US Pharm. 2010;35(12):HS2-HS10.
Diverticular disease comprises diverticulosis and diverticulitis. Diverticulosis--the presence of diverticula without inflammation--is very common, affecting approximately 50% of Americans by age 60 years, although most patients remain asymptomatic.1-3 Diverticula are pouches or sacs within the colon that occur normally or via herniation of the mucous lining. However, roughly 5% to 20% of patients with diverticulosis will develop inflammation and subsequent sequelae.3,4 Once there is inflammation, the condition is called diverticulitis. It is thought that a micro- or macroperforation is the precipitating factor in the development of diverticulitis.4 The perforation may be the result of increased intraluminal pressure or thickened fecal matter in the neck of the diverticulum.4
In the Western world, the left colon (descending and sigmoid) is the area most often affected, with approximately 95% of the cases of acquired diverticular disease involving the sigmoid colon (which is closest to the rectum).3,5,6 In Asian countries, the right colon (cecum and ascending) is most often affected.2 This suggests a genetic, lifestyle, or environmental component for developing right-sided diverticular disease.5 With most right-sided diverticula, there is an outpouching of all three layers of the colonic wall (mucosa, submucosa, and muscle layer).3 This constitutes a “true” diverticulum.3,7 However, most left-sided diverticula involve only the mucosa and the submucosa. When a diverticulum affects only the mucosa and the submucosa, it is called a pseudodiverticulum.3,7 Patients with right-sided diverticular disease are often 20% younger than left-sided patients when they first present with the disease. Their pain is in the right lower quadrant, and it is often difficult to distinguish from appendicitis.2
Risk Factors
There is still not much known about diverticular disease, but some risk factors have been identified. Aging is the primary risk factor.5 Patients 60 years of age and older are more likely to develop diverticulosis.7 Low dietary fiber intake is the other most significant risk factor.7 Because lack of fiber in the stool decreases transit time, the pressure in the colon increases and results in a “blowing out” of the weak areas of the colon.7 With less fiber there is also a lower volume of stool, which causes greater segmentation of the bowel (the process of smooth muscle contraction), resulting in higher luminal pressures.3 Eating a diet high in fiber may actually prevent patients with asymptomatic diverticulosis from progressing to symptomatic disease.4 Physical inactivity may be a risk factor along with gender.4 Diverticular disease is more common in women than in men.5
Obesity has been gaining recognition as a possible contributing factor in diverticulitis.3,8 In a prospective cohort study done by Strate et al, 47,228 male health professionals were followed for 18 years to determine the relationship between diverticulitis and obesity, in particular central obesity.8 After adjusting for known or potential risk factors for diverticular disease (total dietary fat, fiber, and red meat; total caloric intake, physical activity, and current nonsteroidal anti-inflammatory drug [NSAID] and acetaminophen usage), they found that men with a body mass index (BMI) ³30 kg/m2 were 78% more likely to develop diverticulitis than men with a BMI <21 kg/m2 (P = .02). Although they found no association between obesity and diverticulosis, there was a positive association between weight gain and the risk of developing diverticulitis. Men who had gained more than 45 pounds since the age of 21 had a relative risk of 1.66 (P = .003). Likewise, there was a positive association between diverticulitis and waist size.8
Signs and Symptoms
Pain is a hallmark symptom of diverticular disease. The pain of diverticulosis is often relieved by passing flatus or having a bowel movement and can be precipitated by ingesting food.4 The lower left quadrant is the site of pain with left-sided disease. Likewise, lower right quadrant pain is present with right-sided disease.7 In fact, many of the patients who suffer from pain associated with diverticulitis are often misdiagnosed as having inflammatory bowel disease (IBD).3 Patients with symptomatic diverticulosis (without inflammation) often suffer from constipation rather than diarrhea.4 However, diverticulitis patients may suffer from either diarrhea or constipation.9 Other symptoms of uncomplicated diverticulitis include fever, left lower abdominal tenderness (with left-sided disease), mild-to-moderate leukocytosis, irregular bowel habits, urinary symptoms, and abdominal distention.9,10
Complicated diverticulitis is more critical and presents with additional symptoms depending on the complexity of the condition. Up to 25% of the cases of diverticulitis are complicated diverticulitis.5 The majority of patients with complicated diverticulitis have no prior history of the disease.2 Complicated diverticulitis can be associated with abscess, phlegmon, obstruction, fistulization, bleeding, sepsis, generalized peritonitis, and/or stricture.3,9
Often patients with complicated diverticulitis present with perforation first. Diverticulitis with perforation causes the most morbidity and mortality.2 The perforation can be a micro- or a macroperforation. The infection after a microperforation is usually contained by the pericolonic fat, mesentery, or adjacent organs; therefore, a localized phlegmon occurs. However, the infection after a macroperforation is not restricted and can result in peritonitis or a pericolonic abscess.4,9 Upon abdominal examination, the presence of a tender mass is suggestive of an abscess.7 If the infection spreads to the adjacent structures, a fistula may develop.4 Although they are atypical presentations of diverticulitis, the following may be present in complicated diverticulitis: chronic infections in the hip, knee, or thigh; inflammation in the perineum (the pelvic floor and associated structures) or genitalia; abscesses in the liver; subcutaneous emphysema (accumulation of air) of the legs, neck, and abdominal wall; and skin lesions.2
There can be diverticular bleeding, which may result in anemia.7 However, rectal bleeding is less likely to be diverticulitis than ischemia, ulcerative colitis, or Crohn's disease.10
The symptoms of a fistula include pneumaturia (gas or air in the urine), fecaluria (feces in the urine), vaginal discharge, and recurrent urinary tract infections (UTIs).10 Recurrent UTIs can occur with the presence of a colovesical fistula, which is a fistula between the colon and the bladder, and the most common fistula with diverticulitis.3,7 Colovesical fistulas are more common in men than in women due to the fact that the uterus is between the colon and bladder in women.4
Diagnosis
Diverticulitis can mimic many other pathologies. These include acute appendicitis, colorectal cancer, complicated ulcer disease, Crohn's disease, cystitis, ectopic pregnancy, gallbladder disease, incarcerated hernia, ischemic colitis, mesenteric infarction, pancreatic disease, pelvic inflammatory disease, pseudomembranous colitis, renal disease, small bowel obstruction, UTI, ulcerative colitis, and ovarian cyst, abscess, neoplasm, or torsion.4,6,9,10 The European Association of Endoscopic Surgeons (EAES) has devised a classification system to aid in diagnostic testing, which is outlined in TABLE 1.3

A CT scan with the use of oral, IV, or rectal contrast is a very beneficial examination method, because it is highly sensitive and specific. It is associated with a low false-positive rate.6 A CT scan can determine whether hospitalization is warranted.3,6 It can also help determine the risk of secondary complications if medication therapy on an outpatient basis is opted for instead of surgery.6 The findings on a CT scan that suggest diverticulitis include the presence of diverticula and wall thickening (>4 mm, which is called mychosis), pericolic fat infiltration, abscess formation, and extraluminal air or contrast fluid collection.3,7,9,10
Colonoscopy and barium enema are contraindicated during an acute attack of diverticulitis because of the increased risk of perforation.9 After the resolution of an acute episode, a colonoscopy or barium enema should be done at about 6 weeks to rule out carcinoma or IBD.9
Treatment
Outpatient Therapy: Nonoperative treatment is successful in 70% to 100% of patients with uncomplicated acute diverticulitis.6 Patients with mild symptoms and no peritoneal signs may be managed conservatively on an outpatient basis with a clear liquid diet and broad spectrum antibiotics.9 Antibiotics should be tailored to treat the most common bacteria found in the colon, which are gram-negative rods and anaerobic bacteria. Single-agent and multiple antibiotic agent regimens are equally effective as long as both types of bacteria (gram-negative rods and anaerobes) are susceptible.6 (The recommended treatment regimens are detailed in TABLE 2.9) Symptoms should improve within 48 to 72 hours.4,9 Patients should also be placed on a low-fiber diet during this treatment phase.10 After 3 days of treatment, the diet can be slowly advanced to normal.4

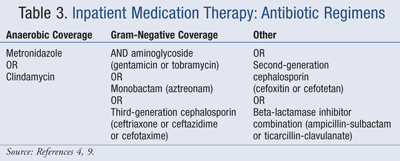
Inpatient Therapy: Patients who do not symptomatically improve or who cannot tolerate oral liquids need to be hospitalized.9 Hospitalization is also indicated if the patient has a high fever, highly elevated white blood cell levels, abscess, uncontrolled pain, limited free air, partial bowel obstruction, fistula, or severe comorbid conditions, or is elderly or immunocompromised.4,9,10 Hospitalized patients should be NPO (nothing by mouth) and on IV fluids and IV antibiotics.7,9 The antibiotics of choice for hospitalized patients are given in TABLE 3.4,9 Symptoms should improve within 48 to 72 hours, after which the patient may be switched to oral antibiotics for 7 to 10 days. The diet may then be advanced to normal, and the patient can be discharged.4,7
A follow-up colonoscopy should be done 4 to 6 weeks after discharge, and a high-fiber diet should be recommended.7 There is evidence that a high-fiber diet alleviates the symptoms of diverticular disease. Fiber intake of greater than 10 g daily (preferably 20-30 g daily) is recommended for all patients with diverticular diseases, except those suffering an acute attack of diverticulosis.11
Nasogastric suction is not indicated unless there is a significant ileus (intestinal obstruction).4,7,9 An abscess larger than 4 cm in diameter should be drained.3 CT-guided percutaneous drainage is the most appropriate way to treat patients with a large abscess.6 For pain control, morphine should not be used because of its propensity to increase intraluminal pressure.4,7 Meperidine (Demerol) is the drug of choice, because it has been shown to decrease colonic pressure.4,7 NSAIDs and steroids should be avoided, because they may cause GI bleeding and perforation.4,7 Steroids may also mask the symptoms of diverticulitis.4
To Operate or Not to Operate? That Is the Question: Much is still not known about diverticulitis, and there does not seem to be a consensus as to when surgical intervention should be done with both acute diverticulitis and recurrent diverticulitis.2,3,5 Approximately 1% of all patients with colonic diverticulitis will require surgery; however, that number increases to 15% to 30% for patients requiring hospitalization.2,4 Surgery is usually not indicated after the first episode of uncomplicated diverticulitis, because only 7% to 35% of patients will have a recurrent episode.4 When the patient is 40 years old or younger, however, surgery may be performed after the first episode, because disease in younger patients is often thought to be more aggressive and have more complications.2 Between 2% to 30% of all cases of diverticular disease in younger patients progress to diverticulitis, and these patients are most commonly obese males. In these cases, if surgery is done, it should be to alleviate symptoms rather than prevent future complications.2
With patients over 40 years, surgery is usually performed after two episodes of diverticulitis.2 With patients experiencing a second episode, there is more than a 50% probability that a third episode will occur. Medical therapy is less likely to be effective with recurrent episodes, and these episodes have a higher mortality rate.4 Colonic resection is done to prevent future complications from diverticular disease that are likely to occur without surgery; however, 2.3% of those patients die and 14.2% require a colostomy.2 Many of the deaths are because of anatomical leaks.2
Indications for immediate surgical intervention include diffuse peritonitis, massive free air, sepsis, undrainable abscess guided by CT or ultrasound, obstruction, or uncontrolled fistulas.10 Fistulas can form by the progression of abscesses from the colon to the surrounding structures.4 This happens in 10% to 12% of cases of diverticulitis.3,4
Some surgeons advocate surgery after the first episode of diverticulitis in immunocompromised patients.3 These patients are not more likely to develop diverticulitis, but they are more likely to develop abscesses and perforation and less likely to respond to medication therapy.2,3,6 However, they do not always present with fever and elevated white blood cell count, so it is difficult to diagnose diverticulitis in these patients. Since immunocompromised patients are more prone to perioperative mortality, caution should be exercised when deciding to perform surgery.3
Chronic diverticular disease may never progress to diverticulitis. Patients may present with chronic lower left quadrant pain but no fever or elevated white blood cell count. Surgery is elective and considered a safe treatment option for these patients.2
Other Treatments
Probiotics: Probiotics are “good” bacteria that are ingested orally and affect the intestinal microbial flora. The three ways in which they are beneficial are: 1) they colonize the gut, which in turn inhibits the growth of “bad” bacteria; 2) they modulate the immune function of the host; and 3) they improve the intestinal epithelial layer, thus improving its barrier function and discouraging the transmigration of bacteria. Since there may be an alteration of the intestinal flora in and around diverticula that can result in chronic inflammation, the concept of using probiotics for the prevention of diverticulitis seems plausible. By discouraging the growth of pathogenic microbes in the diverticula and the adjacent area, as well as boosting immune function, probiotics may play a beneficial role in tempering the inflammation associated with diverticulitis. There are limited data supporting this theory, however, and more studies need to be done in order to solidify this presumption.12
Anti-inflammatories: Anti-inflammatory drugs, 5-aminosalicylic acid (5-ASA) medications in particular, may be of benefit to patients with chronic low-level diverticular symptoms.3 There is strong evidence that mesalamine taken with rifamixin (a nonabsorbable antibiotic) improves the severity of symptoms of patients with diverticular disease. It also prevents recurrence of diverticulitis episodes in patients with complicated diverticulitis.11
Prognosis
Diverticulitis will recur in 20% to 30% of patients.2,7 Roughly one-third of patients treated nonoperatively will have a recurrent episode, in many cases within 1 year. Recurrence may be prevented in more than 70% who supplement their diet with fiber long term.6 Many of the patients who suffer a recurrent attack have co-existing IBD. Even after a colonic resection, recurrence is approximately 1%.2
Inflammatory Bowel Disease
There is now thought to be an overlap between chronic diverticular inflammation and the inflammation of IBD.3 Segmental colitis associated with diverticula (SCAD) is a chronic condition occurring in the areas of the colon with diverticular formation. It is often diagnosed as ulcerative colitis or Crohn's disease; however, there are no ulcers with SCAD. The inflammation associated with SCAD typically affects the mucosa between the diverticula and not the diverticula themselves. Although IBD and SCAD share some of the same histologic changes, it is generally accepted that they are distinct clinical entities. Interestingly, patients with SCAD go on to develop IBD after resection of the affected segment of the colon. This gives rise to an “overlap” hypothesis between diverticular disease and IBD.3
Conclusion
Diverticulitis (inflammation of diverticula) is a painful condition that results in high morbidity and even mortality. Uncomplicated diverticulitis can sometimes be managed on an outpatient basis with dietary restrictions and antibiotics. Complicated diverticulitis, and some cases of uncomplicated diverticulitis, require hospitalization. Patients need to be placed on bowel rest and must be given IV fluids and antibiotics.
A high-fiber diet can alleviate symptoms of diverticular disease (diverticulosis and diverticulitis) and prevent recurrence of acute diverticulitis. A growing body of evidence suggests that mesalamine with rifamixin may also be used as maintenance therapy to alleviate symptoms. There is even some talk of probiotics being beneficial in diverticular disease, though more studies must be done to confirm this.
The pharmacist can be of great value to the patient with diverticular disease. The pharmacist can counsel him or her on appropriate dietary changes, as well as ensure that the proper antibiotics are being used. The pharmacist can also help the patient select appropriate sources of fiber and, possibly in the future, probiotics. Finally, the pharmacist can stress to the patient the importance of medication compliance and offer alternatives to the physician if the patient cannot tolerate a regimen.
REFERENCES
1. Diverticular disease. American Society of Colon and Rectal Surgeons. 2009. www.fascrs.org/patients/
2. Frattini J, Longo WE. Diagnosis and treatment of chronic and recurrent diverticulitis. J Clin Gastroenterol. 2006;40(suppl 3):S145-S149.
3. Sheth AA, Longo W, Floch MH. Diverticular disease and diverticulitis. Am J Gastoenterol. 2008;103:1550-1556.
4. Salzman H, Lillie D. Diverticular disease: diagnosis and treatment. Am Fam Physician. 2005;72:1229-1234.
5. Commane DM, Arasaradnam RP, Mills S, et al. Diet, ageing, and genetic factors in the pathogenesis of diverticular disease. World J Gastroenterol. 2009;15:2479-2488.
6. Rafferty J, Shellito P, Hyman NH, Buie WD. Practice parameters for sigmoid diverticulus. Dis Colon Rectum. 2006;49:939-944.
7. Barter C, Dunne L. Abdominal pain. In: South-Paul JE, Matheny SC, Lewis EL, eds. Current Diagnosis & Treatment in Family Medicine. 2nd ed. New York, NY: McGraw-Hill Companies; 2008; chapter 29.
8. Strate LL, Lui YL, Aldoori WH, et al. Obesity increases the risk of diverticulitis and diverticular bleeding. Gastroenterology. 2009;136:115-122.
9. McQuaid KR. Gastrointestinal disorders. In: McPhee SJ, Papadakis MA, eds. Current Medical Diagnosis & Treatment. 49th ed. New York, NY: McGraw-Hill Companies; 2010; chapter 15.
10. Floch CL. Diagnosis and management of acute diverticulitis. J Clin Gastroenterol. 2006;40(suppl 3):S136-S144.
11. Trivedi CD, Das KM. Emerging therapies for diverticular disease of the colon. J Clin Gastroenterol. 2008;42:1145-1151.
12. White JA. Probiotics and their use in diverticulitis. J Clin Gastroenterol. 2006;40(suppl 3):S160-S162.
To comment on this article, contact rdavidson@uspharmacist.com.





