USPharm. 2018;43(4):19-26.
ABSTRACT: With international travel increasing in past decades, pharmacists should be informed and stay up-to-date on the most pertinent travel-health information available. Preventive measures including prescriptions and other nonpharmacologic therapies are available to reduce the risk of acquiring an infectious disease while traveling internationally. Pharmacists in the community may be the last line of medication information and counseling available to the patient before travel, and they may be asked for recommendations about medications and OTC products to prevent travel-related illnesses such as traveler’s diarrhea, cholera, typhoid fever, malaria, and Zika.
International travel has dramatically increased in past decades, with over 80 million trips booked by Americans in 2016—8% more than in 2015.1 Travelers should consult a medical professional weeks to months prior to international travel, especially when traveling to a tropical, subtropical, or developing country, in order to receive proper counseling and any prophylactic medications or vaccinations that may be recommended.2 This article will focus on information pertinent to pharmacists in the United States in order to field questions about causes, preventive measures, and available treatment options for the most common travel-related illnesses that patients may experience abroad.
Important information to obtain from a patient seeking medical travel advice includes the travel destination, reason for travel (e.g., medical mission trip, work, or leisure), duration of travel, itinerary, and patient-specific health concerns.2 Pharmacists can consult the CDC Travelers’ Health website for specific recommendations.3 Pharmacists may also be instrumental in helping patients locate a travel-medicine clinic. The International Society of Travel Medicine has an online directory of available travel-medicine clinics, which can be searched by state in order to locate the nearest clinics.4
Travel Vaccinations
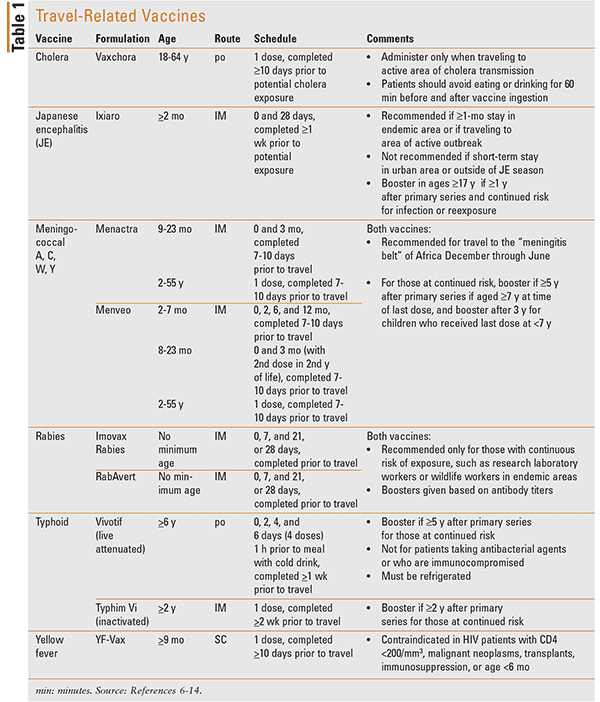
Many diseases that travelers may be at higher risk for can be prevented with vaccinations.5 Common routine vaccinations given at pretravel appointments include influenza, hepatitis A, hepatitis B, and tetanus, diphtheria, and pertussis. Specific travel-related vaccines should be administered based on risk of infection, patient-specific factors, and travel itinerary; further details about available travel vaccines may be found in Table 1.6-14 Many insurance companies do not cover the cost of travel vaccinations, so patients should contact a local travel-medicine clinic for specific information on pricing.
Prevention of Food and Waterborne Disease
Precautionary safety measures during travel are of utmost importance in preventing infectious diseases. Paying close attention to hygiene practices in international restaurants and avoiding places with poor hygiene practices are important. Travelers should avoid eating raw or undercooked foods, including meats, seafood, and raw fruits and vegetables, unless cooked or peeled by the traveler personally. Travelers should avoid purchasing foods and beverages from street vendors, drinking tap water and unpasteurized milk, and consuming ice and dairy products. Any water used for drinking or brushing teeth should either come from an unopened bottle or be boiled prior to use. Hand washing with soap and water should be practiced routinely while traveling abroad. Alcohol-based sanitizers may be used if soap and water are unavailable.15
Traveler’s Diarrhea
Traveler’s diarrhea (TD) is the most common travel-related illness and is caused by consuming fecally contaminated food or water. TD is defined as three or more unformed stools within 24 hours plus one of the following symptoms: abdominal cramping, nausea, vomiting, fever, or fecal urgency. More than 80% of TD cases are caused by bacterial organisms, such as Escherichia coli, Campylobacter jejuni, Shigella spp., or Salmonella spp., but may also be caused by viral or protozoal infections. Norovirus is often associated with outbreaks in patients traveling on cruise ships. A higher incidence of TD is seen in patients traveling to countries in Central and South America, Asia, Africa, Mexico, and the Middle East.16
Symptoms of TD can be mild, with some cramping and loose stools, or severe, with fever, bloody stools, vomiting, and intense abdominal pain. The food and water safety measures previously discussed should be practiced to prevent TD. Bismuth subsalicylate (BSS) has been studied, with success shown in reducing the risk of TD by approximately 50%. In patients wishing to use BSS for prophylaxis, proper counseling about the potential of BSS to blacken the tongue and stool is important. BSS prophylaxis should not be used in pregnant patients or children aged less than 3 years. Additionally, those who have an aspirin allergy, renal dysfunction, or a prescription for an anticoagulant should avoid BSS. Importantly, prophylactic antibiotic therapy is not indicated to prevent TD in most travelers because this practice may lead to further antibiotic resistance.16
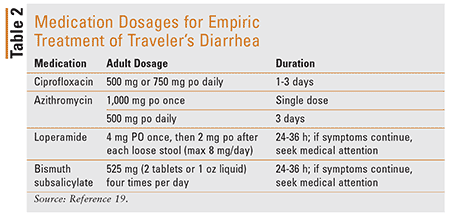
Counseling should be provided to patients about increasing oral fluid intake in the event of a TD episode during travel. Antimotility medications such as loperamide (maximum 8 mg per day) or BSS may be used to reduce the number of stools per day and allow patients to continue with travel plans. Antidiarrheals should be used only in patients who do not have concomitant fever or blood in the stool and who are not pregnant.16 Antibiotics may be used to reduce the duration of moderate-to-severe TD. Azithromycin or fluoroquinolone antibiotics are recommended empiric therapy for infectious diarrhea.17 Importantly, fluoroquinolones should not be used in cases of bloody diarrhea.16 Additionally, fluoroquinolone resistance is increasing throughout the world, so these agents are no longer the preferred treatment options in some locations, as outlined on the CDC website.3 Azithromycin is preferred in patients who are pregnant.18 Single doses of antibiotics have been shown to be as efficacious as multidoses and are also more convenient for patients traveling abroad (Table 2).19
Typhoid
Typhoid and paratyphoid fever, also known as enteric fever, are bacterial infections caused by Salmonella enterica. Southern and Southeast Asia, as well as Africa, are the highest-risk regions for enteric fever. The Caribbean, East Asia, and South America are areas with a lower risk. Typhoid typically presents as a low fever in the morning followed by higher fever in the evening. Typhoid symptoms may last up to 1 month if left untreated, and complications associated with typhoid, such as intestinal perforation and hemorrhage, may present after several weeks of untreated illness.13
Two vaccines are available for typhoid in the U.S.13 Destination-specific vaccine recommendations may be found on the CDC Travelers’ Health website.3 The traditional therapy of choice for enteric fever has been fluoroquinolone antibiotics; however, increasing resistance has been seen across the globe, especially in Southern and Southeast Asia. Third-generation cephalosporins and azithromycin are often used instead of fluoroquinolones owing to this resistance. After antibiotic initiation, patients could continue to spike fevers for several days, with an initial worsening of symptoms.13
Cholera
Cholera is an infectious disease caused by a bacterium, toxigenic Vibrio cholerae. The highest incidence of cholera is found in regions of Africa and Southern and Southeast Asia. Cholera outbreaks have also been reported in parts of the Caribbean. Cholera typically presents as mild, watery diarrhea without fever and may also be asymptomatic. However, some patients may experience severe, profuse, watery diarrhea that appears like “rice-water stools.” This form of cholera may lead to very severe dehydration, shock, or even death if left untreated.7
Owing to high quantities of fluid loss, aggressive rehydration is the key to treating patients with active cholera infections. Oral rehydration therapy may be used to treat moderate dehydration; however, IV fluids are needed in severe cases. Doxycycline is the agent of choice for adult patients in the majority of the world, and azithromycin is the treatment option preferred in pregnant women and children.7 Other options for treatment include ceftriaxone or fluoroquinolone antibiotics, with increasing resistance to fluoroquinolones in many parts of the world.7,17 In addition to safety precautions, an oral vaccine is now available in the U.S. for adults (ages 18-64) traveling to areas of active transmission of cholera. Currently, there are no safety or efficacy data for booster doses of the cholera vaccine.20
Prevention of Insect-Borne Disease
Prophylactic medications and vaccinations are available in the U.S. to prevent vectorborne diseases. Lightweight long-sleeved shirts, long pants, closed-toe shoes, and hats should be worn when possible to minimize the amount of exposed skin. Permethrin may be used to treat clothing or gear but should not be applied directly to the skin. Any exposed skin should be treated with a mosquito repellent. Many commercially available insect repellents are EPA-registered, including DEET, picaridin, oil of lemon eucalyptus, and para-menthane-3,8-diol. Repellents containing less than 10% of the active ingredient are only minimally protective (providing coverage for 1-2 hours). Repellents should not be sprayed directly to the face, under clothing, or on cuts or irritated skin. Combination sunscreen and repellent products are not recommended by the CDC. In addition to wearing proper clothing and using insect repellents, travelers should sleep in screened-in and/or air-conditioned rooms as well as under an insecticide-pretreated bed net.21
Malaria
Malaria is a significant cause of morbidity and mortality in patients traveling internationally.2 Malaria is caused by the Plasmodium parasite and transmitted by the Anopheles mosquito in areas of Africa, Asia, and Central and South America. Different species of Plasmodium are seen throughout the world, and each species and region have unique susceptibility to antimalarial agents. The CDC separates geographical regions into chloroquine-sensitive or chloroquine-resistant malaria, which helps physicians in choosing appropriate prophylaxis or treatment.22
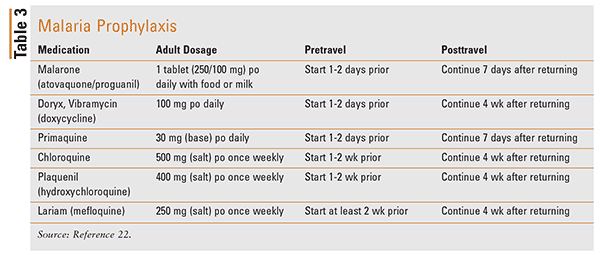
Malaria prophylaxis should be prescribed for patients traveling to high-risk areas and should be taken before, during, and after travel. The travel itinerary, remaining time before travel, age, weight, allergies, concomitant drug interactions, and pregnancy status are important factors to consider in order to choose the most appropriate prophylactic therapy for a patient. Several options for prophylaxis should be started 1 to 2 days prior to travel, while others must be started 1 to 2 weeks prior. In addition, the duration that prophylaxis must be continued post-travel is unique to each agent (Table 3). Patients who believe that they may have been infected with malaria while traveling should seek appropriate medical treatment as soon as possible. Treatment options depend on the severity of infection, area of travel, potential drug resistance, and patient-specific characteristics.22 The CDC provides guidelines for the treatment of malaria in the U.S.23
Zika
Zika is a viral infection that is transmitted by the Aedes mosquito. Zika virus was discovered in 1947 in Uganda; however, much attention has been focused on Zika in recent years owing to its association with severe effects on the fetuses of mothers infected with the virus. There are currently no available vaccinations or prophylactic therapies to prevent infection with Zika. Proper mosquito precautions are important for preventing the illness. The majority of patients infected with Zika remain asymptomatic, and any symptomatic infections are often mild and flulike. Supportive care is the mainstay of therapy in patients with symptomatic Zika infections.24
An increased risk of microcephaly and other brain abnormalities in the fetus has been associated with Zika infection in pregnant women; therefore, the CDC recommends that pregnant women or those trying to become pregnant should not travel to areas of active local transmission.24 Other potential birth defects linked to Zika are neural tube defects such as anencephaly, congenital cataracts, spina bifida, and hearing loss.25 If travel to these areas cannot be avoided, the woman should speak with her healthcare provider and take very strict precautions to avoid mosquito bites. A male who has traveled to an area of local transmission should use condoms or abstain from sex with his partner, if the partner is pregnant, for the duration of the pregnancy. Couples wishing to conceive and who have recently traveled to an endemic area should first speak with a medical provider and wait until risks for transmission are minimized.24
Yellow Fever
Yellow fever (YF) is caused by a virus and is endemic to sub-Saharan Africa and the tropics of Central and South America. YF is transmitted via the bite of Aedes or Haemagogus spp. mosquitoes. During the rainy season, there is an increased risk of infection; however, transmission may still occur outside of these months. The majority of patients infected with YF remain asymptomatic or may have mild flulike symptoms. Approximately 15% of patients infected with YF will progress to severe disease with liver dysfunction, hemorrhage, shock, and ultimately multiorgan failure. Supportive care with fluids, analgesics, and antipyretics is the standard of care. Because of the increased risk of bleeding, aspirin and nonsteroidal anti-inflammatory drugs should not be used in patients with suspected or confirmed YF.14
YF prevention includes mosquito protection as well as the YF vaccine, which is a live attenuated vaccine. Some countries require proof of vaccination with the International Certificate of Vaccination or Prophylaxis, or “Yellow Card.” In 2014, the World Health Organization determined that a single dose of the YF vaccine provides lifelong immunity, so a 10-year booster is no longer needed for most patients.14 The Advisory Committee on Immunization Practices does recommend a one-time booster in patients who received their first vaccine while pregnant or who received a stem-cell transplant after the vaccination. Patients who are living with HIV should be given a booster every 10 years.26 Owing to potential serious adverse effects of the YF vaccine, only certain healthcare providers are certified to administer the vaccine.14 Information about providers who can administer the vaccine may be found via the CDC’s search engine.27
Conclusion
Preventive measures including prescriptions, vaccinations, and other nonpharmacologic therapies are available to reduce the risk of acquiring an infectious disease while traveling internationally. Pharmacists in the community may be the last line of medication information and counseling available to the patient before travel, and they may be asked for recommendations about medications and OTC products to prevent travel-related illnesses such as traveler’s diarrhea, cholera, typhoid fever, malaria, and Zika (sidebar). Pharmacists should be informed and stay up-to-date on the most pertinent travel health information.
REFERENCES
1. National Travel and Tourism Office. 2016 outbound analysis. December 4, 2017. https://travel.trade.gov/outreachpages/download_data_table/2016_Outbound_Analysis.pdf. Accessed January 29, 2018.
2. Chen LH, Hochberg NS, Magill AJ. The pretravel consultation. In: CDC. Travelers’ Health—Yellow Book. Chapter 2. The pretravel consultation. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/the-pre-travel-consultation/the-pre-travel-consultation. Accessed January 25, 2018.
3. CDC. Travelers’ health. wwwnc.cdc.gov/travel. Accessed January 26, 2018.
4. International Society of Travel Medicine. Online clinic directory. www.istm.org/AF_CstmClinicDirectory.asp. Accessed January 26, 2018.
5. Boggild AK, Castelli F, Gautret P, et al. Vaccine preventable diseases in returned international travelers: results from the GeoSentinel Surveillance Network. Vaccine. 2010;28(46):7389-7395.
6. Kroger AT, Strikas RA. General recommendations for vaccination & immunoprophylaxis. In: CDC. Travelers’ Health—Yellow Book. Chapter 2. The pretravel consultation. Updated June 13, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/the-pre-travel-consultation/general-recommendations-for-vaccination-immunoprophylaxis. Accessed January 25, 2018.
7. Wong KK, Burdette E, Mintz ED. Cholera. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/cholera. Accessed January 25, 2018.
8. Nelson NP. Hepatitis A. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated June 12, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/hepatitis-a. Accessed January 25, 2018.
9. Averhoff F. Hepatitis B. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated June 13, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/hepatitis-b. Accessed January 25, 2018.
10. Hills SL, Rabe IB, Fischer M. Japanese encephalitis. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/japanese-encephalitis. Accessed January 25, 2018.
11. MacNeil JR, Meyer SA. Meningococcal disease. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/meningococcal-disease. Accessed January 25, 2018.
12. Petersen BW, Wallace RM, Shlim DR. Rabies. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/rabies. Accessed January 25, 2018.
13. Judd MC, Mintz ED. Typhoid & paratyphoid fever. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/typhoid-paratyphoid-fever. Accessed January 25, 2018.
14. Gershman MD, Staples JE. Yellow fever. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/yellow-fever. Accessed January 25, 2018.
15. Connor BA. Food & water precautions. In: CDC. Travelers’ Health—Yellow Book. Chapter 2. The pretravel consultation. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/the-pre-travel-consultation/food-water-precautions. Accessed January 25, 2018.
16. Connor BA. Travelers’ diarrhea. In: CDC. Travelers’ Health—Yellow Book. Chapter 2. The pretravel consultation. Updated June 13, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/the-pre-travel-consultation/travelers-diarrhea. Accessed January 25, 2018.
17. Shane AL, Mody RK, Crump JA, et al. 2017 Infectious Diseases Society of America clinical practice guidelines for the diagnosis and management of infectious diarrhea. Clin Infect Dis. 2017;65:e45-e80.
18. Morof DF, Carroll D. Pregnant travelers. In: CDC. Travelers’ Health—Yellow Book. Chapter 8. Advising travelers with specific needs. Updated June 13, 2017.
wwwnc.cdc.gov/travel/yellowbook/2018/advising-travelers-with-specific-needs/pregnant-travelers. Accessed January 25, 2018.
19. Steffen R, Hill DR, Dupont HL. Traveler’s diarrhea: a clinical review. JAMA. 2015;313(1):71-80.
20. Advisory Committee on Immunization Practices. Summary report, February 24, 2016. Atlanta, GA: US Department of Health and Human Services, CDC. Advisory Committee on Immunization Practices; 2016. www.cdc.gov/vaccines/acip/meetings/downloads/min-archive/min-2016-02.pdf. Accessed January 31, 2018.
21. Mutebi J, Hawley WA, Brogdon WG. Protection against mosquitoes, ticks, & other arthropods. In: CDC. Travelers’ Health—Yellow Book. Chapter 2. The pretravel consultation. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/the-pre-travel-consultation/protection-against-mosquitoes-ticks-other-arthropods. Accessed January 25, 2018.
22. Arguin PM, Tan KR. Malaria. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated June 12, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/malaria. Accessed January 25, 2018.
23. CDC. Malaria diagnosis and treatment in the United States. Updated February 23, 2017. www.cdc.gov/malaria/diagnosis_treatment/treatment.html. Accessed January 25, 2018.
24. Chen T, Staples JE, Fischer M. Zika. In: CDC. Travelers’ Health—Yellow Book. Chapter 3. Infectious diseases related to travel. Updated May 31, 2017. wwwnc.cdc.gov/travel/yellowbook/2018/infectious-diseases-related-to-travel/zika. Accessed January 25, 2018.
25. Fitzgerald B, Boyle C, Honein MA. Birth defects potentially related to Zika virus infection during pregnancy in the United States. JAMA. January 25, 2018. https://jamanetwork.com/journals/jama/fullarticle/2671017. Epub ahead of print. Accessed January 25, 2018.
26. CDC. Yellow fever vaccine booster doses: recommendations of the Advisory Committee on Immunization Practices, 2015. MMWR. June 19, 2015. www.cdc.gov/mmwr/preview/mmwrhtml/mm6423a5.htm. Accessed January 30, 2018.
27. CDC. Search for yellow fever vaccination clinics. wwwnc.cdc.gov/travel/yellow-fever-vaccination- clinics/search. Accessed January 30, 2018.
To comment on this article, contact rdavidson@uspharmacist.com.