ABSTRACT: Acute pericarditis is the most common form of pericardial disease that results in the need for empirical anti-inflammatory treatment. Aspirin and other nonsteroidal anti-inflammatory drugs, prednisone, and colchicine are the mainstays of therapy. These agents are used for symptom control and to reduce the risk of further complications, including recurrent pericarditis, constrictive disease, and cardiac tamponade. Strong evidence has emerged for the use of colchicine to treat and prevent recurrent pericarditis. Therapies for acute pericarditis carry their own risks of adverse effects. Therefore, pharmacists play a vital role in educating patients, improving their care, and promoting the safe and effective use of these medications.
US Pharm. 2014;39(4):52-57.
Acute pericarditis (inflammation of the pericardial sac) is the most common pericardial disease, accounting for 5% of emergency department admissions in patients presenting with nonischemic chest pain.1,2 In the United States, most cases of acute pericarditis in immunocompetent hosts are predominantly of idiopathic or viral origin.1,3 Other causes include radiation; malignancies; trauma; infectious diseases (e.g., mycoplasmal, fungal, bacterial); drugs (e.g., procainamide, isoniazid, hydralazine); autoimmune disorders (e.g., lupus, rheumatoid arthritis, vasculitis, scleroderma, sarcoidosis, inflammatory bowel disease); metabolic disorders (hypothyroidism, uremia, ovarian hyperstimulation syndrome); and cardiac disorders (early infarction, postcardiac injury, myocarditis, dissecting aortic aneurysm).2
High-risk patients should be hospitalized, as they have a specific etiology and are more likely to experience short-term complications.4,5 Indicators of poor prognosis include fever, leukocytosis, suspected cardiac tamponade, large pericardial effusion, immunocompromised state, history of warfarin treatment, acute trauma, refractoriness to a 7-day course of nonsteroidal anti-inflammatory drugs (NSAIDs), and elevated cardiac troponin.4,5 Complications such as cardiac tamponade and constrictive pericarditis occur more frequently in patients with an identified etiology and rarely in those with idiopathic or viral causes.2,6
Recurrent pericarditis occurs in 10% to 30% of pericarditis patients, usually weeks to months later.2,7 Recurrent pericarditis develops at least 6 weeks after medications for the initial or previous attack are discontinued, whereas incessant pericarditis occurs within the 6-week period immediately following discontinuation. Recurrent pericarditis is most commonly idiopathic, viral, or autoimmune in origin.8 Risk factors for recurrence are not well defined; however, a favorable response to initial treatment of the index case of pericarditis with aspirin or other NSAIDs is associated with lower risk, whereas initial glucocorticoid use is associated with a higher risk.9-11 Fortunately, most patients with recurrence experience only one to two more attacks, and severe complications are rare.10-12
Clinical Evaluation
Acute pericarditis presents in a variety of ways, depending upon the underlying etiology. Pericarditis with an infectious etiology may be preceded by signs and symptoms of infection; by flulike symptoms, for a viral etiology; or, for an autoimmune or malignancy etiology, by exacerbation of symptoms of the underlying disorder. The major clinical signs and symptoms include ECG changes with recent widespread ST elevation or PR depression, pericardial friction rub, sharp or stabbing chest pain, fatigue, breathlessness, and palpitations.13 Patients with pericarditis often present with pericardial effusion. Such patients should be closely monitored for signs of cardiac tamponade, a potentially lethal complication of pericarditis.
During the course of pericarditis, approximately 85% of patients have an audible friction rub upon physical examination. This is a high-pitched scratchy or squeaky sound best heard at end expiration with the patient leaning forward.3 Chest pain associated with acute pericarditis is usually sudden in onset, retrosternal, and pleuritic in that it is exacerbated by inspiration. The pain may lessen when the patient leans forward or assumes the upright position.
Classically, the 12-lead ECG in patients with acute pericarditis shows widespread upward concave ST-segment elevation and PR-segment depression. There are four levels of ECG abnormalities: stage I, diffuse ST-segment elevation and PR-segment depression; stage II, normalization of the ST and PR segments; stage III, widespread T-wave inversions; and stage IV, normalization of T waves.3
Echocardiograms frequently are normal in patients with the clinical syndrome of acute pericarditis, unless there is an associated pericardial effusion. The finding of pericardial effusion supports diagnosis, but its absence does not exclude acute pericarditis. Chest radiographs are usually normal in patients with acute pericarditis, unless there is a large effusion with an accumulation of >200 mL of fluid.1
Markers of inflammation, such as WBC count, erythrocyte sedimentation rate, and C-reactive protein concentration, are usually elevated. These findings are nonspecific to pericarditis. Serum cardiac troponin I levels also have been shown to be elevated in some patients.3
Treatment Overview
The treatment of acute pericarditis should be guided by the underlying cause. Ninety percent of acute pericarditis cases are idiopathic or viral, making NSAIDs, prednisone, and colchicine the foundations of therapy.3,14-16 Drug therapy is empirical and targets symptom control.
NSAID therapy is initiated empirically for idiopathic pericarditis and generally leads to symptom resolution within 2 weeks.4 NSAIDs other than aspirin should be avoided in patients who develop postinfarction pericarditis (Dressler syndrome), owing to these agents’ inhibitory effects on scar-tissue formation and the increased risk of infarction-zone thinning.17-20 In the case of Dressler syndrome, high-dose (HD) aspirin is preferred. Indomethacin should be avoided in elderly patients and in patients with coronary artery disease, owing to its negative impact on coronary flow; ibuprofen is the preferred NSAID.21 Subsequent tapering of these agents should be considered to reduce the risk of recurrence.14
Corticosteroid therapy has resulted in rapid symptom control; however, it has been linked to higher rates of recurrent pericarditis.11,14,22,23 The use of corticosteroids is also limited by some other systemic adverse effects (AEs) associated with long-term corticosteroid therapy, thereby rendering intrapericardial instillation of a nonabsorbable steroid a viable therapeutic option.24 Corticosteroids are reserved for patients who have failed NSAIDs. In Dressler syndrome, corticosteroids should be reserved only for refractory symptoms, because these agents can delay myocardial healing.14 Treatment can last up to 4 weeks, so tapering is recommended. To prevent recurrence, NSAIDs and/or colchicine should be added toward the end of the taper.25
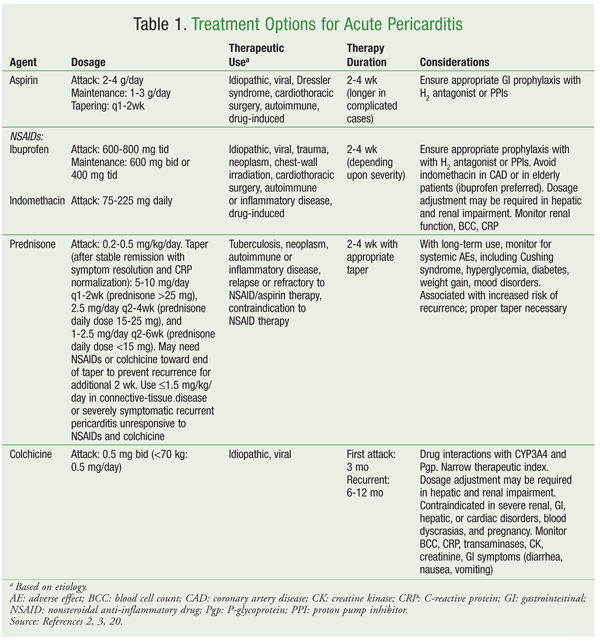
Colchicine is an anti-inflammatory agent that works by inhibiting tubulin polymerization, thereby interfering with migration and phagocytosis and reducing the inflammatory cycle. For acute pericarditis, colchicine is generally used in combination with other therapies. This agent may be useful in recurrent pericarditis, which is immune-mediated, owing to its ability to disrupt the inflammatory cycle involved in pathogenesis.26 Treatment typically lasts up to 12 weeks, but may be administered up to 1 year in the case of recurrent pericarditis. Recent studies have provided strong evidence of colchicine’s effectiveness in treating pericarditis. TABLE 1 summarizes treatment alternatives and dosing for acute pericarditis.2,3,20
Colchicine Evidence
Earlier Studies: The COlchicine for acute PEricarditis (COPE) and COlchicine for REcurrent pericarditis (CORE) trials were the first prospective, open-label, randomized studies to support the use of colchicine for acute and recurrent pericarditis.9,10 COPE and CORE investigated colchicine (>70 kg: 1-2 mg day 1, then 0.5-1 mg daily × 3 months; ≤70 kg: 1 mg day 1, then 0.5 mg daily × 3 months) in combination with HD aspirin (800 mg q6-8h × 7 days and gradual taper over 3-4 weeks) versus HD aspirin alone.9 In cases in which aspirin was contraindicated, prednisone (1-1.5 mg/kg daily × 1 month, followed by taper) was used.9
COPE was conducted in 120 adult patients diagnosed with acute pericarditis.9 The primary endpoint was recurrence rates of incessant-type and intermittent-type disease.9 At 18 months, colchicine significantly reduced recurrence rates by more than 20% compared with aspirin alone (10.7% vs. 32.4%, respectively; P = .004), with a number needed to treat (NNT) of 5.9 CORE examined 84 adult patients with a diagnosis of first recurrence of pericarditis.10 The primary endpoint was colchicine’s effectiveness as first-line therapy for recurrent pericarditis.10 At 18 months, colchicine significantly reduced the recurrence rate by more than 25% compared with aspirin (24% vs. 50.6%, respectively; P = .02), with an NNT of 4.10
Both COPE and CORE revealed that previous corticosteroid use was associated with a more than twofold increase in further recurrences.9,10 The major AE reported in these trials was diarrhea, possibly because of the use of higher doses of colchicine.9,10 COPE and CORE set the stage for the use of colchicine in treating acute and recurrent pericarditis; however, the open-label design of these studies was a major limitation, so definitive conclusions could not be made.
Recent Studies: Colchicine for Recurrent Pericarditis (CORP) was the first prospective, multicenter, double-blind, randomized, placebo-controlled trial investigating the use of colchicine in treating this type of pericarditis.27 CORP’s main objective was to evaluate the efficacy and safety of colchicine for secondary prevention of recurrent pericarditis in 120 patients with a first recurrence of pericarditis.27 In addition to conventional therapy (aspirin 800-1,000 mg or ibuprofen 600 mg q8h × 7 days with gradual taper over 3-4 weeks), patients were randomly assigned to colchicine (>70 kg: 1-2 mg on day 1, then 0.5-1 mg daily × 6 months; ≤70 kg: 0.5 mg q12h day 1, then 0.5 mg daily × 6 months) or placebo.27 When conventional therapy was contraindicated, prednisone (0.2-0.5 mg/kg daily × 1 month, followed by taper) was used.27 At 18 months, colchicine significantly reduced recurrence rates by >30% compared with placebo (24% vs. 55% recurrence, respectively; P <.0001), with an NNT of 3.27 The most common AE was diarrhea.27
The Investigation on Colchicine for Acute Pericarditis (ICAP) was a multicenter, double-blind, randomized trial of 240 adult patients with acute pericarditis.28 The primary objective was to evaluate the efficacy and safety of colchicine in treating a first attack of acute pericarditis and preventing recurrences.28 In addition to conventional therapy (aspirin 800 mg or ibuprofen 600 mg q8h × 7-10 days followed by taper over 3-4 weeks), patients were randomly assigned to colchicine (>70 kg: 0.5-1 mg daily × 3 months; ≤70 kg: 0.5 mg daily × 3 months) or placebo.28 When conventional therapy was contraindicated, prednisone (0.2-0.5 mg/kg daily × 2 weeks, followed by taper) was used.28 At 18 months, colchicine significantly reduced the recurrence rate by about 20% compared with conventional therapy alone (16.7% vs. 37.5%, respectively; P <.001), with an NNT of 5.28 Diarrhea was the AE most commonly reported.28
CORP led to the recommendation of colchicine as a first-line agent for the treatment of recurrent pericarditis in the 2004 guidelines of the European Society of Cardiology.14 ICAP also provided conclusive evidence that colchicine was effective for first acute attacks. Both CORP and ICAP had some limitations, including small sample size, which may have limited the detection of rare AEs. Because patients with neoplastic or bacterial pericarditis were excluded from these studies, the results do not apply to these subsets. The optimal duration of colchicine therapy has not been identified, so further clarification is warranted.
Role of the Pharmacist
Pharmacists play a key role within the healthcare system in informing patients, improving their care, and promoting the safe and effective use of medications. Pharmacists can ensure the safe use of agents used to treat acute pericarditis by educating patients about their medications, recommending appropriate therapies and dose adjustments based on renal function and comorbidities, screening for drug-drug and drug-food interactions, and monitoring for AEs. For instance, in patients receiving NSAIDs, pharmacists can take the lead in evaluating patients and considering the addition of misoprostol or proton pump inhibitors for prophylaxis against NSAID-related gastrointestinal complications such as ulcers, especially in high-risk patients.29 In patients in whom glucocorticoid therapy is warranted, pharmacists can recommend appropriate tapering doses and educate patients and providers about possible long-term AEs associated with prolonged use of corticosteroids. In addition, pharmacists should evaluate the need for prevention of glucocorticoid-induced osteoporosis and recommend calcium, vitamin D, and bisphosphonates as indicated.30
In terms of colchicine, it is imperative that appropriate dosages be used in underweight patients and that frequent monitoring of possible colchicine AEs be conducted. Owing to colchicine’s safety profile, even at lower dosages, caution should be exercised in patients with renal or hepatic impairment. Finally, pharmacists should ensure that medication guides are distributed when required (i.e., with NSAIDs and colchicine).
Conclusion
NSAIDs, glucocorticoids, and colchicine have been demonstrated to have clinical benefit in the treatment of pericarditis. Recent studies have provided strong evidence suggesting that colchicine is an effective treatment option for both acute and recurrent pericarditis. Pharmacists can play a vital role in ensuring the safe and effective treatment of acute and recurrent pericarditis.
REFERENCES
1. Khandaker MH, Espinosa RE, Nishimura RA, et al. Pericardial disease: diagnosis and management. Mayo Clin Proc. 2010;85:572-593.
2. Imazio M. Evaluation and management of pericarditis. Expert Rev Cardiovasc Ther. 2011;9:1221-1233.
3. Lange RA, Hillis LD. Clinical practice. Acute pericarditis. N Engl J Med. 2004;351:2195-2202.
4. Imazio M, Demichelis B, Parrini I, et al. Day-hospital treatment
of acute pericarditis: a management program for outpatient therapy. J Am Coll Cardiol. 2004;43:1042-1046.
5. Imazio M, Cecchi E, Demichelis B, et al. Indicators of poor prognosis of acute pericarditis. Circulation. 2007;115:2739-2744.
6. Imazio M, Brucato A, Adler Y, et al. Prognosis of idiopathic
recurrent pericarditis as determined from previously published reports. Am J Cardiol. 2007;100:1026-1028.
7. Imazio M, Spodick DH, Brucato A, et al. Controversial issues in the management of pericardial diseases. Circulation. 2010;121:916-928.
8. Soler-Soler J, Sagristà-Sauleda J, Permanyer-Miralda G. Relapsing pericarditis. Heart. 2004;90:1364-1368.
9. Imazio M, Bobbio M, Cecchi E, et al. Colchicine in addition to
conventional therapy for acute pericarditis: results of the COlchicine
for acute PEricarditis (COPE) trial. Circulation. 2005;112:2012-2016.
10. Imazio M, Bobbio M, Cecchi E, et al. Colchicine as first-choice
therapy for recurrent pericarditis: results of the CORE (COlchicine for
REcurrent pericarditis) trial. Arch Intern Med. 2005;165:1987-1991.
11. Spodick DH. Intrapericardial treatment of persistent autoreactive pericarditis/myopericarditis and pericardial effusion. Eur Heart J. 2002;23:1481-1482.
12. Imazio M, Demichelis B, Parrini I, et al. Management, risk factors, and outcomes in recurrent pericarditis. Am J Cardiol. 2005;96:736-739.
13. Troughton RW, Asher CR, Klein AL. Pericarditis. Lancet. 2004;363:717-727.
14. Maisch B, Seferovic´ PM, Ristic´ AD, et al. Guidelines on the
diagnosis and management of pericardial diseases executive summary: The
Task Force on the Diagnosis and Management of Pericardial Diseases of
the European Society of Cardiology. Eur Heart J. 2004;25:587-610.
15. Zayas R, Anguita M, Torres F, et al. Incidence of specific
etiology and role of methods for specific etiologic diagnosis of primary
acute pericarditis. Am J Cardiol. 1995;75:378-382.
16. Permanyer-Miralda G, Sagristá-Sauleda J, Soler-Soler J. Primary
acute pericardial disease: a prospective series of 231 consecutive
patients. Am J Cardiol. 1985;56:623-630.
17. Khan AH. The postcardiac injury syndromes. Clin Cardiol. 1992;15:67-72.
18. Hammerman H, Kloner RA, Schoen FJ, et al. Indomethacin-induced scar thinning after experimental myocardial infarction. Circulation. 1983;67:1290-1295.
19. Jugdutt BI, Basualdo CA. Myocardial infarct expansion during
indomethacin or ibuprofen therapy for symptomatic post infarction
pericarditis. Influence of other pharmacologic agents during early
remodelling. Can J Cardiol. 1989;5:211-221.
20. Indik JH, Alpert JS. Post-myocardial infarction pericarditis. Curr Treat Options Cardiovasc Med. 2000;2:351-356.
21. Schifferdecker B, Spodick DH. Nonsteroidal anti-inflammatory drugs in the treatment of pericarditis. Cardiol Rev. 2003;11:211-217.
22. Stubbs DF. Post-acute myocardial infarction symptomatic
pericarditis (PAMISP): report on a large series and the effect of
methylprednisolone therapy. J Int Med Res. 1986;14(suppl 1):25-29.
23. Godeau P, Derrida JP, Bletry O, Herreman G. [Recurrent acute pericarditis and corticoid dependence. Apropos of 10 cases]. Sem Hop. 1975;51:2393-2400.
24. Maisch B, Ristic´ AD, Pankuweit S. Intrapericardial treatment of
autoreactive pericardial effusion with triamcinolone; the way to avoid
side effects of systemic corticosteroid therapy. Eur Heart J. 2002;23:1503-1508.
25. Adler Y, Finkelstein Y, Guindo J, et al. Colchicine treatment for recurrent pericarditis. A decade of experience. Circulation. 1998;97:2183-2185.
26. Markel G, Imazio M, Brucato A, Adler Y. Prevention of recurrent pericarditis with colchicine in 2012. Clin Cardiol. 2013;36:125-128.
27. Imazio M, Brucato A, Cemin R, et al; CORP (COlchicine for
Recurrent Pericarditis) Investigators. Colchicine for recurrent
pericarditis (CORP): a randomized trial. Ann Intern Med. 2011;155:409-414.
28. Imazio M, Brucato A, Cemin R, et al; ICAP Investigators. A randomized trial of colchicine for acute pericarditis. N Engl J Med. 2013;369:1522-1528.
29. Lanza FL, Chan FK, Quigley EM; Practice Parameters Committee of
the American College of Gastroenterology. Guidelines for prevention of
NSAID-related ulcer complications. Am J Gastroenterol. 2009;104:728-738.
30. Grossman JM, Gordon R, Ranganath VK, et al. American College of
Rheumatology 2010 recommendations for the prevention and treatment of
glucocorticoid-induced osteoporosis. Arthritis Care Res (Hoboken). 2010;62:1515-1526.
To comment on this article, contact rdavidson@uspharmacist.com.





