Dermatology. 2000;201:258-260.
7. Hillebrand-Haverkort ME, Budding AE, bij de Vaate LA, van Agtmael MA. Mycoplasma pneumoniae infection with incomplete Stevens-Johnson syndrome. Lancet Infect Dis. 2008;8:586-587.
8. Habif TP. Hypersensitivity syndromes and vasculitis. In: Habif TP, ed. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 4th ed. New York, NY: Mosby; 2004:626-634.
9. Huff JC. Acyclovir for recurrent erythema multiforme caused by herpes simplex. J Am Acad Dermatol. 1988;18:197-199.
10. Yeung AK, Goldman RD. Use of steroids for erythema multiforme in children. Can Fam Physician. 2005;51:1481-1483.
11. Ibsen O. Introduction to preliminary diagnosis of oral lesions. In: Ibsen OA, Phelan JA, eds. Oral Pathology for the Dental Hygienist. 4th ed. Philadelphia, PA: WB Saunders Co.; 2003:2-33.
12. Weston WL. What is erythema multiforme? Pediatr Ann. 1996;25:106-109.
13. Ayangco L, Rogers RS III. Oral manifestations of erythema multiforme. Dermatol Clin. 2003;21:195-205.
14. Hazin R, Ibrahimi OA, Hazin MI, Kimyai-Asadi A. Stevens-Johnson syndrome: pathogenesis, diagnosis, and management. Ann Med. 2008;40:129-138.
15. Sharma VK, Sethuraman G, Minz A. Stevens Johnson syndrome, toxic epidermal necrolysis and SJS-TEN overlap: a retrospective study of causative drugs and clinical outcome. Indian J Dermatol Venereol Leprol. 2008;74:238-240.
16. Parrillo SJ, Parrillo CV. Stevens-Johnson syndrome. eMedicine Web site.
http://emedicine.medscape.com/
17. Tay YK, Huff JC, Weston WL. Mycoplasma pneumoniae infection is associated with Stevens-Johnson syndrome, not erythema multiforme (von Hebra). J Am Acad Dermatol. 1996;35:757-760.
18. Lamoreux MR, Sternbach MR, Hsu WT. Erythema multiforme. Am Fam Physician. 2006;74:1883-1888.
19. Shin HT, Chang MW. Drug eruptions in children. Curr Probl Pediatr. 2001;31:207-234.
20. Volcheck GW. Clinical evaluation and management of drug hypersensitivity. Immunol Allergy Clin North Am. 2004;24:357-371.
21. Mahendran R, Grant JW, Norris PG. Dapsone-responsive persistent erythema multiforme. Dermatology. 2000;200:281-282.
22. Castells MC. Hypersensitivity to antineoplastic agents. Curr Pharm Des. 2008;14:2892-2901.
23. Roujeau JC. Treatment of severe drug eruptions. J Dermatol. 1999;26:718-722.
24. Bakis S, Zagarella S. Intermittent oral cyclosporin for recurrent herpes simplex-associated erythema multiforme. Australas J Dermatol. 2005;46:18-20.
25. Trautmann A, Klein CE, Kämpgen E, Bröcker EB. Severe bullous drug reactions treated successfully with cyclophospha mide. Br J Dermatol. 1998;139:1127-1128.
26. Muller B. Urticaria and angioedema: a practical approach. Am Fam Physician. 2004;69:1123-1138.
27. Greaves M. Chronic urticaria. J Allergy Clin Immunol. 2000;105:664-672.
28. Grattan CE, Sabroe RA, Greaves MW. Chronic urticaria. J Am Acad Dermatol. 2002;46:645-657.
29. Guldbakke KK, Khachemoune A. Classification and treatment of urticaria: a brief review. Dermatol Nurs. 2005;17:361-364.
30. Kaplan AP. Chronic urticaria: pathogenesis and treatment. J Allergy Clin Immunol. 2004;114:465-474.
31. Joint Task Force on Practice Parameters. The diagnosis and management of urticaria: a practice parameter. Part I: acute urticaria/angioedema. Part II: chronic urticaria/angioedema. Ann Allergy Asthma Immunol. 2000;85:521-544.
32. Lee EE, Maibach HI. Treatment of urticaria. An evidence-based evaluation of antihistamines. Am J Clin Dermatol. 2001;2:27-32.
33. Shaw JC. Allergic and nonallergic eczematous dermatitis. Immunol Allergy Clinics North Am. 1996;16:119-135.
34. Schwarz T. No eczema without keratinocyte death. J Clin Invest. 2000;106:9-10.
35. Callahan JM. Rash--eczematous. In: Fleisher GR, Ludwig S, FM Henretig FM, et al, eds. Textbook of Pediatric Medicine. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005:549-558.
36. Horii KA, Simon SD, Liu DY, Sharma V. Atopic dermatitis in children in the United States, 1997-2004: visit trends, patient and provider characteristics, and prescribing patterns. Pediatrics. 2007;120:e527-534.
37. Buys LM. Treatment options for atopic dermatitis. Am Fam Physician. 2007;75:523-528.
38. Novak N, Bieber T, Leung DY. Immune mechanisms leading to atopic dermatitis. J Allergy Clin Immunol. 2003;112:S128-S139.
39. Morelli JG, Weston WL. Skin. In: Hay WW Jr, Hayward AR, Levin MJ, Sondheimer JM, eds. Current Pediatrics Diagnosis & Treatment. 16th ed. New York, NY: McGraw-Hill; 2003:400-419.
40. Klein PA, Clark RA. An evidence-based review of the efficacy of antihistamines in relieving pruritus in atopic dermatitis. Arch Dermatol. 1999;135:1522-1525.
41. Kanerva L, Estlander T, Jolanki R. Allergic contact dermatitis from dental composite resins due to aromatic epoxy acrylates and aliphatic acrylates. Contact Dermatitis. 1989;20:201-211.






