US Pharm. 2018;43(5):6-11.
More than 50 million Americans suffer from allergy, making it the sixth leading cause of chronic illness in the United States.1 Allergic rhinitis (AR) is one of the most common allergic diseases, and it is often under-recognized, misdiagnosed, and ineffectively treated, constituting a global health problem.2 Since the 1980s, the overall prevalence of AR has steadily risen.3 Current data suggest that up to 30% of adults and 40% of children suffer from AR, with healthcare costs in excess of $18 billion annually.2,4 AR is the 16th most common primary diagnosis for outpatient visits.5 The average number of prescriptions for patients with AR is almost double than that for patients without allergies.6
AR can have a negative impact on a patient’s quality of life. This condition leads to missed school and work days; it has been associated with poor sleep quality, impairment in work performance, decreased concentration in school, and overall decreased feelings of mental well-being.5,7,8 AR is rarely found in isolation and is associated with a number of comorbid conditions, including asthma, chronic otitis media, rhinosinusitis, and obstructive sleep apnea.9 If left untreated, AR can worsen comorbidities.
It is important for pharmacists to have a thorough understanding of AR and the options available for its management. Many times, identification and treatment of AR begin at the pharmacy counter; pharmacists play a pivotal role in the management of this condition, guiding treatment based on patients’ symptoms and severity.
Pathophysiology
AR is an immunoglobulin E–mediated inflammatory response of the nasal mucous membranes and upper respiratory tract following exposure to aeroallergens that the patient has been previously sensitized to.10 This reaction can be divided into two phases: the immediate or early-phase response and the late-phase response.
Early-Phase Response: Upon immediate exposure to an inhaled allergen, mast cell degranulation occurs, causing the release of preformed mediators, such as histamines, prostaglandins, and leukotrienes.10,11 These newly released mediators bind to nasal receptors, causing many of the manifestations of AR within minutes of exposure, which include nasal itching, sneezing, rhinorrhea, and some degree of nasal congestion.10
Late-Phase Response: A late-phase response can occur in up to half of AR sufferers 4 to 8 hours after the initial allergen exposure.10 This reaction is characterized by eosinophil chemotaxis, which is caused by the same proinflammatory mediators produced in the early phase.10,11 Clinically, patients will experience a prolongation of symptoms such as sneezing and rhinorrhea, but the most predominant manifestation is nasal congestion that is often severe and long-lasting.10,11
Clinical Presentation
As described above, patients will typically present with rhinorrhea, sneezing, nasal congestion, and itching of the eyes, ears, nose, and throat. Up to 70% of patients will also experience allergic conjunctivitis, which is characterized by intense eye itching, swelling, and discharge.12 Many of the signs and symptoms of the common cold overlap with AR; ocular itching is often a hallmark of allergy, while an accompanying sore throat, fever, and body aches are indicative of an infectious etiology.13,14
Classification
AR can be classified according to the temporal pattern of exposure to allergens, frequency of symptoms, or severity.15 Traditionally, the temporal pattern has been used. Temporal patterns may be seasonal, perennial, or episodic. When the FDA approves new medications for AR, they are classified as either seasonal or perennial. Seasonal AR (SAR) has a seasonal variation and is dependent on geographic location and climatic conditions; trees, grass, weed pollens, and outdoor mold spores are common triggers.5,15 Perennial AR (PAR) is attributed to exposure to year-round environmental aeroallergens, including dust mites, mold, animal dander, and certain occupational allergens.5 Episodic AR describes allergic nasal symptoms in patients who have sporadic exposure to aeroallergens that are not typically encountered in their usual indoor or outdoor environments.5 The SAR and PAR distinctions do have some limitations because some allergens that are considered seasonal can be considered perennial in certain climates and conditions.
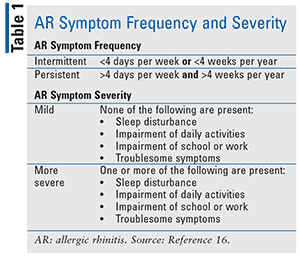
Alternatively, a patient’s symptoms can be classified according to severity and frequency, allowing for more appropriate treatment selection.5 AR symptom frequency is divided into intermittent and persistent categories; AR severity is classified as mild or more severe (Table 1).16
Management Strategies
There is currently no cure for AR. The goals of therapy include symptom relief, minimizing sleep disturbances, improving work and school performances, and improving quality of life. One of the most important strategies is the prevention or avoidance of environmental triggers, although this is not always practical and is often difficult to achieve.5,15,17 A successful treatment plan will incorporate both nonpharmacologic strategies and pharmacologic therapy for the management and prevention of AR symptoms. There are many self-care options available to help with AR symptom relief. OTC medications include intranasal corticosteroids, antihistamines, decongestants, and mast-cell stabilizers.
Intranasal Corticosteroids
Intranasal corticosteroids are the most potent and effective medications for the treatment of AR. They are potent anti-inflammatory agents that are effective for relieving all symptoms of AR, including sneezing, rhinorrhea, nasal congestion, nasal itching, and ocular symptoms.5 This relief has been seen with both continuous and as-needed use; however, as-needed use may not be as effective as continuous use.5,15 It is important to educate patients about the onset of action of these agents; the onset of action after the first dose ranges anywhere from 3 to 36 hours, but it may take up to 1 week for patients to experience full relief.5 By improving symptoms, these agents significantly improve the quality of life of patients with AR.5
The efficacy and adverse-event profiles of all intranasal corticosteroids are similar among available formulations; when recommending an agent, factors including product sensory attributes—such as aftertaste, nose runout, throat rundown, and smell—and each medication’s distinct physicochemical properties should be considered.5,18 Generally, the intranasal corticosteroids are well tolerated. The most common adverse effects are a result of local mucosal irritation and include dryness, burning, stinging, and epitaxis; in rare cases, nasal septal perforation can occur.5
Antihistamines
Antihistamines are recommended for patients with AR who have primary complaints of sneezing and itching, but they have little effect on congestion.5 They are categorized as first- and second-generation agents.
First-generation antihistamines, which include diphenhydramine and chlorpheniramine, are highly lipophilic and cross the blood-brain barrier easily, thus contributing to adverse central-nervous system effects including sedation, drowsiness, and decreased cognitive processing.19 Because of their anticholinergic profile, they should be avoided in the elderly population.20 In young children, diphenhydramine has been associated with paradoxical excitation, resulting in irritability, hyperactivity, and insomnia.19
Second-generation antihistamines are lipophobic and have poor penetration of the blood-brain barrier; they are less likely to be sedating than first-generation drugs.19 These agents include cetirizine, desloratadine, fexofenadine, levocetirizine, and loratadine. Second-generation antihistamines have longer half-lives, permitting once- or twice-daily dosing compared with first-generation antihistamines, which have relatively short half-lives, necessitating multiple daily doses.19 Second-generation agents are generally nonsedating; however, cetirizine and levocetirizine carry a modest risk of sedation. Overall, second-generation antihistamines are preferred over first-generation agents on the basis of safety and efficacy data.5,15,17 For best results, antihistamines should be taken either prophylactically 2 to 5 hours before allergen exposure or on a regular basis, rather than as needed.19
Decongestants
Systemic and topical decongestants are effective in AR patients who experience nasal congestion. They work by stimulating the alpha-adrenergic receptors to constrict dilated arteries within the nasal mucosa.21
The two systemic decongestants available in the U.S., pseudoephedrine and phenylephrine, are both nonprescription medications. Oral pseudoephedrine appears to relieve nasal congestion more effectively than phenylephrine.22,23 Systemic decongestants are generally well tolerated and relatively safe, but their use is associated with adverse effects resulting from stimulation of the central nervous system. Common adverse effects include insomnia, increased blood pressure, tachycardia, palpitations, arrhythmias, hallucinations, and urinary dysfunction.24 Their use should be avoided in patients with uncontrolled hypertension, thyroid disease, diabetes, and benign prostatic hypertrophy.24
Topical decongestants such as oxymetazoline provide a local effect at the nasal mucosal, limiting the occurrence of systemic adverse effects. These agents should only be used episodically and never for more than 3 to 5 days to avoid the occurrence of rhinitis medicamentosa or rebound congestion.25
Mast-Cell Stabilizers
The use of intranasal cromolyn sodium is considered a second-line agent in the management of allergic rhinitis; it is less effective than antihistamines and intranasal corticosteroids.21 Mast-cell stabilizers inhibit the influx of calcium into the mast cell, preventing mediator release of the allergic response and inflammation.26 If degranulation has already occurred, cromolyn will have no effect; it is more useful as a preventive agent rather than as treatment.26
Conclusion
Pharmacists play an integral role in the management of AR. This is a condition that can significantly affect a patient’s quality of life. Management strategies should include the combination of allergen avoidance and pharmacotherapy. Treatment should be individualized based on the frequency and severity of bothersome symptoms. With appropriate questioning and education, pharmacists can aid the patient in achieving optimum symptom control.
Patient Information
What Options May Help Relieve My Symptoms?
There is no cure for allergic rhinitis. However, it can be managed with allergen avoidance and treatment with a variety of medications.
Avoiding Allergens
You can help control your symptoms by reducing your exposure to allergens. If you have seasonal allergies, stay indoors when the pollen count is high. Keep windows and doors shut at home and in your car during allergy season. Take a shower, wash your hair, and change your clothes after you’ve been outdoors.
If you have dust mite allergies, use pillow and mattress covers. Wash your sheets and bedding in hot water every week. Use a vacuum cleaner with a HEPA filter. Try to keep your indoor humidity at about 40%.
If you are allergic to animals, the most effective treatment is removing the pet from the home. If this is not possible, avoid having the pet spend time in your bedroom. Washing your pets at least twice a week may also help reduce allergen levels.
You may also find that rinsing your nasal passages with a saltwater solution may help relieve throat irritation, nasal dryness, and nasal congestion.
OTC Treatment Options
Consult a healthcare provider for assistance in selecting an OTC allergy medication that treats your most bothersome symptoms.
Intranasal corticosteroids are the most effective treatments available for relief of symptoms. Improvement can be seen almost immediately, but it may take up to 7 days to feel full relief. Most common side effects include bad taste, dry nose, and unpleasant smell. When using intranasal corticosteroids, be sure to spray away from the septum to prevent nosebleeds. Ask your pharmacist about the proper technique to administer nasal mediations.
Antihistamines help with the sneezing, itchy, and runny nose but will not help with nasal congestion. You may find better relief if you combine these agents with an intranasal corticosteroid or decongestant. Use a nondrowsy product such as Allegra (fexofenadine), Claritin (loratadine), Xyzal (levocetirizine), or Zyrtec (cetirizine). Do not take this medication without consulting a doctor or pharmacist if you are over age 65 years, have glaucoma, difficulty urinating, prostate enlargement, thyroid disorders, or other medical conditions.
Nasal and oral decongestants can help provide relief from nasal congestion. Nasal decongestants such as Afrin (oxymetazoline) should not be used for more than 3 days because you can become dependent on them, causing more nasal congestion. Oral decongestants such as Sudafed (pseudoephedrine) can raise your blood pressure and make you feel jittery. They may also cause insomnia if taken too close to bedtime. These drugs should not be taken if you have uncontrolled hypertension, heart disease, closed-angle glaucoma, hyperthyroid, or are on certain medications.
Mast-Cell Stabilizer: Cromolyn sodium is available as a nasal spray. This product is most useful when used to prevent an allergic reaction. It will not do much to relieve your symptoms if you are already suffering from symptoms. This agent may take up to 2 weeks to have an effect.
When to Seek Medical Attention
You should seek medical help when your allergy symptoms worsen while you are taking any nonprescription medication or do not decrease after 2 to 4 weeks of therapy. You should also seek medical attention if you develop signs and symptoms of a secondary bacterial infection, such as thick nasal or respiratory secretions that are not clear, oral temperature higher than 101.5°F, shortness of breath, chest congestion, wheezing, significant ear pain, and rash.
REFERENCES
1. CDC. Gateway to health communication and social marketing practice. Allergies. March 26, 2018. www.cdc.gov/healthcommunication/toolstemplates/entertainmented/tips/Allergies.html. Accessed April 10, 2018.
2. Meltzer EO, Blaiss MS, Naclerio RM, et al. Burden of allergic rhinitis: allergies in America, Latin America, and Asia-Pacific adult surveys. Allergy Asthma Proc. 2012;33(Suppl 1):S113-S141.
3. Meltzer EO, Gross GN, Katial R, Storms WW. Allergic rhinitis substantially impacts patient quality of life: findings from the Nasal Allergy Survey Assessing Limitations. J Fam Pract. 2012;61(2 Suppl):S5-S10.
4. American College of Allergy, Asthma and Immunology. Allergy facts. January 16, 2015. https://acaai.org/news/facts-statistics/allergies. Accessed April 10, 2018.
5. Seidman MD, Gurgel RK, Lin SY, et al. Clinical practice guideline: allergic rhinitis. Otolaryngol Head Neck Surg. 2015;152(1 Suppl):S1-S43.
6. Bhattacharyya N. Incremental healthcare utilization and expenditures for allergic rhinitis in the United States. Laryngoscope. 2011;121(9):1830-1833.
7. Mir E, Panjabi C, Shah A. Impact of allergic rhinitis in school going children. Asia Pac Allergy. 2012;2(2):93-100.
8. Dykewicz MS, Hamilos DL. Rhinitis and sinusitis. J Allergy Clin Immunol. 2010;125(Suppl 2):S103-S115.
9. Hadley JA, Derebery MJ, Marple BF. Comorbidities and allergic rhinitis: not just a runny nose. J Fam Pract. 2012;61(2 Suppl):S11-S15.
10. Skoner DP. Allergic rhinitis: definition, epidemiology, pathophysiology, detection, and diagnosis. J Allergy Clin Immunol. 2001;108(1 Suppl):S2-S8.
11. Min Y-G. The pathophysiology, diagnosis and treatment of allergic rhinitis. Allergy Asthma Immunol Res. 2010;2(2):65-76.
12. Greiner AN, Hellings PW, Rotiroti G, Scadding GK. Allergic rhinitis. Lancet Lond Engl. 2011;378(9809):2112-2122.
13. Allan GM, Arroll B. Prevention and treatment of the common cold: making sense of the evidence. CMAJ. 2014;186(3):190-199.
14. dePietro M. Cold or allergies? How to tell the difference. Medical News Today. www.medicalnewstoday.com/articles/315756.php. Accessed April 17, 2018.
15. Dykewicz MS, Wallace DV, Baroody F, et al. Treatment of seasonal allergic rhinitis: an evidence-based focused 2017 guideline update. Ann Allergy Asthma Immunol. 2017;119(6):489-511.e41.
16. Bousquet J, Van Cauwenberge P, Khaltaev N, Aria Workshop Group, World Health Organization. Allergic rhinitis and its impact on asthma. J Allergy Clin Immunol. 2001;108(5 Suppl):S147-334.
17. Bousquet J, Khaltaev N, Cruz AA, et al. Allergic Rhinitis and its Impact on asthma (ARIA) 2008 update (in collaboration with the World Health Organization, GA(2)LEN and AllerGen). Allergy. 2008;63(Suppl 86):8-160.
18. Herman H. Once-daily administration of intranasal corticosteroids for allergic rhinitis: a comparative review of efficacy, safety, patient preference, and cost. Am J Rhinol. 2007;21(1):70-79.
19. Simon FER, Simons KJ. H1 Antihistamines: current status and future directions. World Allergy Organ J. 2008;1(9):145-155.
20. American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 updated Beers criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2015;63(11):2227-2246.
21. Sur DKC, Plesa ML. Treatment of allergic rhinitis. Am Fam Physician. 2015;92(11):985-992.
22. Meltzer EO, Bukstein DA. The economic impact of allergic rhinitis and current guidelines for treatment. Ann Allergy Asthma Immunol. 2011;106(2 Suppl):S12-16.
23. Hatton RC, Winterstein AG, McKelvey RP, et al. Efficacy and safety of oral phenylephrine: systematic review and meta-analysis. Ann Pharmacother. 2007;41(3):381-390.
24. Malone M. Review: side effects of some commonly used allergy medications (decongestants, anti-leukotriene agents, antihistamines, steroids, and zinc) and their safety in pregnancy. https://clinmedjournals.org/articles/ijam/international-journal-of-allergy-medications-ijam-3-024.php?jid=ijam. Accessed April 15, 2018.
25. Mortuaire G, de Gabory L, François M, et al. Rebound congestion and rhinitis medicamentosa: nasal decongestants in clinical practice. Critical review of the literature by a medical panel. Eur Ann Otorhinolaryngol Head Neck Dis. 2013;130(3):137-144.
26. Melvin T-AN, Patel AA. Pharmacotherapy for allergic rhinitis. Otolaryngol Clin North Am. 2011;44(3):727-739.
To comment on this article, contact rdavidson@uspharmacist.com.