US Pharm. 2019;44(2)(Specialty&Oncology suppl):4-7.
ABSTRACT: Hematopoietic cell transplantation (HCT) is the transfer of hematopoietic stem cells and progenitor cells from one donor to another or the harvesting of cells from a patient that are returned to that patient. In both scenarios, patients are at increased risk for infection. HCT is used for various hematologic cancers and noncancerous conditions affecting the blood or bone marrow. Patients undergoing this treatment are at risk for many infectious complications owing to impaired cell-mediated immunity and an immunocompromised state. These complications are influenced by factors such as amount of time after HCT, the prophylactic strategy used, comorbidities, pathogen exposure, and the degree of immunosuppression. The prevention of infections—including bacterial, fungal, and viral—is a priority in the care of HCT patients.
Hematopoietic cell transplantation (HCT) is the transfer of hematopoietic stem cells and progenitor cells from one donor to another (allogeneic) or the harvesting of cells from a patient that are then returned to that patient (autologous).1 The first successful bone marrow transplant, which took place more than six decades ago, involved the transfer of healthy bone marrow from one identical twin to the other twin, who had leukemia. Since the discovery of HCT in 1956, thousands of patients each year with various hematologic cancers and noncancerous conditions affecting the blood or bone marrow have benefited from this treatment.2 Some of the more common indications for HCT include aplastic anemia, hemoglobinopathies, leukemia, lymphoma, myeloproliferative disorders, myelodysplastic syndrome, bone marrow failure syndromes, congenital immunodeficiencies, and enzyme deficiencies.3
Prior to transplantation, patients undergo an arduous process known as myeloablation. The goal of this regimen is to provide sufficient immunoablation to reduce tumor burden and prevent graft rejection. This aim is achieved mainly through the use of chemotherapeutic agents and/or radiation of varying intensities.4 Myeloablation results in a profound pancytopenia that can last for days to weeks. Immune recovery begins with neutrophils, monocytes, and natural killer cells, followed by platelets and erythrocytes, and, finally, by B and T cells.5 The immunosuppression renders these patients susceptible to a plethora of opportunistic infections. Bacterial, viral, and fungal pathogens are characteristic of these infections, but the amount of time post transplantation seems to be involved in the etiology.5
There are three phases of opportunistic infections among allogeneic HCT recipients. Time since transplantation and the presence or absence of graft-versus-host disease (GVHD) remain the primary determinants of infection risk. GVHD is a serious complication of allogeneic transplants.6 In GVHD, the donated bone marrow or peripheral blood stem cells consider the recipient’s body to be foreign and consequently attack it. GVHD can be acute (occurring in the first 100 days) or chronic (occurring after the 100-day mark).7
Phase I, or the preengraftment phase (days 0-45 post HCT), is characterized by prolonged neutropenia and breaks in the mucocutaneous barriers, which increase the patient’s risk of bacterial and fungal infections. Additionally, herpes simplex virus reactivation may occur. Phase II, or the postengraftment phase (days 30-100 post HCT), is characterized by impaired cell-mediated immunity and is directly related to the severity of GVHD and immunosuppressive therapy. Cytomegalovirus (CMV), Pneumocystis jiroveci, and Aspergillus species are common pathogens during this phase. During phase III, or the late phase (more than 100 days post HCT), the risk of infection corresponds to the severity of the patient’s GVHD during the first two phases. Common pathogens include CMV, varicella-zoster virus, and infections from encapsulated bacteria, such as Streptococcus pneumoniae.4
Prevention of Bacterial Infection
For the prevention of early infection (days 0-100 post HCT), prophylaxis with a fluoroquinolone should be strongly considered for adult HCT patients with anticipated neutropenic periods of 7 or more days. Prophylaxis is generally started at the time of stem-cell infusion and continued until recovery from neutropenia or initiation of empirical antibacterial therapy for fever during neutropenia. It is recommended that antibiograms be consulted prior to the use of fluoroquinolones, owing to emerging resistance to gram-negative bacteria. The addition of an antibiotic with gram-positive or anaerobic coverage is not recommended because they are not beneficial for prophylaxis and promote the emergence of resistance.4
For the prevention of late infections, prolonged antibiotic prophylaxis is recommended only for preventing S pneumoniae infection in patients with chronic GVHD (cGVHD) as long as active cGVHD treatment is administered. Antibiotic selection should be guided by local antibiotic-resistance patterns. TABLE 1 addresses the most common bacterial etiologies and disease-prevention strategies.4

Central line–associated bloodstream infections are also a leading cause of infection in patients, especially those in the preengraftment phase. Central-line insertion precautions are of utmost importance in preventing central-line infections in HCT recipients.4
Prevention of Viral Disease
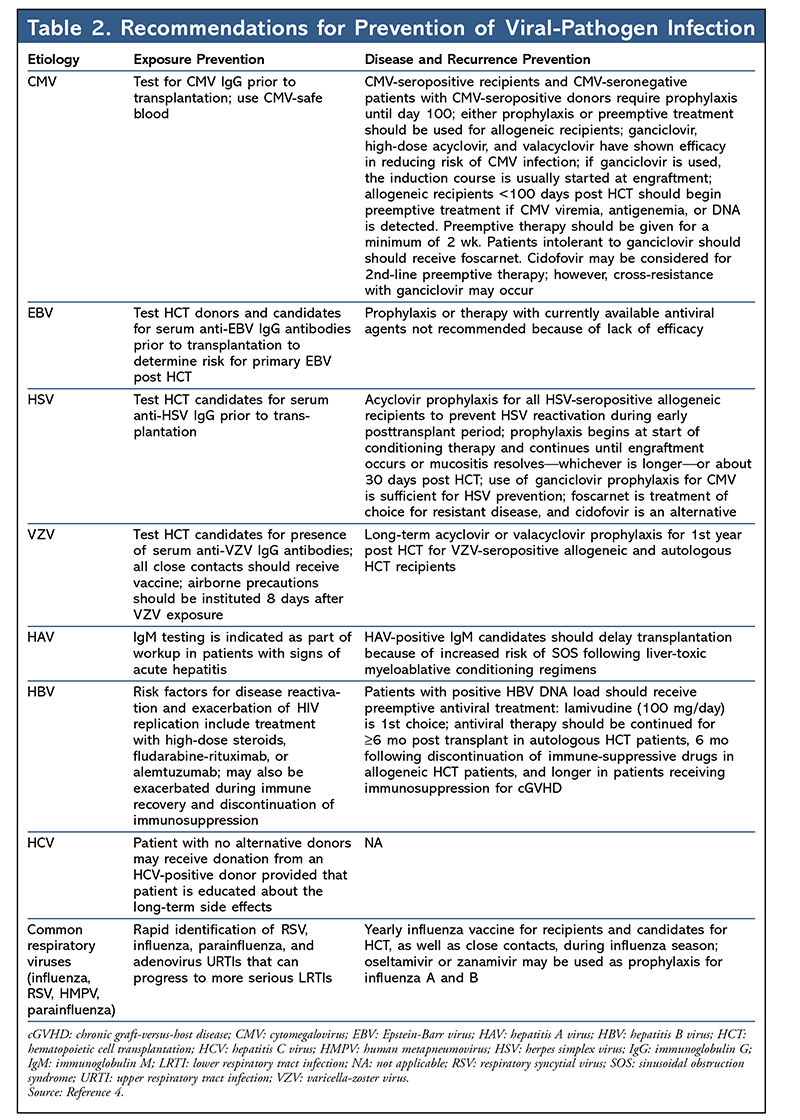
Detailed guidelines exist for the prevention of viral disease in HCT patients. TABLE 2 is a summary of the various recommendations for the prevention of viral-pathogen infections.4
Prevention of Fungal Disease
HCT recipients and candidates undergoing conditioning therapy should avoid certain foods that increase risk of exposure to fungi. These common foods include raw milk and cheeses, raw or undercooked meats, unwashed fruit or raw berries, raw honey, and herbal and nutritional supplements, among others.4 Patients receiving antifungal prophylaxis who develop clinical signs or symptoms of infection should be evaluated for breakthrough bloodstream or pulmonary fungal infection. The risk of invasive candidiasis is increased in these patients during neutropenia phases, severe mucositis, or gastrointestinal GVHD, and in the presence of a central venous catheter. Fluconazole is the agent of choice for the prophylaxis of invasive candidiasis before engraftment in allogeneic HCT recipients, and it may be started at the beginning of or just after the end of the conditioning regimen. It is unclear how long prophylaxis should be continued, although one study showed prolonged protection in patients receiving prophylaxis up to 75 days post HCT.8 Micafungin should be used instead of fluconazole for certain Candida species, such as Candida krusei and Candida glabrata.4
Vaccination Recommendations
Reimmunization of HCT recipients is recommended because of the loss of immunity to common childhood illnesses caused by a decline in antibody titers for vaccine-preventable diseases. Generally, three or four doses of pneumococcal conjugate vaccine are recommended; these should be initiated 3 to 6 months post HCT. One or two doses of inactivated influenza vaccine are recommended 4 to 6 months post HCT. Tetanus, diphtheria, acellular pertussis, Haemophilus influenzae conjugate, inactivated polio, and recombinant hepatitis B require three doses and should be initiated 6 to 12 months post HCT. Similarly, meningococcal conjugate should be initiated 6 to 12 months post HCT; however, this vaccine requires only one dose to be given. One or two doses of measles-mumps-rubella vaccine should be given 24 months post HCT.4
Conclusion
Bacterial, viral, and fungal infections are among the most common and significant contributing factors to morbidity and mortality in HCT recipients. These patients should be cared for according to the appropriate prophylactic measures following transplantation, and immediate medical attention should be given to any patient experiencing signs or symptoms of an infection. Vaccines, proper hygiene, avoidance of certain foods, and environmental awareness help reduce the risk of infection in this population.
REFERENCES
1. Forman SJ, Nakamura R. Hematopoietic cell transplantation. www.cancernetwork.com/cancer-management/hematopoietic-cell-transplantation. Accessed November 2018.
2. Australian Cancer Research Foundation. 1956: the first successful bone marrow transplantation. https://home.cancerresearch/1956-the-first-successful-bone-marrow-transplantation. Accessed November 2, 2018.
3. Paknikar S. Indications of bone marrow or hematopoietic stem cell transplantation. www.medindia.net/patients/patientinfo/bone-marrow-transplantation-indications.htm. Accessed November 2, 2018.
4. Tomblyn M, Chiller T, Einsele H, et al. Guidelines for preventing infectious complications among hematopoietic cell transplantation recipients: a global perspective. Biol Blood Marrow Transplant. 2009;15(10):1143-1238.
5. Gyurkocza B, Sandmaier BM. Conditioning regimens for hematopoietic cell transplantation: one size does not fit all. Blood. 2014;124(3):344-353.
6. Cleveland Clinic. Graft vs host disease: an overview in bone marrow transplant. https://my.clevelandclinic.org/health/diseases/10255-graft-vs-host-disease-an-overview-in-bone-marrow-transplant. Accessed January 1, 2019.
7. Toubai T, Sun Y, Reddy P. GVHD pathophysiology: is acute different from chronic? Best Pract Res Clin Haematol. 2008:21(2):101-117.
8. Marr KA, Seidel K, Slavin MA, et al. Prolonged fluconazole prophylaxis is associated with persistent protection against candidiasis-related death in allogeneic marrow transplant recipients: long-term follow-up of a randomized, placebo-controlled trial. Blood. 2000;96:2055-2061.
To comment on this article, contact rdavidson@uspharmacist.com.





