US Pharm. 2014;39(3):HS2-HS8.
ABSTRACT: Acetaminophen toxicity is one of the most common causes of both intentional and unintentional poisoning in the United States. It has become the most common cause of acute liver failure and the second most prevalent cause of liver failure requiring transplantation. Acetaminophen is often recommended by doctors and highly utilized by patients in both prescription and OTC products for a variety of conditions. The FDA has long been updating its recommendations regarding acetaminophen use to help improve patient safety. This article reviews the etiology, signs, and symptoms of acetaminophen toxicity and the role of the pharmacist in the prevention of acetaminophen misuse.
Acetaminophen is often recommended by doctors and highly utilized by patients in both prescription and OTC products for a variety of conditions, making it undoubtedly one of the most common drugs encountered by pharmacists.1-3 In the United States, 40% of the adult population reported using OTC acetaminophen monthly, and 23% of the adult population reported using either OTC or prescription acetaminophen weekly.1,2
Acetaminophen (paracetamol or APAP) has analgesic and antipyretic properties similar to aspirin’s, but minimal anti-inflammatory properties.4 It is indicated for mild-to-moderate pain or fever, and it is not associated with stomach discomfort or bleeding at recommended doses. When used appropriately, it has a very well-established safety and efficacy profile.5 However, hepatotoxicity is a common consequence of overconsumption, which can result in a range of problems, including abnormalities in liver function, acute liver failure, and even death.6
Acetaminophen toxicity is one of the most common causes of both intentional and unintentional poisoning in the U.S. In fact, there has been a steady increase in the incidence of acetaminophen-related toxicity over the past decade.7,8 This is likely attributed to the widespread availability of acetaminophen as both a single ingredient and in combination with other OTC and prescription medications in various concentrations and formulations. Acetaminophen-associated overdoses account for approximately 56,000 emergency department visits, 26,000 hospitalizations, and over 450 deaths annually.9 Acetaminophen-induced liver toxicity has become the most common cause of acute liver failure and the second most common cause of liver failure requiring transplantation.10,11 Therefore, it is imperative that pharmacists recognize signs and symptoms of overdose and toxicity, and counsel their patients on proper dosing and usage.
Pharmacokinetics
Upon ingestion, acetaminophen is rapidly absorbed from the gastrointestinal (GI) tract and quickly distributed throughout the body. Peak plasma concentrations are achieved within 30 to 60 minutes4; food may delay time to peak concentration, but the extent of absorption is not affected.12 With overdoses, peak plasma concentrations are usually achieved within 4 hours.13 The half-life of acetaminophen is approximately 2 to 3 hours after therapeutic doses, yet can be increased to more than 4 hours in patients with hepatic injury.4,12,14
Acetaminophen is extensively metabolized by the liver via three main hepatic pathways: glucuronidation, sulfation, and CYP450 2E1 oxidation.12 Approximately 90% of acetaminophen is conjugated to sulfated and glucuronidated metabolites that are renally eliminated.14 Of the remaining acetaminophen, approximately 2% is excreted unchanged in the urine and the rest undergoes CYP450-mediated oxidation to form a reactive metabolite, N-acetyl-p-benzoquinone imine (NAPQI).15-18 Under normal circumstances, this toxic metabolite reacts with sulfhydryl groups in glutathione, converting it to harmless metabolites before being excreted in the urine.4
Toxicity
Drugs may have toxic effects due to various reasons. Toxicity of some drugs is related to the formation of an undesirable metabolite; consequently, toxicity of acetaminophen is related to the production of NAPQI. With large acute doses or with chronic use, the major metabolic pathways—the glucuronide and sulfate conjugation systems—become saturated, and more acetaminophen is metabolized by the CYP450 system. This results in increased production of NAPQI. When glutathione is approximately 70% depleted, NAPQI begins to accumulate in the hepatocytes, resulting in hepatic damage.15,16,18 Therefore, the replacement of glutathione with glutathione-mimicking compounds such as N-acetylcysteine serves as a useful antidote to acetaminophen toxicity.
Acetaminophen toxicity can result from either an acute overdose or from chronic overuse. Acute overdose is defined as consumption of a toxic amount of a drug within an 8-hour period, whereas chronic overdose occurs as a result of repeated doses at or above the recommended limit.12 Unintentional overdoses may also occur as a result of ingestion of multiple products containing acetaminophen. The recommended dose of acetaminophen in adults is 650 to 1,000 mg every 4 to 6 hours, not to exceed 4,000 mg in a 24-hour period; in children, the recommended dose is 10 to 15 mg/kg every 4 to 6 hours, not to exceed 50 to 70 mg/kg in 24 hours.12 Single doses of more than 150 mg/kg or 7.5 g in adults have been considered potentially toxic, although the minimal dose associated with liver injury can range anywhere from 4 to 10 g.6,12,14,19 In children, single doses of 120 mg/kg to 150 mg/kg have been associated with hepatotoxicity; however, doses <200 mg/kg are unlikely to result in toxicity.14,20
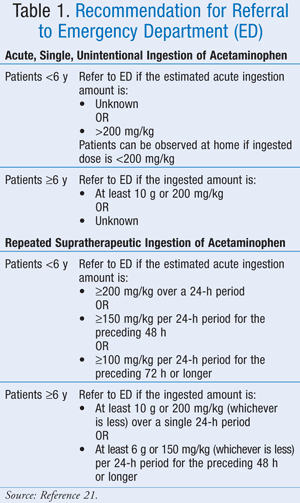
While the exact maximum dose has not been well defined, the American Association of Poison Control Centers (AAPCC) has recommended that regardless of the amount of drug ingested, a patient should be brought for medical evaluation if he or she displays signs or symptoms consistent with toxicity.21 The AAPCC has provided guidelines for hospital referral both for acute, single, unintentional ingestion of acetaminophen and for repeated supratherapeutic ingestion of acetaminophen (TABLE 1).21
Clinical Presentation
Regardless of whether acetaminophen toxicity occurs because of a single overdose or after repeated supratherapeutic ingestion, the progression of acetaminophen poisoning can be described in four sequential phases: preclinical toxic effects (phase one), hepatic injury (phase two), hepatic failure (phase three), and recovery (phase four).6,22 Patients treated during the preclinical stage may develop transient liver damage but fully recover.22 Patients who are not treated until hepatic injury is already evident have a variable prognosis; however, those who present with hepatic failure have a mortality rate of 20% to 40%.22
The first phase occurs a few hours after ingestion of a toxic dose, and lasts 12 to 24 hours. It is important to note the delay in the appearance of symptoms, as healthcare providers should understand the implications of toxicity that will follow this quiescent period. Symptoms during the first 24 hours are not diagnostic or specific and include nausea, vomiting, diaphoresis, anorexia, and lethargy, the severity of which will be in direct correlation to the size of the dose ingested.8
In the second phase, occurring up to 24 to 48 hours after ingestion, there may be a false sense of recovery as GI symptoms improve or disappear.6,8 However, as hepatotoxicity continues to emerge, abdominal pain or right upper quadrant tenderness may surface. In addition, laboratory values will begin to show evidence of hepatotoxicity; hepatic enzymes, lactate, phosphate, prothrombin time, and international normalized ratio (INR) will increase dramatically.6,8,12 Most patients do not progress beyond this stage, especially if the antidote acetylcysteine is administered.8,12
A few patients will progress to phrase three, usually occurring 3 to 5 days postingestion. This phase is characterized by the reappearance or worsening of nausea and vomiting accompanied by malaise, jaundice, and central nervous symptoms including confusion, somnolence, and coma.6 Serious and possibly fatal hepatic necrosis may occur. Although less common, renal insufficiency, as demonstrated by oliguria, can manifest as a result of acetaminophen-induced tubular necrosis.6,8,12 Hepatic enzyme levels will reach their peak, measuring as high as 10,000 IU/L. Jaundice, hypoglycemia, bleeding and coagulation abnormalities, and hepatic encephalopathy will also be evident.8,12 Death may occur as a consequence of complications associated with hepatic failure, including multiorgan system failure, cerebral edema, and sepsis.15
Lastly, phase four involves survival and recovery, generally with return of full liver function and no long-term effects.6 Approximately 70% of patients who enter phase four recover completely, while 1% to 2% of patients develop fatal hepatic failure.6 Severe, untreated acetaminophen toxicity will result in death within 4 to 18 days after ingestion.6
Patients at Increased Risk
Because the mechanism of acetaminophen toxicity occurs via the formation of NAPQI, any factors that influence the availability of metabolic enzymes will therefore affect toxicity. Alcohol use, malnutrition, and induction of CYP450 enzymes by drugs, including long-term treatment with carbamazepine, primidone, rifampin, efavirenz, and St. John’s wort, may impact how an individual responds to acetaminophen.23 Patients affected by any of the above factors should be identified so that pharmacists may counsel them closely on how to safely use acetaminophen.
Acutely, ethanol serves as both a substrate for and inhibitor of CYP2E1, limiting the amount of NAPQI formed. Conversely, in chronic alcohol use, ethanol is an inducer of CYP2E1, leading to a potential increase in the formation of NAPQI should an overdose of acetaminophen occur. Another consequence of chronic alcohol use is the depletion of glutathione stores, reducing the last defense against the formation of NAPQI.17 There is no evidence to suggest that use of acetaminophen in therapeutic doses is toxic in an alcoholic person; therefore, in therapeutic amounts acetaminophen can be used safely both acutely and chronically.23-25
Although controversial, starvation (prolonged fasting) and malnutrition are additional risk factors for acetaminophen toxicity.16,18,23 Similar to chronic alcohol use, malnutrition causes depletion of glutathione stores. However, there is also evidence that CYP2E1 function is markedly reduced in this patient population. These effects would thereby counteract each other, potentially resulting in no change in toxicity.26 Nevertheless, it is still prudent to identify such patients and caution them about their increased risk potential.
Management
Upon presentation, the patient should be thoroughly assessed. A detailed recent drug history should be obtained. Serum acetaminophen levels should ideally be drawn at least 4 hours after ingestion. Pharmacists can play an important role by gathering pertinent information such as the amount of drug taken, the dosage form ingested, the amount of time that has elapsed since the last ingested dose, and if any other drugs were consumed. All of these factors are important when analyzing serum acetaminophen concentrations.
If the patient presents within an hour of ingestion, gastric decontamination may be considered; activated charcoal is the only GI decontamination method recommended. Administration of activated charcoal may be considered, especially in patients who ingested delayed-release formulations of acetaminophen or who consumed other medications that would slow acetaminophen’s absorption.12 However, due to acetaminophen’s quick absorptive and distributive phases, there is otherwise little role for this method as time passes.27-29 Activated charcoal should only be administered if the patient is mentally alert with an intact airway. It should also be avoided in those with an increased risk of aspiration, uncontrolled vomiting, or coingestion of a corrosive or proconvulsant.30
Acetylcysteine: The mainstay of treatment for acetaminophen toxicity is acetylcysteine. This agent replenishes hepatic glutathione stores and increases sulfate conjugation, preventing accumulation of NAPQI.31 Acetylcysteine may be beneficial in patients presenting with acetaminophen-induced hepatic failure, as it improves hemodynamics and oxygen use, decreases cerebral edema, and improves mitochondrial energy production.14,22
Acetylcysteine may prevent hepatic failure from an acetaminophen overdose when administered early enough (within 8-10 hours following an acute overdose) but may still be of value up to 48 hours after ingestion.6,11,14,31 The standard acetaminophen toxicity nomogram, the Rumack-Matthew nomogram, can be utilized to determine the likelihood of serious liver damage. However, it is rendered ineffective when evaluating possible toxicity due to multiple ingestions over time, when time of ingestion is unknown, or when altered metabolism occurs.11 Taking this into consideration, acetylcysteine should be administered in any case of acute liver failure or when there is any evidence of liver toxicity in which acetaminophen overdose is suspected.11
Acetylcysteine is available orally and intravenously; the choice is dependent on the clinical scenario.21 Oral administration may be beneficial for patients with preclinical toxic effects or hepatic injury, although the presence of altered mental status and vomiting may limit its use.22 The dosing regimen for oral acetylcysteine is a loading dose of 140 mg/kg, followed by 17 doses of 70 mg/kg every 4 hours for a total of 72 hours.11 Patients with hepatic failure should receive IV therapy.22 Continuous IV infusion is recommended at a loading dose of 150 mg/kg IV in 200 mL D5W infused over 60 minutes followed by a maintenance dose of 50 mg/kg over 4 hours, followed by a second maintenance dose of 100 mg/kg in 1,000 mL D5W administered over 16 hours.11 If the patient is under 40 kg, fluid should be adjusted as per guidelines to avoid fluid overload, hyponatremia, and seizures. If the patient is doing well yet has not fully recovered after the recommended dosing, acetylcysteine therapy can be continued using either the last oral dose or the last IV infusion rate. Acetylcysteine should be continued beyond the protocol length until acetaminophen concentrations are undetectable, serum AST has normalized or significantly improved, and there is resolution of any evidence of hepatic failure.13
Because its unpleasant taste and smell, vomiting frequently occurs with oral acetylcysteine administration.31,32 Adverse effects associated with IV acetylcysteine include anaphylactoid reactions, including rash, pruritus, angioedema, bronchospasm, tachycardia, and hyper-tension.31,32 In addition, when using IV acetylcysteine, pharmacists must be aware of the potential for medication errors. The complicated regimen, length of therapy, and need for multiple health professionals to administer doses at various treatment sites greatly increase the risk for errors.33 One retrospective study identified a 33% incidence of medication errors with IV acetylcysteine.33 The most common type of error found in this study was a delay in therapy, which can potentially reduce the efficacy of acetylcysteine. Another common error identified was the unnecessary administration of acetylcysteine, resulting in unnecessary costs. It is important for healthcare providers to consult with poison centers in cases of acetaminophen overdoses. They can provide the most up to date dosing information and protocols to ensure proper administration of acetylcysteine.
FDA Labeling
In hopes of increasing safety and reducing toxicity, the FDA has long been updating its recommendations regarding acetaminophen use. In the late 1990s, research demonstrated that acetaminophen was a leading cause of acute liver failure in the U.S., the majority of cases having resulted from accidental overdoses.34 In 1998, the FDA issued a warning label on acetaminophen products that urged patients who consumed more than three alcoholic beverages per day to consult a physician before using this medication. As years passed and the correlation between acetaminophen and liver toxicity became even more evident, the FDA convened a meeting to act upon these findings. In 2002, the FDA Advisory Committee recommended that a liver toxicity warning be placed on all acetaminophen-containing products. In 2009, new labeling was developed to help patients easily identify which products contained acetaminophen, reducing the potential for accidental overdoses. A black box warning was later placed on all prescription acetaminophen products emphasizing the potential risk for severe liver injury, and a warning for rare but serious anaphylaxis and other hypersensitivity reactions was implemented.34
In August 2013, the FDA alerted consumers of rare but serious and potentially fatal skin reactions, such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and acute generalized exanthematous pustulosis (AGEP), linked to acetaminophen use.35 Patients should be counseled for signs and symptoms of skin reactions, such as peeling, blistering, reddening, and detachment of skin, wherein they should stop any further drug use and seek medical attention immediately.
The FDA has also announced that as of January 2014, the amount of acetaminophen found in prescription combination products must be limited to 325 mg per tablet or capsule.36,37 In May 2011, manufacturers of nonprescription acetaminophen products voluntarily announced that a single children’s strength of liquid acetaminophen (160 mg/5 mL) will be the only concentration available; the concentrated infant drops will no longer be produced.38
Although progress has been made, some things are still to be determined. The FDA Advisory Committee has voted in favor of many changes thought to improve safety and decrease toxicity, yet the FDA has not yet taken action. For example, while the maximum daily dose of acetaminophen was previously set at 4 g/day, the FDA Advisory Committee suggests decreasing it in an effort to reduce overdoses.37 It is important to note that some manufacturers have already updated their labeling to reflect these recommendations, although it is not yet mandatory to do so. Efforts are also being made to improve product labeling, enhance patient education, create a universal pediatric formulation, eliminate acetaminophen combination products, and reduce the strength of OTC acetaminophen products to 325 mg per tablet with a maximum single dose of 650 mg.37 While no final consensus on any of these issues has been reached, healthcare providers should educate their patients on the importance of following labeling instructions.
Role of the Pharmacist
Pharmacists are in a position to effectively promote the safe use of acetaminophen. Many patients are not aware of the maximum daily dose of acetaminophen and the potential for toxicity.39 In addition, patients may not understand that acetaminophen is contained in more than 600 different products.39 All patients receiving a prescription for an acetaminophen-containing product need to be counseled to ensure awareness of the active ingredient. Pharmacists must take a proactive role in educating patients who purchase OTC acetaminophen products. Pharmacists are vital to preventing acetaminophen misuse by guaranteeing the safe use of the drug through patient education and a review of patients’ medication histories.
In addition, pharmacists should recommend that patients contact the national Poison Help Line if they suspect an acetaminophen overdose. The toll-free number is 1-800-222-1222.40 By calling this number, patients will be connected to the nearest regional poison control center with specialists available 24 hours a day, 7 days a week. These specialists will be able to help assess and manage the potential acetaminophen overdose. Such activities will minimize the risk of inappropriate dosing, duplication of therapy, and inappropriate drug use.
REFERENCES
1. Kaufman DW, Kelly JP, Rosenberg L, et al. Recent
patterns of medication use in the ambulatory adult population of the
United States: the Slone survey. JAMA. 2002;287:337-344.
2. Paulose-Ram R, Hirsch R, Dillon C, et al. Prescription
and nonprescription analgesic use among the US adult population: results
from the third National Health and Nutrition Examination Survey (NHANES
III). Pharmacoepidemiol Drug Saf. 2003;12:315-326.
3. Paulose-Ram R, Hirsch R, Dillon C, et al. Frequent
monthly use of selected nonprescription and prescription non-narcotic
analgesics among U.S. adults. Pharmacoepidemiol Drug Saf. 2005;14:257-266.
4. Burke A, Smyth EM, Fitzgerald GA. Analgesic-antipyretic
agents; pharmacotherapy of gout. In: Brunton LL, Laso JS, Parker K,
eds. Goodman and Gilman’s the Pharmacological Basis of Therapeutics. 11th ed. New York, NY: McGraw-Hill; 2006:671-716.
5. Watkins PB, Kaplowitz N, Slattery JT, et al.
Amino-transferase elevations in healthy adults receiving 4 grams of
acetaminophen daily: a randomized controlled trial. JAMA. 2006;296:87-93.
6. Chun LJ, Tong MJ, Busuttil RW, et al. Acetaminophen hepatotoxicity and acute liver failure. J Clin Gastroenterol. 2009;43:342-349.
7. Bronstein AC, Spyker DA, Cantilena LR, et al. 2011
annual report of the American Association of Poison Control Centers’
National Poison Data System (NPDS): 29th annual report. Clin Toxicol. 2012;50:911-1164.
8. Schilling A, Corey R, Leonard M, et al. Acetaminophen: old drug, new warnings. Cleve Clin J Med. 2010;77:19-27.
9. Nourjah P, Ahmad SR, Karwoski C, et al. Estimates of acetaminophen (paracetamol)-associated overdoses in the United States. Pharmacoepidemiol Drug Saf. 2006;15:398-405.
10. Larson AM, Polson J, Fontana RJ, et al.
Acetaminophen-induced acute liver failure: results of a United States
multicenter, prospective study. Hepatology. 2005;42:1364-1372.
11. Lee WM, Larson AM, Stravitz T. AASLD position paper:
the management of acute liver failure: update 2011. Baltimore, MD:
American Association for the Study of Liver Diseases; September 2011.
www.aasld.org/practiceguidelines/Documents/AcuteLiverFailureUpdate2011.pdf.
Accessed December 15, 2013.
12. Tylenol (acetaminophen) professional product information. Fort Washington, PA: McNeil Consumer Healthcare; 2010.
13. Hendrickson RG. Acetaminophen. In: Nelson LS, Lewin NA, Howland M, eds. Goldfrank’s Toxicologic Emergencies. 9th ed. New York, NY: McGraw-Hill; 2011:483-99.
14. Hodgman MJ, Garrard AR. A review of acetaminophen poisoning. Crit Care Clin. 2012;499-516.
15. Larson AM. Acetaminophen hepatotoxicity. Clin Liver Dis. 2007;11:525-548.
16. Rumack BH. Acetaminophen hepatotoxicity: the first 35 years. J Toxicol Clin Toxicol. 2002;40:3-20.
17. Nelson SD. Molecular mechanisms of the hepatotoxicity caused by acetaminophen. Semin Liver Dis. 1990;10:267-278.
18. Lee WH. Drug-induced hepatotoxicity. N Engl J Med. 1995;333:1118-1127.
19. Fontana RJ. Acute liver failure including acetaminophen overdose. Med Clin North Am. 2008;92:761-794.
20. American Academy of Pediatrics Committee on Drugs. Acetaminophen toxicity in children. Pediatrics. 2001;108:1020-1024.
21. Dart RC, Erdman AR, Olson KR, et al. Acetaminophen
poisoning: an evidence-based consensus guideline for out-of-hospital
management. Clin Toxicol. 2006;44:1-18.
22. Heard KJ. Acetylcysteine for acetaminophen poisoning. N Engl J Med. 2008;359:285-292.
23. Ferner RE, Dear JW, Bateman DN. Management of paracetamol poisoning. BMJ. 2011;342:d2218.
24. Kuffner EK, Dart RC, Bogdan GM, et al. Effect of
maximal daily doses of acetaminophen on the liver of alcoholic patients:
a randomized, double-blind, placebo-controlled trial. Arch Intern Med. 2001;161:2247-2252.
25. Kuffner EK, Green JL, Bogdan GM, et al. The effect of
acetaminophen (four grams a day for three consecutive days) on hepatic
tests in alcoholic patients—a multicenter randomized study. BMC Med. 2007;5:13.
26. Rumack BH. Acetaminophen misconceptions. Hepatology. 2004;40:10-15.
27. Christophersen AB, Levin D, Hoegberg LC, et al.
Activated charcoal alone or after gastric lavage: a simulated large
paracetamol intoxication. Br J Clin Pharmacol. 2002;53;312-317.
28. Sato RL, Wong JJ, Sumida SM, et al. Efficacy of
super-activated charcoal administration late (3 hours) after
acetaminophen overdose. Am J Emerg Med. 2003;21:189-191.
29. Spiller HA, Winter ML, Klein-Schwartz W, et al.
Efficacy of activated charcoal administered more than four hours after
acetaminophen overdose. J Emerg Med. 2006;30:1-5.
30. Chyka PA, Seger D, Krenzelok EP, et al. Position paper: single-dose activated charcoal. Clin Toxicol. 2005;43:61-87.
31. Kozer E, Koren G. Management of paracetamol overdose: current controversies. Drug Safety. 2001;24:503-512.
32. Sandilands EA, Bateman DN. Adverse reactions associated with acetylcysteine. Clin Toxicol. 2009;47:81-88.
33. Hayes BD, Klein-Schwartz W, Doyon S. Frequency of
medication errors with intravenous acetylcysteine for acetaminophen
overdose. Ann Pharmacother. 2008;42:766-770.
34. June 29-30, 2009: Joint meeting of the Drug Safety and
Risk Management Advisory Committee with the Anesthetic and Life Support
Drugs Advisory Committee and the Nonprescription Drugs Advisory
Committee: FDA briefing material. Updated July 30, 2013.
www.fda.gov/downloads/AdvisoryCommittees/CommitteesMeetingMaterials/Drugs/DrugSafetyandRiskManagementAdvisoryCommittee/UCM164897.pdf.
Accessed December 15, 2013.
35. FDA Drug Safety Communication: FDA warns of rare but
serious skin reactions with the pain reliever/fever reducer
acetaminophen. August 1, 2013.
www.fda.gov/Drugs/DrugSafety/ucm363041.htm. Accessed December 16, 2013.
36. FDA Drug Safety Communication: Prescription
acetaminophen products to be limited to 325 mg per dosage unit; boxed
warning will highlight potential for severe liver failure. January 13,
2011. www.fda.gov/Drugs/DrugSafety/ucm239821.htm. Accessed December 16,
2013.
37. Krenzelok EP. Commentary: the FDA Acetaminophen
Advisory Committee meeting. What is the future of acetaminophen in the
United States? The perspective of a committee member. Clin Toxicol. 2009;47:784-789.
38. Pappas M, Bryan K. OTC industry announces voluntary
transition to one concentration of single-ingredient pediatric liquid
acetaminophen medicines. Consumer Health Care Products. May 11, 2011.
www.chpa.org/05_04_11_PedAcet.aspx. Accessed December 15, 2013.
39. Hornsby LB, Whitley HP, Hester EK, et al. Survey of
patient knowledge related to acetaminophen recognition, dosing, and
toxicity. J Am Pharm Assoc. 2010;50:485-489.
40. American Association of Poison Control Centers. www.aapcc.org. Accessed February 25, 2014.
To comment on this article, contact rdavidson@uspharmacist.com.





