US Pharm. 2022;47(1):14.
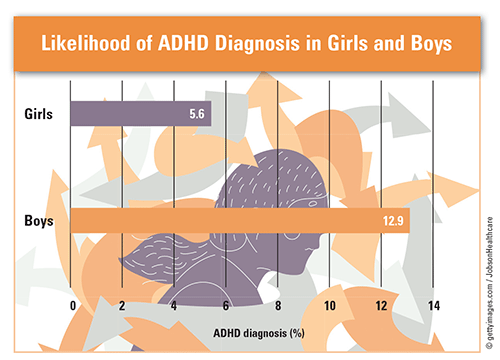
The CDC reported that 6.1 million children were diagnosed with attention-deficit disorder or attention-deficit/hyperactivity disorder (ADD/ADHD) in 2018, accounting for 13.6 million physician office visits. Additionally, 52.7% fewer girls than boys (6.9% vs. 14.6%) were diagnosed with ADD/ADHD. The prevalence of ADD/ADHD diagnoses was lowest in children aged 2 to 5 years (6.4%), and it was six and eight times higher in children aged 6 to 11 years (39.4%) and 12 to 17 years (54.2%), respectively. The prevalence of comorbid disorders in children with ADD/ADHD was 52% for behavior/conduct problems, 33% for anxiety, 17% for depression, 14% for autism spectrum, and 1% for Tourette syndrome.
Treatment for ADD/ADHD: The American Academy of Pediatrics (AAP) recommends behavioral therapy and medication for children aged 6 years and older with ADD/ADHD. Of children who received treatment, 30%, 15%, and 32% were treated with medication only, behavioral treatment only, or combined drug and behavioral treatment, respectively. The remaining 23% did not receive ADD/ADHD drugs or behavioral treatment. According to the 2016 National Parent Survey, among those aged 2 to 17 years, more children received ADD/ADHD medication (62%) than behavioral treatment (47%). Although the AAP recommends behavioral treatment as first-line therapy for children aged 2 to 5 years, 18% were taking ADD/ADHD medication alone and 60% were receiving behavioral treatment. This pattern was reversed among those aged 6 to 11 years, with more children receiving ADD/ADHD medication (69%) than behavioral treatment (51%). The percentage of children aged 12 to 17 years who were taking ADD/ADHD medication was 62%.
Psychological Services: In a study published in 2014 in Journal of Pediatrics, the most common psychological service provided to children aged 4 to 17 years with ADD/ADHD was school support (90%), followed by some type of behavioral treatment or behavioral-skills training (60%) or training in social skills (24%). Less frequently provided psychological services were peer interventions (18%) and parent-delivered behavioral therapy (18%), and the least-used intervention was cognitive-behavioral therapy (12%). The same trend was seen among children aged 12 to 17 years (62% for school support vs. 42% for behavioral treatment/skills training).
Clinical Care: The use of medication alone for treatment in children with ADD/ADHD decreased by 38% (from 48.5% to 30%) from 2014 to 2016, and the use of psychological services combined with medication rose by 17.2% (from 27.3% to 32%). From 2014 to 2016, there was a significant increase (2.5 times) in the number of children diagnosed with ADD/ADHD who received neither medication nor psychological services. However, the number of children with ADD/ADHD who received psychological services alone remained constant at about 15% from 2014 to 2016.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





