US Pharm. 2011;36(2):44-50.
The American College of Lifestyle Medicine defines lifestyle medicine as “the use of lifestyle interventions in the treatment and management of disease. Such interventions include diet (nutrition), exercise, stress management, smoking cessation, and a variety of other non-drug modalities.”1 Lifestyle-medicine strategies have been shown to be effective in the prevention and treatment of most chronic conditions.2
Medication therapy management (MTM) services have become a hallmark of pharmacy practice for patients with chronic conditions such as hypertension.3 Incorporating lifestyle medicine with MTM services may further improve blood pressure (BP) control and reduce the incidence of cardiovascular morbidity and mortality.4 The purposes of this paper are to present lifestyle-medicine strategies that are effective for lowering BP and to recommend intervention strategies for pharmacists.
Hypertension Treatment Guidelines
According to the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7), lifestyle modifications should be employed as first-line therapy to both prevent and manage high BP.4 The major lifestyle changes that have been shown to lower BP include weight loss, increased physical activity, and adoption of the DASH (Dietary Approaches to Stop Hypertension) eating plan. Dietary sodium restriction, smoking cessation, stress reduction, and alcohol moderation also have been shown to reduce BP.4 Practicing multiple lifestyle modifications simultaneously can have an additive effect on lowering BP. A summary of lifestyle modifications and their effects on BP appears in TABLE 1. Discussed below are details supporting the implementation of each of these lifestyle modifications in patients with hypertension.

Physical Activity: Physical activity is one of the cornerstones of both the prevention and the treatment of high BP. The U.S. Department of Health and Human Services currently recommends that adults perform a total of at least 150 minutes of moderate-intensity activity each week, 75 minutes of vigorous-intensity aerobic activity per week, or an equivalent combination of moderate- and vigorous-intensity aerobic activity.5 In addition, moderate- to high-intensity resistance-training activities that involve all the major muscle groups should be performed at least 2 days per week. TABLE 2 gives specific recommendations for physical activity in hypertensive patients.

Research has shown that aerobic exercise can significantly reduce BP in patients with hypertension.6,7 Two review articles summarized 121 studies examining the effects of endurance exercise training on BP in nearly 2,200 subjects with systolic BP (SBP) and diastolic BP (DBP) exceeding 140/90 mmHg. SBP and DBP reductions were an average of approximately 11 mmHg and 8 mmHg, respectively, and were consistent across nearly all of the studies.6
Nutrition: Nutrition is a fundamental component of the prevention and treatment of hypertension. Landmark studies published in the late 1990s and early 2000s laid the foundation for current nutrition recommendations for patients with high BP. The dietary recommendations from this research have come to be known collectively as the DASH eating plan. The DASH plan recommends the consumption of fruits and vegetables, whole grains, and low-fat dairy products and the avoidance of foods that contain saturated fat, cholesterol, and large amounts of sodium. This type of eating pattern results in a greater consumption of fiber, potassium, magnesium, and calcium, which are effective nutrients for helping lower BP.4
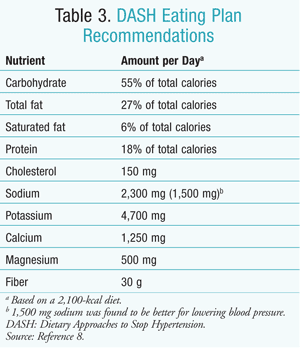
Collective results from research on the DASH eating plan show that individuals who consume four to five servings of fruits and vegetables and seven to eight servings of whole-grain foods daily; limit saturated fats to <6% of total calories; limit cholesterol intake to 150 mg per day; and limit sodium intake to <1,500 mg per day may experience significant BP reductions, compared with individuals whose eating habits are consistent with the typical American diet.4,8 Specifically, individuals with hypertension ( >140/90 mmHg) have been shown to reduce SBP and DBP measurements by 11.4 mmHg and 5.5 mmHg, respectively.4,8 Even individuals who do not have hypertension can decrease their SBP and DBP by 5.5 and 3.0 mmHg, respectively.4,8 Dietary recommendations from the DASH eating plan are summarized in TABLE 3.
Weight Loss: Increased body weight has been shown to have a significant effect on raising BP.9 Therefore, weight loss in overweight and obese individuals is an important and effective strategy for the prevention and management of high BP. According to research, a 22-lb reduction in body weight can result in an SBP reduction of between 5 mmHg and 20 mmHg.4 The most recent guidelines on obesity state that overweight and obese individuals should aim for a 10% weight loss within a 6-month time period.9 Weight loss is most effective if it occurs at a rate of approximately 0.5 to 2 pounds per week.9 In addition, it is recommended that weight loss occur through adoption of these concurrent lifestyle behaviors: decreased food consumption, increased physical activity, and behavior-change strategies.9
Alcohol Moderation: It is recommended that adults consume alcohol in moderate amounts (one drink per day for women; two drinks per day for men) or less each day. One drink is defined as 12 oz. of regular beer, 5 oz. of wine, or 1.5 oz. of 80-proof distilled spirits. Moderation refers to the amount consumed per day, not the average consumption over several days. A hypertensive patient who regularly consumes large amounts of alcohol can reduce his or her BP by 2 mmHg to 4 mmHg through restricting alcohol intake to a moderate level.4
Stress Reduction: Recent reviews have provided evidence that psychosocial stress contributes to hypertension, coronary artery disease, and cardiovascular mortality.10,11 A meta-analysis comparing the effects of stress-reduction techniques showed that Transcendental Meditation (TM) was the most effective method for lowering BP. TM can reduce SBP and DBP measurements in hypertensive patients by 5.0 mmHg and 2.8 mmHg, respectively.10
Smoking Cessation: Tobacco use is one of the most significant risk factors for cardiovascular disease, cancer, and many other health conditions. Among other physiologic changes, smoking causes an increase in peripheral vascular resistance, leading to hypertension.12 A study measuring the effects of smoking cessation on BP and heart rate found significant changes even after 1 week.13 Subjects with normal BP experienced SBP and DBP reductions of 3.5 mmHg and 1.9 mmHg, respectively, 1 week after quitting. In addition, resting heart rate decreased by more than 7 beats per minute after the first week.13 All health care professionals, including pharmacists, are strongly encouraged to assist patients who smoke in their cessation efforts (see RESOURCES SIDEBAR).12

Behavior Change
Behavior change is a critical step in the maintenance of long-term lifestyle behaviors. Adherence to lifestyle modifications may often be challenging for patients. Because of this, it is important to proactively implement behavior-change strategies to promote adherence. TABLE 4 lists some patient-related and program-related strategies for improving patient adherence to lifestyle-modification programs.

Combination of Lifestyle Modifications
The JNC 7 guidelines recommend that patients with hypertension adopt multiple lifestyle-modification strategies, because the BP-reducing effects of these strategies are additive. The ENCORE study found that the addition of weight loss and exercise to the DASH eating plan resulted in significantly better BP control compared with the DASH eating plan alone (P <.001).14 The PREMIER trial showed that multiple lifestyle-medicine strategies (weight loss, exercise, reduced sodium intake, limited alcohol intake, DASH eating plan) can be successfully implemented in patients with high BP and can significantly decrease the prevalence of hypertension, compared with results in patients who do not adopt multiple lifestyle behaviors (P <.001).15
Conclusion
Implementing lifestyle medicine with existing MTM services can be a natural fit for the pharmacist. Pharmacists are ideally positioned within the community to be an accessible resource for people who would like to adopt lifestyle changes to better manage their health care needs. Integrating lifestyle medicine with MTM offers patients a more comprehensive approach to the management of their chronic conditions, such as hypertension. Pharmacists can design and implement general lifestyle-medicine programs, as well as programs that target specific conditions, such as cardiovascular disease, obesity, and diabetes.
Lifestyle medicine is beneficial for patients because it enables them be involved in their own health and wellness at a higher level. Lifestyle medicine is advantageous for pharmacists because it provides a greater number of opportunities to make contact with patients. This not only increases the likelihood that a patient’s chronic conditions are being managed appropriately, but allows more frequent monitoring of medication adherence. Implementing lifestyle medicine with MTM can be professionally rewarding by enabling pharmacists to more comprehensively care for patients with chronic conditions.
REFERENCES
1. American College of Lifestyle Medicine. What is lifestyle medicine? www.lifestylemedicine.org/
2. American College of Preventive Medicine. Lifestyle medicine—evidence review. June 30, 2009. www.acpm.org/
3. American Pharmacists Association (APhA). Medication therapy management. www.pharmacist.com/AM/
4. National Institutes of Health (NIH). The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. NIH Pub. No. 04-5230. August 2004.
5. U.S. Department of Health and Human Services (DHHS). 2008 Physical Activity Guidelines for Americans. ODPHP Pub. No. U0036. October 2008.
6. Hagberg JM, Park JJ, Brown MD. The role of exercise training in the treatment of hypertension: an update. Sports Med. 2000;30:193-206.
7. Hagberg JM, Brown MD. Does exercise training play a role in the treatment of essential hypertension? J Cardiovasc Risk. 1995;2:296-302.
8. Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med. 2001;344:3-10.
9. National Institutes of Health. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. NIH Pub. No. 98-4083. September 1998.
10. Rainforth MV, Schneider RH, Nidich SI, et al. Stress reduction programs in patients with elevated blood pressure: a systematic review and meta-analysis. Curr Hypertens Rep. 2007;9:520-528.
11. Rozanski A, Blumenthal JA, Davidson KW, et al. The epidemiology, pathophysiology, and management of psychosocial risk factors in cardiac practice: the emerging field of behavioral cardiology. J Am Coll Cardiol. 2005;45:647-651.
12. The Health Consequences of Smoking: A Report of the Surgeon General. Atlanta, GA: DHHS, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office of Office of Smoking and Health; May 2004.
13. Minami J, Ishimitsu T, Matsuoka H. Effects of smoking cessation on blood pressure and heart rate variability in habitual smokers. Hypertension. 1999;33:586-590.
14. Blumenthal JA, Babyak MA, Hinderliter A, et al. Effects of the DASH diet alone and in combination with exercise and weight loss on blood pressure and cardiovascular biomarkers in men and women with high blood pressure: the ENCORE study. Arch Intern Med. 2010;170:126-135.
15. Appel LJ, Champagne CM, Harsha DW, et al. Effects of comprehensive lifestyle modification on blood pressure control: main results of the PREMIER clinical trial. JAMA. 2003;289:2083-2093.
16. Stewart SH, Latham PK, Miller PM, et al. Blood pressure reduction during treatment for alcohol dependence: results from the Combining Medications and Behavioral Interventions for Alcoholism (COMBINE) study. Addiction. 2008;103:1622-1628.
17. Whitley JA, Lewis B, Napolitano MA, Marcus BH. Health counseling skills. In: Kaminsky LA, Bonzheim KA, Ewing Garber C, et al, eds. ACSM’s Resource Manual for Guidelines for Exercise Testing and Prescription. 5th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2006:588-597.
18. Dunn AL, Chambliss HO. Psychopathology. In: Kaminsky LA, Bonzheim KA, Ewing Garber C, et al, eds. ACSM’s Resource Manual for Guidelines for Exercise Testing and Prescription. 5th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2006:581-587.
19. Enhancing patient adherence: proceedings of the pinnacle roundtable discussion. APhA Highlights Newsletter. 2004;7:1-12.
To comment on this article, contact rdavidson@uspharmacist.com.






