US Pharm. 2012;37(3):22-27.
Syncope, also referred to as fainting or passing out, is a temporary and sudden loss of consciousness, typically due to transient cerebral hypoperfusion—or simply put, a decline in blood flow to the brain.1-3 Experiencing an episode of syncope may be frightening, not only for the patient, but for observers as well. While some individuals have a single fainting episode, others may faint repeatedly over time, resulting in limitation of activities such as driving. While syncope affects all age groups and can occur in otherwise healthy people, it occurs more often in the elderly.3 Syncope often results in falls, and in older adults, a fracture secondary to a fall is more likely to ensue.4 Additional complications from recurrent falls can include lacerations and intracranial trauma.5 In some cases of syncope, pharmacotherapy is introduced to prevent complications and reduce morbidity.
Independent Risk Factor: Advancing Age
Syncope in seniors can be attributed to age-related neurohumoral and physiological changes in conjunction with medications (TABLE 1) and comorbid chronic diseases, ultimately decreasing the delivery of cerebral oxygen via multiple mechanisms.6
While 60% of persons experience their first faint (syncope) at younger
than 25 years of age, 10% to 15% have their first faint after 65 years
of age.7,8 Advancing age, which correlates with increasing
frequency of coronary artery and myocardial disease, arrhythmia,
vasomotor instability, autonomic failure, polyneuropathy, and use of
polypharmacy, is an independent risk factor for both syncope and death.5 Syncope is the seventh most common reason for emergency department admission of adults over the age of 65.9

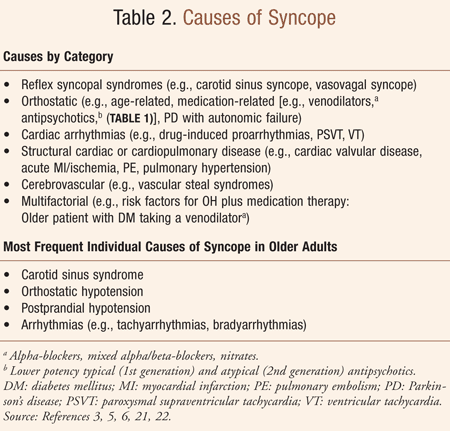
Of note, it may not be possible to attribute a cause (TABLE 2)
of syncope with clarity in 40% to 60% of elderly patients, usually due
to the frequent presence of more than one potential cause.6,10 However, in older patients, categorically, 75% of syncope is attributed to noncardiac causes and 15% is due to cardiac causes.11
Patients with a history of myocardial infarction (MI), arrhythmia,
structural cardiac defects, cardiomyopathies, or congestive heart
failure (CHF) have a uniformly worse prognosis than other patient
groups.5 Higher mortality rates are seen with syncope secondary to cardiac causes irrespective of age.6
In patients with noncardiac or unknown cause of syncope, the following
are important prognostic factors of mortality: older age, male sex, and
a history of CHF.12
Presentation
Syncope occurs with a rapid onset and a spontaneous, complete, and typically prompt recovery.6 A premonitory period may occur and includes dizziness, lightheadedness, nausea, sweating, weakness, and visual disturbances (“white out” or “black out” field of vision).3,6 An individual’s skin may become cold and clammy. The patient experiences loss of postural tone and drops to the floor while losing consciousness.2,3 During the syncopal episode, an individual may be unconscious for a minute or two, but will revive and slowly return to normal.3 In many older adults and those with cognitive impairment, amnesia for loss of consciousness occurs.6
Misdiagnoses of Syncope
Disorders, some common in the elderly, may be misdiagnosed as syncope. These include transient ischemic attacks (e.g., of carotid or vestebrobasilar origin), metabolic disorders (e.g., hypoglycemia), some forms of epilepsy, alcohol and other substance intoxications, and hyperventilation with hypocapnia.6 These conditions may or may not be associated with loss of consciousness.6 In older adults, considering the broad differential diagnosis of syncope would encompass the possibility of stroke (cerebrovascular accident), diabetes, history of seizure disorder, deep venous thrombosis (DVT), or abdominal aortic aneurysm.5
Recent guidelines recommend having the following questions answered to assist with syncopal evaluation: 1) Was loss of consciousness complete? 2) Was loss of consciousness with rapid onset and short duration? 3) Was recovery spontaneous, complete, and without sequelae? 4) Was postural tone lost?5,13 Affirmative responses to all these questions drive the high likelihood of the episode being syncope; if one or more answers are negative, the clinician should consider other forms of loss of consciousness prior to proceeding with syncope evaluation.5,13 An effort should be made to collect all information with respect to symptoms preceding the syncope.
Management of Common Causes of Syncope
TABLE 2 lists the most common causes of syncope. A geriatric clinician encounters the following common individual causes of syncope: orthostatic hypotension, carotid sinus syndrome, vasovagal syncope, postprandial syncope, sinus node disease, atrioventricular block, and ventricular tachycardia. The most frequent individual causes of syncope in older adults are also listed in TABLE 2. The goals of pharmacotherapy are to prevent complications and to reduce morbidity. Data suggest that specialized syncope units (i.e., with protocoled approaches to ruling out cardiac causes) reduce hospital costs and length of stay without compromising quality of care.14 For a more detailed discussion of the management of syncope, refer to references 5 and 6.
Carotid Sinus Syndrome: In asymptomatic carotid sinus hypersensitivity, no treatment is necessary.15 Due to the high rate of injury in symptomatic episodes in seniors, treatment of all patients with a history of two or more symptomatic episodes is considered prudent.6
Currently, the treatment of choice in patients with symptomatic cardioinhibitory carotid sinus syndrome is dual-chamber (atrioventricular sequential) cardiac pacing; syncope can be abolished in 85% to 90% of patients with cardioinhibition.6 Recently, a report of cardiac pacing in older patients with falls who had cardioinhibitory carotid sinus hypersensitivity, syncopal episodes were reduced by 50% during 1 year of follow up in patients who received dual-chamber systems.16
Medication management of vasodepressor carotid sinus syndrome is less successful: Ephedrine has been reported to be useful, but long-term use is limited by side effects; dihydroergotamine is effective but poorly tolerated; fludrocortisone produces good results but its long-term usefulness is limited due to adverse effects.6 Midodrine use appears promising based on a recent small, randomized, controlled trial.17
Another valid treatment option may include surgical denervation of the carotid artery.18
Orthostatic Hypotension (OH): This is the result of failure of normal mechanisms to compensate for the temporary decrease in venous return after standing.2 Medications (TABLE 1, 2) are important causes of OH, among others (e.g., age-related factors, Parkinson’s disease with autonomic failure). Medication-related management of OH in older adults includes: 1) reducing or eliminating agents known to cause OH; 2) avoiding diuretics and eating salt-containing fluids (in patients without congested heart failure); and 3) use of drug therapy to raise blood pressure (BP) such as fludrocortisone, midodrine, ephedrine, desmopressin (DDAVP), octreotide, erythropoietin, and nonsteroidal anti-inflammatory agents.5,6,19 In orthostatic syncope, if not contraindicated, patients are instructed to drink 500 mL of fluid each morning (in addition to their usual routine) and avoid standing up too quickly.5 In addition to medication-related guidance, pharmacists should take advantage of the opportunity to counsel patients on avoiding situations that may exacerbate OH, for example: prolonged standing (motionless) or recumbency, large meals, dehydration, hot showers, hot weather, straining with defecation/voiding, ingesting alcohol, isometric exercise, and hyperventilation.6
Postprandial Hypotension: The medication regimen should be reviewed carefully to eliminate agents associated with hypotension. Orthostatic syncope treatment also focuses on educating the patient to: avoid postprandial dips in BP; elevate the head of their bed to prevent rapid BP fluctuations upon arising; and slowly assuming an upright posture.5 Additional therapy may include thromboembolic disease stockings, fludrocortisone, and other agents such as midodrine.5 The frequency and severity of symptoms in these patients may be decreased through intentional oral fluid consumption, where appropriate.
Vasovagal Syncope: Syncope is suspected to occur secondary to efferent vasodepressor reflexes by a number of mechanisms; decreased peripheral vascular resistance ensues.5 This type of syncope is not life threatening and occurs sporadically.5 Vasovagal syncope is the most common type in young adults but can occur at any age.5 The most common triggers of vasovagal syncope in older adults are prolonged standing and vasodilator medication.6 Some elderly adults are susceptible to syncope secondary to reflex increase in vagal tone caused by situations such as coughing, straining at stool and micturition, which leads to bradycardia and hypotension.10 Involuntary movements may occur during the brief syncopal period, mimicking a seizure.6 Although recovery is typically rapid, symptoms of longer duration (e.g., confusion, disorientation, dizziness) can occur in older patients.6

In the elderly, modifying or discontinuing medications known to cause syncope is often the only necessary intervention. Seniors with hypertension who take antihypertensive medication and develop syncope (i.e., either orthostatic or vasovagal) present a difficult therapeutic dilemma; individualized therapy is required.6 Medication management is necessary in patients who experience symptoms without warning, and fludrocortisone has been reported as useful; midodrine can be used either alone or in combination with fludrocortisone but with caution.6 Serotonin antagonists, such as fluoxetine and sertraline, have been reported to be effective, although further clinical trials need to validate this finding.6 Adjuvant therapies include elastic support hose, relaxation techniques (biofeedback), and conditioning using repeated head-up tilt as therapy.6 In some patients who have recurrent syncope due to cardioinhibitory responses, permanent cardiac pacing is beneficial.20
Conclusion
Sudden, brief loss of consciousness, known as syncope, is followed by spontaneous revival. Although the cause is often unknown, pharmacists can assist in identifying medication-related causes and contributing factors and can recommend pharmacological interventions when necessary to prevent complications and reduce morbidity.
REFERENCES
1. Dorland’s Pocket Medical Dictionary. 28th ed. Philadelphia, PA: Elsevier Saunders; 2009.
2. Beers MH, Porter RS, Jones TV, et al. The Merck Manual
of Diagnosis and Therapy. 18th ed. Whitehouse Station, NJ: Merck
Research Laboratories; 2006:584-588.
3. NINDS Syncope Information Page. National Institute of
Neurological Disorders and Stroke. National Institutes of Health.
Updated October 4, 2011. www.ninds.nih.gov/disorders/syncope/
syncope.htm. Accessed February 20, 2012.
4. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck
Manual of Health & Aging. Whitehouse Station, NJ: Merck Research
Laboratories; 2004:239-253.
5. Morag R. Syncope. Medscape. Updated: August 11, 2011.
http://emedicine.medscape.com/article/811669-overview. Accessed
February 20, 2012.
6. Kenny RA. Syncope. In: Fillit HM, Rockwood K,
Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and
Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:338-347.
7. Chen LY, Shen WK, Mahoney DW, et al. Prevalence of syncope in a population aged more than 45 years. Am J Med.
2006;119(12):[epub1081-epub1108.7].
8. van Dijk N, Boer MC, De Santo T, et al. Daily, weekly,
monthly, and seasonal patterns in the occurrence of vasovagal syncope
in an older population. Europace. 2007;9(9):823-828.
9. Romme JJ, van Dijk N, Boer KR, et al. Influence of age
and gender on the occurrence and presentation of reflex syncope. Clin
Auton Res. 2008;18(3):127-133.
10. Kane RL, Ouslander JG, Abrass IB. Essentials of Clinical Geriatrics. 5th ed. New York, NY: McGraw-Hill, Inc; 2004:223-227.
11. Galizia G, Abete P, Mussi C, et al. Role of early
symptoms in assessment of syncope in elderly people: results from the
Italian group for the study of syncope in the elderly. J Am Geriatr
Soc.
12. Parry SW, Frearson R, Steen N, et al. Evidence-based
algorithms and the management of falls and syncope presenting to acute
medical services. Clin Med. 2008;8(2):157-162.
13. Moya A, Sutton R, Ammirati F, et al. Guidelines for
the diagnosis and management of syncope (version 2009): the Task Force
for the Diagnosis and Management of Syncope of the European Society of
Cardiology (ESC). Eur Heart J. 2009;30(21):2631-2671.
14. Shen WK, Decker WW, Smars PA, et a. Syncope
Evaluation in the Emergency Department Study (SEEDS): a
multidisciplinary approach to syncope management. Circulation. 2004;110(24):3636-3645.
15. Kerr SRJ, Pearce MS, Brayne C, et al. Carotid sinus
hypersensitivity in asymptomatic older persons: implications for
diagnosis of syncope and falls. Arch Intern Med. 2006;166(5):515-520.
16. Kenny RAM, Richardson DA, Steen N, et al. Carotid
sinus syndrome: a modifiable risk factor for nonaccidental falls in
older adults (SAFE PACE). J Am Coll Cardiol. 2001;38(5):1491-1496.
17. Moore A, Watts M, Sheehy T, et al. Treatment of
vasodepressor carotid sinus syndrome with midodrine: a randomized,
controlled pilot study. J Am Geriatr Soc. 2005;53(1):114-118.
18. Tooron RJ, Scheltinga MR, Bender MH, et al. Effective
surgical treatment of the carotid sinus syndrome. J Cardiovasc Surg.
2009;50(5):683-766.
19. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 16th ed. Hudson, OH: Lexi-Comp, Inc; 2011.
20. Raviele A, Giada F, Menozzi C, et al: A randomized,
double-blind, placebo-controlled study of permanent cardiac pacing for
the treatment of recurrent tilt-induced vasovagal syncope. The
vasovagal syncope and pacing trial (SYNPACE). Eur Heart J.
2004;25(19):1741-1748.
21. Saseen JJ, Maclaughlin EJ. Hypertension. In: DiPiro
JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic
Approach. 7th ed. New York, NY: McGraw-Hill Inc; 2008:156.
22. Crimson ML, Argo TR, Buckey PF. Schizophrenia.In:
DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A
Pathophysiologic Approach. 7th ed. New York, NY: McGraw-Hill Inc;
2008:1111.
To comment on this article, contact rdavidson@uspharmacist.com.





