US Pharm. 2012;37(11):Epub.
ABSTRACT: Schizophrenia is a psychotic disorder that is characterized by positive and negative symptoms as well as cognitive dysfunction, although the etiology is unknown. Antipsychotics have been the mainstay of therapy for symptom management since the introduction of chlorpromazine in the 1950s. It was observed that typical (first-generation) antipsychotics caused extrapyramidal symptoms; hence, newer atypical (second-generation) antipsychotics were researched. However, some atypical antipsychotics may cause metabolic disturbances and therefore may not be useful in certain patients. There are presently a number of antipsychotics on the market, and the choice of agent depends upon individual preference, prior treatment response, side-effect profiles, and patient medical history.
Schizophrenia is a chronic remitting and relapsing psychotic disorder that impairs mental and social functioning and often leads to comorbid conditions.1 It is not a disease but rather a cluster of symptoms that last for a particular time.2 Schizophrenia occurs in approximately 1% of the population in all cultures and is found equally in men and women.1 This translates to about 2.4 million adults in the United States who have schizophrenia.3
Even with its relatively low prevalence, schizophrenia places a high economic burden on the U.S. economy. In 2002, the overall cost of schizophrenia in the U.S. was estimated to be $62.7 billion in direct and indirect health care costs.4 The largest share was a result of costs due to unemployment.4 Furthermore, it has been shown that approximately one-third of all schizophrenics will attempt suicide and about 1 out of 10 will eventually take his or her own life.5
ETIOLOGY, RISK FACTORS, AND PATHOPHYSIOLOGY
The etiology of schizophrenia is primarily attributable to genetics; having a close relative with the disorder increases one’s own risk 15-fold.1 Schizophrenia is a polygenic disorder that is influenced by environmental and developmental factors including season and location of birth, socioeconomic status, and maternal infections.1
These underlying causal factors are overtly expressed through neurochemical abnormalities.2 To date, dopamine is the only neuro-transmitter that is confirmed to be involved in schizophrenia. It has been shown that positive symptoms are associated with increased dopaminergic transmission and that most antipsychotics exert their effect by reducing dopaminergic transmission. The role of other neurotransmitters such as gamma-aminobutyric acid (GABA) is still under investigation.1
PRESENTATION
The first symptoms that are diagnostic of schizophrenia were listed by Kurt Schneider in the 1930s. Known as Schneider’s first-rank symptoms, these include thought insertion, withdrawal, broadcasting, passivity experiences, delusional perceptions, écho de la pensée ( a condition whereby the individual hears voices that echo thoughts immediately after they have occurred to the person), running commentary, and third-person auditory hallucinations.2
Today, schizophrenia is characterized by three major symptom clusters: positive (+) symptoms, negative (-) symptoms, and disorganized behavior.1,2 Positive symptoms include hallucinations, voices that converse with or about the patient, and delusions that are often paranoid.1 Negative symptoms include flattened affect, loss of a sense of pleasure, loss of will or drive (avolition), and social withdrawal.1 Disorganized behavior refers to affect, thought, and behavior resulting in disorganized speech including moving through multiple topics quickly.2
The types and severity of the symptoms vary from patient to patient, and as such, five different subtypes of schizophrenia have been identified (TABLE 1).1

Furthermore, the onset may be either abrupt or insidious.1 Typically, a prodromal phase demonstrated by slow and gradual development of negative symptoms is followed by the active phase. The prodromal phase includes social withdrawal, loss of interest in school or work, deterioration in hygiene and grooming, unusual behavior, and outbursts of anger; the active phase is characterized by psychosis.1
DIFFERENTIAL DIAGNOSIS
No one symptom is diagnostic of schizophrenia.1 Furthermore, the diagnosis changes with time in many cases. A diagnosis of schizophrenia may change to bipolar or organic disorders, while organic disorders, psychotic disorders, and major depression may eventually change to schizophrenia.1 Patients are often misdiagnosed because the symptoms overlap. A number of diagnoses, such as depression, bipolar disorder, or substance abuse, can produce symptoms similar to that of schizophrenia.1
MANAGEMENT
The effective management of schizophrenia includes a combination of pharmacotherapy and psychosocial interventions, as will be discussed in the following sections.6
Pharmacotherapy
Antipsychotics have become the cornerstone of pharmacologic treatment of schizophrenia since the introduction of the first antipsychotic, chlorpromazine, in the 1950s.6 First-generation antipsychotics (FGAs), also known as neuroleptics, are “conventional” agents that confer a high degree of extrapyramidal symptoms (EPS) such as tardive dyskinesia (TD) and akathisia. Second-generation antipsychotics (SGAs) are atypical agents that have a lower degree of EPS than the FGAs. A recent study has demonstrated inconclusive benefits of FGAs versus SGAs for treating schizophrenia because of variation in assessing outcomes and lack of clinically important differences for most comparisons.7 However, SGAs may have more modest benefits for cognitive impairments of schizophrenia compared to FGAs.
There are oral and long-acting injectable forms of both FGAs and SGAs; the depot injections are useful for patients who are nonadherent to oral medications.7
Typical Antipsychotics (FGAs): All typical or conventional antipsychotics are dopamine D2 antagonists, and the agents currently on the U.S. market can be divided into five classes (TABLE 2).2 The first FGA was chlorpromazine, but this drug is no longer available in the U.S.6 Symptoms usually begin to improve within a week with drugs of this class, and the effect continues to accrue with a peak effect seen at 6 weeks of treatment.2 Conventional antipsychotics may also be used for maintenance therapy to suppress the psychotic symptomatology and/or prevent the recurrence of a psychotic episode.2
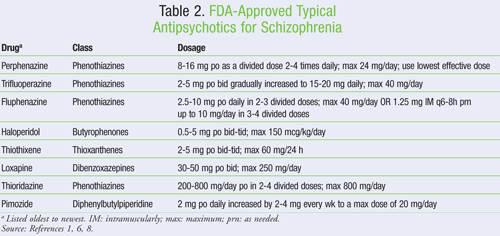
FGAs have a broad range of side effects, the most important ones being EPS such as akathisia, dystonia, tremor, and TD.8 High-potency FGAs such as haloperidol and fluphenazine are more likely to cause EPS and neuroleptic malignant syndrome (NMS), whereas low-potency antipsychotics including thioridazine are more prone to causing sedation and orthostatic hypotension.2 NMS is characterized by muscle rigidity and autonomic instability (elevated pulse rate and blood pressure). It is interesting to note that EPS constitute a major cause of nonadherence in patients. Other side effects that are associated with chlorpromazine and may be experienced by patients taking other FGAs include8:
- Antimuscarinic: dry mouth, blurred vision, urinary retention, tachycardia, and mydriasis
- Cardiac: altered ECG, hypotension, and, rarely, cardiac arrhythmias
- Hematologic: hemolytic anemia, aplastic anemia, thrombocytopenia, purpura, leukocytosis, and potentially fatal agranulocytosis
- Endocrine: endocrine and metabolic function may translate into amenorrhea, galactorrhea, gynecomastia, weight gain, hyperglycemia, and altered glucose tolerance.
Additionally, patients often complain about delirium, agitation, catatonic-like states, insomnia, drowsiness, nightmares, depression, and nasal congestion. Minor abnormalities are found in liver function tests, and males taking chlorpromazine may experience inhibition during ejaculation, impotence, and priapism.8
Atypical Antipsychotics (SGAs): Atypical antipsychotics were developed with the aim of reducing EPS and TD (TABLE 3). The first atypical antipsychotic, clozapine, was introduced in the late 1960s but was not approved for use in the U.S. until 1990. It is the only atypical antipsychotic that is effective for the management of positive symptoms that are resistant to conventional antipsychotics.9 In addition to having potent dopamine D2 antagonist and 5-HT2A antagonist activity, atypical antipsychotics have noradrenergic, histaminergic, and cholinergic effects, the extent of which varies between the individual agents. Furthermore, their varied affinities for neuroreceptors result in different side-effect profiles.6
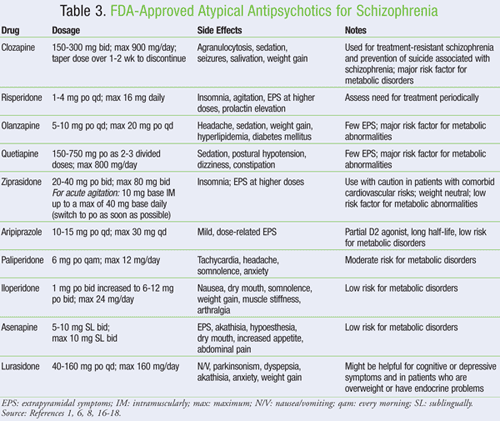
While FGAs confer a higher risk of developing EPS, the atypical agents are associated with a higher risk of metabolic side effects such as diabetes, hypercholesterolemia, and weight gain.1 The diabetogenic potential seems to be reversible if the medication is discontinued. Even though clozapine is not associated with EPS or tardive dyskinesia, its use is associated with a greater risk for agranulocytosis, a factor that has greatly limited its use.6 Greater interest in atypical antipsychotics developed when clozapine was found to be more effective in the treatment of refractory schizophrenia and in reducing suicidality. Since the 1980s, nine more atypical antipsychotics have become available in the U.S.6
Consensus Guidelines: There are five major algorithms for the management of schizophrenia in the U.S. (TABLE 4).10 These guidelines vary somewhat in scope, focus, goals, and recommendations, although none are incorrect or more correct in their assessments. The difference is in the way that they are established. In general, SGAs are considered first-line therapy.10
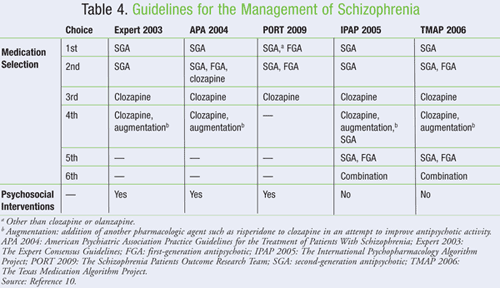
Selecting the correct drug therefore requires a consideration of the risk and benefits to the particular patient together with patient preference, goals of therapy, patient history, possible drug-drug interactions, and prior medication adherence history. The expert consensus guidelines recommend that patients either cross-taper or overlap, then taper, antipsychotics when switching from one to another.10
Psychosocial Support
Psychotherapy covers a wide range of interventions including individual, group, and family treatments. Family treatment may be one of either therapy with individual families, psychoeducation with groups of families, and family group therapy.1 Individual programs incorporate social skills training to enable the individual to function as normally as possible from a social perspective. Assertive community treatment and supported employment are also recommended interventions.11
PROGNOSIS
An understanding of the prognosis of the disorder will allow pharmacists to make therapeutic drug choices. Schizophrenics typically have a high rate of substance abuse resulting in first hospitalization at earlier ages, more frequent hospitalizations, and more interpersonal and family discord.1 They are poor at executive functioning and suffer low marital and high divorce rates.1 A schizophrenic, particularly one with severe psychotic disturbances, often exhibits aggressive behavior.1 These patients develop accelerated heart disease, the most common cause of death in schizophrenics. An individual suffering from schizophrenia has a 10% lifetime risk of suicide.1
ROLE OF THE PHARMACIST
Since therapeutic compliance rates are so low and side effects are varied, pharmacists have an important role to play in the management of schizophrenia. A recent study showed that 74% of schizophrenic patients discontinued their medication within 18 months.12 The likelihood that a patient will develop a particular side effect depends upon the patient’s vulnerability as well as the dose being administered and other coadministered medications.6 Pharmacists can monitor side effects and hence improve compliance by inquiring about positive and negative symptoms when the patient refills prescriptions, and communicate regularly with the patient’s other health care professionals about changes in symptoms. In addition to ensuring the correct dosing of appropriate drugs, pharmacists are key in guiding patients about where they can obtain further help (e.g., through individual or group therapy).
While existing antipsychotic medications are often effective for treating positive symptoms, they have little impact on negative symptoms and cognitive deficits. Therefore, there is a need to develop drugs that will allow for patient-specific treatment of symptoms. For example, lurasidone is a newer SGA that may be effective for cognitive symptoms. Additionally, while the newer therapies have addressed the issue of motor side effects, safety, and tolerability, there are increased concerns regarding weight gain and metabolic abnormalities.14
CONCLUSION
Untreated schizophrenia contributes to increased mortality, poor vocational and social functioning, and a reduced quality of life. Since it is not currently possible to predict which antipsychotic will suit a particular patient, pharmacists can be very useful in the trial and error process to find the correct drug and dosage for a particular patient. While the impact of antipsychotics on the social functioning and quality of life in schizophrenia is not well documented, increasing research efforts are being focused on developing new agents with increased efficacy for the treatment of the cognitive and negative symptoms of schizophrenia.15
REFERENCES
1. Schultz SH, North SW, Shields CG. Schizophrenia: a review. Am Fam Physician. 2007;75:1821-1829.
2. Lewis SW, Buchanan RW. Fast Facts: Schizophrenia. 3rd ed. Oxford, UK: Health Press Limited; 2007.
3. The numbers count: mental disorders in America.
National Institute of Mental Health.
www.nimh.nih.gov/health/publications/the-numbers-count-mental-disorders-in-america/index.shtml.
Accessed August 20, 2012.
4. Wu EQ, Birnbaum HG, Shi L, et al. The economic burden of schizophrenia in the United States in 2002. J Clin Psychiatry. 2005;66:1122-1129.
5. Andreasen NC, Black DW. Introductory Textbook of Psychiatry. 4th ed. Washington, DC: American Psychiatric Publishing, Inc; 2006.
6. Tandon R. Antipsychotics in the treatment of schizophrenia: an overview. J Clin Psychiatry. 2011;72(suppl 1):4-8.
7. Hartling L, Abou-Setta AM, Dursun S. Antipsychotics in
adults with schizophrenia: comparative effectiveness of first-generation
versus second-generation medications. Ann Intern Med. 2012 Aug 14 [Epub ahead of print].
8. Sweetman SC, ed. Martindale: The Complete Drug Reference. 34th ed. London, UK: Pharmaceutical Press; 2005.
9. Buchanan RW, Breier A, Kirkpatrick B, et al.
Positive and negative symptom response to clozapine in schizophrenic
patients with and without the deficit syndrome. Am J Psychiatry. 1998;155:751-760.
10. Moore T. Schizophrenia treatment guidelines in the US. Clin Schizophr Relat Psychoses. 2011;5:40-49.
11. Dixon LB, Dickerson F, Bellack AS, et al. The 2009
schizophrenia PORT psychosocial treatment recommendations and summary
statements. Schizophr Bull. 2010;36:48-70.
12. Lieberman JA, Stroup TS, McEvoy JP, et al, for the
Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE)
Investigators. Effectiveness of antipsychotic drugs in patients with
chronic schizophrenia. N Engl J Med. 2005;353:1209-1223.
13. Leucht S, Corves C, Arbter D, et al. Second-generation
versus first-generation antipsychotic drugs for schizophrenia: a
meta-analysis. Lancet. 2009;373:31-41.
14. Miyamoto S, Miyake N, Jarskog LF. Pharmacological
treatment of schizophrenia: a critical review of the pharmacology and
clinical effects of current and future therapeutic agents. Mol Psychiatry. 2012 May 15 [Epub ahead of print].
15. Tandon R, Nasrallah HA, Keshavan MS. Schizophrenia,
“just the facts” 5. Treatment and prevention. Past, present, and future.
Schizophr Res. 2010;122:1-23.
16. Arif SA. Iloperidone: a new drug for the treatment of schizophrenia. Am J Health Syst Pharm. 2011;68:301-308.
17. Kane JM. Lurasidone: a clinical overview. J Clin Psychiatry. 2011;72(suppl 1):24-28.
18. Novakovic V, Barkin RL, Hamner MB. Schizophrenia: improving the continuity of care to ensure optimal patient outcomes. Dis Mon. 2012;58:395-409.
To comment on this article, contact rdavidson@uspharmacist.com.





