US Pharm.
2008;33(2):HS-16-HS-25.
Cocaine is one of the most
commonly used illicit drugs, and its abuse is a widespread problem in the
United States and around the world. Approximately 13.8% (33.7 million) of
Americans age 12 and older have reported trying cocaine at least once.1
Although the psychological effects of cocaine are widely known due to media
exposure, most users know little about the medical consequences. This review
will focus on cocaine-associated chest pain, the most common cocaine-related
medical problem.2
Cocaine History
Cocaine
(benzoylmethylecgonine) is an alkaloid isolated from the leaves of
Erythroxylon coca, a plant indigenous to western South America.3
The use of the cocaplant dates back to early recorded history; archaeological
evidence suggests that the chewing of coca leaves was practiced by the Incan
civilization 5,000 years ago. The Incas purportedly used the plant for the
relief of hunger and fatigue and as a local anesthetic.3,4 Cocaine
was isolated by the German chemist Friedrich Gaedcke in 1855, and Albert
Niemann is credited with being the first to purify and name it.5
The substance became popular in the United States in the late 1800s, when it
was used in such products as cigarettes, toothache drops, and beverages (coca
wines, Coca-Cola).3,6
Cocaine use was first
restricted by the 1906 Pure Food and Drugs Act, which required the proper
labeling of medications to list all constituents.7 The Harrison
Narcotics Act, which followed in 1914, identified cocaine as a narcotic and
limited its use to prescription medications.8 In 1970, the
Controlled Substances Act further prohibited the manufacture, distribution,
and possession of cocaine, except for limited medicinal use. Today, cocaine is
classified as a Schedule II drug, indicating its high potential for abuse and
its high incidence of psychological and physical dependence while also
recognizing its medi!=cinal value.9 Currently, cocaine's only
pharmacotherapeutic use is as a local anesthetic for topical application to
the mucous membranes of the nasal, oral, or laryngeal cavities.
Forms of Cocaine
Cocaine is
available as a hydrochloride salt, as "free base," and as "crack" cocaine.
6 The hydrochloride form is prepared by dissolving the alkaloid in
hydrochloric acid to form a water-soluble powder or granule. This
water-soluble form can be taken orally, IV, or intranasally; it cannot be
smoked because it decomposes when heated.10 The free-base form is
lipophilic and is produced by dissolving the cocaine in water and then
extracting it using a solvent.10 This type of cocaine is smoked.
Crack cocaine is molecularly the same as free base, but is prepared by the
simpler method of alkalinizing the cocaine with ammonia or sodium bicarbonate
(baking soda) and then heating it.10 It is heat stable and melts at
98C, thereby allowing it to be smoked.6 Because crack cocaine is
inexpensive to make, it is easily accessible and thus a popular form of the
drug.6
Pharmacokinetics
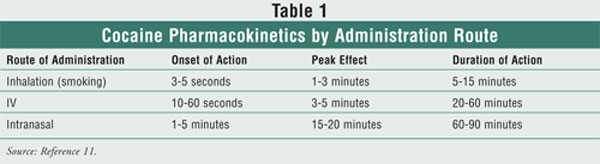
Since cocaine
hydrochloride is well absorbed through all mucous membranes, cocaine users may
achieve high blood concentrations via intranasal, sublingual, intra!=vaginal,
or rectal administration (see TABLE 1).11 Compared with IV
injection of the drug, mucosal administration has a slower onset of action, a
delayed peak effect, and a longer duration of action.6 Intranasal
administration causes local vasoconstriction, delaying absorption into the
vasculature, which may contribute to the longer duration of action.6
When crack cocaine is smoked, it is rapidly absorbed by the extensive
pulmonary vasculature, leading to euphoria within seconds. Due to its rapid
and intense euphoric action, crack cocaine is considered to be the most potent
and addictive form of the drug.3,6,12
Detection of active cocaine in
the blood is difficult due the short serum half-life of 45 to 90 minutes.
10 Instead, cocaine metabolites are commonly used as an indicator of
recent drug ingestion.6,10,12
Cocaine is metabolized by
plasma and liver cholinesterases to the metabolite ecgonine methyl ester.
10 Nonenzymatic hydrolysis metabolizes cocaine to benzoylecgonine.10
Both metabolites are excreted in the urine.12 While these
metabolites are generally thought to be inactive, research has shown that they
may have pharmacologic activity and could be responsible for some adverse
effects, including vasoconstriction.10,13 Interestingly, some
research has shown that individuals with low plasma cholinesterase levels may
be predisposed to the cardiotoxic effects of cocaine due to their poor ability
to metabolize it into inactive compounds.14,15
Another important metabolite,
cocaethylene, is formed when cocaine and ethanol are ingested together, a
common occurrence among cocaine users.16 Cocaethylene is an active
metabolite with psychoactive effects similar to those of cocaine.17,18
Conversion of cocaine and ethanol to cocaethylene leads to less formation of
the benzoylecgonine, an inactive metabolite, which may lead to increased
adverse events.19 Importantly, cocaethylene may contribute to
cardiovascular adverse events, possibly by blocking cardiac sodium channels.
20,21 Some animal research has shown that cocaethylene and cocaine have
similar toxicities relating to the heart.17,22 Additionally,
cocaethylene has a longer half-life than cocaine (2.5 hours versus 50 to 90
minutes), which may explain why many patients experiencing myocardial
infarction (MI) after cocaine use have low plasma cocaine levels.22,23
However, some researchers disagree that cocaethylene contributes to the
cardiovascular adverse events of cocaine.24
Pharmacology
Cocaine is a potent
central nervous system stimulant. When taken systemically, cocaine binds to
catecholamine transport protein, altering synaptic transmission by blocking
the presynaptic reuptake of norepinephrine, dopamine, and serotonin. This
blockade results in an excess of neurotransmitters at the site of the
postsynaptic receptors, leading to an increase in postsynaptic receptor
stimulation.11 The inhibition of dopamine reuptake is primarily
responsible for cocaine's euphoric action.6
When applied topically,
cocaine acts as a local anesthetic by blocking the initiation and transmission
of electrical signals. The action is due to cocaine's ability to inhibit
membrane permeability to sodium ions during depolarization.25
Inhibition of norepinephrine uptake leads to increased alpha-adrenergic
stimulation and thus can result in vasoconstriction.10
Pathophysiology of
Cocaine-Induced Chest Pain
Of the many
complications that are associated with cocaine use (see TABLE 2), the
most frequent complaint is chest pain.3,26-31 The incidence among
cocaine users who present to the hospital has been reported to be as high as
40%.2,32 Ischemia, including acute coronary syndrome (ACS), is the
most common cocaine-associated cardiac disorder.2

Of all patients presenting
with cocaine-associated chest pain, approximately 6% are experiencing MI and
15% have ACS. The risk of MI is 24-fold higher in the first hour after cocaine
use, but has been documented for up to six weeks following cocaine withdrawal.
33 Demographic and historical factors are not reliable for predicting
cocaine-associated MI, but most patients are young, male cigarette smokers
without other risk factors for atherosclerosis.34 Patients,
especially young ones, should be questioned about cocaine use if they present
with chest pain, and anyone with potential cocaine toxicity should receive a
complete evaluation.12,33
The pathophysiology of
cocaine-induced myocardial ischemia is multifactorial. Proposed mechanisms are
coronary thrombosis, coronary artery vasoconstriction, mismatch between
myocardial oxygen demand and supply, and accelerated atherosclerosis.3,33
The extent to which the mechanisms may interact is unknown.
Coronary thrombosis can
develop in the presence of normal or diseased coronary arteries, possibly as a
result of alterations in platelet and endothelial functions. Studies have
proven that cocaine increases human platelet activation and aggregation.
Additionally, vascular spasm may cause damage to the endothelium, creating a
nidus for platelet aggregation and fibrin deposition and resulting in thrombus
formation.3,34
Coronary artery
vasoconstriction or spasm results from alpha-adrenergic stimulation and may
occur in patients without coronary artery disease. Although this mechanism is
not completely understood, it is known that it differs from Prinzmetal's
angina.3,34
Cocaine has sympathomimetic
effects that induce tachycardia and hypertension, resulting in an increased
myocardial-oxygen demand. When this demand exceeds the supply, myocardial
ischemia occurs. These sympathomimetic effects most likely act synergistically
with other mechanisms to cause ischemia and are exacerbated by concomitant
cigarette smoking.3,34
Chronic use of cocaine may
lead to premature atherosclerosis. In autopsies, coronary atherosclerosis has
been found with increased prevalence in young cocaine users compared with
age-matched non-using controls.3,34,35
The differential diagnosis of
cocaine-associated chest pain is similar to that of chest pain unrelated to
cocaine use, but may vary depending on the route by which the drug was
ingested. The smoking of crack cocaine has been associated with alveolar
rupture resulting in pneumothorax, pneumopericardium, and pneumomediastinum.
An ailment known as "crack lung syndrome," which involves pulmonary
hemorrhage, chest pain, pulmonary edema, and an interstitial lung process, can
occur. In addition, asthma, pneumonia, and pulmonary vascular disease must be
considered. In patients using IV cocaine, endocarditis should be ruled out,
especially if the patient also has fever. Finally, although it is a rare
condition, aortic dissection must be considered in any patient with chest pain
and a history of cocaine use because of the high mortality rate of roughly 27%.
3,33
EKG interpretation in patients
with cocaine-induced chest pain is problematic. Approximately 60% of patients
with cocaine-induced MI have a nondiagnostic EKG, and 56% to 84% of patients
with cocaine-associated chest pain have abnormalities present on EKG. Thus, in
cocaine users, MI cannot be ruled out in the setting of a normal initial EKG,
nor can it be concluded that a patient needs reperfusion therapy if
abnormalities are present on EKG.3,33
The most useful diagnostic
tool for detecting cardiac injury in this patient population is serum
biochemical markers. Cardiac troponin I and T are the most specific, and are
preferred. Elevations in creatine kinase (CK) and CK-MB occur in the absence
of myocardial ischemia due to cocaine-induced skeletal-muscle injury. It has
been reported that, after using cocaine, approximately half of patients have
elevated serum CK with or without myocardial injury.33,36
Urine drug testing also may be
useful, especially in patients who initially deny using cocaine. The
metabolite benzoylecgonine can be detected for up to 48 to 72 hours after
cocaine use.33
Treatment
The treatment of
patients with cocaine-related ischemia or MI varies only slightly from the
traditional treatment of ACS. All patients should be administered oxygen and
placed on a cardiac monitor. Based on extensive investigation in patients with
ischemic heart disease unrelated to cocaine, a favorable safety profile, and
theoretical considerations, aspirin should be given to prevent the formation
or extension of thrombi if there are no contraindications (i.e., allergy or
suspected subarachnoid hemorrhage).33,36
Initial therapy also should
include nitroglycerin. Nitroglycerin has been shown to reduce infarct-related
complications and limit the extent of acute MI in patients with ischemia
unrelated to cocaine. Studies also indicate that nitroglycerin alleviates
cocaine-induced vasoconstriction and relieves symptomatic chest pain.
37-39
Benzodiazepines, in particular
lorazepam, also have established benefits. Early use may decrease cocaine's
cardiovascular toxicity by decreasing its central stimulatory effects.40
The combination of lorazepam plus nitroglycerin appears to be more
efficacious than either agent alone for relieving chest pain associated with
cocaine use.41 The same was not proven for diazepam in a similar
study, however.42
Although they are used in the
treatment of coronary ischemia that is not related to cocaine use,
beta-blockers are contraindicated for cocaine-associated ischemia. Presumably
through unopposed alpha-adrenergic stimulation, beta-blockers enhance coronary
vasoconstriction and increase blood pressure.3,43 They also
increase the likelihood of seizures and may decrease survival.40
Although labetalol has been used safely in some patients, it is not
recommended based on controlled studies performed in animals and humans.
Labetalol has combined alpha-beta antagonism, but the beta antagonism is far
more potent.33,40
Owing to conflicting data, the
role of calcium-channel blockers in the treatment of cocaine-associated
ischemia has not been established. Cardiac-catheterization studies in patients
with cocaine-induced coronary vasoconstriction found that verapamil reverses
the vasoconstrictive effects of cocaine, but large-scale clinical trials have
shown no benefit in acute MI unrelated to cocaine use.33,44 The
American College of Cardiology/American Heart Association's 2007 guidelines
for the management of patients with unstable angina/nonñST-elevation MI
recommend calcium-channel blockers in combination with nitroglycerin for
patients with chest pain after cocaine use.37
Phentolamine, an
alpha-adrenergic antagonist, also can be used to achieve vasodilation in
patients who continue to have chest pain after administration of oxygen,
aspirin, benzodiazepines, and nitrogly!=cerin.33 One case report
describes a 38-year-old man with cocaine-associated chest pain refractory to
oxygen, diazepam, and nitroglycerin that resolved after low-dose phentolamine.
45 To avoid hypotension while maintaining the anti-ischemic effects,
phentolamine 1 mg was recommended for such patients.45
Thrombolytic therapy should be
considered in patients having ST-segment elevation MI only when cardiac
catheterization is impossible. Although cocaine's known thrombogenic
properties make thrombolytic therapy attractive in theory, adverse outcomes
have been documented in several case reports. When it is balanced against the
low mortality seen in patients with cocaine-associated MI, thrombolytic
therapy's risks most likely outweigh its benefits in this patient population.
33
Secondary Prevention
The key to
secondary prevention of cocaine-related chest pain is the cessation of cocaine
use. Sadly, 60% of patients use cocaine again during the year following an
episode of chest pain.46 Cocaine-related death, MI, and recurrent
chest pain are extremely rare in patients who stop using cocaine. Tobacco
should be avoided as well, as it is a major contributor to the risk for
coronary artery disease; it also is associated with a faster onset of chest
pain and vasoconstriction after cocaine use.47 Patients likely will
benefit from modification of other traditional risk factors for heart disease
such as high cholesterol, high blood pressure, and obesity. The use of aspirin
to prevent platelet aggregation also may be beneficial for secondary
prevention. The role of calcium-channel blockers and nitrates remains
unproven, and beta-blockers should be avoided in any patient who may use
cocaine again.46,47
REFERENCES
1. Office of
National Drug Control Policy. Drug Facts. Cocaine. Available at:
www.whitehousedrugpolicy.gov/drugfact/cocaine/index.html. Accessed October 24,
2007.
2. Brody SL, Slovis CM,
Wrenn KD. Cocaine-related medical problems: consecutive series of 233
patients. Am J Med. 1990;88:325-331.
3. Levis JT, Garmel GM.
Cocaine-associated chest pain. Emerg Med Clin North Am.
2005;23:1083-1103.
4. Gay GR, Inaba DS,
Sheppard CW, Newmeyer JA. Cocaine: history, epidemiology, human pharmacology,
and treatment. A perspective on a new debut for an old girl. Clin Toxicol
. 1975;8:149-178.
5. Van Dyke C, Byck R.
Cocaine. Sci Am. 1982;246:128-141.
6. Boghdadi MS, Henning
RJ. Cocaine: pathophysiology and clinical toxicology. Heart Lung.
1997;26:466-483.
7. US Food and Drug
Administration. Federal Food and Drugs Act of 1906 (the "Wiley Act").
Available at: www.fda.gov/opacom/lawswileyact.htm. Accessed October 24, 2007.
8. US Drug Enforcement
Administration (DEA). Cocaine. Available at:
www.usdoj.gov/dea/concern/cocaine.html. Accessed November 7, 2007.
9. US DEA. Drugs of
abuse. Chapter 1. The Controlled Substances Act (CSA). Available at:
www.usdoj.gov/dea/pubs/abuse/1-csa.htm. Accessed October 24, 2007.
10. Warner EA. Cocaine
abuse. Ann Intern Med. 1993;119:226-235.
11. Lange RA, Hillis D.
Cardiovascular complications of cocaine use. N Engl J Med.
2001;345:351-358.
12. Egred M, Davis GK.
Cocaine and the heart. Postgrad Med J. 2005;81:568-571.
13. Brogan WC, Lange
RA, Glamann DB, Hillis LD. Recurrent vasoconstriction caused by intranasal
cocaine: possible role for metabolites. Ann Int Med. 1992;116:556-561.
14. Om A, Ellahham S,
Omato JP. Medical complications of cocaine: possible relationship to low
plasma cholinesterase enzyme. Am Heart J. 1993;125:1114-1117.
15. Hoffman RS, Henry
GC, Howland MA, et al. Association between life-threatening cocaine toxicity
and plasma cholinesterase activity. Ann Emerg Med. 1992;21:247-253.
16. Kolodgie FD, Farb
A, Virmani R. Pathobiological determinants of cocaine-associated
cardiovascular syndromes. Hum Pathol. 1995;26:583-586.
17. McCance EF, Price
LH, Kosten TR, Jatlow PI. Cocaethylene: pharmacology, physiology and
behavioral effects in humans. J Pharmacol Exp Ther. 1995;274:215-223.
18. Perez-Reyes M.
Subjective and cardiovascular effects of cocaethylene in humans.
Psychopharmacology (Berlin). 1993;113:144-147.
19. Harris DS, Everhart
ET, Mendelson J, Jones RT. The pharmacology of cocaethylene in humans
following cocaine and ethanol administration. Drug Alcohol Depend.
2003;72:169-182.
20. FarrÈ M, de la
Torre R, Llorente M, et al. Alcohol and cocaine interactions in humans. J
Pharmacol Exp Ther. 1993;266:1364-1373.
21. Xu Y, Crumb WJ,
Clarkson CW. Cocaethylene, a metabolite of cocaine and ethanol, is a potent
blocker of cardiac sodium channels. J Pharmacol Exp Ther.
1994;271:319-325.
22. Henning RJ, Wilson
LD. Cocaethylene is as cardiotoxic as cocaine but is less toxic than cocaine
plus ethanol. Life Sci. 1996;59:615-627.
23. Randall T. Cocaine,
alcohol mix in body to form even longer lasting, more lethal drug. JAMA
. 1992;267:1043-1044.
24. Lepere B, Charbit
B. Cardiovascular complications of cocaine use: recent points on cocaethylene
toxicity. Ann Med Interne (Paris). 2002;153(suppl 3):1S45-1S46.
25. Catterall WA,
Mackie K. Local anesthetics. In: Brunton LL, Lazo JS, Parker KL, eds.
Goodman and Gilman's The Pharmacological Basis of Therapeutics. 11th ed.
New York, NY: McGraw Hill Inc; 2006:369-386.
26. Krendel DA, Ditter
SM, Frankel MR, Ross WK. Biopsy-proven cerebral vasculitis associated with
cocaine abuse. Neurology. 1990;40:
1092-1094.
27. Niazi M, Kondru A,
Levy J, Bloom AA. Spectrum of ischemic colitis in cocaine users. Dig Dis Sci
. 1997;42:1537-1541.
28. Haim DY, Lippmann
ML, Goldberg SK, Walkenstein MD. The pulmonary complications of crack cocaine.
A comprehensive review. Chest. 1995;107:233-240.
29. Ness RB, Grisso JA,
Hirschinger N, et al. Cocaine and tobacco use and the risk of spontaneous
abortion. N Engl J Med. 1999;340:333-339.
30. Daras M, Tuchman
AJ, Marks S. Central nervous system infarction related to cocaine abuse.
Stroke. 1991;22:1320-1325.
31. Roth D, AlarcÛn FJ,
Fernandez JA, et al. Acute rhabdomyolysis associated with cocaine
intoxication. N Engl J Med. 1988;319:673-677.
32. Hoffman RS,
Hollander JE. Evaluation of patients with chest pain after cocaine use.
Crit Care Clin. 1997;13:809-828.
33. Hollander JE, Henry
TD. Evaluation and management of the patient who has cocaine-associated chest
pain. Cardiol Clin. 2006;24:103-114.
34. Mouhaffel AH, Madu
EC, Satmary WA, Fraker TD. Cardiovascular complications of cocaine. Chest
. 1995;107:1426-1434.
35. Eichhorn EJ,
Peacock E, Grayburn PA, et al. Chronic cocaine abuse is associated with
accelerated atherosclerosis in human coronary arteries. J Am Coll Cardiol
. 1992;19(suppl):105A.
36. Hollander JE,
Hoffman RS, Gennis P, et al. Prospective multicenter evaluation of
cocaine-associated chest pain. Acad Emerg Med. 1994;1:330-339.
37. Anderson JL, Adams
CD, Antman EM, et al. ACC/AHA 2007 guidelines for the management of patients
with unstable angina/nonñST-elevation myocardial infarction. J Am Coll
Cardiol. 2007;50:e1-e157.
38. Brogan WC, Lange
RA, Kim AS, et al. Alleviation of cocaine-induced coronary vasoconstriction by
nitroglycerin. J Am Coll Cardiol. 1991;18:581-586.
39. Hollander JE,
Hoffman RS, Gennis P, et al. Nitroglycerin in the treatment of cocaine
associated chest pain--clinical safety and efficacy. J Toxicol Clin Toxicol
. 1994;32:243-256.
40. Hollander JE. The
management of cocaine-associated myocardial ischemia. N Engl J Med.
1995;333:1267-1272.
41. Honderick T,
Williams D, Seaberg D, Wears R. A prospective, randomized, controlled trial of
benzodiazepines and nitroglycerine or nitroglycerine alone in the treatment of
cocaine-associated acute coronary syndromes. Am J Emerg Med.
2003;21:39-42.
42. Baumann BM, Perrone
J, Hornig SE, et al. Randomized, double-blind, placebo-controlled trial of
diazepam, nitroglycerin, or both for treatment of patients with potential
cocaine-associated acute coronary syndromes. Acad Emerg Med.
2000;7:878-885.
43. Lange RA, Cigarroa
RG, Flores ED, et al. Potentiation of cocaine-induced coronary
vasoconstriction by beta-adrenergic blockade. Ann Intern Med.
1990;112:897-903.
44. Negus BH, Willard
JE, Hillis LD, et al. Alleviation of cocaine induced coronary vasoconstriction
with intravenous verapamil. Am J Cardiol. 1994;73:510-513.
45. Hollander JE,
Carter WA, Hoffman RS. Use of phentolamine for cocaine-induced myocardial
ischemia. N Eng J Med. 1992;327-361.
46. Hollander JE,
Hoffman RS, Gennis P, et al. Cocaine-associated chest pain: one year
follow-up. Acad Emerg Med. 1995;2:179-184.
47. Hollander JE, Thode
HC, Hoffman RS. Chest discomfort, cocaine and tobacco.
Acad Emerg Med. 1995;2:238.
To comment on this
article, contact
editor@uspharmacist.com.





