US Pharm. 2016;41(11):7-11.
Acne vulgaris is one of the most common dermatologic conditions that affects nearly everyone at some point in their lifetime. Once thought as a condition only affecting teenagers, prevalence in adulthood has been increasing, especially in women 25 years of age and older.1 Almost 90% of all teenagers will report acne, and many will experience persistent acne into adulthood; by 40 years of age 1% of men and 5% of women will still have lesions.2 Despite the prevalence being higher in adolescents, the mean age for presentation to a physician is 24 years with 10% of office visits being made by patients between the ages of 35 and 44 years.3 Total direct costs for acne have been reported to exceed $3 billion annually.4
Although not life-threatening, acne may result in permanent scarring and long-lasting psycho-social effects, including low self-esteem, social anxiety, and depression. The avoidance of such consequences motivates patients to seek treatment; over $1 billion is spent on prescription medications annually, and the OTC market is estimated to be anywhere from 2 to 4 times this amount.5,6 Many patients will frequently seek OTC options prior to being evaluated by a physician for many reasons, including lower out-of-pocket costs, ease of accessibility, less irritation compared with prescription products, and perceived safety.1,6 There are many products available without a prescription for the treatment of acne, and pharmacists are in an ideal position to aid patients in the appropriate selection of a therapeutic regimen and provide education on the appropriate use.
Pathophysiology
Acne is a multifactorial inflammatory disease of the pilosebaceous duct, resulting in bacterial over-growth and inflammation. Four pathophysiologic processes have been identified in contributing to the formation of lesions2: 1) abnormal keratinocyte proliferation and desquamation; 2) androgen-driven increase in sebum production; 3) proliferation of Propionibacterium acnes; and 4) inflammatory mediators.
The pilosebaceous unit consists of a hair follicle and surrounding sebaceous glands. These units can be found all over the dermis except for the palms and soles; the highest concentrations can be found on the face, upper back, and chest area.2 An increased production of androgen, usually coinciding with the onset of puberty, causes abnormal epithelial desquamation and hyperkeratin-ization, along with an increase in sebum secretion by the sebaceous glands. The accumulation of sebum, epithelial cells, and keratin within the follicle eventually obstructs the follicle, leading to the formation of a keratin plug and follicle swelling.2,7 This results in the formation of a microcomedone, the primary precursor lesion of acne that is not visible to the naked eye.2,7 With the continued swelling of the follicle and enlargement of the keratin plug, a visible comedone will eventually form. Two types of comedones can emerge: a comedone with a widely dilated opening (open comedone or blackhead) or a comedone with a microscopic opening (closed comedone or whitehead).7
Increased sebum production can result in the proliferation of P acnes, a gram-positive anaerobe that is part of the normal skin flora. This leads to release of chemical mediators that promote inflammation.2,7,8 The formation of more severe acne lesions such as papules, pustules, nodules, or cysts develop when comedones rupture and contents of the pilosebaceous unit spill out into the surrounding area.2,8
Risk Factors and Clinical Characteristics
Acne appears earlier in girls, but more boys are affected during the adolescence years; the average age for the onset of acne is 11 years in girls, affecting up to 82%, and 12 years in boys, affecting up to 95%. Recently, there has been a rise in the appearance of acne in those as young as 8 or 9 years of age. This increase at such a young age has been attributed to the decreasing age of puberty onset.8 Adult acne occurs more commonly in women.
Ethnicity and genetics may influence acne prevalence and severity. A positive family history of acne can greatly increase someone’s risk. Scarring and hyperpigmentation occur more commonly in those with darker pigmented skin. Several modifiable factors have also been associated with increasing acne risk. These include cigarette smoking, a diet high in dairy and glycemic carbohydrate intake, hot and humid conditions, local irritation or friction (occlusive clothing or repeated scrubbing), use of oil-based skin and hair products, prolonged sweating, and emotional stress.2,8,9
A patient’s medication history should also be taken into consideration when evaluating risk factors for acne. Drugs that can increase an individual’s risk include anti-epileptics, corticosteroids, hormones, calcineurin blockers, phenytoin, carbamazepine, lithium, aripiprazole, trazodone, and haloperidol.10
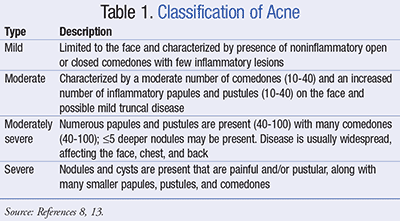
Acne is characterized by the presence of lesions most commonly on the face, neck, chest, or back. These lesions include noninflammatory open or closed comedones and inflammatory lesions characterized as papules, pustules, nodules, and cysts. Currently, there is no single accepted universal grading system. In general, acne can be classified as mild, moderate, or severe (TABLE 1).8,13
Prevention
Patients should avoid any contributing factors that may increase their risk of developing acne. In addition, basic facial care with twice-daily washings using a mild noncomedogenic soap is recommended. Patients should also avoid oily skin products, touching their face, and manipulating or picking at the lesions.
Treatment
Acne is usually a self-limiting dis-ease, but many agents are available to help minimize symptoms and reduce scarring, which can lead to improvements in quality of life. Management of acne can be divided into two phases: the initial treatment phase, which aims at reducing the severity in a relatively short period of time, and the maintenance phase, which aims to prevent recurrence.11 Acne treatment may be required for a few months to several years. Initial symptom improvement may take up to 8 weeks. It is important to educate patients about the importance of continual use and that symptoms may actually appear to worsen during the first few weeks of treatment.
There is an array of therapies available OTC for the management of acne. They include topical products, mechanical treatments, essential oils, and vitamins (TABLE 2).1,6 Product choice is dependent upon patient age, preference, skin type, site of involvement, and severity of disease.

Topical therapy is the standard of care in mild-to-moderate disease.12 There are many topical nonprescription products available for the management of acne. Topical agents are only active where and when they are applied. Topical therapy can be used as monotherapy or in combination with other topical therapies and/or oral agents for both initial control and maintenance of acne.12
Benzoyl Peroxide: Benzoyl peroxide has been used in the management of acne since the late 1970s. It has bactericidal activity against P acnes and is most commonly used as a first-line treatment.12 Response is rapid and can be seen as early as 5 days after the start of therapy.13 No bacterial resistance has been reported with this agent, making it an ideal adjunct to topical or oral prescription antibiotic therapy.6,12
Benzoyl peroxide remains the most commonly purchased OTC acne products.6 It is available in a variety of dosage forms, including creams, lotions, gels, foams, and washes and in concentrations ranging from 2.5% to 10%. It can be used as a leave-on or wash-off agent; however, reduction of P acnes is more effective with leave-on products.6 Some studies have shown no differences in effectiveness between the various concentrations, but there were increases in skin irritation.2,6 Recommend a lower concentration, water-based, wash-off product to patients with sensitive skin. Newer products are often combined with a moisturizer to decrease skin redness and irritation. Patients should be counseled on the importance of avoiding excessive sun exposure and use of sunscreen and protective clothing. In addition, patients should be warned about the possibility of staining and bleaching of fabric and hair.
Hydroxy Acids: Hydroxy acids are classified into two categories: alpha-hydroxy acids (AHAs) and beta-hydroxy acids (BHAs). The two types of AHAs found in OTC products are glycolic acid from sugar cane and lactic acid from milk. They are available in concentrations up to 10% and can be found as washes, creams, lotions, and peel kits. Glycolic acid used in the form of a chemical peel may be useful in the treatment of mild scarring and mild improvement in noninflammatory lesions.12,14
Salicylic acid is the only BHA used in dermatologic practice. It is a comedolytic agent but is considered less potent than benzoyl peroxide; it should be considered for use in patients who cannot tolerate benzoyl peroxide or in combination with other more effective medications.6 It is available in many OTC acne products in concentrations ranging from 0.5% to 2%. When used in concentrations >2%, it has been associated with local skin peeling.6 Topical salicylic acid should be avoided in patients with diabetes or poor blood circulation.
Sulfur: Sulfur has been used medicinally for hundreds of years. It has antifungal, bacteriostatic, and mild keratolytic properties.1,6 It is not effective as monotherapy and is usually combined with other products, including benzoyl peroxide, salicylic acid, and resorcinol.6 Side effects are rare but may be associated with mild irritation and sensitization. Malodor limits its use.
Other Agents: Tea tree oil is an essential oil that has broad antimicrobial and antifungal properties.1 Two studies have demonstrated tea tree oil’s efficacy in treating acne, although when compared to benzoyl peroxide, it had a slower onset of action.15,16 Nicotinamide is a derivative of niacin that is used both orally and topically in the treatment of acne. Topical nicotinamide 4% has been shown to be as effective as clindamycin gel 1%, but further studies are needed to assess nicotinamide’s role in the treatment of acne. Retinol is naturally occurring vitamin A. It is transformed into several metabolites, including retinoic acid. Theoretically, topical retinol should be beneficial in the treatment of acne, but no studies have been performed demonstrating this effect. Zinc is bacteriostatic against P acnes and may be effective in the treatment of severe and inflammatory acne.6 Gastrointestinal effects associated with oral zinc may limit its usefulness.
Adapalene Gel: In July 2016, the FDA approved Differin Gel 0.1% (adapalene) for OTC use in those 12 years of age and older.17 This approval made Differin the first prescription acne medication to go OTC since the 1980s. Patients will now have access to a new, safe, and effective OTC option, which is important since acne is so frequently occurring. Differin is also available as a 0.3% gel; however, this strength still requires a prescription.17
Differin is a type of retinoid, a class of medications commonly used to treat acne. Differin attaches to skin-cell DNA and modifies the production of enzymes needed for creation of new skin cells. In addition, it counteracts the processes of hyperkeratinization and excessive growth in pore linings, and desensitizes the skin to inflammation.18 These mechanisms make it harder for dead skin cells to accumulate inside pores, which allows them to drain. Differin is lipophilic, allowing the medication to penetrate follicles quickly. It is important to note that Differin does not cure acne. It aids in ceasing the formation of new breakouts, so hygienic skin care routines should also be implemented.18
Differin exhibits no systemic effects and is overall a gentler alternative to powerful acne medications. The clinical development program for Differin consisted of five studies that assessed safety and efficacy in treating patients with mild-to-moderate acne severity.19 Efficacy endpoints were met, and superiority with treatment of Differin compared to vehicle was confirmed with reduction of total lesion counts from baseline reported between 30% and 50% by week 12 of treatment. In addition, some studies have shown regression of acne as early as 1 week after starting Differin therapy.19
Although there are many acne treatments, specifically in the retinoid class, there are reasons why Differin was the first to go OTC. Perhaps the most distinct difference between Differin and other retinoids is its safety profile. Differin is very chemically stable and has been shown to be extremely tolerable compared to other medications in its class.20 This feature allows Differin to be combined with other acne treatments, such as benzoyl peroxide and clindamycin. In addition, Differin is safe for use in pregnant women. Many other retinoids cause birth defects, but no studies have shown this to be true with Differin when applied topically.20
Differin has been an FDA-approved acne medication since 1996; however, since it is now available without a prescription, it is important to counsel patients on proper usage. Differin increases photosensitivity; patients may get sunburned more easily, so it is important to be mindful of sunlight exposure. Sunlamps and tanning beds should also be avoided. Differin is meant for once-daily topical use only, and should not be applied to open lesions, cuts, scrapes, eczema, or damaged skin. The most common side effects of Differin were dry skin, itching, and skin discomfort. Patients should stop use and consult a physician if irritation becomes severe, if there is no improvement of acne in 3 months with daily use, or if an allergic reaction occurs.18
Conclusion
Acne is a chronic condition affecting both adolescents and adults. It is easily recognizable and self-treated, so many patients will approach the pharmacist regarding appropriate treatment recommendations. Until now, benzoyl peroxide has been the most commonly used and effective OTC product to treat acne. With the recent Rx-to-OTC switch of Differin, patients now have another acne treatment option to choose from that is effective and recommended for all cases of acne, except when oral retinoids are used.8 Pharmacists will be instrumental in ensuring the appropriate use of this product in the treatment of acne.
PATIENT INFORMATION

What Causes Acne Vulgaris?
Acne occurs when skin follicles (pores) become blocked or inflamed. Sebum is an oily substance that is made by the sebaceous glands that helps keep hair and skin moisturized. Hormone changes during the teenage years cause the body to make more of this oily substance, clogging the follicles. A pimple eventually forms. Bacteria can get inside the follicle or oil gland and cause redness, swelling, and pus.
Many factors can bring on or worsen acne. These include:
- Family history
- Cigarette smoking
- Hot and humid conditions
- Irritation or friction caused by wearing tight clothes
- Using oil-based skin and hair products
- Prolonged sweating
- Emotional stress
- Certain medications.
What Can I Do to Prevent Acne or Make It Better?
There are several things you can do to help prevent acne and lessen breakouts.
- Wash your face at least twice a day with a gentle nondrying cleanser. Avoid scrubbing your face because this can make the condition worse.
- Use noncomedogenic and oil-free cosmetics, moisturizers, and sunscreens.
- Do not touch, pop, squeeze, or pick at pimples.
What Can I Do to Treat my Acne?
There are many products available to effectively treat acne. Topical agents are most commonly used to treat mild cases. Many of these products are available without a prescription and include benzoyl peroxide, salicylic acid, and most recently, Differin (adapalene gel 0.1%).
Some people may have a reaction to these products. Try a small amount on a limited area first before applying to larger areas. Most topical products can cause local irritation and dryness, which can be prevented by using mild moisturizing soaps and lotions.
Other products require a prescription. Topical antibiotics may be prescribed alone or in combination with benzoyl peroxide. Other topical products include tretinoin and adapalene gel 0.3%. For more severe cases of acne, oral medications may be prescribed, which include isotretinoin and oral antibiotics used in combination with topical products. Women who take isotretinoin must follow strict rules to avoid pregnancy because the drug can cause severe birth defects.
What Can I Expect From Treatment?
Sometimes acne will get worse during the first few weeks of treatment. It will get better as treatment is continued, although it may take up to 8 weeks to see improvement. If you do not notice improvement after 3 months of use, or if you have moderate or severe acne, speak with your primary care provider or dermatologist about treatment options. Once acne is cleared, treatment should be continued to prevent future breakouts.
Remember, if you have questions, Consult Your Pharmacist.
REFERENCES
1. Decker A, Graber EM. Over-the-counter acne treatments: a review. J Clin Aesthetic Dermatol. 2012;5(5):32-40.
2. Dawson AL, Dellavalle RP. Acne vulgaris. BMJ. 2013;346:f2634.
3. McConnell RC, Fleischer AB, Williford PM, Feldman SR. Most topical tretinoin treatment is for acne vulgaris through the age of 44 years: an analysis of the National Ambulatory Medical Care Survey, 1990-1994. J Am Acad Dermatol. 1998;38(2 Pt 1):221-226.
4. Bhate K, Williams HC. Epidemiology of acne vulgaris. Br J Dermatol. 2013;168(3):474-485.
5. Bickers DR, Lim HW, Margolis D, et al. The burden of skin diseases: 2004 a joint project of the American Academy of Dermatology Association and the Society for Investigative Dermatology. J Am Acad Dermatol. 2006;55(3):490-500.
6. Bowe WP, Shalita AR. Effective over-the-counter acne treatments. Semin Cutan Med Surg. 2008;27(3):170-176.
7. Mancini AJ. Incidence, prevalence, and pathophysiology of acne. John Hopkins Adv Stud Med. 2008;8(4):100-105.
8. Knutsen-Larson S, Dawson AL, Dunnick CA, Dellavalle RP. Acne vulgaris: pathogenesis, treatment, and needs assessment. Dermatol Clin. 2012;30(1):99-106.
9. Williams HC, Dellavalle RP, Garner S. Acne vulgaris. Lancet. 2012;379(9813):361-372.
10. Scheinfeld N. Drug-induced acne and acneiform eruptions: a review. Dermatologist. 2009;17(8). www.the-dermatologist.com/content/drug-induced-acne-and-acneiform-eruptions-a-review. Accessed October 1, 2016.
11. Tan X, Al-Dabagh A, Davis S, et al. Medication adherence, healthcare costs and utilization associated with acne drugs in Medicaid enrollees with acne vulgaris. Am J Clin Dermatol. 2013;14(3):243-251.
12. Zaenglein AL, Pathy AL, Schlosser BJ, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5):945-973.e33.
13. James WD. Clinical practice. Acne. N Engl J Med. 2005;352(14):1463-1472.
14. Thiboutot D, Gollnick H, Bettoli V, et al. New insights into the management of acne: an update from the Global Alliance to Improve Outcomes in Acne group. J Am Acad Dermatol. 2009;60(5 suppl):S1-S50.
15. Bassett IB, Pannowitz DL, Barnetson RS. A comparative study of tea-tree oil versus benzoylperoxide in the treatment of acne. Med J Aust. 1990;153(8):455-458.
16. Enshaieh S, Jooya A, Siadat AH, Iraji F. The efficacy of 5% topical tea tree oil gel in mild to moderate acne vulgaris: a randomized, double-blind placebo-controlled study. Indian J Dermatol Venereol Leprol. 2007;73(1):22-25.
17. FDA approves Differin Gel 0.1% for over-the-counter use to treat acne. FDA news release. July 8, 2016. www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm510362.htm. Accessed October 1, 2016.
18. Differin (adapalene) gel 0.3% package insert. Fort Worth, TX: Galderma Laboratories; December 2013. www.galdermausa.com/PI/DifferinGel03PI.pdf. Accessed October 1, 2016.
19. FDA Nonprescription Drugs Advisory Committee briefing document: Differin Gel adapalene 0.1% topical gel. April 15, 2016. Galderma. www.fda.gov/downloads/AdvisoryCommittees/CommitteesMeetingMaterials/Drugs/NonprescriptionDrugsAdvisoryCommittee/UCM495797.pdf. Accessed October 1, 2016.
20. Rolewski SL. Clinical review: topical retinoids. Dermatol Nurses Assoc. 2003;15(5):447-450, 459-465.
To comment on this article, contact rdavidson@uspharmacist.com.





