US Pharm. 2011;36(1):HS-12-HS-18.
Insomnia is a common complaint in hospitalized patients, especially the elderly.1 It is characterized by an increase in sleep latency (trouble falling asleep), a decrease in sleep maintenance (trouble staying asleep), or a decline in sleep quality (less time sleeping compared with time spent in bed).2 In one study, 47% of 222 patients reported that they had insomnia and/or excessive daytime somnolence while in the hospital. Interestingly, when the medical records were reviewed, no patient had physician documentation of insomnia symptoms.1 In a longitudinal observational study of insomnia prevalence in 280 hospitalized elderly patients, 21% reported new-onset insomnia, 38% reported moderate or severe insomnia, and 38% reported sleep disturbances during hospitalization, and severe morbidity, pain, and impaired functional status were significantly associated with insomnia.3
Contributing Factors
Multiple factors can lead to insomnia in hospitalized patients, including sleep disorders, psychological and physical factors, certain medical conditions, medications, environment, clinical activities, and poor sleep hygiene. Sleep disorders include obstructive sleep apnea (OSA), restless legs syndrome (RLS), and periodic limb movement disorder (PLMD).4
OSA, which occurs in 24% of men and 9% of women in the United States, is characterized by repetitive episodes of breathing pauses (apnea) and hypoventilation (hypopnea) that precipitate brief awakenings.4,5 This sleep fragmentation and oxygen desaturation causes snoring or gasping during sleep and can lead to hypertension, cardiac arrhythmias, cognitive decline, and increased mortality.4
RLS is characterized by an urge to move the legs while at rest, especially at night. Usually associated with leg discomfort, RLS is relieved with movement; prolonged bed rest during hospitalization can worsen it.6 The estimated prevalence of RLS is 5% to 15%.6 PLMD, which is characterized by repetitive flexion and extension of the lower leg during sleep, occurs in about 80% of RLS patients.5 These sleep disorders can lead to nighttime awakenings, sleep-onset difficulty, and daytime sleepiness.4
Psychological factors associated with insomnia include anxiety, depression, and grief. Physical factors that can cause sleep problems include pain; stress; difficulty breathing (e.g., from chronic obstructive pulmonary disease (COPD), pulmonary embolus, heart failure); cough; frequent urination; and withdrawal from illicit drug or alcohol use.5
Other medical conditions associated with insomnia are fibromyalgia, dementia, epilepsy, traumatic brain injury, Parkinson's disease, and stroke.5 Medications associated with insomnia include anticholinergics, antiepileptics, bupropion, beta agonists, caffeine, corticosteroids, methylphenidate, nicotine, selective serotonin reuptake inhibitors, and theophylline.4,5,7
Many studies have found the hospital environment to be a contributing factor to insomnia. Noise--from staff conversations, alarms, pagers, intercoms, doors, medical equipment, or televisions--is a major contributor.4 One study found the noise level in hospitals to be 50 to 70 decibels during the day and an average of 67 decibels at night. The Environmental Protection Agency recommends a maximum of 45 decibels during the day and 35 decibels at night.8
A lack of diurnal light cycles also can contribute to insomnia, as can clinical activities performed at night. These activities include checking vital signs, bathing, drawing blood, changing dressings, and making room changes.4,9 A study of 50 hospitalized critical care patients revealed a mean of 43 interactions per patient per night, with 62% of routine baths performed between 11 pm and 6 am.10 Poor sleep hygiene, another factor, includes frequent or lengthy naps during the day.4
Treatment
If a hospitalized patient complains of insomnia, the physician should obtain a thorough sleep history. The patient should be questioned about sleep patterns, sleep environment, and sleep hygiene at home to determine whether the insomnia is a new problem or a continuation or exacerbation of an existing problem. Assessments such as patient questionnaires, direct observation, and formal sleep studies (i.e., polysomnography) also may be done.4,5
If a patient's insomnia is thought to be due to OSA, he or she should be referred to a sleep specialist.4 RLS may be a sign of iron deficiency anemia, so patients exhibiting RLS symptoms should have a ferritin level drawn; if the level is low (<50 mcg/mL), an iron supplement, such as ferrous sulfate 325 mg (65 mg elemental) by mouth 1 to 3 times daily, should be given.6 If RLS symptoms occur intermittently, one-half to 1 tablet of carbidopa/levodopa (Sinemet) 25 mg/100 mg may be given at bedtime as needed.6 If the symptoms occur every night, a dopamine agonist such as pramipexole (Mirapex) 0.125 mg to 2 mg taken at bedtime or ropinirole (Requip) 0.25 mg to 4 mg taken 2 hours before bedtime should be prescribed. PLMD is treated similarly to RLS.6,11
Insomnia caused by depression may be relieved with antidepressants. However, the onset of the drug's effect can take up to 2 to 4 weeks, so behavioral counseling, good sleep hygiene, and possibly a hypnotic should be employed until the antidepressant takes effect.9
If insomnia is caused by a medical problem, treatment of the underlying condition should improve the patient's sleep. Any specific symptom that is preventing sleep should be addressed. Cough may be treated with a cough suppressant. Nocturnal urination may be treated by minimizing diuretic use, especially close to bedtime.9 Elevating the head of the bed 30 degrees or more can improve sleep in disorders such as heart failure, COPD, gastroesophageal reflux disease, and stroke.5 Atypical antipsychotics may be used to treat insomnia in patients experiencing acute psychotic or manic episodes.12
Environmental factors such as noise may be minimized by having nurses respond to alarms quickly; close patient doors; enforce visiting-hour restrictions; post “quiet” signs; offer eye masks or ear plugs; and keep drapes closed at night and open during the day. When possible, health care professionals should perform clinical activities during the day and minimize assessments at night. Patients should be discouraged from taking frequent or lengthy daytime naps.7
Other nonpharmacologic therapies for insomnia in the hospital include white noise or music, back massage, and warm drinks. A prospective cohort study of 111 patients in a general medical ward examined the effect of a nonpharmacologic sleep protocol (back rubs, warm drinks, and relaxation tapes) on sleep quality (rated good fair, or poor). Good sleep was reported in 51% of patient-days when all three parts of the protocol were used and in 24% when only one or two parts were used. Poor sleep was reported in 45% of patient-days when the protocol was not used. Sedative-hypnotic use was reduced from 54% prestudy to 31% at the end of the study.13
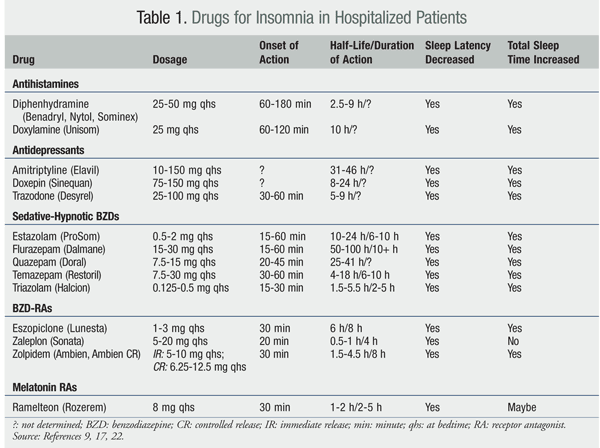
Pharmacologic therapy should be considered if treatment of the underlying problem does not resolve the insomnia or if a hospitalized patient has failed or refused nonpharmacologic therapy. Data on the use of pharmacologic therapy for the treatment of insomnia in hospitalized patients are limited; most information is extrapolated from outpatient data. Drug choices for insomnia in hospitalized patients include benzodiazepines (BZDs), BZD receptor agonists (BZD-RAs), melatonin RAs, antidepressants, and antihistamines (TABLE 1). BZDs, BZD-RAs, and antidepressants have been shown to be efficacious in outpatient studies.14 The choice for inpatient use depends on patient factors, drug factors, and formulary issues.12
A prospective single-center study examined 100 hospitalized patients' preference for pharmacologic versus nonpharmacologic therapy for insomnia. Forty patients developed insomnia while in the hospital; the other 60 had insomnia prior to admission. While hospitalized, all patients were given BZDs to treat their insomnia. Significantly, 79% of patients felt that sleeping pills improved their insomnia; 56% were not aware of BZD side effects; 78% said that they were not instructed about side effects of sleeping pills; 89% said that they were not offered nonpharmacologic treatment for insomnia; 82% believed that nonpharmacologic treatment of insomnia is healthier; and 67% would have accepted nonpharmacologic treatment for insomnia in the hospital if it had been offered.15
A prospective single-center study of 100 patients found that 60% were given a hypnotic while in the hospital. Only 29% of patients used a hypnotic at home (of these, 63% were prescribed a BZD and 14% were prescribed an antidepressant). Thirty-one percent of inpatients who were prescribed a hypnotic continued their home medication. The remaining patients were prescribed a BZD (69%), BZD-RA (29%), or both (2%).16
BZDs are the most common hypnotic class prescribed in the hospital setting. Five BZDs are approved for insomnia (TABLE 1). Side effects include residual daytime sedation, anterograde amnesia, and respiratory depression. BZDs should not be used in patients with COPD, OSA, or a history of drug abuse. BZDs with a long half-life (i.e., flurazepam, quazepam) should be avoided because they have the highest risk of causing residual daytime sedation. Agents with a short half-life (i.e., triazolam) should not be used long-term because they have the highest association with withdrawal, dependence, and tolerance. Agents with a quick-to-moderate onset of action and a moderate duration of action (i.e., estazolam, temazepam) are the most appropriate BZDs in the hospital setting. All agents are available generically, except Restoril (7.5 mg and 22.5 mg) and Doral.17
The pharmacokinetics of lorazepam are similar to those of temazepam. Lorazepam is sometimes used for sleep in the hospital, but it is not approved as a hypnotic.9,16
BZD-RAs are the second most commonly prescribed hypnotic class in the hospital setting (TABLE 1). Their advantages over BZDs include fewer withdrawal symptoms and less tolerance and dependence. BZD-RAs have a quicker onset of action, and their duration of action is similar to that of temazepam.9 Zaleplon has a short duration of action, so it should be used only to decrease sleep latency. Zolpidem is pregnancy category B, and the American Academy of Pediatrics classifies it as compatible with breastfeeding; therefore, it is the drug of choice for pregnant or breastfeeding patients.18 Side effects are mild and include headache and dizziness. Eszopiclone has been associated with a bitter taste in up to 25% of patients.17 BZD-RAs should be used with caution in COPD or OSA patients and avoided in patients with a history of drug abuse.9 Immediate-release zolpidem is the only BZD-RA available generically.17
Antihistamines, including diphenhydramine and doxylamine, have been used to treat insomnia (TABLE 1), but these agents should not be administered long-term because tolerance can develop in less than a week.12 Diphenhydramine is listed in the 2002 Criteria for Potentially Inappropriate Medication Use in Older Adults, which cites the risk of confusion and sedation and states that the drug should not be used as a hypnotic.19 A large prospective cohort study of elderly hospitalized patients found a 70% increased risk of cognitive decline in patients receiving diphenhydramine versus 24% in those not receiving it. The treatment group also experienced more behavioral disturbances and urinary catheter placement, which could be signs of anticholinergic effects of delirium, agitation, and urinary retention.20 Because of its anticholinergic effects, diphenhydramine should not be used as a hypnotic in hospitalized patients.12
Antidepressants, including trazodone, mirtazapine, and tricyclic antidepressants (TCAs), also have been used for insomnia (TABLE 1). TCAs are sedating, but they are not recommended, especially in the elderly, because of their anticholinergic and adverse cardiovascular effects. Mirtazapine is sedating at low doses (7.5-15 mg); it also stimulates appetite, so it may be useful for cancer or AIDS patients who have insomnia, depression, and anorexia.12 Trazodone can cause gastrointestinal side effects and orthostatic hypotension, but it may be an option in patients with depression or a history of substance abuse.9 All antidepressants used for insomnia are available generically.17
Ramelteon is the only melatonin receptor agonist available (TABLE 1). Side effects, which are mild, include headache and dizziness. It is not available generically. Ramelteon may be useful as a hypnotic in patients with a history of drug abuse.21
Other agents used for insomnia include barbiturates, chloral hydrate, and herbals, but their routine use in the hospital should be discouraged because their benefits rarely outweigh their risks.12
Pharmacist's Role
For hospitalized patients, pharmacists can recommend appropriate hypnotics and dosages based on patients' renal and hepatic function and age. They can also recommend that hypnotic orders be written at bedtime as needed or scheduled nightly while allowing for patient refusal of the medication.
For patients who need a hypnotic after discharge, pharmacists should recommend that a short-term prescription (2-4 weeks) of the lowest effective dose be given.22 Patients should be advised to avoid alcohol with hypnotics. If alcohol is consumed, the hypnotic dose should be skipped.23 Patients should be told to take the hypnotic approximately 15 to 30 minutes before bedtime. If the hypnotic is taken too early, there is an increased risk of confusion and falls.22
Pharmacists should also discuss nonpharmacologic treatments--especially good sleep hygiene--with discharge patients. Counseling points should include refraining from food, exercise, smoking, or alcohol before bedtime, as well as the avoidance of excessive daytime naps.9
Conclusion
Hospitalization can contribute to insomnia in many patients. Treating the underlying cause of the insomnia is the best therapy. If the patient's insomnia persists, nonpharmacologic treatment should be used, when possible, to minimize drug interactions and side effects. Pharmacologic treatment includes medium duration-of-action BZDs, BZD-RAs, and trazodone. The choice of drug depends on comorbid conditions, drug pharmacokinetics, and hospital formulary. Hospital pharmacists should expand their role to include providing recommendations to physicians and counseling to patients regarding pharmacologic and nonpharmacologic treatments for insomnia to help optimize patient care and reduce costs.
REFERENCES
1. Meissner HH, Riemer A, Santiago SM, et al. Failure of physician documentation of sleep complaints in hospitalized patients. West J Med. 1998;169:146-149.
2. Bloom HG, Ahmed I, Alessi CA, et al. Evidence-based recommendations for the assessment and management of sleep disorders in older persons. J Am Geriatr Soc. 2009;57:761-789.
3. Isaia G, Corsinovi L, Bo M, et al. Insomnia among hospitalized elderly patients: prevalence, clinical characteristics and risk factors. Arch Gerontol Geriatr. 2010;Mar 23 [Epub ahead of print].
4. Nagel CL, Markie MB, Richards KC, Taylor JL. Sleep promotion in hospitalized elders. Medsurg Nurs.
5. Young JS, Bourgeois JA, Hilty DM, Hardin KA. Sleep in hospitalized medical patients, part 1: factors affecting sleep. J Hosp Med. 2008;3:473-482.
6. Silber MH, Ehrenberg BL, Allen RP, et al. An algorithm for the management of restless legs syndrome. Mayo Clin Proc. 2004;79:916-922.
7. Flaherty JH. Insomnia among hospitalized older persons. Clin Geriatr Med. 2008;24:51-67.
8. Tullmann DF, Dracup K. Creating a healing environment for elders. AACN Clin Issues. 2000;11:34-50.
9. Lenhart SE, Buysse DJ. Treatment of insomnia in hospitalized patients. Ann Pharmacother.
10. Tamburri LM, DiBrienza R, Zozula R, Redeker NS. Nocturnal care interactions with patients in critical care units. Am J Crit Care. 2004;13:102-112.
11. Natarajan R. Review of periodic limb movement and restless leg syndrome. J Postgrad Med. 2010;56:157-162.
12. Young JS, Bourgeois JA, Hilty DM, et al. Sleep in hospitalized medical patients, part 2: behavioral and pharmacological management of sleep disturbances. J Hosp Med. 2009;4:50-59.
13. McDowell JA, Mion LC, Lydon TJ, Inouye SK. A nonpharmacologic sleep protocol for hospitalized older patients. J Am Geriatr Soc. 1998;46:700-705.
14. Buscemi N, Vandermeer B, Friesen C, et al. The efficacy and safety of drug treatments for chronic insomnia in adults: a meta-analysis of RTCs. J Gen Intern Med. 2007;22:1335-1350.
15. Azad N, Byszewski A, Sarazin FF, et al. Hospitalized patients' preference in the treatment of insomnia: pharmacological versus non-pharmacological. Can J Clin Pharmacol. 2003;10:89-92.
16. Frighetto L, Marra C, Bandali S, et al. An assessment of quality of sleep and the use of drugs with sedating properties in hospitalized adult patients. Health Qual Life Outcomes. 2004;2:17-26.
17. Williams AL, ed. Drug Facts and Comparisons. St. Louis, MO: Wolters Kluwer Health; 2010.
18. Briggs GG, Freeman RK, Yaffe SJ, eds. Drugs in Pregnancy and Lactation. 8th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
19. Fick DM, Cooper JW, Wade WE, et al. Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a US consensus panel of experts. Arch Intern Med.
20. Agostini JV, Leo-Summers LS, Inouye SK. Cognitive and other adverse effects of diphenhydramine use in hospitalized older patients. Arch Intern Med. 2001;161:2091-2097.
21. Ramakrishnan K, Scheid DC. Treatment options for insomnia. Am Fam Physician. 2007;76:517-526.
22. Passarella S, Duong MT. Diagnosis and treatment of insomnia. Am J Health Syst Pharm.
23. Ahmed QA. Effects of common medications used for sleep disorders. Crit Care Clin.
2008;24:493-515.
To comment on this article, contact rdavidson@uspharmacist.com.





