US Pharm. 2022;47(6):HS2-HS6.
ABSTRACT: A hernia is the protrusion of a visceral organ through a weakened area of tissue that normally holds it in. Common risk factors for hernia development include advanced age, obesity, pregnancy, malignancy, abdominal surgery, and intense physical activity. Hernias are classified based on their location and etiology, with abdominal hernia being the most prevalent type in the United States. Inguinal hernia and hiatal hernia offer opportunities for pharmacists to be involved in patient care. Although hernias are usually repaired surgically, in some cases nonsurgical therapies may be used. Regardless of the approach taken, pharmacists can play a role in medication optimization, selection of self-care products, counseling on lifestyle modifications, and postsurgical wound-care management.
A hernia occurs when a visceral organ, such as the bowel or stomach, protrudes through a weakened area of musculature and/or connective tissue that normally keeps it contained.1 There are many different types of hernia. Although the exact prevalence of all hernia types in the United States is unknown, the estimated prevalence of abdominal hernia—the most common form of hernia—is 1.7%, with more than 700,000 surgical repairs performed annually.2,3 Generally, the risk factors for developing a hernia depend on the hernia type, and hernia development is associated with the presence of congenital abnormalities of underlying tissue; the existence of comorbidities such as malignancy, chronic obstructive lung disease, ascites, and chronic intestinal obstruction; diet; pregnancy; and intense or repetitive physical activity.4,5
There is not one classification system for all hernias; instead, most hernias are classified based on their anatomical location (e.g., abdominal, diaphragmatic, perineal, lumbar) and characteristics (e.g., size, severity, etiology). As stated above, most hernias occur in the abdomen. The two most common forms of abdominal hernia are inguinal hernia (IH) and femoral hernia, which are generally treated and managed similarly. A common diaphragmatic hernia is the hiatal hernia (HH). Although the cornerstone of treatment for the various types of hernias is surgery, this article will focus on IH and HH, as they offer opportunities for pharmacists to be involved in patient care.6,7
Inguinal Hernia
More than 2.3 million inpatient abdominal hernias were repaired in the U.S. over a 10-year period (2001 to 2010).2 IH, which involves the protrusion of a visceral structure or adipose tissue through the abdominal wall, is the most prevalent subtype of abdominal hernia and accounts for nearly two-thirds of cases in the U.S.8 Risk factors for developing IH include a history of hernia or hernia repair, older age, male sex, Caucasian ethnicity, low BMI, systemic connective-tissue disorders, smoking and associated chronic cough, chronic constipation, and low birthweight.7 Signs and symptoms of IH may include a visible lump, heavy discomfort around the gut, pain or aching upon exertion, enlargement of the lump upon coughing, and constipation.7 Severe pain and discomfort with a visible bulge may indicate a strangulated hernia, a phenomenon in which the blood flow in part of the intestine is cut off, resulting in necrosis.
IHs are usually identified via physical examination. Ultrasound imaging may be used to diagnose groin hernias that are difficult to visualize or palpate.9 For many patients, the presence of a small IH does not cause significant pain or discomfort that would affect day-to-day quality of life. In fact, more than one-third of patients who present with an IH are asymptomatic. The international guidelines for groin hernia management recommends that asymptomatic and some mildly symptomatic patients enter a watch-and-wait period following initial diagnosis.7 It is also recommended that surgery be withheld in male patients with minimal symptoms that do not significantly affect their physical activity.10,11
There are a number of nonpharmacologic and nonsurgical approaches to IH management (TABLE 1). One nonsurgical method is the use of a truss.12,13 A truss is similar to an athletic supporter, with a hard plug positioned over the hernia site.14 The efficacy of truss use is questionable, but when fitted appropriately, the hard plug exerts pressure to keep the hernia contents in the abdomen. Trusses may be available through an outpatient pharmacy.

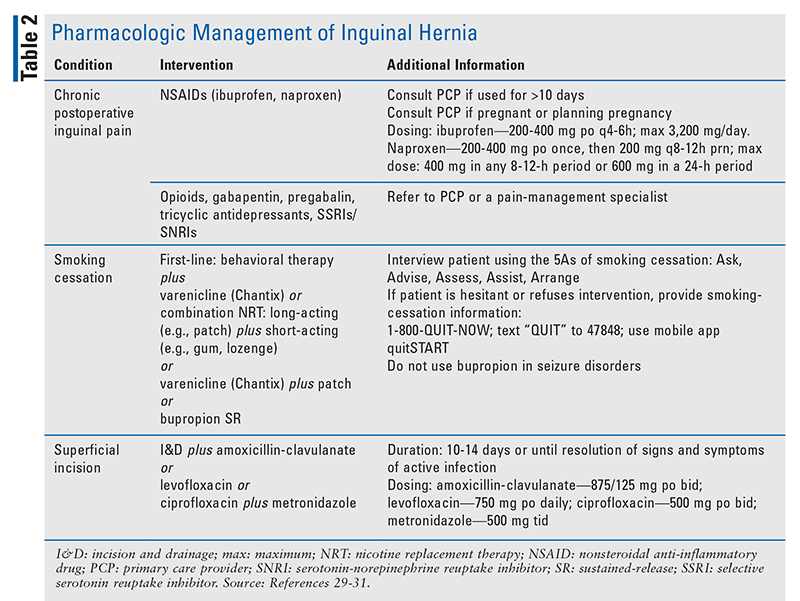
Symptomatic management of IH is crucial to a patient’s quality of life. OTC analgesics can help ameliorate pain symptoms both before and after surgical repair. More than 15% of patients experience pain that significantly alters their quality of life within 6 months after surgery.15 Postoperative pain occurring within 3 months of surgery can be managed with nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids. Pain occurring 3 to 6 months after surgery, known as chronic postoperative inguinal pain, is often treated with neuropathic pain analgesics (e.g., tricyclic antidepressants, selective serotonin reuptake inhibitors or serotonin-norepinephrine reuptake inhibitors, gabapentinoids) and NSAIDs (TABLE 2).16 Other postoperative complications that a patient may experience include chronic constipation and superficial incisional surgical-site infections requiring the initiation of empiric antibiotics.17
Hiatal Hernia
HH is characterized by a protrusion of the upper stomach and/or abdominal viscera (other than the esophagus) into the thoracic cavity through the esophageal hiatus in the diaphragm.18 HH is frequently associated with gastroesophageal reflux disease (GERD) because the hiatal laxity causes gastric content and acid to back up into the esophagus. Therefore, symptoms range from heartburn, dysphagia, or regurgitation to extraesophageal symptoms such as chronic cough or asthma.19 HHs are most often confirmed by radiographic, endoscopic, or manometric assessment.20
HH is relatively common, with a higher prevalence in the aging and overweight populations. In fact, 55% to 60% of persons older than 50 years of age have some degree of HH.19 However, this is variable because the majority of HHs are asymptomatic; only about 9% of patients present with symptoms.19 Older age and high BMI are key risk factors; other known risk factors include multiple pregnancies, history of esophageal surgery, gastrectomy, and certain disorders of the skeletal system associated with bone decalcification and degeneration.20,21
HHs are classified into four subtypes. Type I, or sliding HH, is the most common (>95% of cases) and is most closely associated with GERD.22 A sliding HH occurs when the gastroesophageal junction (GEJ) migrates up toward the hiatus, above the diaphragm. Types II, III, and IV are paraesophageal HHs. A paraesophageal HH occurs when part of the stomach herniates into the mediastinum adjacent to the esophagus while the GEJ remains in place.23
The management of HH depends on the type of hernia and the severity of symptoms. Similar to IH, the presence of HH is not an indication for treatment; therefore, therapy is recommended only for patients who have symptoms attributable to the condition.20 Management sometimes requires a multifaceted approach, including lifestyle modifications, pharmacologic therapy, surgical interventions, and endoscopic management.24 Most symptomatic sliding HHs are related to acid reflux; therefore, goals of treatment goals involve the alleviation of symptoms of acid reflux and the promotion of esophageal healing.
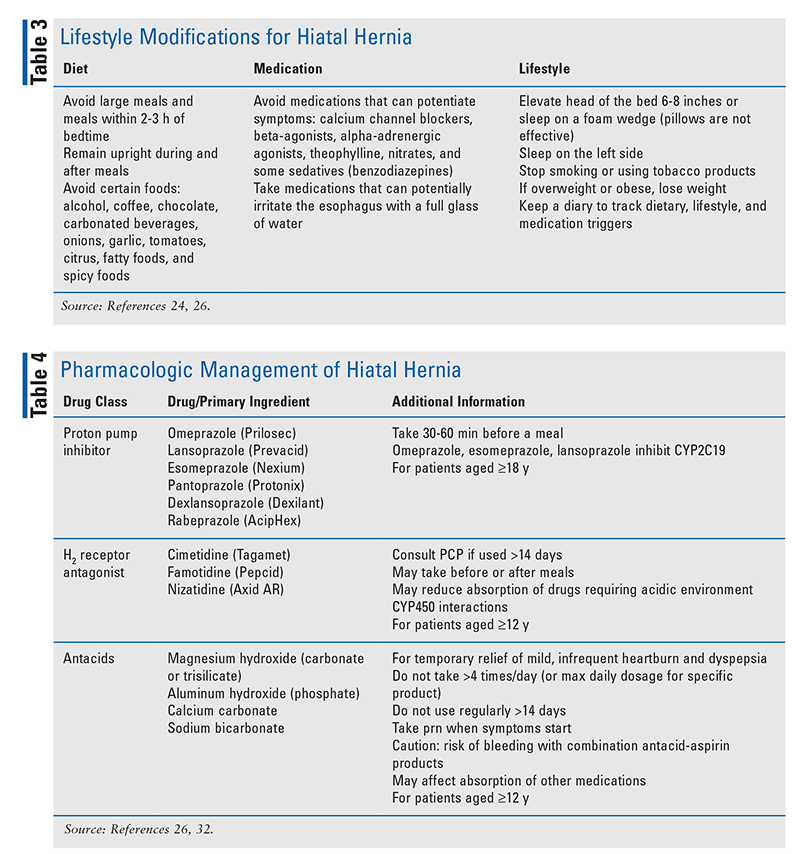
Lifestyle and dietary modifications (TABLE 3) are the initial step in the general treatment approach for GERD.24 The backbone of pharmacologic treatment constitutes medications that neutralize gastric acid, with proton pump inhibitors (PPIs) being the medications of choice (TABLE 4). Current guidelines recommend using the lowest possible PPI dose that will adequately control the symptoms.25 Alternatives include antacids and H2 receptor antagonists (H2RAs). Antacids should be used only for the relief of mild symptoms associated with GERD; this is because of their short duration of action and inability to heal erosive esophagitis. H2RAs may be effective for symptoms of mild-to-moderate GERD, but response rates vary based on disease severity, drug dose, and duration of therapy.26 These options may be used as needed or as add-on therapy for persistent symptoms despite PPI use. There is no evidence supporting the efficacy of prokinetic drugs in the treatment of HH associated with GERD; therefore, they are not recommended.23
Paraesophageal HH often requires a different treatment approach because gastric fundal migration above the diaphragm puts patients at risk for complications such as bleeding, obstruction, and perforation. Symptomatic patients with paraesophageal HH will derive little to no relief from gastric acid–lowering medications. The definitive treatment for paraesophageal HH is surgery, either laparoscopic or open repair.21 Surgery may also be recommended for patients with a sliding HH who have severe or refractory symptoms and also exhibit poor medication compliance, or for younger patients who wish to avoid a lifetime of treatment.20 The function of surgical interventions is to correct the HH by restoring the intraabdominal esophagus, reconstructing the diaphragmatic hiatus, and reinforcing the lower esophageal sphincter.
The Pharmacist’s Role
Because hernias are common, pharmacists should have a basic understanding of hernia care in order to better assist patients. Managing the various types of hernias requires an interprofessional team approach. Although surgery is the mainstay of hernia treatment, pharmacists can play a role in the management of hernias and support patients who have undergone treatment. Regardless of the setting, pharmacists can assist patients with managing pain medication and selecting appropriate self-care products. Pharmacists can also advise patients about postoperative care, such as wound care, and lifestyle modifications, such as smoking cessation (TABLE 2). A truss may be recommended for some patients, and pharmacists can counsel on their proper use. Above all, pharmacists can ensure that medications for hernia therapy are being used safely, effectively, and optimally.
REFERENCES
1. Hammoud M, Gerken J. Inguinal hernia. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2021. www.ncbi.nlm.nih.gov/books/NBK513332/. Accessed May 6, 2022.
2. Beadles CA, Meagher AD, Charles AG. Trends in emergent hernia repair in the United States. JAMA Surg. 2015;150(3):194-200.
3. Schumpelick V, Treutner KH, Arlt G. Inguinal hernia repair in adults. Lancet. 1994;344(8919):375-379.
4. Rosemar A, Angerås U, Rosengren A. Body mass index and groin hernia: a 34-year follow-up study in Swedish men. Ann Surg. 2008;247(6):1064-1068.
5. Ruhl CE, Everhart JE. Risk factors for inguinal hernia among adults in the US population. Am J Epidemiol. 2007;165(10):1154-1161.
6. Perez JE, Schmidt MA, Narvaez A, et al. Evolving concepts in ventral hernia repair and physical therapy: prehabilitation, rehabilitation, and analogies to tendon reconstruction. Hernia. 2021;25(4):1-13.
7. HerniaSurge Group. International guidelines for groin hernia management. Hernia. 2018;22(1):1-165.
8. Jenkins JT, O’Dwyer PJ. Inguinal hernias. BMJ. 2008;336(7638):269-272.
9. Shakil A, Aparicio K, Barta E, Munez K. Inguinal hernias: diagnosis and management. Am Fam Physician. 2020;102(8):487-492.
10. Hair A, Paterson C, Wright D, et al. What effect does the duration of an inguinal hernia have on patient symptoms? J Am Coll Surg. 2001;193(2):125-129.
11. Gong W, Li J. Operation versus watchful waiting in asymptomatic or minimally symptomatic inguinal hernias: the meta-analysis results of randomized controlled trials. Int J Surg. 2018;52:120-125.
12. Cheek CM, Williams MH, Farndon JR. Trusses in the management of hernia today. Br J Surg. 1995;82(12):1611-1613.
13. McIntosh A, Hutchinson A, Roberts A, Withers H. Evidence-based management of groin hernia in primary care—a systematic review. Fam Pract. 2000;17(5):442-447.
14. Pearson DG. Hernia truss: can it help an inguinal hernia? Mayo Clinic. www.mayoclinic.org/diseases-conditions/inguinal-hernia/expert-answers/hernia-truss/faq-20058111. Accessed March 28, 2022.
15. Andresen K, Burcharth J, Fonnes S, et al. Chronic pain after inguinal hernia repair with the ONSTEP versus the Lichtenstein technique, results of a double-blinded multicenter randomized clinical trial. Langenbecks Arch Surg. 2017;402(2):213-218.
16. Alfieri S, Amid PK, Campanelli G, et al. International guidelines for prevention and management of post-operative chronic pain following inguinal hernia surgery. Hernia. 2011;15(3):239-249.
17. Bratzler DW, Dellinger EP, Olsen KM, et al. Clinical practice guidelines for antimicrobial prophylaxis in surgery. Surg Infect (Larchmt). 2013;14(1):73-156.
18. Kohn GP, Price RR, DeMeester SR, et al. Guidelines for the management of hiatal hernia. Surg Endosc. 2013;27(12):4409-4428.
19. Smith RE, Shahjehan RD. Hiatal hernia. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2022. www.ncbi.nlm.nih.gov/books/NBK562200/. Accessed May 6, 2022.
20. Hyun JJ, Bak YT. Clinical significance of hiatal hernia. Gut Liver. 2011;5(3):267-277.
21. Sfara A, Dumitrascu DL. The management of hiatal hernia: an update on diagnosis and treatment. Med Pharm Rep. 2019;92(4):321-325.
22. Weston AP. Hiatal hernia with Cameron ulcers and erosions. Gastrointest Endosc Clin N Am. 1996;6(4):671-679.
23. Kahrilas PJ, Kim HC, Pandolfino JE. Approaches to the diagnosis and grading of hiatal hernia. Best Pract Res Clin Gastroenterol. 2008;22(4):601-616.
24. Katz PO, Dunbar KB, Schnoll-Sussman FH, et al. ACG Clinical Guideline for the diagnosis and management of gastroesophageal reflux disease. Am J Gastroenterol. 2022;117(1):27-56.
25. Roman S, Kahrilas PJ. The diagnosis and management of hiatus hernia. BMJ. 2014;349:g6154.
26. Law EJ, Fong JJ. Upper gastrointestinal disorders. In: Zeind CS, Carvalho MG, eds. Applied Therapeutics: The Clinical Use of Drugs. 11th ed. Philadelphia, PA: Wolters Kluwer; 2018:480-517.
27. O’Keefe SJ. The association between dietary fibre deficiency and high-income lifestyle-associated diseases: Burkitt’s hypothesis revisited. Lancet Gastroenterol Hepatol. 2019;4(12):984-996.
28. Kingsnorth A, LeBlanc K. Hernias: inguinal and incisional. Lancet. 2003;362(9395):1561-1571.
29. Martínez C, Castellano Y, Andrés A, et al. Factors associated with implementation of the 5A’s smoking cessation model. Tob Induc Dis. 2017;15:41.
30. Naproxen. Lexi-Drugs [online database]. Riverwoods, IL: Lexi-Comp, Inc. https://online.lexi.com. Accessed March 25, 2022.
31. Ibuprofen. Lexi-Drugs [online database]. Riverwoods, IL: Lexi-Comp, Inc. https://online.lexi.com. Accessed March 25, 2022.
32. Whetsel T, Zweber A. Ch. 13: Heartburn and dyspepsia. In: Krinsky DL, Ferreri SP, Hemstreet B, et al, eds. Handbook of Nonprescription Drugs: An Interactive Approach to Self-Care. 19th ed. Washington, DC: American Pharmacists Association; 2017.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





