US Pharm. 2019:44(3):HS-9-HS-12.
ABSTRACT: Pain, agitation, and delirium (PAD) are commonly observed in critically ill patients. Many factors in the ICU can contribute, and it is imperative for all team members to know how to prevent, diagnose, and treat PAD. In patients experiencing pain, opioids remain the gold standard of treatment, with use of nonopioid analgesics in appropriate patient populations. Treating pain can help decrease agitation, while limiting sedation can help prevent delirium within the ICU. Pharmacists play an important role in PAD management.
The 2013 American College of Critical Care Medicine Clinical Practice Guidelines for the Management of Pain, Agitation, and Delirium in Adult Patients in the Intensive Care Unit (PAD) were expanded in 2018 to include immobility and sleep in critically ill adult patients.1,2 This update (PADIS) provides insight on the rehabilitation, mobilization, and sleep disruption commonly seen in critically ill adult patients. This expansion also focuses on long-term clinical outcomes and includes ICU survivors as collaborators and coauthors.
Pain
Pain management in critically ill adult patients is complex, owing to patient variability, pain tolerance, and type of pain. Patients experience visceral, somatic, and neuropathic pain while in the ICU, as well as procedural and surgical pain and pain during necessary daily activities (e.g, tracheal tube suctioning).1,2 In order to adequately treat pain, clinicians must use appropriate scales for assessment. The validated assessment tools for pain were not reevaluated in the PADIS guidelines, and therefore the ones endorsed in the 2013 PAD guidelines should be used. The gold standard is self-reporting, but this is not always feasible in the ICU setting because patients may be nonverbal. The Critical-Care Pain Observation Tool or Behavioral Pain Scale are options for pain assessment.
Although opioids remain the foundation for pain management in the ICU, side-effect profile and safety concerns make pharmacologic adjuncts to opioid therapy an important aspect of a multimodal analgesic approach. Multimodal analgesia is likely to reduce opioid consumption and improve long-term clinical outcomes for patients.2 Opioid adjuncts should be individualized, and side-effect profiles assessed, prior to use.
For nonneuropathic pain, the PADIS guidelines recommend the use of acetaminophen to decrease pain and opioid use. The guideline authors make no recommendations for a particular route of administration, but it is important to note that oral and rectal acetaminophen may have variable bioavailability in the critically ill patient. When considering the use of IV acetaminophen, it is important to note the acquisition costs as compared with other routes of administration. Low-dose ketamine (0.5 mg/kg IV push, then 1-2 mcg/kg/min infusion) is also recommended as an adjunct to opioid therapy as a way to decrease opioid consumption postoperatively.2 In the treatment of pain, ketamine works by inhibiting the N-methyl-d-aspartate receptor and has a secondary effect of decreasing the risk of opioid hyperalgesia.3 Ketamine was evaluated in post–abdominal surgery ICU patients, with those receiving ketamine having reduced morphine consumption.4 While this randomized controlled trial (RCT) found no difference in the side-effect profile between ketamine and opioid-alone groups, it is important to recognize that ketamine can cause hallucinations and delirium, and it exhibits sympathomimetic properties.
For neuropathic pain and nonneuropathic pain in the post–cardiovascular surgery adult ICU patient, the PADIS guidelines recommend the use of gabapentin (15 mg/kg/day), carbamazepine (100 mg/day), and pregabalin (150 mg/day) with opioids for pain management. Unlike adjuncts to nonneuropathic pain, this carries a strong recommendation with moderate quality of evidence. The guideline authors recommend against the use of IV lidocaine as an adjunct to opioids due to its inability to affect patient’s self-reported pain and its side-effect profile; the risks associated with use far outweighed any theoretical benefit.2 Additionally, nonsteroidal anti-inflammatory drugs (NSAIDs) are not recommended because of their ability to cause acute kidney injury and their bleeding profile.2
The PADIS guidelines integrated a new section on nonpharmacologic interventions aimed at reducing pain. These interventions included massage, music therapy, cold therapy, and relaxation techniques. Overall, these nonpharmacologic interventions should be used in the appropriate patient setting; available resources may limit their utility.2
Agitation/Sedation
Analgosedation was first introduced in the 2013 PAD guidelines and reemphasized in the PADIS update.1,2 Analgosedation supports the concept that not all mechanically ventilated patients require sedatives throughout the duration of intubation. Instead, a pain-management approach should be trialed before any sedative agent is added to a patient’s therapeutic regimen. Often the cause of a patient’s agitation and anxiety is a direct result of unmanaged pain, which is why evaluation of the patient’s pain through validated tools is important prior to assessing sedation. The validated assessment tools for agitation and sedation were not reevaluated in the PADIS guidelines, and therefore the ones endorsed in the 2013 PAD guidelines should be used (Sedation-Agitation Score [SAS] or Richmond Agitation Scale Score [RASS]).
The PADIS guidelines advocate using light sedation versus deep sedation in critically ill, mechanically ventilated adults, either by daily sedative interruption or nurse-protocolized sedation.2 Previous guidelines had suggested that a RASS of 0 to -2 was considered light sedation; however, in the preparation of the PADIS guidelines it was discovered that the definition of light sedation varied with values ranging from RASS -2 to +1. Providers should be targeting a light level of sedation in the majority of patients; the RASS goal should be individualized based on the patient because no universally accepted definition exists. Multiple RCTs were evaluated comparing the effect of light versus deep sedation on patient outcomes; patients in the light-sedation group had a shorter time to extubation and a reduced tracheostomy rate. There were no differences seen in 90-day mortality, incidence of delirium, post-traumatic stress disorder, depression, or self-extubation. None of the RCTs evaluated the difference between light versus deep sedation on cognitive or physical functioning, presenting an opportunity for further research.5-7
When it is deemed that a patient needs a pharmacologic agent for management of agitation and sedation, the agents to use remain the same as those outlined in the 2013 PAD guidelines; no new recommendations were provided in the 2018 PADIS update.1,2 The PADIS panel recognized that elective cardiac surgery patients were different from critically ill medical and surgical patients, owing to differences in ICU length of stay and duration of mechanical ventilation. The desired goal time to extubation in cardiac surgery patients is less than 6 hours, and it is expected that those patients also would have a reduced length of stay in the ICU. In cardiac surgery patients, the PADIS panel recommends the use of propofol over the use of a benzodiazepine. Data to support this come from multiple RCTs that evaluated infusions of propofol and benzodiazepines. In two RCTs, patients who received propofol had a shorter time to light sedation of at least 30 minutes.8,9 Another RCT evaluated time to extubation, defined as at least 1 hour, and found that patients receiving propofol had a shorter time to extubation versus those given benzodiazepines.10
Studies that evaluated dexmedetomidine compared with midazolam or lorazepam found that there was a shorter time on mechanical ventilation as well as a significant reduction in delirium.11,12 When it comes to a preference for either dexmedetomidine or propofol, PADIS guidelines make no recommendation and state that the effects of either agent are balanced. The propofol versus dexmedetomidine (PRODEX) study demonstrated that delirium incidence was decreased with dexmedetomidine, with no differences in bradycardia or hypotension between groups.13 Although the guidelines do not make specific recommendations regarding propofol or dexmedetomidine, they do recognize that patient-specific factors should be considered in agent selection. Due to the inability of dexmedetomidine to induce a deep level of sedation, propofol would be a preferred agent in patients requiring deep sedation, such as those receiving neuromuscular blockade or those with an open abdomen. Other patient-specific factors that play a role in sedation-agent selection include acute alcohol withdrawal or status epilepticus. In such patients it is reasonable to consider sedation using a benzodiazepine approach as a first-line agent.
Delirium
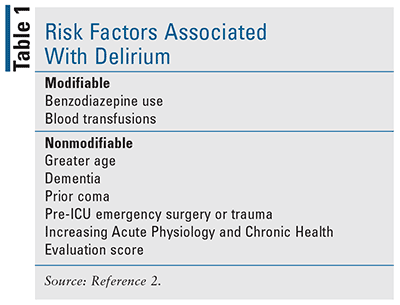
Delirium affects up to 80% of mechanically ventilated adult ICU patients, contributing to an overwhelming cost to the healthcare system, increased length of stay, and increased mortality at 6 months.1 The PADIS guidelines discuss modifiable and nonmodifiable risk factors for delirium (Table 1). In order to discern if a patient in the ICU has delirium, it is recommended that a validated assessment tool be used, either the Confusion Assessment Method for the ICU or the Intensive Care Delirium Screening Checklist.2 Unfortunately delirium can be disturbing not only for ICU patients but also for their visitors and hospital staff. As delirium can be a detriment to patient care, studies have tried using antipsychotics, dexmedetomidine, HMG CoA reductase inhibitors, or ketamine to prevent delirium.2 Low-dose IV haloperidol did not prevent delirium or reduce 90-day survival.14 However, nocturnal administration of low-dose dexmedetomidine was associated with a greater number of patients remaining delirium-free.15 Duration of mechanical ventilation, ICU and hospital stay, and ICU and hospital mortality were similar between the low-dose dexmedetomidine group and the placebo group.15
As meaningful endpoints were similar between treatment and placebo groups, PADIS guidelines recommend not using pharmacologic management for the prevention of delirium. Additionally, it is recommended not to routinely treat delirium with antipsychotics. Multiple studies have failed to show a correlation between treatment of delirium and shorter duration of delirium or ICU length of stay, a reduced duration of mechanical ventilation, or decreased mortality.2
Although these recommendations are made for the routine treatment of delirium, patients who are experiencing distress secondary to symptoms of delirium such as anxiety, fearfulness, hallucinations, and delusions or those who may be agitated and causing physical harm to themselves or others may benefit from short-term use of antipsychotics.2 Of note, this recommendation is based solely on the clinical experience of panel members. Not only have antipsychotics failed to show any meaningful long-term benefit, but when antipsychotics are started in the ICU setting for delirium, studies have shown that they are continued inappropriately at discharge, leading to increased risk of drug-drug interactions, financial burden, and polypharmacy.16
Dexmedetomidine is recommended for use in mechanically ventilated patients who are delirious and have agitation precluding extubation.2 PADIS guidelines recommend utilizing a multicomponent, nonpharmacologic method that is focused on reducing modifiable risk factors for delirium (Table 1). Nonpharmacologic methods might include improving cognition and optimizing sleep, mobility, hearing, and vision in critically ill patients.2 Assessments in the ICU can be easily done to determine if patients wear eyeglasses or hearing aids at home. These small measures may reduce the risk of delirium in ICU patients.
Immobility
Patient immobility during ICU admission has a significant impact on muscle strength upon awakening and even at discharge, especially in those receiving mechanical ventilation.17,18 The PADIS guidelines answer several logistical questions for clinicians on how to best increase mobility (Table 2). Early mobility has been shown to improve several clinical outcomes including muscle strength at ICU discharge, duration of mechanical ventilation, and patient-reported quality of life 2 months post–hospital discharge.2
Sleep Disruption
The physiological impact of sleep disruption during ICU admission is an increasing area of study, reflected in the expanded section in the PADIS guidelines. Many factors are believed to contribute to this disruption, including psychoactive medications, bedtime medication administration, the nature of critical illness, and delirium. Although the guidelines do not recommend preventative sleep-cycle screening, they do identify several risk factors including sleep disorder prior to hospitalization, use of pharmacologic sleep aid before hospitalization, pain, environmental stimuli, healthcare-related interruptions, medications, and other respiratory or psychological factors.2
Recommendations for several nonpharmacologic measures are newly introduced into the PADIS guidelines. They include adjusting ventilator settings and noise and light reduction via earplugs and eye shades. The guidelines authors do not endorse aromatherapy, acupressure, or music during bedtime, owing to insufficient evidence.2
Although the guidelines do acknowledge that promoting sleep is an important aspect of quality ICU care, there is a low depth and breadth of evidence surrounding the use of melatonin or dexmedetomidine. Three RCTs evaluated melatonin versus placebo and did not show any significant clinical impact on improving sleep. This lack of evidence, paired with the absence of FDA regulation, led the authors to provide no recommendation regarding use in the ICU.2 RCTs evaluating the use of dexmedetomidine did show improvement in various stages of the sleep cycle, but not in sleep fragmentation or REM, which are believed to be the most impactful on quality of sleep. The guideline authors did not provide any recommendation regarding the use of dexmedetomidine in the ICU.2 However, when comparing propofol to placebo or benzodiazepines there was greater REM suppression and an increase in serious side effects, including the need for mechanical ventilation. Therefore, the guidelines recommend against utilizing propofol strictly to improve sleep in the ICU.2
Pharmacists Role
Pharmacists play an integral role in the multidisciplinary ICU team. Pharmacists in the ICU should be able to employ evidence-based recommendations in order to appropriately assess and treat pain, agitation, and delirium. The pharmacist plays a unique role in identifying drug-drug interactions, side effects, and pharmacokinetic profiles of commonly used medications in the ICU.
REFERENCES
1. Barr J, Fraser GL, Puntillo K, et al. American College of Critical Care Medicine. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. Crit Care Med 2013;41:263-306.
2. Devlin JW, Skrobik Y, Gélinas C, et al. Clinical practice guidelines for the prevention and management of pain, agitation/sedation, delirium, immobility, and sleep disruption in adult patients in the ICU. Crit Care Med. 2018;46(9):e825-e873.
3. Velayudhan A, Bellingham G, Morley-Forster P. Opioid-induced hyperalgesia. Continuing Education Anesth, Critical Care Pain. 2014;14(3):125-129.
4. Guillou N, Tanguy M, Seguin P, et al. The effects of small-dose ketamine on morphine consumption in surgical intensive care unit patients after major abdominal surgery. Anesth Analg. 2003;97:843-847.
5. Shehabi Y, Bellomo R, Reade MC, et al; Sedation Practice in Intensive Care Evaluation Study Investigators; Australian and New Zealand Intensive Care Society Clinical Trials Group. Early goal-directed sedation versus standard sedation in mechanically ventilated critically ill patients: a pilot study. Crit Care Med. 2013;41:1983-1991.
6. Bugedo G, Tobar E, Aguirre M, et al. The implementation of an analgesia-based sedation protocol reduced deep sedation and proved to be safe and feasible in patients on mechanical ventilation. Rev Bras Ter Intensiva. 2013;25:188-196.
7. Treggiari MM, Romand JA, Yanez ND, et al. Randomized trial of light versus deep sedation on mental health after critical illness. Crit Care Med. 2009;37:2527-2534.
8. Snellen F, Lauwers P, Demeyere R, et al. The use of midazolam versus propofol for short-term sedation following coronary artery bypass grafting. Intensive Care Med. 1990;16:312-316.
9. Roekaerts PM, Huygen FJ, de Lange S. Infusion of propofol versus midazolam for sedation in the intensive care unit following coronary artery surgery. J Cardiothorac Vasc Anesth. 1993;7:142-147.
10. Searle NR, Côté S, Taillefer J, et al. Propofol or midazolam for sedation and early extubation following cardiac surgery. Can J Anaesth. 1997;44:629-635.
11. Riker RR, Shehabi Y, Bokesch PM, et al; SEDCOM (Safety and Efficacy of Dexmedetomidine Compared With Midazolam) Study Group. Dexmedetomidine vs midazolam for sedation of critically ill patients: a randomized trial. JAMA. 2009;301:489-499.
12. Pandharipande PP, Pun BT, Herr DL, et al. Effect of sedation with dexmedetomidine vs lorazepam on acute brain dysfunction in mechanically ventilated patients: the MENDS randomized controlled trial. JAMA. 2007;298:2644-2653.
13. Jakob SM, Ruokonen E, Grounds RM, et al; Dexmedetomidine for Long-Term Sedation Investigators. Dexmedetomidine vs midazolam or propofol for sedation during prolonged mechanical ventilation: two randomized controlled trials. JAMA. 2012;307:1151-1160.
14. van den Boogaard M, Slooter AJC, Bruggemann RJM, et al. Effect of haloperidol on survival among critically ill adults at high risk for delirium: the REDUCE randomized clinical trial. JAMA. 2018;319:680-690.
15. Skrobik Y, Duprey MS, Hill NS, et al. Low-dose nocturnal dexmedetomidine prevents ICU delirium: a randomized, placebo-controlled trial. Am J Respir Crit Care Med. 2018;197:1147-1156.
16. Tomichek JE, Stollings JL, Pandharipande PP, et al. Antipsychotic prescribing patterns during and after critical illness: a prospective cohort study. Crit Care. 2016;20:378.
17. De Jonghe B, Sharshar T, Lefaucheur JP, et al. Paresis acquired in the intensive care unit: a prospective multicenter study. JAMA. 2002;288:2859-2867.
18. Fan E, Dowdy DW, Colantuoni E, et al. Physical complications in acute lung injury survivors: a two-year longitudinal prospective study. Crit Care Med. 2014;42(4):849-859.
To comment on this article, contact rdavidson@uspharmacist.com.