US Pharm. 2021;46(9):8-12.
ABSTRACT: In the United States, almost 50% of pregnancies are unintended, and the rate is 75% among teens aged 15 to 19 years. Emergency contraceptives (ECs), including levonorgestrel (Plan B One-Step and generic brands), ulipristal acetate, and the copper intrauterine device, are crucial for preventing unintended pregnancies. The approval of levonorgestrel for OTC use increased patient access to ECs, but many patients still face barriers. Obstacles such as state regulations, antitheft boxes, and misinformation prevent patients from obtaining ECs in a timely manner. Because of their accessibility, pharmacists play a key role in counseling patients on ECs; consequently, it is imperative for pharmacists to address these barriers to access.
In 2011, the CDC reported that 45% of U.S. pregnancies were unintended, and the rate was higher (75%) in teens aged 15 to 19 years.1 OTC emergency contraceptives (ECs) play a critical role in preventing unintended pregnancies. In 2017, the FDA approved Plan B One-Step (levonorgestrel [LVG]) and its generics for OTC use without age or point-of-sale restrictions.2
In a national survey conducted from 2017 to 2019, 24.3% of women aged 22 to 49 years had ever used ECs, and women with a higher educational level were more likely to have used them.3 FDA approval of LVG for OTC use placed pharmacists at the forefront of educating patients about ECs. However, it also sparked a national controversy when some pharmacists refused to dispense ECs for ethical, moral, or religious reasons.
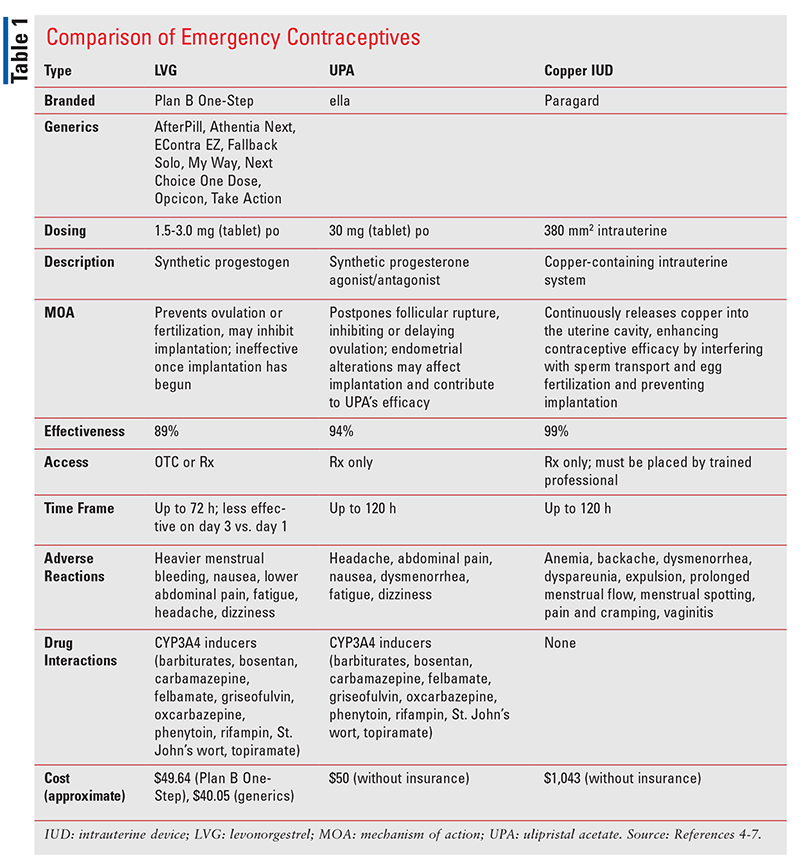
See TABLE 1 for a comparison of the different types of ECs.
Plan B One-Step and Generic LVG
Plan B One-Step, a synthetic progestogen available as a 0.75-mg tablet, is the first progestin-only EC.4 LVG prevents ovulation or fertilization by altering the tubal transport of sperm and/or ova, and it also may inhibit implantation by altering the endometrium. LVG should be taken within 72 hours after unprotected intercourse or suspected contraceptive failure; the sooner it is taken, the more effective it will be.4 Generic versions of Plan B One-Step include, but are not limited to, Take Action, My Way, AfterPill, Aftera, and EContra EZ.
The most common side effects are heavier menstrual bleeding, nausea, lower abdominal pain, and fatigue.4 Some drugs and herbal products, such as barbiturates, carbamazepine, topiramate, and St. John’s wort, may reduce the effectiveness of LVG by inhibiting CYP3A4 enzymes. If the menstrual period is more than a week late, the patient should take a pregnancy test. LVG will not be effective if pregnancy has already occurred, and it should not be mistaken for an abortion pill. There is no evidence that LVG will harm fetal development. Importantly, it must be noted that LVG should not replace regular birth control; rather, it should be used as a backup method for preventing pregnancy.4
Prescription EC Alternatives
Prescription-only EC alternatives to LVG are ulipristal acetate (UPA) and the copper intrauterine device (IUD).5,6 In 2010, UPA (ella) was FDA-approved for use as an EC.5 UPA is a progestin receptor antagonist that prevents pregnancy by delaying or inhibiting ovulation. This 30-mg tablet may be taken up to 120 hours after unprotected intercourse to prevent pregnancy. Unlike LVG, UPA works as effectively on day 4 as it does on day 1.5 The average cost of UPA, without insurance, is approximately $50.7
In 2014, a shortage of UPA occurred when the U.S. distributor discontinued the product. The manufacturer partnered with a new distributor, but many prescribers remained unaware that UPA was once again available.7 Studies have found that UPA is rarely stocked, with an average of 3% to 10% of pharmacists reporting the product to be in stock. A national study also indicated that fewer than 30% of reproductive-health prescribers had heard of UPA and only 7% had prescribed it.8 This lack can deter pharmacies from stocking UPA in an effort to avoid losing money on expired products.
Nonhormonal copper IUDs, which have been in use since 1988, are the most effective EC method.6 Copper IUDs prevent pregnancy by decreasing sperm motility and viability, changing the speed of ovum transport, and damaging or destructing the ovum. They also work post fertilization by damaging or destroying the fertilized ovum. Copper IUDs are unaffected by the patient’s BMI or time of menstrual cycle at insertion.6 Disadvantages of this EC are the price, procedure, and side effects.7 The cost of the device ranges from $500 to $1,000, not including the costs for provider visits for insertion, removal, and confirmation that the device is properly placed. Copper IUDs have become more accessible since the passage of the Affordable Care Act, which mandates coverage for this device without cost sharing.7
FDA OTC Guidelines for LVG
Plan B One-Step was first approved by the FDA in 1999.2 Soon afterward, the manufacturer sought a switch to OTC status, a process that took several years before the FDA granted approval for OTC use of LVG.2 In 2009, LVG was made available without a prescription for women aged 17 years and older, and in 2013, the FDA approved OTC use of LVG without age or point-of-sale restrictions.2 The increased ability of patients to purchase ECs made pharmacists the primary provider of EC education and counseling to patients. Although LVG is approved for OTC use, each state has its own regulations, which in some cases has created barriers to access. For example, nine states have adopted restrictions on EC. Arizona, Arkansas, Georgia, Idaho, Mississippi, and South Dakota explicitly allow pharmacists to refuse to dispense contraceptives, including EC.8 In contrast, eight states allow pharmacists to dispense EC without a physician’s prescription under certain conditions.8 These varying regulations among states can impact EC access and counseling.
Barriers to EC Access
State Regulations: A study that used a telephone-based mystery-caller survey to determine EC availability and counseling provided by pharmacists in San Diego and San Francisco, California, and Atlanta, Georgia, suggested that access and counseling may be better in states with an expanded scope of practice.9 (Pharmacists in California are authorized to prescribe hormonal contraceptives if they completed a Doctorate of Pharmacy from an accredited California college of pharmacy after 2014; they can also prescribe ECs, but 1 hour of continuing education is required. Georgia does not allow pharmacists to prescribe hormonal contraceptives or ECs, and pharmacists are explicitly allowed to refuse to dispense ECs.) Most pharmacists responded that ECs were available, but California pharmacists mentioned UPA and were more likely to correctly note that LVG may be less effective when used 4 days after intercourse.9 A significantly larger percentage of California pharmacists said that LVG was in stock, compared with Georgia pharmacists (89.5% vs. 67.8%, respectively). Results suggest that pharmacists in states that permit them to prescribe ECs are more likely to provide immediate access and accurate information regarding ECs. Patients in states such as California would also have access to UPA, which can be crucial if they have missed the 72-hour efficacy window for LVG.9
Physical Barriers: In addition to differing state regulations regarding the sale of LVG, patients have other barriers to overcome before gaining access to ECs. Research comprising an online questionnaire targeted to reproductive-health professionals across the U.S. and local data collection revealed that approximately 68% of 220 pharmacies kept LVG in a plastic box that the customer had to take to the register to be unlocked.10 Moreover, one-third of stores did not sell LVG on OTC shelves. Having to ask an employee to unlock or locate ECs can be embarrassing and draw unwanted attention to the patient; physical barriers also compromise the patient’s confidentiality. Many stores chose to keep LVG locked up because of the high cost (the average price of Plan B One-Step was $49.64, and that for generic LVG was $40.05). Some stores kept LVG behind the counter to prevent theft, but the signage directing customers to where to locate it frequently was limited. Chain stores were more likely than independent pharmacies to stock LVG (77% vs. 5%, respectively). This was due to chain stores’ ability to provide OTC shelf space and prevent product loss.10
Cost Issues and Misinformation: The high cost of LVG also creates financial barriers, especially for younger patients, who may be unable to afford it. Additionally, the study involving the online questionnaire plus local data collection found that 40% of pharmacies incorrectly reported an age restriction for purchasing LVG without a prescription.10 The reported age ranged from 13 years to 18 years, and most pharmacy staff stated that the customer had to be at least 17 or 18 years old to purchase nonprescription LVG. Stores that sold ECs behind the counter were more likely to report an age restriction compared with stores selling them on OTC shelves (64% and 27% of stores, respectively).10 Misinformation and confusion surrounding EC regulation and purchase can prevent patients from accessing ECs in a timely manner. To improve LVG availability for patients, pharmacies should ensure that the product is on OTC shelves and that staff keep abreast of current regulations.
Patient Education
After FDA approval of LVG for OTC use, pharmacists became the primary source for EC access and counseling. Availability of LVG in pharmacies is especially important for younger patients who are unable to visit the emergency room (ER) or a gynecologist to get an EC prescription. Given that the rate of unintended pregnancy is highest among teens aged 15 to 19 years, increased access to ECs, as well as the provision of sex education by pharmacists, can help prevent many of these pregnancies.1
In one study, an anonymous survey was administered to female and male patients aged 10 to 25 years at a mobile health clinic in the San Francisco Bay Area.11 All patients were uninsured, and some were homeless. Many of the 439 patients knew about ECs, but only 38% were aware that they could be obtained OTC. Forty percent of patients incorrectly identified or were uncertain whether ECs could be used as birth control or as an abortion pill, and 44% believed that LVG had to be taken within 1 day of unprotected sex.11
Lack of awareness regarding purchasing regulations for ECs is a barrier to preventing unintended pregnancies; also, the misconception that LVG is effective only within 1 day of unprotected sex could lead to underuse of ECs.11 Pharmacist education is essential to ensure that teens are aware of available resources. Pharmacists can inform patients that LVG is an OTC EC that is effective within 72 hours after unprotected sex and UPA is a prescription EC that is effective within 120 hours after unprotected sex. Additionally, pharmacists can debunk the belief that LVG is an abortion pill and can counsel teens to visit their primary care physician or a gynecologist to obtain regular birth control.1
Patient Confidentiality
A study that conducted small group interviews to assess the experiences and perceptions of OTC ECs among female college students found that although participants were aware that unprotected sex could result in pregnancy, many had incomplete knowledge surrounding EC timing, effectiveness, and side effects.12 Participants’ main concern was that their confidentiality would be compromised. Confidential and affordable reproductive healthcare was not easily available to many participants. Visiting the ER or a gynecologist would involve their health insurance, leading to parental discovery; health services on campus were also viewed as inconvenient because participants feared that other students might witness them using these services.12
Some participants noted that their educational level contributed to their decision to use ECs.12 Those with a higher level of education had greater awareness of the risks of unintended pregnancy and methods to prevent its occurrence. Cost was a potential barrier for some, but many participants commented that the cost of EC was substantially less than the cost of having an abortion or raising a child.12 Although OTC LVG can be expensive ($40-$50), the advantage for young female patients is that pharmacists are readily accessible and maintain patient confidentiality; they also can provide sex education to these patients and counsel them on how to properly take LVG.
Pharmacist Ethics and Duties
Another barrier to access is the conscience clause, which gives pharmacists the right to refuse to perform certain services if it violates their religious or personal beliefs.13 The dispensing of ECs may go against the religious and personal beliefs of some pharmacists, and—depending on the state—refusal to do so can greatly impact patient access to ECs. Given the time-sensitive window for EC use, some states require a pharmacist to refuse with patient protections.13
For example, in New York State, pharmacists are required to inform their supervisor if their beliefs may limit the drug products they will dispense.13 In some states, such as New Jersey, pharmacists are required to fill a prescription regardless of their beliefs. NJ Rev. Stat. §45:14-67.1 states that “a pharmacy practice site has a duty to properly fill lawful prescriptions…without undue delay, despite any conflicts of employees to filling a prescription and dispensing a particular prescription drug or device due to sincerely held moral, philosophical or religious beliefs.”13
In certain states, such as Arizona, Arkansas, Georgia, Idaho, and South Dakota, pharmacists have the right to refuse without patient protections.13 The law in these states gives pharmacists the right to refuse to dispense ECs, based on religious or personal beliefs, without having to provide patient support.13 This, however, can result in delayed patient access to ECs. Each state has its own laws regarding the right to refuse, so it is essential for both pharmacists and patients to be aware of the laws in their state.
Consequences of Barriers to EC Access
It is imperative that barriers to LVG access are addressed so that patients receive ECs in a timely manner. Women who have unprotected sex have a limited time frame—72 hours—to take LVG for pregnancy prevention, and the more time that passes, the less effective LVG will be. A patient who is unable to obtain LVG in time to prevent a pregnancy may resort to an abortion, which is more expensive and can lead to complications. According to the American College of Obstetricians and Gynecologists, the risk of death from an abortion is less than 1 in 100,000 but increases with every week of pregnancy.14 In 2014, more than 50% of all U.S abortion patients were in their 20s, 12% were adolescents, and 75% had an income below the federal poverty level. The average cost of an abortion with local anesthesia is $508, the average cost of an early medication abortion is $535, and the cost increases the further pregnancy progresses.15 These listed costs does not include transportation, food, childcare, and lost wages.
Younger patients may also delay getting an abortion if their state requires parental consent or notification, putting them at greater risk for complications. In 2021, many states have introduced or enacted legislation that restricts access to abortion.16 For example, South Carolina placed a ban on abortion as early as the 6th week of pregnancy, Kentucky granted its Attorney General additional authority to close abortion clinics, and Kansas has an August 2022 ballot initiative that would amend its state constitution to explicitly exclude abortion rights.16 Pharmacists play a crucial role in ensuring that patients have timely access to LVG for pregnancy prevention in order to avoid an unintended pregnancy or an abortion.
Conclusion
FDA approval of LVG for OTC use without age restriction expanded access to birth control and sex education for many female patients. However, many barriers remain that must be addressed. For many patients, purchasing ECs is confusing, intimidating, and embarrassing. About 40% of pharmacies incorrectly reported that there was an age restriction for buying ECs without a prescription. The high cost of LVG is also a barrier, with most chain stores using antitheft devices or placing LVG behind the pharmacy counter to prevent theft. Independent pharmacies are less likely to stock LVG based on their inability to absorb product losses. To address these barriers, education should be provided to all staff, not just pharmacy staff. In addition, regulations concerning the sale of LVG would give pharmacists who are uncomfortable with selling ECs a guideline on how to ensure that patients obtain these products. The use of ECs is time-sensitive, and it is important to remove all barriers to access and to provide accurate education.
REFERENCES
1. CDC. Unintended pregnancy. www.cdc.gov/reproductivehealth/contraception/unintendedpregnancy/index.htm. Accessed May 15, 2021.
2. FDA. FDA approves Plan B One-Step emergency contraceptive for use without a prescription for all women of child-bearing potential. http://web.archive.org/web/20160602063312/http:/www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm358082. Accessed April 21, 2021.
3. QuickStats: percentage of women who have ever used emergency contraception among women aged 22-49 years who have ever had sexual intercourse, by education—National Survey of Family Growth, United States, 2017–2019. MMWR Morb Mortal Wkly Rep. 2021;70:145.
4. Plan B One-Step (levonorgestrel) package insert. Pomona, NY: Barr Pharmaceuticals, Inc; July 2009.
5. ella (ulipristal acetate) package insert. Morristown, NJ: Watson Pharma, Inc; August 2010.
6. Paragard (intrauterine copper contraceptive) package insert. Trumbull, CT: CooperSurgical, Inc; September 2019.
7. Rafie S, Stone RH, Wilkinson TA, et al. Role of the community pharmacist in emergency contraception counseling and delivery in the United States: current trends and future prospects. Integr Pharm Res Pract. 2017;6:99-108.
8. Guttmacher Institute. Emergency contraception. www.guttmacher.org/state-policy/explore/emergency-contraception. Accessed April 21, 2021.
9. Stone RH, Rafie S, Ernest D, Scutt B. Emergency contraception access and counseling in urban pharmacies: a comparison between states with and without pharmacist prescribing. Pharmacy (Basel). 2020;8:105.
10. Cleland K, Bass J, Doci F, Foster AM. Access to emergency contraception in the over-the-counter era. Womens Health Issues. 2016;26:622-627.
11. Yen S, Parmar DD, Lin EL, Ammerman S. Emergency contraception pill awareness and knowledge in uninsured adolescents: high rates of misconceptions concerning indications for use, side effects, and access. J Pediatr Adolesc Gynecol. 2015;28:337-342.
12. Hickey MT, White J. Female college students’ experiences with and perceptions of over-the-counter emergency contraception in the United States. Sex Reprod Healthc. 2015;6:28-32.
13. National Conference of State Legislatures. Pharmacist conscience clauses: laws and information. www.ncsl.org/research/health/pharmacist-conscience-clauses-laws-and-information.aspx. Accessed May 29, 2021.
14. American College of Obstetricians and Gynecologists. Induced abortion. www.acog.org/womens-health/faqs/induced-abortion. Accessed May 27, 2021.
15. Guttmacher Institute. Induced abortion in the United States. www.guttmacher.org/fact-sheet/induced-abortion-united-states?gclid=CjwKCAjwqcKFBhAhEiwAfEr7zVS-7xpmBkdbmtu3oBZLxXyWXVir3Sj0yJAa6sXaNcp3stz5fz_KFRoC1PQQAvD_BwE#. Accessed May 28, 2021.
16. Nash E. The danger ahead: early indicators show states will be the main abortion battleground in 2021. www.guttmacher.org/article/2021/03/danger-ahead-early-indicators-show-states-will-be-main-abortion-battleground-2021#. Accessed May 29, 2021.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





