US Pharm. 2013;38(8):43-50.
ABSTRACT: Innovative health care technologies are often blamed for rising health care costs, but they can also be part of the solution as the nation strives to create a value-based health care system. The next generation of mobile and telehealth technologies for chronic disease management holds great promise in terms of improving the quality and lowering the cost of care, while also creating significant business opportunities for community pharmacies. As pharmacies strive to become more comprehensive wellness centers, these technologies create opportunities to expand service offerings, engage patients in their care, and ultimately define a greater role in the evolving health care delivery system.
The United States is under growing pressure to create a value-based health care system in the face of escalating health care costs and shrinking budgets. One significant driver of cost has been the rising prevalence of chronic diseases, especially cardiovascular disease, diabetes, and asthma. Nearly half of all American adults have at least one chronic disease, and more than 75% of Medicare spending is dedicated to their care.1,2
The burden of these diseases often falls on underserved populations. The safety-net delivery system usually lacks the financial resources, human resources, and information technology infrastructure needed to properly manage chronic diseases, while these patients face additional challenges in their lives over literacy and language barriers and housing instability.
Innovative health care technologies are often blamed for the rising cost of health care, but they can also play a critical role in the quest for value-based health care, offering the potential to lower costs, improve access, and enhance clinical outcomes. In 2012, NEHI, with support from the California HealthCare Foundation, conducted a research project to identify the next generation of chronic disease management technologies, paying special attention to the needs of the underserved. NEHI, formerly known as the New England Healthcare Institute, is a national health policy institute focused on enabling innovation to improve health care quality and lower health care costs.3
As these technologies continue to gain popularity, they are not only transforming the health care delivery system and how patients and providers interact, but they are also offering a new business opportunity for the community pharmacy world. Many of the emerging technologies and services identified by NEHI can be sold by community pharmacies and used to complement existing service offerings by pharmacists and retail clinics. This article will explore several of the technologies with promise for improving the quality and reducing the cost of care for chronic disease patients and show how these technologies have been used in community pharmacies to date.
NEHI’s Technology Project
In NEHI’s 2012 report, Getting to Value: Eleven Chronic Disease Technologies to Watch,3 a robust and replicable methodology was designed to identify, assess, and aid the adoption of transformative technologies for chronic disease care. The scan process began by identifying a diverse list of over 80 technologies, which was winnowed down to 11 through a process that identified those technologies with the highest potential for clinical benefit, cost savings, and adoption. Extensive research was conducted to create profiles for each of the 11 technologies.
Additional research in the form of literature reviews and primary interviews with technology developers and medication adherence experts was conducted to assess the emergence of these technologies in the community pharmacy world. Because these partnerships are in their infancy, research was predominantly comprised of the insights gleaned from these primary interviews.
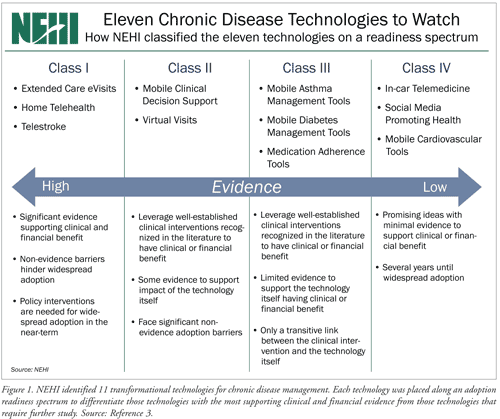
Snapshot of Technologies: A subset of the 11 technologies that NEHI identified has already found its way into community pharmacies, including virtual visits and medication adherence tools. There is a logical business case for pharmacies to sell many of the others, including home telehealth, mobile diabetes management tools, mobile asthma management tools, and mobile cardiovascular tools. FIGURE 1 shows how these technologies were classified.3
Home Telehealth: These technologies are remote monitoring devices that allow patients to actively track and manage their chronic diseases by wirelessly transmitting physiological data from their homes to physicians’ offices and, in turn, receive health coaching. Recent estimates suggest a sizable portion of the chronic disease population may benefit. One study estimates that about 50% of its total patient population could be cared for with home telemedicine technologies.4 Despite their potential, adoption rates remain relatively small when considering the immense target population of chronic disease patients.
Several significant barriers have slowed adoption, including the cost of these devices, which can reach as much as several thousand dollars per unit. Reimbursement remains another challenge, as many third-party insurers still do not cover the cost of these tools. Providers are increasingly adopting home telehealth technology, although physician and patient behavior remains a challenge as well. Finally, legal and licensure barriers across state lines remain a significant challenge for telehealth technologies in general.3
Virtual Visits: These technologies facilitate real-time interactions between patients and providers. Unlike home telehealth, these platforms do not require a hub device; instead, virtual visit technology can be accessed from smartphones, personal computers, and kiosks. These technologies offer the potential to ease access challenges for patients while allowing providers to intervene before costly complications ensue. A recent survey revealed that nearly 75% of patients are interested in interacting with providers online, while only 25% are willing to pay extra to do so.5
Barriers to adoption for virtual visit technologies include the fact that these technologies present a difficult business model requiring an organization—like a drug store—to offer the service, and they often are not a direct-to-consumer product. The use of these technologies also requires a shift in behavior for providers and patients as they need to become comfortable with remote consultations.
Mobile Diabetes Management Tools: These tools represent the next generation of diabetes management and use wireless devices to collect and log blood glucose readings, provide alerts, and interpret data over time. Results from a manufacturer study showed that patients who received automated, real-time educational and behavioral messaging in response to blood glucose values exhibited a 1.9% decline in A1C compared to 0.7% for the usual care group after 1 year.6 A single percentage point drop in A1C level can reduce the risk of heart, kidney, and eye disease by up to 40%.7
Widespread adoption is dependent on the reimbursement model. If these new devices are not covered by insurance, it is unlikely patients will purchase these technologies out-of-pocket, if the less sophisticated alternatives are covered. Another barrier is that many of these tools still require patients to take an active role in data transmission, either by manually entering data into a platform or plugging in their device. Finally, for these technologies to realize their true potential, they must be compatible with existing blood glucose monitors and the growing health information technology infrastructure in the delivery system.
Medication Adherence Tools: These tools leverage cell phones to alert patients and caregivers when to take their medications. Many patients do not take their chronic disease medications as prescribed—up to half of all patients in the U.S. do not take their medications as prescribed by their doctors, and NEHI research suggests that poor medication adherence represents $290 billion in wasteful spending annually.8
Often the elderly and the underserved are impacted by poor medication adherence. Many of these technologies use smartphone applications, which could be costly and confusing for the elderly or those not technologically savvy. Reimbursement is another significant barrier for widespread adoption. If these technologies are not covered by third-party insurers, patients are unlikely to pick up the added out-of-pocket expense.
Mobile Asthma Management Tools: These tools use GPS technology to log when and where asthma attacks occur and provide feedback to patients on how to make appropriate lifestyle changes. These tools have been shown to have a number of positive clinical outcomes, such as helping patients get their asthma symptoms under control, improving the effectiveness of inhaler therapy, and decreasing flare-ups, which results in fewer hospitalizations and trips to the emergency department or physician’s office for uncontrolled asthma. One study showed that many patients were able to get their symptoms under control after being given baseline data collected from a rescue inhaler with a GPS attachment.9,10
Additional research is needed to accurately quantify the clinical and financial benefits. The cost of these devices also poses a barrier to expanded adoption. Most of these technologies require smartphones or add-on devices that may be cost-prohibitive to many patients. Without insurance coverage, it is unlikely that patients will purchase them out-of-pocket, especially the underserved and the elderly.
Mobile Cardiovascular Tools: These tools enable patients with cardiovascular disease to monitor and share their vital signs with caregivers and providers using wireless technology. Often patients with cardiovascular disease will not recognize or will ignore symptoms, leading to costly interventions, sometimes resulting in mortality. These tools allow patients to manage their disease and identify clinical aberrations before they become serious problems. The clinical benefit of specific mobile cardiovascular tools has not been robustly quantified to date, though controlled blood pressure can lower the risk for stroke and heart attack.
Similar to many of these other technologies, one of the greatest challenges is the reimbursement model. Without the financial and clinical evidence to justify reimbursement, third-party payers are unlikely to cover these technologies. Additional studies are needed to clearly define the appropriate use of these technologies and to verify the clinical and financial benefits.
Opportunities for Community Pharmacies
Community pharmacies continue to seek opportunities to expand service offerings, engage patients in their care, and ultimately define a greater role in the evolving health care delivery system. There has been a shift in the mission of many of these retailers from being solely a drug store to a more comprehensive wellness center. Over the last few years, most of the large pharmacy chains have experimented with new technologies as a means to bring them closer to this goal.
Rite Aid NowClinic: In September 2011, Rite Aid partnered with OptumHealth and American Well to create NowClinic, a virtual visit technology that customers can use to engage with nurses and physicians.11 As part of Rite Aid’s larger strategy of rebranding their stores as wellness centers rather than pharmacies and to avoid the significant start-up costs that have plagued the expansion of retail clinics, Rite Aid invested in virtual visit technology to connect patients to nurses and physicians remotely. Rite Aid piloted these in-store kiosks in the Detroit area, a market where residents often have difficulty accessing health care due to low incomes and low availability of primary care physicians in the area.
The services offered at NowClinic are similar to those that would be offered in retail clinics and include treatment for allergies, bladder infections, bronchitis, pink eye, sore throat, and other minor illnesses.11 Customers can have a free online consultation with a nurse or select optional upgrades for a 10-minute virtual visit with a physician for $45 and purchase additional time in 5-minute increments payable by credit card. The customer is responsible for submitting claims to the insurer for reimbursement, if covered. Depending on the consultation, the nurse or physician can advise the patient whether an in-person visit with a doctor is necessary, have a certified pharmacist deliver vaccines, or have the pharmacist fill a prescription. Rite Aid’s in-store NowClinics are available in four states (Michigan, Maryland, Massachusetts, and Pennsylvania) and can also be accessed through an online portal.11
Walgreens Pill Reminder Application: Over the last several years, Walgreens has been one of the industry leaders in terms of offering convenient mobile applications that promote medication adherence, including their Pill Reminder and Refill by Scan applications.12 Pill Reminder is a free mobile application that allows customers to easily track drug schedules and receive alerts to remind them to take their medications. These reminders can easily be set by scanning a prescription barcode and selecting preferences. Customers can add additional prescriptions, vitamins, and other supplements to a single reminder.
Refill by Scan is another convenient and free mobile application that allows patients to order refills simply by scanning a prescription barcode with a smartphone.12 Many of the other large retail pharmacy chains, including CVS and Rite Aid, offer similar applications.
Discussion
Community pharmacies have a long history of marketing various consumer health devices and providing counseling on their use. This remains true today. Recently, pharmacies have been much quicker to embrace mobile health and telehealth technologies than physician practices and hospital systems. Retail pharmacy chains now routinely offer smartphone applications for medication alerts and refill reminders, just as they earlier offered customer Web portals.
Improving Care Coordination Through the Exchange of Health Information: There is enormous opportunity for the pharmacy sector to consider leveraging the wealth of information already at their fingertips to advance health policy goals. These emerging smartphone applications and existing Web portals create a number of opportunities to promote medication management and adherence goals. If a patient fills all of his or her prescriptions at a single pharmacy chain, that person has access to his or her prescription history, creating a real time medication list, something that remains elusive in health care.
There is also an opportunity for the pharmacy sector to consider how to leverage its existing investment in accessible medication records to achieve Meaningful Use goals (i.e., the set of standards from the Centers for Medicare and Medicaid Services [CMS] that governs the use of electronic health records and allows eligible providers and hospitals to earn incentive payments by meeting specific criteria).3 The information housed in these already existing systems could be beneficial not only to pharmacists and patients, but also to physician teams, hospital discharge planners, and other clinicians in improving coordinated care of patients’ pharmaceutical needs.
Expanding Service Offerings to Improve Access: Community pharmacies could also be in line to sell many of the peripheral devices profiled in NEHI’s report, including the next generation of asthma, diabetes, and cardiovascular tools.3 Most, if not all, pharmacies are actively expanding their clinical services, including additional counseling services for patients and medication review by pharmacists. The question for community pharmacies is how to leverage these new technologies to expand their clinical offerings to patients. Rite Aid’s NowClinic is one example of how large pharmacy chains are entering into this new world of technology and expanded service offerings.11
Rite Aid’s choice to leverage virtual visit technology is a strategy that in many ways bypasses the retail clinics staffed by nurse practitioners that major retailers have invested in across the country. On the other hand, community pharmacies that have already made major investments in retail clinics could find additional value in actively marketing some of the other peripheral devices profiled in NEHI’s report.3 Major chains such as Walgreens and CVS have begun an expansion into services that include limited prescribing, lab orders, and more extensive chronic care case management, where these are permitted by state regulation.11
Defining a New Role in an Era of Accountable Care: An accountable care organization (ACO) is a group of health care providers formed to provide coordinated, high-quality care to Medicare patients. As the pharmacy sector considers its role in the world of ACOs and other forms of global payments, pharmacies will need to weigh how these new devices and applications can help them achieve their performance goals.3 ACO and other payment innovations tie payment heavily to the achievement of population health goals in major chronic disease areas like diabetes, heart disease, and asthma—disease states that are major targets of the new mobile and telehealth technologies. Community pharmacy chains are actively considering their place in new ACO structures, as demonstrated by the recent approval by CMS of three Walgreens-affiliated Pioneer ACOs in New Jersey, Texas, and Florida.13
How will pharmacies use and effectively price these technologies for patients to help them achieve larger population health goals?
Conclusion
The continued transformation of the community pharmacy world will depend upon the flexibility of practice regulation at the state level and specifically on whether pharmacists and nurse practitioners will be allowed to provide more “top of the license” services. Historically, physicians have been reluctant to delegate tasks to pharmacists, although such delegation happens routinely in highly integrated health care systems and emerging models of practice. A common criticism of the retail clinics by physicians has been that they will divert patients from their primary care provider and fragment patient care. The emergence of ACOs with their distinct population health goals and emphasis on coordination across the care continuum may alter these historic battle lines. If so, community pharmacies may find a growing incentive to market, service, and promote innovative mobile and home telehealth technologies.
REFERENCES
1. CDC. Chronic disease and health promotion. Published
2011. www.cdc.gov/chronicdisease/overview/index.htm. Accessed March 13,
2013.
2. Thorpe KE, Howard DH. The rise in spending among
Medicare beneficiaries: the role of chronic disease prevalence and
changes in treatment intensity. Health Affairs. 2006;25:378-388.
3. Bartolini E, McNeill N. Getting to Value: Eleven Chronic Disease Technologies to Watch.
Cambridge, MA: NEHI; June 2012.
www.nehi.net/publications/72/getting_to_value_eleven_chronic_disease_technologies_to_watch.
Accessed March 13, 2013.
4. Darkins A, Ryan P, Kobb R, et al. Care
coordination/home telehealth: the systematic implementation of health
informatics, home telehealth, and disease management to support the care
of veteran patients with chronic conditions. Telemed J E Health. 2008;14:1118-1126.
5. Seidman J, Eytan T. Helping Patients Plug In: Lessons in the Adoption of Online Consumer Tools.
Oakland, CA: California HealthCare Foundation; June 2008.
www.chcf.org/~/media/MEDIA%20LIBRARY%20Files/PDF/H/PDF%20HelpingPatientsPlugIn.pdf.
Accessed March 13, 2013.
6. Quinn C. Cluster-randomized trial of a mobile phone personalized behavioral intervention for blood glucose control. Diabetes Care. 2011;34:1934-1942.
7. CDC. National Diabetes Fact Sheet: National Estimates and General Information on Diabetes and Prediabetes in the United States. Published 2011. www.cdc.gov/diabetes/pubs/pdf/ndfs_2011.pdf. Accessed March 13, 2013.
8. NEHI. Thinking Outside the Pillbox: A System-Wide Approach to Improving Patient Medication Adherence for Chronic Disease. Cambridge, MA: NEHI; August 2009.
9. Newman J. High-tech inhaler from Madison company would help doctors track asthma attacks. Wisconsin State Journal.
June 15, 2011.
http://host.madison.com/wsj/business/article_e79d070e-9791-11e0-a329-001cc4c002e0.html.
Accessed March 13, 2013.
10. Klein S. Quality Matters Q&A. Asthmapolis:
improving asthma control with mobile technology. The Commonwealth Fund.
October/November 2011.
www.commonwealthfund.org/Newsletters/Quality-Matters/2011/October-November-2011/Q-A.aspx.
Accessed March 13, 2013.
11. Dolan PL. Rite Aid clinics place new twist on “doc-in-a-box.” American Medical News. February 6, 2012. www.ama-assn.org/amednews/2012/02/06/bil20206.htm. Accessed March 13, 2013.
12. Better health through mobile—Walgreens introduces new pharmacy tools to help smartphone users manage prescription needs. Walgreens News. March 9, 2012. http://news.walgreens.com/article_print.cfm?article_id=5560. Accessed March 13, 2013.
13. Walgreens forms accountable care organizations (ACO)
to deliver seamless, coordinated care to improve patient health, lower
costs and close critical gaps in care for Medicare patients. Walgreens News. January 10, 2013. http://news.walgreens.com/press+releases/general+news/aco.htm. Accessed July 1, 2013.
To comment on this article, contact rdavidson@uspharmacist.com.






