US Pharm. 2011;36(12):41-44.
Functional bowel disorders (FBDs) are gastrointestinal (GI) disorders related to the middle or lower GI tract that lack identifiable pathoetiology.1,2 FBDs include irritable bowel syndrome (IBS); recurrent abdominal pain (RAP); chronic bloating, constipation, and/or diarrhea; and other unspecified chronic bowel disorders.1 Hadler et al reported FBDs in up to 40% of the community.3 In 2004, it was estimated that 4 out of every 100 emergency department visits were due to FBDs, accounting for more than 11 million visits.2 In a study of 3,933 subjects, 18% reported chronic diarrhea, 16% chronic constipation, 15% abdominal pain, 10% symptoms of IBS, and 2% dyspepsia. The economic burden is estimated to be as high as $1.6 billion for IBS and $621 million for chronic diarrhea.4
Functional Bowel Disorders
Irritable Bowel Syndrome: Despite the research dedicated to IBS, there is little known about its cause or development process. The most recent comprehensive prevalence study, conducted in 2002, found that IBS occurred in 3% to 20% of North Americans.5 IBS is a similar issue globally in both developed and developing countries.6 Chang et al estimated that in 1 year, IBS accounted for 500,000 inpatient hospital stays.7 Women reported an incidence of 2:1 compared to men.5 Triggers for IBS include stress, hormonal fluctuations, and certain foods, including chocolate, alcohol, carbonated beverages, fruits, and vegetables.5,8 Diagnosis is predominantly based on symptoms, defined as abdominal pain and altered bowel activity with no organic origin.5
IBS affects the large intestine, causing cramping, abdominal pain, bloating, gas, diarrhea, and constipation. It is classified into several subtypes: diarrhea (IBS-D), constipation (IBS-C), and a mixed subtype (IBS-M). Fortunately, IBS does not cause permanent damage to the colon and few people have disabling symptoms. IBS is generally managed through diet, lifestyle changes, and stress reduction techniques. When these techniques fail, symptom-based pharmacotherapy is employed. Constipation may be treated with prokinetic agents, while diarrhea may be treated with antispasmodics, opioids, 5-HT3 antagonists, and/or anticholinergics.5
Recurrent Abdominal Pain: RAP is another major form of FBD that is common in children. It is considered pain severe enough to interfere with normal functioning at least once per month for 3 consecutive months.9 For decades, the pathophysiology of RAP has remained unclear. The original research and defining of RAP came from a British pediatrician, John Apley, MD. In establishing the definition of RAP, Apley and Naish surveyed 1,000 primary and secondary school children.9 Approximately 11% of the children met the criteria for RAP. Another study conducted by Hyams et al evaluated 507 adolescents in an American suburban area.10 Of the adolescents studied, approximately 15% experienced abdominal pain on a weekly basis. However, only half sought medical attention, implying the potential for a higher rate of occurrence than seen in clinical practice.11 Many pediatricians treat RAP predominantly with emotional support and reassurance for the family that no serious disease is present.12

Fructose Malabsorption
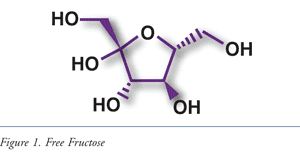
One area gaining interest with those who study FBD is fructose malabsorption, a condition characterized by gas, bloating, discomfort, nausea, disturbed bowel function, and occasionally gastroesophageal reflux (TABLE 1).13 During fructose malabsorption, the small intestines are unable to fully absorb ingested fructose, leading to increased osmotic load and bacterial fermentation, as well as promotion of mucosal biofilm formation.14 This is distinguished from fructose intolerance, a hereditary disease caused by a mutation in the aldolase B gene that renders patients unable to metabolize fructose. This metabolic disease may result in hepatic and renal injury, growth retardation, and, in severe cases, even death.15-17
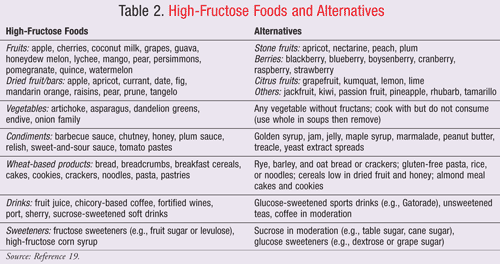
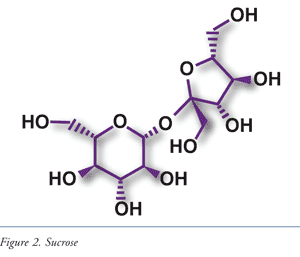
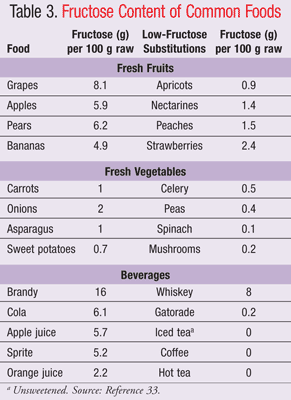
Fructose, the sweetest of all naturally occurring sugars, is found in four primary forms: a naturally occurring free fructose (FIGURE 1), as a constituent of sucrose (FIGURE 2), as a polymer, and in an enzymatically produced form. Free fructose makes up as much as 35% by weight of honey and fruits such as apples, pears, and cherries (TABLE 2). Prior to the advent of food-processing technology in the 1960s, honey and fruits were the main dietary sources of fructose.18 Since that time, technology has led to the use of alternatives, including sucrose (a disaccharide of fructose and glucose commonly known as table sugar) and high-fructose corn syrup or HFCS (a monosaccharide enzymatically produced from corn). Today HFCS is commonly found in a variety of beverages and baked goods, as well as in canned and processed foods.19,20
The availability of inexpensive, tasty, fructose-laden products makes reducing or eliminating fructose from the diet difficult. According to the U.S. Agriculture Fact Book, HFCS consumption increased from 16% to 42% of total sweetener consumption between the years 1978 and 1999.21,22 In addition to its effect on the GI tract, a recent study by Stanhope et al evaluating the health consequences of excessive HFCS consumption found an increase in postprandial triglycerides, low-density lipoprotein (LDL) cholesterol, and other coronary heart disease risk factors after 2 weeks of consuming fructose- or HFCS-sweetened beverages (as 25% of their total daily energy requirement).23 Furthermore, the authors discovered a decrease in postprandial glucose and insulin response following fructose consumption. These findings confirm that side effects of long-term, sugar-sweetened beverage consumption can be attributed to specific properties of fructose.23,24
Pathophysiology of Fructose Malabsorption
Fructose empties more rapidly from the stomach in comparison to other sugars, utilizing an energy-dependent absorption process in the small intestines. GLUT5 and GLUT2 are transmembrane proteins primarily located in the lumen of the small intestines that are responsible for the transportation of fructose. GLUT5 transports fructose from the intestinal lumen into enterocytes by a facilitated energy-dependent process. Therefore, saturation of GLUT5 transporters with excessive fructose ingestion results in incomplete absorption, leading to GI symptoms (TABLE 1).25 This transport-mediated process is limited in carrier capacity, calculated to be approximately 15 g of fructose per consumption. Fructose absorption occurs along with glucose via solvent drag and passive diffusion. Due to its osmotic effect, unabsorbed fructose combines with water and is rapidly propelled into the colonic lumen where luminal bacteria ferment fructose to carbon dioxide, hydrogen, and short-chain fatty acids. This osmotic load has a laxative effect and causes rapid gas production, leading to luminal distention, bloating, abdominal discomfort, and increased motility.19
Assessment of Dietary Fructose Intake
The hydrogen breath test is the foundational diagnostic assessment for identification of dietary fructose malabsorption.26 One description of this test comes from a study conducted by Choi et al of 183 patients with unexplained chronic abdominal pain.27 Subjects were asked to refrain from consuming foods containing high fat, lactose, or fructose for 1 day prior to testing and to fast after midnight. Subjects were asked to blow into a modified bag in order to collect a 50 mL end-expiratory breath sample. The sample was injected into a gas chromatography analyzer to measure baseline values for hydrogen and methane. The subjects were then asked to drink a 33% fructose solution. Breath samples were analyzed at 30-minute intervals for 5 hours. Based on the amount of fructose that escaped absorption in the small intestines, commensal flora in the large intestines metabolized the fructose and released hydrogen and methane consequently.28 A positive breath test was inferred in subjects with a rise in breath hydrogen and/or methane of at least 3 parts per million (ppm) over three consecutive breath samples from the baseline value or from having a value 20 ppm above baseline.27
The pitfall of the hydrogen breath test in diagnosis of fructose malabsorption is that 28% of the population does not expel hydrogen through the lungs and/or does not have hydrogen-producing bacteria inhabiting the GI tract.14 In such patients, fructose malabsorption is often undiagnosed due to lack of an alternative diagnostic test.
In the Choi et al study, fructose malabsorption was discovered in 39% of the 183 patients who had consumed 25 g of fructose and in 66% of the patients who had consumed 50 g of fructose, with 73% of total patients having a positive hydrogen breath test.27 To put these quantities of fructose in perspective, depending on the type of corn syrup sweetener used, one 22-oz soft drink contains approximately 30 to 40 g of fructose.
Fructose Malabsorption in IBS
One in three adults with IBS presents with the inability to absorb fructose in 25- to 50-g increments. However, fructose malabsorption is not limited to patients with IBS. Although GI symptoms associated with fructose malabsorption are generally magnified (TABLE 1), the perception that fructose does not play a major role in patients with IBS often leads to a lack of treatment.19
Fructose-Restricted Diet
International consensus on treatment of traditional IBS starts with increased fiber intake as first-line therapy.29 However, there are no published guidelines to assist the patient with fructose malabsorption in constructing a manageable diet.11
Despite the lack of specific guidelines, three separate studies demonstrated that identification and dietary monitoring of fructose consumption in patients with fructose malabsorption was clinically significant in reducing abdominal symptoms.19,30,31 For instance, in the Choi et al study, 31 patients with positive hydrogen breath tests received verbal and written instructions on fructose restriction or exclusion, and then were followed up to 1 year later. Fourteen of the subjects were considered compliant patients and experienced a statistically significant reduction in abdominal pain, belching, bloating, fullness, indigestion, and diarrhea symptom scores compared to baseline 1 year prior.27
In another study, Fernandez-Banares et al found that when given recommendations to eliminate all foods with free fructose, patients showed clinical symptom improvement after just 1 month of dietary adjustment. Furthermore, a group of these patients continued to have symptomatic improvement for up to 1 year later.32
These two studies demonstrate positive impact on clinical symptoms with dietary intervention.27,32 Lack of guidelines on fructose restriction in patients suffering from fructose malabsorption should not deter pharmacists from making such dietary recommendations.
Role of the Pharmacist
As a member of the health care team, pharmacists need to be aware of the common symptoms of fructose malabsorption, in addition to the foods that contain high amounts of fructose.19,33 Although the normal capacity for absorption of fructose is unknown, in general, consumption of fructose in excess of 15 to 25 g in one sitting can lead to malabsorption and FBDs.12,19 Recommendations to substitute foods and beverages containing high amounts of fructose for those containing lower amounts (TABLE 3) can be helpful to patients suffering from fructose malabsorption symptoms. Pharmacists should encourage patients to focus on food alternatives. Realistic goals can positively impact symptoms and improve quality of life.27 Patients should be encouraged to consult with a registered dietitian if they are unable to self-manage dietary needs.
REFERENCES
1. Longstreth GF, Thompson WG, Chey WD, et al. Functional bowel disorders. Gastroenterology. 2006;130:1480-1491.
2. Porter CK, Gormley R, Tribble DR, et al. The incidence and gastrointestinal infectious risk of functional gastrointestinal disorders in a healthy US adult population. Am J Gastroenterol. 2011;106:130-138.
3. Hadler SL, Locke GR III, Chleck CD, et al. Natural history of functional gastrointestinal disorders: a 12-year longitudinal population-based study. Gastroenterology. 2007;133:799-807.
4. Lembo AJ. The clinical and economic burden of irritable bowel syndrome. Pract Gastroenterol. 2007;31(suppl)3-9.
5. Grundmann O, Yoon SL. Irritable bowel syndrome: epidemiology, diagnosis and treatment: an update for health-care practitioners. J Gastroenterol Hepatol. 2010;25:691-699.
6. Tally NJ. Functional gastrointestinal disorders as a public health problem. Neurogastroenterol Motil. 2008;20(suppl 1):121-129.
7. Chang JY, Locke GR, McNally MA, et al. Impact of functional gastrointestinal disorders on survival in the community. Am J Gastroenterol. 2010;105:822-832.
8. Chang L. The role of stress on physiologic responses and clinical symptoms in irritable bowel syndrome. Gastroenterology. 2011;140:761-765.
9. Apley J, Naish N. Recurrent abdominal pains: a field survey of 1,000 school children. Arch Dis Child. 1958;33:165-170.
10. Hyams JS, Burke G, Davis PM, et al. Abdominal pain and irritable bowel syndrome in adolescents: a community-based study. J Pediatr. 1996:129:220-226.
11. Rao SS, Attaluri A, Anderson L, Stumbo P. The ability of the normal human small intestine to absorb fructose: evaluation of breath testing. Clin Gastroenterol Hepatol. 2007;5:959-963.
12. Weydert JA, Ball TM, Davis MF. Systemic review of treatments for recurrent abdominal pain. Pediatrics. 2003;111:e1-e11.
13. Piche T, Des Varannes SB, Sacher-Huvelin S, et al. Colonic fermentation influences lower esophageal sphincter function in gastroesophageal reflux disease. Gastroenterology. 2003;124:894-902.
14. Gibson PR, Newnham E, Barrett JS, et al. Review article: fructose malabsorption and the bigger picture. Aliment Pharmacol Ther. 2007;25:349-363.
15. Wong D. Hereditary fructose intolerance. Mol Genet Metab. 2005;85:165-167.
16. Ali M, Rellos P, Cox TM. Hereditary fructose intolerance. J Med Genet. 1998;35:353-365.
17. Bouteldja N, Timson DJ. The biochemical basis of hereditary fructose intolerance. J Inherit Metab Dis. 2010;33:105-112.
18. Hanover LM, White JS. Manufacturing, composition and applications of fructose. Am J Clin Nutr. 1993;58(suppl):724S-732S.
19. Shepherd SJ, Gibson PR. Fructose malabsorption and symptoms of irritable bowel syndrome: guidelines for effective dietary management. J Am Diet Assoc. 2006;106:1631-1639.
20. Skoog SM, Bharucha AE. Dietary fructose and gastrointestinal symptoms: a review. Am J Gastroenterol. 2004;99:2046-2050.
21. Agriculture Fact Book 2000. Washington, DC: U.S. Department of Agriculture; 2000:314. www.usda.gov/news/pubs/
22. Marriott BP, Cole N, Lee E. National estimates of dietary fructose intake increased from 1977 to 2004 in the United States. J Nutr. 2009;139:1228S-1235S.
23. Stanhope KL, Bremer AA, Medici V, et al. Consumption of fructose and high fructose corn syrup increase postprandial triglycerides, LDL-cholesterol, and apolipoprotein-B in young men and women. J Clin Endocrinol Metab. 2011;96:E1596-E1605.
24. Hu FB, Malik VS. Sugar-sweetened beverages and risk of obesity and type 2 diabetes: epidemiologic evidence. Physiol Behav. 2010;100:47-54.
25. Douard V, Ferraris RP. Regulation of the fructose transporter GLUT5 in health and disease. Am J Physiol Endocriol Metab. 2008;295:E227-E237.
26. Romagnuolo JM, Schiller D, Bailey RJ. Using breath tests wisely in a gastroenterological practice: an evidence based review of indications and pitfalls in interpretation. Am J Gastroenterol. 2002;97:1113-1126.
27. Choi YK, Johlin FC, Summers RW, et al. Fructose intolerance: an under-recognized problem. Am J Gastroenterol. 2003;98:1348-1353.
28. Jones HF, Butler RN, Brooks DA. Intestinal fructose transport and malabsorption in humans. Am J Physiol Gastrointest Liver Physiol. 2011;300:G202-G206.
29. DecisionBase. Irritable Bowel Syndrome: A New Therapy for Non-Constipation-Predominant IBS With Greatly Improved Efficacy Will Reach Near-Blockbuster Status. Decision Resources. Inc. March 2010. http://decisionresources.com/
30. Choi YK, Kraft N, Zimmerman B, et al. Fructose intolerance in IBS and utility of fructose-restricted diet. J Clin Gastroenterol. 2008;42:233-238.
31. Johlin FC Jr, Panther M, Kraft N. Dietary fructose intolerance: diet modification can impact self-rated health and symptom control. Nutr Clin Care. 2004;7:92-97.
32. Fernandez-Banares F, Rosinach M, Esteve M, et al. Sugar malabsorption in functional abdominal bloating: a pilot study on the long-term effect of dietary treatment. Clin Nutr. 2006;25:824-831.
33. Nutrition Data Laboratory. USDA. www.nal.usda.gov/fnic/
To comment on this article, contact rdavidson@uspharmacist.com.