US Pharm. 2009;34(7):30-35.
Asthma is a chronic airway disease characterized by airflow obstruction, bronchial hyperresponsiveness, and inflammation.1 There are many triggers and comorbid conditions that have been shown to increase asthma symptoms and/or precipitate asthma exacerbations. The Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma recognizes gastroesophageal reflux disease (GERD) as a comorbid condition of asthma and recommends medical management of GERD in appropriate patients.1
The relationship between asthma and GERD has been discussed for many years. In 1892, Sir William Osler described an association: “severe paroxysms of asthma may be induced by overloading the stomach, or by taking certain articles of food.”2 Although these two disorders often occur together, the relationship between GERD and asthma remains unclear. This article will review the prevalence, proposed pathophysiology, and treatment recommendations for persons with both asthma and GERD.
Prevalence
In the United States, an estimated 20 million people have asthma, and almost 20% of the U.S. population suffers from the classic symptoms of GERD, such as heartburn and regurgitation, at least once a week.3,4 The prevalence of GERD in patients with asthma is estimated to be 34% to 89%.5
Although it remains unclear whether or not a true causal relationships exists, several studies show that GERD symptoms tend to be increased in patients with asthma. Field et al investigated the prevalence of symptomatic gastroesophageal reflux using a questionnaire-based survey.6 Among the 109 patients with asthma who participated in the study, 77% experienced heartburn and 55% experienced regurgitation; symptoms were higher than in the control groups. O’Connell et al also utilized a symptom survey to examine prevalence of GERD in 189 patients with asthma in a Veterans Administration (VA) hospital.7 Seventy-two percent of the patients reported heartburn. Perrin-Fayolle et al found reflux symptoms in 65% of 150 surveyed patients with asthma.8 These results suggest that the prevalence of GERD symptoms in patients with asthma is increased; however, it does not establish causality.
Pathophysiology of GERD-induced Asthma
Several proposed mechanisms about the pathophysiology of GERD-induced asthma exist, although these mechanisms are not completely understood. Proposed mechanisms of GERD-induced asthma include a vagally mediated reflex, heightened bronchial reactivity, microaspiration, and immune system modification.
Vagal Reflex: The esophagus and bronchial tree share embryonic origins and innervation through the vagus nerve; therefore, acid in the esophagus could stimulate esophageal receptors, initiating a vagally mediated reflex.9 Many studies show that the vagally mediated reflex mechanism is important to GERD-induced bronchoconstriction, while others report conflicting data. Mansfield and Stein showed that patients with reflux had a 10% increase in airway flow resistance.10 Wright et al measured airflow and arterial oxygen saturation before and after esophageal acid infusions in 136 individuals.11 Results indicated that there was a significant decrease in both airflow and arterial oxygen saturation after infusion of the acid.
Other studies have failed to show significant pulmonary response to esophageal acid. Field analyzed 18 studies that reviewed the effects of GERD on pulmonary function in adults with asthma.12 He concluded that the effects of esophageal acid on pulmonary function are minimal and only affect a minority of subjects. In patients with nocturnal asthma, Tan et al found no significant changes in airflow resistance when esophageal acid was present.13
Heightened Bronchial Reactivity: Another proposed mechanism of GERD-induced asthma is heightened bronchial reactivity. Some data suggest that exposure to esophageal acid may increase bronchial activity to other stimuli. Herve et al reported on the effects of esophageal acid on expiratory flow with methacholine challenge testing.14 When esophageal acid was infused versus normal saline, the total dose of methacholine needed to reduce the forced expiratory volume in one second (FEV1) by 20% was significantly lower.
Microaspiration: Microaspiration of gastric acid into the larynx and upper airway could cause stimulation of the upper airway and increase airway resistance. Jack et al showed that microaspiration of gastric fluid into the upper airway may trigger asthma symptoms in patients with asthma.15 When the esophageal and endotracheal pH was decreased, the mean peak expiratory flow fell 84 L/min. When acid was introduced in the esophagus without microaspiration of gastric fluid into the trachea, the peak expiratory flow fell only 8 L/min. In an animal study, Tuchman et al found a significant increase in response when acid was introduced directly into the trachea versus the esophagus.16 Although microaspiration may be an inducer of bronchial reactivity, other studies suggest that microaspiration does not play a significant role in GERD-induced asthma.17
Immune System Modification: A recent study conducted at Duke University showed that GERD may alter the immune system’s response to allergens, further strengthening the link between GERD and asthma.18 Researchers compared the immune system’s response to allergens in mice with gastric fluid in the lungs to its response in normal mice. Results showed that the mice with GERD developed a response similar to that found in patients with asthma by releasing a type 2 helper T cell. The comparison group’s response was more balanced, releasing both type 1 and type 2 helper T cells. This study shows that microaspiration may lead the immune system to generate an asthmatic response.
Other Factors
Many factors may lead to GERD development in patients with asthma. Potential predisposing elements include an increased pressure gradient, airway obstruction, and asthma medications. During an asthma exacerbation, there may be an increase in negative pleural pressure, which increases pressure on the diaphragm. This may override lower esophageal pressure, thereby promoting reflux.19
Airway obstruction may also predispose asthma patients to GERD by relaxing the lower esophageal sphincter (LES). Zerbib et al showed that airflow obstruction significantly increased the number of LES relaxations and the number of reflux episodes.20 The number of LES relaxations decreased when airflow obstruction was reversed.
Bronchodilator medications may decrease lower esophageal pressure, which favors gastroenterologic reflux. One study found a 24% increase in reflux time and a threefold increase in symptoms over baseline with theophylline therapy. Patients with subtherapeutic levels of theophylline did not have a significant increase in reflux symptoms.21 Another study examined the effects of nebulized albuterol versus placebo on lower esophageal relaxation and reported that albuterol therapy reduced lower esophageal tone and may increase the likelihood of acid reflux in a subset of patients.22 Furthermore, oral corticosteroids have been shown to increase esophageal acid contact time significantly.23 However, Field et al reported that no asthma medications were associated with an increased likelihood of having GERD symptoms.6
Diagnosing GERD in Patients With Asthma
Every patient with asthma should be asked about GERD as well. Questions should include whether frequent cough and hoarseness are present and whether asthma symptoms occur after meals or when lying down. In addition, inhaler use when experiencing GERD symptoms should be assessed.5 The signs and symptoms of GERD are listed in TABLE 1.
If typical GERD symptoms are present, a trial of pharmacologic therapy is warranted. Empiric therapy is considered successful if asthma outcomes are improved.24 Further testing is recommended in patients in whom empiric therapy is unsuccessful or who have symptoms suggesting complicated GERD.5 Of note, many asthma patients with GERD do not experience reflux symptoms; this subset of patients may be difficult to diagnose.

Treatment
The current asthma guidelines recommend that medical management of GERD be instituted for patients who have asthma and complain of frequent heartburn (pyrosis), particularly those who have frequent episodes of nocturnal asthma.1 Three categories of medications are widely available for the treatment of reflux disease: proton pump inhibitors (PPIs), H2 antagonists, and antacids.
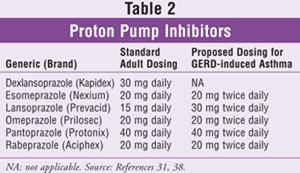
Proton Pump Inhibitors: The PPIs are the most potent inhibitors of gastric secretion available and the recommended therapy when treating GERD-induced asthma. These medications suppress gastric acid secretion by inhibition of the hydrogen-potassium adenosine triphosphatase (H+, K+–ATPase) enzyme system found on the surface of parietal cells. PPIs should be administered 30 to 60 minutes before meals. Dexlansoprazole (the newest PPI), pantoprazole, and rabeprazole may be taken without regard to timing of meals. A minimum of 3 months of therapy is recommended. Common adverse effects include abdominal pain, nausea, diarrhea, and headache.25 The available PPIs, their standard adult dosing, and their proposed dosing in GERD-related asthma are displayed in TABLE 2.
Studies evaluating the efficacy of PPIs on asthma outcomes have been conducted. In a trial evaluating the dose of omeprazole required for adequate acid suppression in 30 nonsmoking adults with asthma and GERD, 73% of subjects had improved asthma symptoms and/or peak expiratory flow rates after 3 months.26 Many of the subjects required more than the standard dose (20 mg/day) to suppress the acid; therefore, a high-dose PPI (i.e., double-standard or twice-daily dosing) is recommended in the treatment of coexisting asthma and GERD. In a double-blind, placebo-controlled, crossover study, 107 patients with asthma were randomized to either omeprazole 40 mg/day or placebo for 8 weeks.27 A significant reduction in nighttime asthma symptoms was found in the omeprazole group, although daytime symptoms did not improve. Ford et al noted no improvements in daytime or nocturnal symptoms using omeprazole 20 mg/day for 4 weeks.28
Littner et al reported the effects of lansoprazole on asthma symptoms in patients with severe asthma and reflux.29 Lansoprazole did not improve daily asthma symptoms; however, therapy did significantly decrease the number of asthma exacerbations and improved quality of life. In a study evaluating the effects of esomeprazole on asthma outcomes in patients with asthma, esomeprazole improved the peak expiratory flow in subjects with both nocturnal symptoms and GERD. No significant improvement in peak expiratory flow was detected in other subjects.30
H2 Antagonists: H2-receptor antagonists inhibit acid secretion by blocking histamine receptors on the parietal cell. Four H2 antagonists are currently available in the U.S.: cimetidine (Tagamet), famotidine (Pepcid), nizat idine (Axid), and ranitidine (Zantac). Depending on the severity of the disease, H2 antagonists can be given in low (OTC), standard, and high doses. For example, standard doses of H2 antagonists include cimetidine 400 mg four times daily or 800 mg twice daily, famotidine 20 mg twice daily, nizatidine 150 mg twice daily, and ranitidine 150 mg twice daily. The dosage of these medications should be reduced by 50% in patients with moderate-to-severe renal failure. Common side effects include headache, fatigue, dizziness, and gastrointestinal (GI) disturbances.31
Cimetidine, and to a much lesser extent ranitidine, can inhibit the CYP450 system. Drugs metabolized via the CYP450 system, such as theophylline and warfarin, may be affected. Famotidine and nizatidine do not inhibit this pathway; therefore, drug interactions mediated by hepatic metabolism are not expected. Drug interactions, especially with cimetidine, should be monitored.31
In a study evaluating 18 patients with both asthma and GERD, 14 patients felt that their chest symptoms had improved significantly after cimetidine therapy.32 Another trial reported the effects of ranitidine 150 mg twice daily for 4 weeks on reflux and asthma control. Only a modest improvement in nocturnal asthma occurred, with no change in lung function and peak flow values.33
Antacids: Antacids relieve heartburn and dyspepsia by neutralizing gastric acid. In addition to increasing the intragastric pH, they may also increase LES pressure. Several nonprescription antacid products are available, including Alka-Seltzer, Gaviscon, and Maalox (i.e., aluminum and magnesium salts). Most of these products are inexpensive, making them a desirable option for patients seeking temporary relief of symptoms.34 Generally, antacids have a short duration of action, requiring frequent daily administration. Dosing intervals range from hourly to as needed. These products may cause GI side effects and acid-base disturbances. Significant interactions with drugs, including iron and tetracycline, may occur.31 In a trial evaluating the effectiveness of Gaviscon and lifestyle changes in patients with GERD and asthma, there was a 44% improvement in symptoms only. Lung function tests did not differ between the treatment and control groups.35
Surgical Interventions: Surgical therapy, such as laparoscopic Nissen fundoplication, is an option for patients who have failed to respond to medications, experience complications of GERD, or have elected to have surgery despite successful medication therapy. Several studies suggest that surgical intervention improves asthma symptom control. Sontag et al reported complete resolution of asthma symptoms after surgery in 6 of 13 patients.36 After reviewing 24 reports of surgical antireflux therapy in patients with asthma, Field et al reported that GERD and asthma symptoms were improved in 90% and 79% percent of the subjects, respectively.37 Surgical antireflux therapy has been found superior to an H2 antagonist; comparisons with PPIs were found to be similar.31
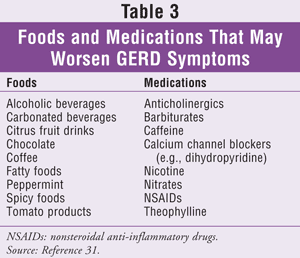
Lifestyle Modifications: Asthma symptoms associated with GERD can be aggravated by high-fat meals that delay gastric emptying and foods that lower LES pressure. Eating or drinking acidic foods may also trigger symptoms.31 Foods and medications that may worsen GERD symptoms are shown in TABLE 3.
Lifestyle changes should be initiated in patients with both asthma and GERD. These modifications include elevating the head of the bed on 6- to 8-inch blocks, avoiding food and drink at least three hours before retiring, and not lying down within 2 hours after a meal. Other lifestyle modifications include weight reduction, smoking cessation, and alcohol avoidance. These patients should also avoid foods and drinks that may worsen symptoms of GERD.
Conclusion
Health care providers should be aware that GERD is a potential trigger of asthma, although not all asthma patients with GERD experience reflux symptoms. All patients with asthma should be questioned about reflux symptoms, and antireflux therapy, in particular high-dose PPI therapy, should be initiated if appropriate. If symptoms are not improved after 3 months of empiric therapy, then either reflux is inadequately controlled or GERD-induced asthma is not present. Referral to a gastroenterologist may be warranted.
REFERENCES
2. Osler W. The Principles and Practice of Medicine. Birmingham, AL: LB Adams; 1892:497-503.
3. Surveillance for asthma–United States, 1908-2005. MMWR. 2007;56:1-60.
4. Locke GR, Talley NJ, Fett SL, et al. Prevalence and clinical spectrum of gastroesophageal reflux: a population-based study in Olmsted County, Minnesota. Gastroenterology. 1997;112:1448-1456.
5. Harding SM, Richter JE. The role of gastroesophageal reflux in chronic cough and asthma. Chest. 1997;111:1389-1402.
6. Field SK, Underwood M, Brant R, Cowie RL. Prevalence of gastroesophageal reflux symptoms in asthma. Chest. 1996;109:316-322.
7. O’Connell S, Sontag SJ, Miller T, et al. Asthmatics have a higher prevalence of reflux symptoms regardless of the use of bronchodilators [abstract]. Gastroenterology. 1990;98:A97.
8. Perrin-Fayolle, Bel A, Kofman J, et al. Asthma and gastroesophageal reflux. Results of a survey of over 150 cases. Poumon Coer. 1980;36:225-230.
9. Richter JE. Gastroesophageal reflux disease and asthma: the two are directly related. Am J Med. 2000;108(suppl 4A):153S-158S.
10. Mansfield LE, Stein MR. Gastroesophageal reflux and asthma: a possible reflex mechanism. Ann Allergy. 1978;41:224-226.
11. Wright RA, Miller SA, Corsello BF. Acid-induced esophagobronchial-cardiac reflexes in humans. Gastroenterology. 1990;99:71-73.
12. Field SK. A critical review of the studies of the effects of simulated or real gastroesophageal reflux on pulmonary function in asthmatic adults. Chest. 1999;115:848-856.
13. Tan WC, Martin RJ, Pandey R, Ballard RD. Effects of spontaneous and stimulated gastroesophageal reflux on sleeping asthmatics. Am Rev Respir Dis. 1990;141:1394-1399.
14. Herve P, Denjean A, Jian R, et al. Intraesophageal perfusion of acid increases the bronchomotor response to methacholine and to isocapnic hyperventilation in asthmatic subjects. Am Rev Respir Dis. 1986;134:986-989.
15. Jack CI, Calverley PM, Donnelly RJ, et al. Simultaneous tracheal and esophageal pH measures in asthma patients with gastroesophageal reflux. Thorax. 1995;50:201-204.
16. Tuchman DN, Boyle JT, Pack AI, et al. Comparison of airway responses following tracheal or esophageal acidification in a cat. Gastroenterology. 1984;87:872-881.
17. Harding SM, Schan CA, Guzzo MR, et al. Gastroesophageal reflux-induced bronchoconstriction. Is microaspiration a factor? Chest. 1995;108:1220-1227.
18. Barbas AS, Downing TE, Balsara HE. Chronic aspiration shifts the immune response from Th1 to Th2 in a murine model of asthma. Eur J Clin Invest. 2008;38:596-602.
19. Mittal RK, Balaban DH. The esophagogastric junction. N Engl J Med. 1997;336:924-932.
20. Zerbib F, Guisset O, Lamouliatte H, et al. Effects of bronchial obstruction on lower esophageal sphincter motility and gastroesophageal reflux in patients with asthma. Am J Respir Crit Care Med. 2002;166:1206-1211.
21. Ekstrom T, Tibbling L. Influence of theophylline on gastro-oesophageal reflux and asthma. Eur J Clin Pharmacol. 1988;35:353-356.
22. Crowell MD, Zayat EN, Lacy BE, et al. The effects of an inhaled beta2-adrenergic agonist on lower esophageal function: a dose-response study. Chest. 2001;120:1184-1189.
23. Lazenby JP, Guzzo MR, Harding SM, et al. Oral cortico steroids increase esophageal acid contact times in patients with stable asthma. Chest. 2002;121:625-634.
24. Harding SM. Gastroesophageal reflux and asthma. www.uptodate.com. Accessed August 6, 2008.
25. Boparai V, Rajagopalan J, Triadafilopoulos G. Guide to the use of proton pump inhibitors in adult patients. Drugs. 2008;68:925-947.
26. Harding SM, Richter JE, Guzzo MR, et al. Asthma and gastroesophageal reflux: acid-suppressive therapy improves asthma outcome. Am J Med. 1996;100:395-405.
27. Kiljander TO, Salomaa ER, Hietanen EK, Terho EO. Gastroesophageal reflux in asthmatics: a double-blind, placebo-controlled crossover study with omeprazole. Chest. 1999;116:1257-1264.
28. Ford GA, Oliver PS, Prior JS, et al. Omeprazole in the treatment of asthmatics with nocturnal symptoms and gastro-esophageal reflux: a placebo-controlled crossover study. Postgrad Med J. 1994;70:350-354.
29. Littner MR, Leung FW, Ballard ED II, et al. Effects of 24 weeks of lansoprazole therapy on asthma symptoms, exacerbations, quality of life, and pulmonary function in adult asthmatic patients with acid reflux symptoms. Chest. 2005;128:1128-1135.
30. Kiljander TO, Harding SM, Field SK, et al. Effects of esomeprazole 40 mg twice daily on asthma. Am J Respir Crit Care Med. 2006;173:1091-1097.
31. Williams DB, Schade RR. Gastroesophageal reflux disease. In: DiPiro JT, Talbert RL, Yee GC, et al. Pharmacotherapy: A Pathophysiologic Approach. 6th ed. New York, NY: McGraw-Hill; 2005:613-628.
32. Goodall RJ, Earis JE, Cooper DN, et al. Relationship between asthma and gastroesophageal reflux. Thorax. 1981;36:116-121.
33. Ekstrom T, Lindgren BR, Tibbling L. Effects on ranitidine treatment on patients with asthma and a history of gastro esophageal reflux: a double blind crossover study. Thorax. 1989;44:19-23.
34. Zweber A, Berardi RR. Heartburn and dyspepsia. In: Berardi RR, Kroon LA, McDermott JH, et al. Handbook of Nonprescription Drugs: An Interactive Approach to Self Care. 15th ed. Washington, DC: American Pharmacists Association; 2006:265-281.
35. Kjellen G, Tibbling L, Wranne B. Effects of conservative treatment of oesophageal dysfunction on bronchial asthma. Eur J Respir Dis. 1981;62:190-197.
36. Sontag S, O’Connell SO, Greenlee H, et al. Is gastroesophageal reflux a factor in some asthmatics? Am J Gastroenterol. 1987;82:119-126.
37. Field SK, Gelfand GA, McFadden SD. The effects of antireflux surgery on asthmatics with gastroesophageal reflux. Chest. 1999;116:766-774.
38. Kiljander TO. The role of proton pump inhibitors in the management of gastroesophageal reflux disease-related asthma and chronic cough. Am J Med. 2003;115(suppl 3A):65S-71S.
To comment on this article, contact rdavidson@jobson.com.






