US Pharm. 2015;40(8):HS2-HS6.
ABSTRACT: Acute kidney injury is characterized by a rapid loss in kidney function with or without changes in urine output. The severity of the condition ranges from mild to severe, and the type of acute kidney injury is based upon the causative agent. A patient history, complete physical examination, and basic laboratory tests are part of the initial diagnosis. Further investigation, including imaging studies and a biopsy, may be required if a diagnosis cannot be established. The initial management of all patients with acute kidney injury should be supportive and should aim to prevent further injury. Following this, the patient may need restoration of cardiac function, replenishment of electrolyte volumes, and—in severe cases—renal replacement therapy.
Acute kidney injury, also known as acute renal failure, is a condition characterized by the rapid loss (within 48 hours) of the excretory function of the kidneys based upon an elevation in serum creatinine and urea concentrations (both of which are end products of nitrogen metabolism). Patients may be nonoliguric (having normal urine output), oliguric (urine output reduced to <400 mL/day), or even anuric (urine output <100 mL/day). In severe cases, renal replacement therapy may be required.1-3
Acute kidney injury has an estimated incidence of two to three cases per 1,000 persons, which is higher than the incidence of conditions such as acute lung injury and severe sepsis.4 Furthermore, the incidence of acute kidney injury is increasing in community and hospital settings.1,4,5 It has been shown that 7% of hospitalized patients and as many as 67% of patients in the ICU develop acute kidney injury.6 Since acute kidney injury is associated with a high incidence of complications and mortality rates can range from 25% and 80%, it is vital that the condition be detected early and managed appropriately.7-9
CLASSIFICATION
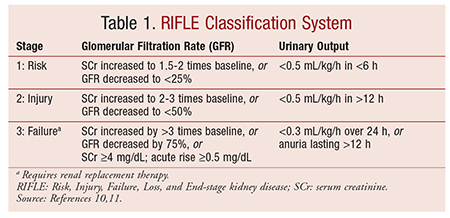
The Risk, Injury, Failure, Loss, and End-stage kidney disease (RIFLE) classification system divides acute kidney injury into three stages based upon the change in serum creatinine level, the change in urine output, or the need for renal replacement therapy (TABLE 1).10,11
CAUSES
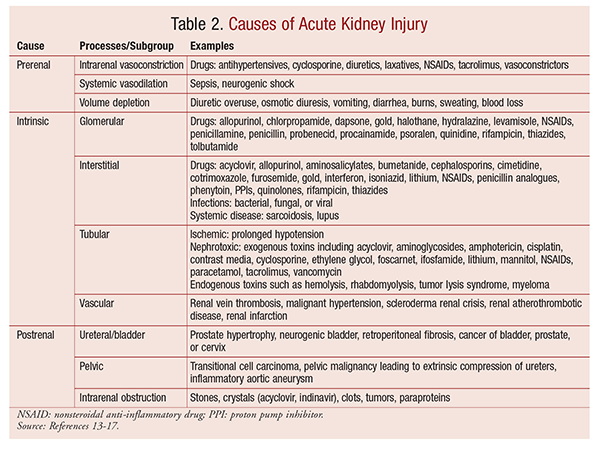
The causes of acute kidney injury may be divided into three classes: prerenal, intrinsic, and postrenal (TABLE 2). While this classification seems quite simple in theory, the causes can sometimes overlap. Healthy kidneys autoregulate their blood supply over a wide range of perfusion pressures, so minor changes in perfusion pressure do not cause any major disruption. However, in disease states, the autoregulatory process may be defective or be reset. In such cases, even the slightest change in perfusion pressure can have drastic effects.12
Prerenal Causes
Prerenal causes of acute kidney injury are processes in which the underlying kidney function may be normal, but the effective arteriolar blood volume is reduced, depriving the kidneys of blood flow. Prerenal factors are the leading cause of acute kidney injury in the community, comprising about 70% of cases.13 The processes can be further divided into intrarenal vasoconstriction, systemic vasodilation, and volume depletion (TABLE 2).14,15
Intrinsic Causes
Intrinsic factors are important causes of acute kidney injury that can be subdivided into four categories based upon the component of the kidney that is primarily affected. These categories are glomerular, interstitial, tubular, and vascular.15,16
Tubular: Acute tubular necrosis, the most common type of intrinsic acute kidney injury in hospitalized patients, is typically caused by ischemia or nephrotoxicity.16 While tubular cells usually can regulate their processes and survive in an ischemic environment, factors that reduce the supply of metabolites to these cells can cause acute tubular necrosis. In most cases, patients with acute tubular necrosis will experience a reduction in urine output.15 Damaged tubular cells slough off the basement membrane and obstruct the tubules, and unchanged glomerular filtrate leaks back into the capillaries. Furthermore, there is a reduction in renal blood flow, and blood is diverted away from the cortex toward the medulla.15
Acute tubular necrosis does not improve with adequate repletion of intravascular volume and blood flow to the kidneys. However, ischemic and nephrotoxic acute tubular necrosis will resolve over time, although some patients may require temporary renal replacement therapy.16
Glomerular: Glomerular causes of acute kidney injury are the result of immune-mediated inflammation of the blood vessels and glomeruli.15,16 Glomerulonephritis is diagnosed based on a thorough history, physical examination, and urinalysis. This step is usually followed by a renal biopsy to confirm the diagnosis before therapy with immunosuppressive or cytotoxic medications is started.16
Interstitial: Since acute interstitial nephritis is usually caused by drugs, a thorough patient history is vital to establish a diagnosis. Eosinophiluria occurs in most patients with drug-induced interstitial nephritis. Corticosteroids have been used to manage acute interstitial nephritis, along with the removal of the offending agent.17
Vascular: Vascular injuries are acute events involving the renal arteries or veins. Blockage causes an inflammatory reaction that obliterates the lumen. The most common type of vascular acute kidney injury is renal atherothrombolic disease, which is thought to be caused by arterial catheterization or vascular surgery.14 While physical examination and history are useful in working up a diagnosis, imaging is usually required to confirm it.16
Postrenal Causes
Postrenal causes of acute kidney injury are usually the result of obstructed urinary flow. These causes may be categorized according to the site at which the blockage occurs; i.e., ureteral, intrarenal, or pelvic.16
CLINICAL PRESENTATION
The clinical presentation of acute kidney injury varies with the cause and severity of renal injury and associated diseases. Most mild-to-moderate cases are asymptomatic and can be identified only through laboratory testing. Severe cases may present with listlessness, confusion, fatigue, anorexia, nausea, vomiting, weight gain, edema, hypertension, and hyperkalemia.18 Patients may be oliguric, anuric, or nonoliguric. Other possible presentations include uremic encephalopathy, anemia, or bleeding caused by uremic platelet dysfunction.
DIAGNOSIS
A thorough history and physical examination with a focus on the patient’s volume statistics are useful in establishing a diagnosis.16
Risk factors for acute kidney injury that may be evident in the history include hypertension, chronic heart failure, diabetes, multiple myeloma, chronic infections, myeloproliferative disorder, connective-tissue disorder, and autoimmune disease. The patient’s history will also highlight any nephrotoxic medications that might lead to poor renal perfusion or directly impair renal function. Laboratory tests that can assess the etiology of acute kidney disease include CBC, urinalysis, and measurement of serum creatinine level and fractional excretion of sodium. Renal imaging is particularly useful in identifying a renal obstruction. If both pre- and postrenal causes of acute kidney injury have been excluded and the cause of intrinsic renal injury is unclear, then a renal biopsy may be performed.15,16
MANAGEMENT
The management of patients with acute kidney injury requires close collaboration between healthcare professionals. While it is primarily supportive, management should also be directed at halting or reversing the decline in renal function.16 All patients with acute kidney injury should be hospitalized, unless the condition is mild and clearly results from an easily reversible cause. At this stage, it is important to ensure adequate renal perfusion by achieving and maintaining hemodynamic stability and avoiding hypovolemia.
Nephrotoxic insults should be removed through dialysis or adsorption, and causative medications should be discontinued. In the case of essential lifesaving medications, the dosage should be reviewed and reduced, if possible. In some cases, specific antidotes, such as the use of N-acetylcysteine for acetaminophen overdose, may be required.15
Fluid resuscitation in patients with intravascular volume depression may be performed using isotonic rather than hyperoncotic solutions.19 The aim should be to obtain a mean arterial pressure of >65 mmHg. If this cannot be achieved with volume repletion, vasopressors may be required, particularly in patients with persistent hypotension.20 Since renal-dose (low-dose) dopamine has demonstrated poor outcomes in various studies, its use is no longer recommended.21,22 Cardiac function varies in patients and can be managed appropriately with positive inotropes, or afterload and preload reduction. Electrolytes should be monitored regularly to detect hyperkalemia, hyperphosphatemia, hypermagnesemia, hyponatremia, hypernatremia, or metabolic acidosis. If any of these complications arise, appropriate measures must be taken to normalize electrolytes.
Severe hyperkalemia can lead to life-threatening cardiac arrhythmias and is therefore considered a medical emergency. Hyperkalemia should be treated immediately if serum potassium levels are >6.5 mmol/L or if there are any changes in the patient’s ECG reading. Treatment should begin with stabilization of cardiac myocytes and be immediately followed by reduction of potassium concentrations in the plasma, removal of excess potassium from the body, and prevention of further accumulation of potassium.23
An infusion of calcium gluconate antagonizes the physiological effects of hyperkalemia, but does not lower the serum potassium levels. A bolus of 10 to 20 mL of 10% calcium gluconate produces an effect within 1 to 3 minutes that lasts up to 1 hour.24 The plasma potassium concentrations can be reduced by various means, including insulin and beta-adrenergic blockers.
Insulin indirectly activates the sodium/potassium–adenosine triphosphate (Na+/K+-ATPase) system and therefore promotes cellular potassium uptake. This action is thought to occur through the activation of the Na+/H+ (sodium/hydrogen) channels, which increases the intracellular Na+ levels.25 It is important to add glucose to the insulin to prevent hypoglycemia, unless the patient is hyperglycemic.26 Ten units of fast-acting soluble insulin in 50 mL of 50% dextrose infused over 10 to 20 minutes begin to exert an effect within 15 to 30 minutes. The effect lasts 4 to 6 hours, and plasma potassium levels are reduced by 0.65 to 1.0 mmol/L.
Beta-adrenergic blockers such as salbutamol bind to beta2 receptors and activate Na+/K+-ATPase, thereby increasing cellular uptake. Salbutamol may be given as either a nebulized solution or an IV infusion, but higher dosages than those given for bronchospasm are needed to produce an effect similar to that of insulin for the reduction of plasma potassium concentration. An IV infusion of 0.5 mg or a nebulized solution of 10 to 20 mg produces an effect in about 30 minutes and is effective for 2 to 4 hours.23
In patients with exclusive prerenal failure, increased renal potassium excretion is sufficient to restore potassium levels to normal. In other patients, ion-exchange resins or hemodialysis may be required to remove potassium. Ion-exchange resins bind to potassium in the gastrointestinal tract in exchange for calcium or sodium, promoting excretion of potassium in the stool. An oral dosage of 15 g of calcium polystyrene sulfonate or sodium polystyrene sulfate three times daily will produce an effect within 2 to 3 hours. Every gram of resin removes 0.5 to 1.0 mmol/L of potassium, and the effect lasts for 4 to 6 hours. An osmotic laxative, such as 10 mL lactulose, is added to reduce the risk of constipation. Hemodialysis definitively removes potassium from the body, and maximal removal occurs in the first hour.23
Diuretics have been indicated to manage volume overload; however, they should not be used in the absence of volume overload, since they do not improve morbidity, mortality, or renal outcomes.27 Renal replacement therapy is reserved for patients with severe hyperkalemia, intractable fluid overload, or metabolic acidosis.
CONCLUSION
Acute kidney disease, a common disorder in hospitalized patients, is associated with significant mortality and morbidity. Since drugs are a common cause of acute kidney disease, pharmacists must be involved in the management of patients with acute kidney disease as part of a multidisciplinary healthcare team. Pharmacists play a key role in advising on appropriate drug therapy for management of patients with acute kidney disease.
REFERENCES
1. Nash K, Hafeez A, Hou S. Hospital-acquired renal insufficiency. Am J Kidney Dis. 2002;39:930-936.
2. Thadhani R, Pascual M, Bonventre JV. Acute renal failure. N Engl J Med. 1996;334:1448-1460.
3. Klahr S, Miller SB. Acute oliguria. N Engl J Med. 1998;338:671-675.
4. Hoste EA, Schurgers M. Epidemiology of acute kidney injury: how big is the problem? Crit Care Med. 2008;36(suppl 4):S146-S151.
5. Hsu CY, McCulloch CE, Fan D, et al. Community-based incidence of acute renal failure. Kidney Int. 2007;72:208-212.
6. Bellomo R, Kellum JA, Ronco C. Acute kidney injury. Lancet. 2012;25;380:756-766.
7. Ympa YP, Sakr Y, Reinhart K, Vincent JL. Has mortality from acute renal failure decreased? A systematic review of the literature. Am J Med. 2005;118:827-832.
8. Gruberg L, Weissman NJ, Pichard AD, et al. Impact of renal function on morbidity and mortality after percutaneous aortocoronary saphenous vein graft intervention. Am Heart J. 2003;145:529-534.
9. Uchino S, Kellum JA, Bellomo R, et al; Beginning and Ending Supportive Therapy for the Kidney (BEST Kidney) Investigators. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA. 2005;294:813-818.
10. Bellomo R, Ronco C, Kellum JA, et al. Acute renal failure—definition, outcome measures, animal models, fluid therapy and information technology needs: the Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group. Crit Care. 2004;8:R204-R212.
11. Mehta RL, Kellum JA, Shah SV, et al. Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care. 2007;11:R31.
12. Christensen PK, Hansen HP, Parving HH. Impaired autoregulation of GFR in hypertensive non-insulin dependent diabetic patients. Kidney Int. 1997;52:1369-1374.
13. Kaufman J, Dhakal M, Patel B, Hamburger R. Community-acquired acute renal failure. Am J Kidney Dis. 1991;17:191-198.
14. Holley JL. Clinical approach to the diagnosis of acute renal failure. In: Greenberg A, Cheung AK, eds. Primer on Kidney Diseases. 5th ed. Philadelphia, PA: National Kidney Foundation; 2009:278.
15. Ashley C, Holt S. Acute renal failure. Pharm J. 2001;266:625-628.
16. Rahman M, Shad F, Smith MC. Acute kidney injury: a guide to diagnosis and management. Am Fam Physician. 2012;86:631-639.
17. González E, Gutiérrez E, Galeano C, et al; Grupo Madrileño De Nefritis Intersticiales. Early steroid treatment improves the recovery of renal function in patients with drug-induced acute interstitial nephritis. Kidney Int. 2008;73:940-946.
18. Meyer TW, Hostetter TH. Uremia. N Engl J Med. 2007;357:1316-1325.
19. Schortgen F, Lacherade JC, Bruneel F, et al. Effects of hydroxyethylstarch and gelatin on renal function in severe sepsis: a multicentre randomised study. Lancet. 2001;357:911-916.
20. Brochard L, Abroug F, Brenner M, et al. An official ATS/ERS/ESICM/SCCM/SRLF statement: prevention and management of acute renal failure in the ICU patient: an international consensus conference in intensive care medicine. Am J Respir Crit Care Med. 2010;181:1128-1155.
21. Friedrich JO, Adhikari N, Herridge MS, Beyene J. Meta-analysis: low-dose dopamine increases urine output but does not prevent renal dysfunction or death. Ann Intern Med. 2005;142:510-524.
22. Bellomo R, Chapman M, Finfer S, et al. Low-dose dopamine in patients with early renal dysfunction: a placebo controlled randomised trial. Lancet. 2000;356:2139-2143.
23. Fry AC, Farrington K. Management of acute renal failure. Postgrad Med J. 2006;82:106-116.
24. Kim HJ, Han SW. Therapeutic approach to hyperkalaemia. Nephron. 2002;92(suppl 1):33-40.
25. Throssell D. Hyperkalaemia. In: Glynne P, Allen A, Pusey C, eds. Acute Renal Failure in Practice. London, England: Imperial College Press; 2002:156-162.
26. Weiner ID, Linas SL, Wingo CS. Disorders of potassium metabolism. In: Johnson RJ, Feehally J, eds. Comprehensive Clinical Nephrology. 2nd ed. London, England: Mosby; 2003:109-121.
27. Ho KM, Sheridan DJ. Meta-analysis of frusemide to prevent or treat acute renal failure. BMJ. 2006;333:420.
To comment on this article, contact rdavidson@uspharmacist.com.






