US Pharm. 2009;34(8):58-69.
Some 7.3 million Americans or 15% of couples in the United States experience infertility.1 While society generally blames infertility on women, statistics show that infertility is a shared problem with male issues contributing to at least 50% of cases.1-3 More specifically, approximately 20% of cases of infertility are due entirely to male factors, with an additional 30% to 40% of cases involving both male and female factors.2
Recent data suggest that infertility affects one in 25 American men.2,4 A wide variety of factors—including lifestyle, concurrent disease states, environmental exposures, and medications—have been linked to male infertility. Determining the etiology of male infertility is extremely important, since many of the causes can be successfully treated with surgery and/or medical therapies.2,4 This article examines the causes and treatments of male infertility and discusses the role of the pharmacist in providing pharmaceutical care to male patients suffering from infertility.
Defining Infertility
Infertility is defined as the inability to achieve conception despite one year of frequent unprotected intercourse.5,6 Use of this time period, while arbitrary, was based upon a study of over 5,500 English and American women engaged in unprotected intercourse who ultimately conceived between 1946 and 1956.3 Among the women in the study, 50% conceived within 3 months, 72% within 6 months, and 85% within 12 months.7 A one-year prevalence of infertility of 15% among couples in North America and Europe has been confirmed by other studies. Not surprisingly, the rates of infertility are higher in less developed countries.3 Of infertile couples without treatment, 25% to 35% will conceive at some time by intercourse alone. Within the first 2 years, 23% will conceive, whereas an additional 10% will do so within 2 more years.2 Generally speaking, if a pregnancy does not occur by 3 years, persistent infertility is very likely in the absence of medical intervention.3
Diagnosing Male Infertility
The basic workup for the suspected infertile man includes an interview, physical examination, and laboratory work.8 First, the patient’s past medical history, sexual history, and social history are ascertained. Pertinent past medical history includes the incidence of mumps after puberty, hernia repairs, athletic injuries to the groin, and a history of undescended testicles. Pertinent sexual history includes sexually transmitted diseases, urinary tract infections, prostatitis, and impotence or ejaculatory problems. Pertinent social history includes excessive smoking, drinking, and illicit drug use. During the physical examination, the hair growth pattern in the genital area, the penis, testes, prostate gland, and breasts are examined.2 Finally, laboratory assessments are performed. This includes a semen analysis that examines sperm count, ability of sperm to swim (motility), velocity or forward progression of the sperm, size and shape of the sperm (morphology), total semen volume, and the liquefaction of the semen (the ability to go from a normal gel-like state at ejaculation to a liquid state).8,9 (The sidebar above further discusses semen analysis.) Endocrine evaluation of the suspected infertile man is also important and includes measurements of serum testosterone, luteinizing hormone (LH), follicle-stimulating hormone (FSH), and prolactin.2,8

Lifestyle Choices
In many instances, lifestyle factors are solely responsible for low sperm counts. Emotional stress may interfere with gonadotropin-releasing hormone (GnRH) and reduce sperm counts. Testicular overheating (from high fevers, saunas, and hot tubs) may temporarily lower sperm counts and impair fertility. Cocaine and/or heavy marijuana use may reduce the number and quality of sperm by as much as 50%. Smoking impairs sperm mobility, reduces sperm lifespan, and may cause genetic changes that affect the offspring.5 Lubricants used with condoms (i.e., spermicides, oils, Vaseline) kill sperm and lower viable sperm counts. Sexual issues (e.g., impotence, premature ejaculation, relationship problems) have also been associated with low sperm counts.6 Fortunately, such causes of low sperm counts are usually treatable and reversible when the lifestyle choice is modified.2
Causes of Male Infertility
There are four primary causes of male infertility: primary hypogonadism, secondary hypogonadism, posttesticular defects, and unknown etiology. It is important to note that a proper diagnosis cannot be made without a physical examination and semen analysis.3
Hypogonadism refers to low levels of circulating testosterone and is one of the primary causes of infertility in males. In fact, most androgen-deficient men are infertile.9 There are two types of male hypogonadism: primary and secondary hypogonadism.10,11
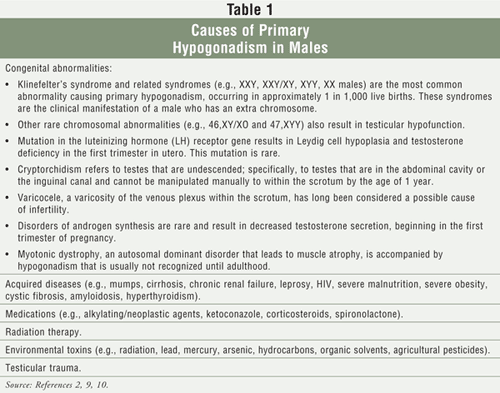
Primary hypogonadotropic hypogonadism, which accounts for 30% to 40% of cases of male infertility, indicates that the abnormality originates in the testes. Primary hypogonadotropic hypogonadism is more likely to be associated with a decrease in sperm production than in testosterone production. As a consequence, the sperm count is typically low; whereas serum LH and FSH concentrations are normal or high.10 Gynecomastia (excessive development of the breasts) commonly occurs with primary hypogonadism because serum FSH and LH levels are increased.10,11 Some of the more common causes of primary hypogonadotropic hypogonadism are listed in TABLE 1.
Secondary hypogonadotropic hypogonadism, which accounts for 1% to 2% of cases of male infertility, indicates a defect in the hypothalamus or pituitary gland, resulting in decreased gonadotropins (LH, FSH, or both) and secondary impairment of testicular function.9 It is important to note that any hypothalamic or pituitary disease can cause GnRH or gonadotropin deficiency and therefore infertility. Secondary hypo gonadotropic hypogonadism is rarely associated with gynecomastia because serum FSH and LH levels are not high and therefore do not stimulate testicular aromatase.11 The causes of secondary hypogonadism are listed in TABLE 2.

Posttesticular defects (or disorders of sperm transport) account for 10% to 20% of cases of male infertility. The epididymis is an important site for sperm maturation and an essential part of the sperm transport system. The vas deferens transports sperm from the epididymis to the urethra, where they are diluted by secretions from the seminal vesicles and prostate. The sperm are then ejaculated. Abnormalities at any of these sites can cause infertility.3 Major causes of posttesticular defects are discussed in TABLE 3.
Idiopathic (unexplained) causes account for 40% to 50% of cases of male infertility. In these instances, despite careful assessments of all possible causes, reasons for abnormal sperm number and/or morphology cannot be identified.3

Medical (Pharmacologic) Management of Male Infertility
The pharmacologic management of male infertility involves proven and unproven therapies. Generally speaking, the exact cause of the infertility must be identified prior to initiating therapy with a specific pharmacologic agent. When a cause cannot be identified, numerous empiric therapies are available.
Proven Therapies
Gonadotropins: Gonadotropins are the first-line treatment for hypogonadotropic hypogonadism. Normal male fertility requires adequate levels of intratesticular testosterone and FSH in order to initiate and maintain spermatogenesis. FSH administration to men who have hypogonadotropic hypogonadism has demonstrated increases in sperm count, motility, morphology, and testicular volume. Typically, the initial management consists of human chorionic gonadotropin (HCG), 3,000 to 6,000 IU per week, until adequate serum testosterone levels are detected.4
Antibiotics: The incidence of genital tract infections among men who have infertility varies between 10% and 20%.4 Interestingly enough, infertile men rarely present with symptoms or signs of acute genital infections or prostatitis, but these are usually diagnosed by the presence of increased leukocytes in the semen. Despite the absence of symptoms, patients with leukospermia (elevated leukocytes in the semen) are generally treated with at least a 10-day course of extended spectrum antibiotics, such as erythromycin, trimethoprim-sulfamethoxazole, or a quinolone. A second course of therapy is usually given if leukocytes persist in the semen after the initial antibiotics.6
Corticosteroids: Sperm autoimmunity is diagnosed by the presence of sperm antibodies on the sperm surface or in the seminal fluid by the immunobead test or mixed antiglobulin reaction.6 Continuous or intermittent high doses of glucocorticoids (prednisone 40-80 mg per day) for up to 6 months have been shown in placebo-controlled trials to improve cumulative pregnancy significantly in partners of men with sperm autoantibodies.6,12 Many patients cannot tolerate this regimen because of the adverse effects of high-dose glucocorticoids (e.g., hyperglycemia, weight gain, osteoporosis, acne).6
Alpha-sympathomimetics and Anticholinergics:
Ejaculatory dysfunction may take the form of failure of emission or retrograde ejaculation. The cause may be psychogenic or idiopathic. Medical therapy for ejaculatory dysfunction is initiated with an alpha-sympathomimetic medication such as ephedrine, pseudo ephedrine, or imipramine.4
Unproven Therapies
Clomiphene Citrate: This synthetic antiestrogen is the most commonly used drug in the treatment of idiopathic oligospermia (deficiency of sperm in the semen). The drug works by increasing GnRH, LH, and FSH secretion and stimulating the production of testosterone and spermatogenesis.2 Although clomiphene citrate is widely used, its efficacy has not been clinically proven.4
Aromatase Inhibitors: Aromatase inhibitors, which block the conversion of androgen to estrogen and therefore increase testosterone, are increasingly being used to treat male infertility. While preliminary results are promising, larger, controlled clinical trials are needed for this to be considered an efficacious therapy.4
Gonadotropins: In addition to treatment for hypo gonadotropic hypogonadism, gonadotropins are also commonly used in the treatment of idiopathic infertility; however, randomized controlled trials have observed no significant effects on pregnancy rates or seminal parameters.2,4 In contrast, many uncontrolled studies with positive outcomes have sparked interest in continued research on the topic.4
Surgical Management of Male Infertility
Surgical management provides many options to correct male factor infertility. Problems amenable to surgery include varicoceles and obstruction.
Varicocele Repair: Varicoceles cause a duration-dependent decline in semen parameters and testosterone production.4 Surgical ligation of varicoceles reduces intratesticular temperature to the normal range and improves semen parameters.4,6 No consistent data exist regarding the efficacy of varicocele repairs—some studies have yielded positive results, whereas others have not.13,14
Obstruction: Vasectomies are the most common obstructive cause of male infertility. Injury to the vas deferens is also a common cause of obstruction, most often the result of childhood hernia repair, orchiopexy, or hydrocelectomy. Success rates of repair obstructions are between 90% and 99%.2,4
Role of the Pharmacist
The pharmacist can play many roles in providing pharmaceutical care to men experiencing infertility. A thorough medication review identifying drugs that can affect infertility is an important first step. Next, pharmacists should encourage patients to make positive lifestyle changes (e.g., decreasing stress, stopping smoking, ceasing illicit drug activity). Pharmacists should also ensure that patients are having intercourse at the correct time of the month. Although there is some controversy, most experts advise vaginal intercourse every 2 days near the woman’s time of ovulation.2
Pharmacists should also be realistic with patients about the available treatment options for male infertility and explain to patients that there are a variety of causes of irreversible infertility for which no therapy exists. For example, there is no known therapy that will stimulate sperm production when the seminiferous tubules have been severely damaged, as with Klinefelter’s syndrome, microdeletions of the Y chromosome, Sertoli-cell–only syndrome, and idiopathic infertility associated with azoospermia (absence of sperm in semen).6
Likewise, pharmacists should encourage infertile couples to consider assisted reproductive technology (ART), including intrauterine insemination and in vitro fertilization, when medical and surgical interventions fail or are not applicable.2,5 Explain to patients that ART is commonly used for the successful treatment of the female partners of males with moderate or severe oligospermia and azoospermia.6
Conclusion
Infertility is a couple’s problem, and both partners must be properly evaluated so that the most appropriate therapy can be tailored to the man and to the woman.6 In the vast majority of cases, male infertility can be successfully treated with either medical or surgical interventions.4
REFERENCES
1. Infertility 101: Get the facts. RESOLVE: The National Infertility Association. https://secure2.convio.net/
2. Sigman M, Jarow J. Male infertility. In: Wein AJ, Kavoussi LR, Novick AC, et al, eds. Campbell-Walsh Urology. 9th ed. Philadelphia, PA: Saunders; 2007.
3. Swerdloff R, Wang C. Causes of male infertility. In: Snyder P, Matsumoto A, eds. UpToDate. Waltham, MA: UpToDate; 2008 [subscription required].
4. Schiff J, Ramirez M, Bar-Chama N. Medical and surgical management male infertility. Endocrinol Metab Clin North Am. 2007;36:313-331.
5. Hornstein M, Gibbons W. Treatment of unexplained infertility. In: Barbieri R, ed. UpToDate. Waltham, MA: UpToDate; 2008 [subscription required].
6. Wang C, Swerdloff R. Treatment of male infertility. In: Snyder P, Matsumoto A, eds. UpToDate.
Waltham, MA: UpToDate; 2008 [subscription required].
7. Guttmacher AF. Factors affecting normal expectancy of conception. JAMA. 1956;161:855-860.
8. Swerdloff R, Wang C. Evaluation of male infertility. In: Snyder P, Matsumoto A, eds. UpToDate.
Waltham, MA: UpToDate; 2008 [subscription required].
9. Swerdloff R, Wang C. The testis and male sexual function. In: Goldman L, Ausiello D, eds. Cecil Textbook of Medicine. 22nd ed. Philadelphia, PA: Saunders; 2007.
10. Snyder P. Causes of primary hypogonadism in males. In: Matsumoto A, ed. UpToDate. Waltham, MA: UpToDate; 2008 [subscription required].
11. Snyder P. Causes of secondary hypogonadism in males. In: Matsumoto A, Kirkland J, eds. UpToDate. Waltham, MA: UpToDate; 2008 [subscription required].
12. Hendry WF, Hughes L, Scammell G, et al. Comparison of prednisolone and placebo in subfertile men with antibodies to spermatozoa. Lancet. 1990;335:85-88.
13. Evers JL, Collins JA. Assessment of efficacy of varicocele repair for male subfertility: a systematic review. Lancet. 2003;361:1849-1852.
14. Evers JL, Collins J, Clarke J. Surgery or embolisation for varicocele in subfertile men. Cochrane Database Syst Rev. 2008;(3):CD000479.
To comment on this article, contact rdavidson@jobson.com.





