US Pharm. 2014;39(1):52-56.
ABSTRACT: Attention-deficit/hyperactivity disorder (ADHD) is often thought of as a disorder of childhood, but approximately one-half of individuals who exhibit ADHD early in life will go on to have persistent symptoms into adulthood. These symptoms generally differ in presentation from the typical presentation of a school-aged child with hyperactivity and academic difficulties. Further complicating the picture is the fact that co-occurring psychiatric disorders that were not apparent during an individual’s younger years can present in later adolescence. Therefore, the diagnosis and treatment of symptomatic patients can change over time, requiring some similar and some unique approaches to therapeutically managing ADHD in adults.
Attention-deficit/hyperactivity disorder (ADHD; also called attention-deficit disorder) is a neurobehavioral condition that causes impairments in concentration, impulsivity, and cognitive processing. As with many psychiatric conditions, the diagnosis of ADHD relies on subjective observations. Attempts to pinpoint the neuropathology of ADHD are ongoing. It was formerly believed that ADHD was a disorder of childhood that resolved with age. It was not until the publication of the Diagnostic and Statistical Manual of Mental Disorders, Third Edition–Revised, in 1987 that the existence of ADHD in adults was recognized, provoking the question of how patients with childhood ADHD differ from those who continue to have symptoms beyond adolescence.1 Although this question has not been completely answered, current research has been able to increase understanding of ADHD and how to best manage the unique symptomology of the adult patient.
Diagnosis
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), classifies ADHD into three subtypes (primarily inattentive, primarily hyperactive/impulsive, and mixed) (TABLE 1). In order for a patient to qualify for diagnosis, the symptoms must have been present to a significantly impairing degree prior to age 12 years, must occur in two or more settings, and may not be better explained by an alternative mental disorder.2 The DSM-5 has made multiple changes to the definition in the previous edition, reflecting new research supporting the existence of ADHD that persists beyond adolescence. Older ADHD patients develop coping mechanisms to dampen overt hyperactivity symptoms, necessitating the need for an adult diagnosis to be directed toward the concentration and prioritizing difficulties that hinder the relationships and work environments of older ADHD patients.3 These changes to the definition make it possible for the etiology of adult ADHD to be recognized even if the hyperactivity has been remedied and memory recall of early childhood is hazy.

Pathophysiology
The symptomology of ADHD was initially thought to be caused by brain damage from illness or traumatic injury. While current research shows that this is not the case, brain development in a person with ADHD differs significantly from the norm. Functional and structural studies of the ADHD brain compared with the typical brain show an activity deficit in the prefrontal cortex. This area of the brain is known for its involvement in working memory, attention, organization, constraint, and impulsivity, all of which can be impaired in the individual with ADHD. However, it is not known where these deficits exist structurally on a neurologic level. Is the neurologic abnormality in the prefrontal cortex itself or in another area of the brain that projects to the prefrontal cortex, or is there an area in a state of plasticity that may or may not correct itself with age? The answer is unknown, but current research tends to support plasticity.4,5
Genetics and Environment
Numerous studies have confirmed a genetic component to the development of ADHD. While the genome does not entirely account for the existence or absence of the disorder, a 2011 meta-analysis of more than 1,800 genetic studies determined heritability to be between 75% and 91%.6 It is likely that a group of genes, rather than a single gene, combines with certain in utero and early-life stressors to create the necessary physiology for ADHD. Heavy genetic and early environmental influences create an extremely high instance of ADHD within families. One large population study found that 84% of adult subjects with persistent ADHD had at least one child diagnosed with the disorder.7 This finding is supported by sibling and twin studies showing a strong genetic component to the disorder and an even stronger familial link in subjects experiencing ADHD into adulthood.7
Environmental factors linked to ADHD are numerous. Just as there is no one genetic factor that can predict the presence of ADHD, there is no single environmental factor that can do the same. Certain gestational and neonatal exposures—including toxemia during gestation and delivery, maternal illness, maternal psychosocial stress, and fetal nicotine exposure—seem to be significant indicators of ADHD and other cognitive problems later in life. Later in childhood, maternal malaise, caregiver emotional distance, and criticism directed at the young child have been correlated with an increased incidence of ADHD.7 The biologic link to the majority of these risk factors is an increased presence of the human stress response in the young child, causing the developing brain to be overexposed to catecholamines. It stands to reason, then, that ADHD—at least in part—is an adaptive measure to dampen the catecholamine response in a constantly stimulated brain.7
Epidemiology
By definition, ADHD always begins in childhood. Symptoms may or may not continue beyond adolescence. The prevalence of patients who continue to show symptoms into adulthood is estimated at roughly 50%, based on retrospective surveys.5 One large meta-analysis found the prevalence of ADHD in American children to be between 5% and 8%, and in the 2007 National Survey of Children’s Health, 9.5% of parents reported having a child with ADHD.8 These observational estimates, if correct, translate to 3% to 5% of American adults. The National Comorbidity Survey Replication determined the prevalence of ADHD in adults to be 4.4%.9
Co-occurring Conditions and Differential Diagnoses
Co-occurring conditions are disorders that are distinctly different, yet occur concurrently in the same individual. The practice of psychiatry is often complicated by this blurred type of disease presentation, and ADHD is no exception. Reports of co-occurring conditions with ADHD vary with regard to exact prevalence, but it is accepted that individuals with ADHD are more likely than not to have a co-occurring condition.7 The symptoms of ADHD can mimic those of anxiety, depression, emotional trauma, bipolar disorder, and many other psychological disorders and syndromes (depending upon the specific symptom), or they can occur in addition to these disorders. The process of differential diagnosis, therefore, is crucial. Lifetime studies have found, within the ADHD patient’s life span, a prevalence of 45% for mood disorders, 59% for anxiety, and 36% for substance abuse.9 Also, certain genetic subsets are more likely to show unique co-occurring conditions, such as conduct disorders (e.g., oppositional defiant disorder) occurring with ADHD.7 These factors can mean drastic differences in treatment, depending upon the cause of the symptoms. This makes the importance of diagnosis and consistent follow-up with a mental health professional not merely advisable, but vital to the success and improved quality of life of the adult ADHD patient.
Treatment
As the brain evolves with age, so does the pathophysiology of ADHD. This may translate to a need to alter therapy in the maturing adult. The symptomology, societal expectations, and co-occurring conditions that accompany adult ADHD warrant further exploration of the options available to curb ADHD symptoms. Some of the consequences of unrecognized and/or undertreated ADHD are lower occupational achievement, greater financial distress, increased rates of divorce or relationship turmoil, more sexually transmitted infections, more altercations with law enforcement, higher rates of substance abuse/addiction, more anxiety and depression, chronic lateness, and increased explosive outbursts.10
Stimulants: Methylphenidate (MPH) and amphetamines have long been the drugs of choice for children and, by extension, adults with ADHD. At first glance, the use of stimulants seems counterintuitive in a group of patients who already seem highly stimulated, but in reality the stimulation involves the neurotransmitters of the central nervous system (CNS). This class of drugs acts by binding to presynaptic dopamine transporters and/or blocking reuptake mechanisms, allowing the catecholamine deficit existing in ADHD to be temporarily remedied. MPH and amphetamines appear to have a specific proclivity for the prefrontal cortex, although both have limited actions throughout the CNS.1
There is concern about the tendency of stimulants to increase blood pressure and create cardiovascular (CV) stress in children, and this is a particular concern in adults, as well. Long-term safety in adults has not yet been studied; therefore, caution should be taken, particularly in patients with CV risk factors.11 Furthermore, the anxiety and depression that often accompany ADHD in adults should be considered. There is a well-established correlation between stimulant use and depression.1 Whether this is a cause-and-effect relationship or simply an unmasking of an underlying disorder remains to be determined, but the correlation warrants caution in patients with a history of depression. In such cases, a primary antidepressant (discussion follows) with an adjunctive stimulant may be a more appropriate first step.
With all stimulants, the overall response rate hovers around 70%, and it is unclear why some patients respond better to methylphenidate than to amphetamines.1 Dosage and dosage form vary from patient to patient, and numerous options are available (TABLE 2).
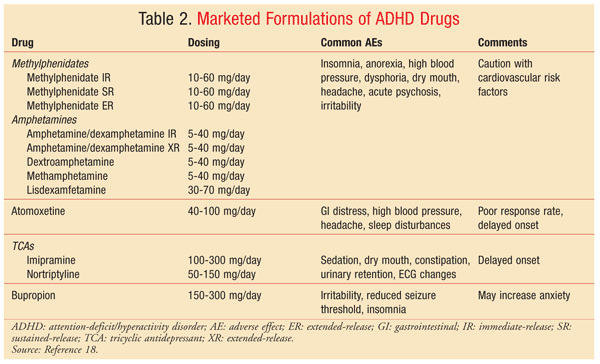
Nonstimulants: Atomoxetine (Strattera) is a novel drug that acts on the reuptake mechanism of norepinephrine (NE) without significantly interfering with the function of other neurotransmitters. It seeks to correct the imbalance of NE insufficiency in the prefrontal cortex in ADHD patients by inhibiting the presynaptic reuptake of NE and increasing the amount of time NE spends interacting with the synaptic cleft.12 Efficacy studies are positive, with a significant number of patients demonstrating a symptom decrease of at least 25% from baseline versus placebo. However, the percentage of responders is quite low (20%-60%, with an average response rate of ~30%) compared with the response rate of approximately 70% for children and adults taking stimulants for symptom management.12 This profile indicates that atomoxetine is a viable adjunct or second-line agent for suppressing negative ADHD symptoms, but may not be warranted as a first-line agent.
Tricyclic antidepressants (TCAs) such as imipramine and nortriptyline offer benefits particularly useful for adult ADHD. Not only are these drugs significantly more effective than placebo in treating ADHD symptoms, they also treat depression, anxiety, and tic disorders, all of which commonly occur with ADHD. Additionally, they may increase the ability to fall asleep if taken at bedtime, which is useful when used as adjunct to a stimulant that can cause insomnia. The anticholinergic side-effect profile of TCAs is intolerable for many patients, thus limiting the use of TCAs as a primary agent. If the side-effect profile can be overcome, patients with ADHD and co-occurring psychiatric conditions may benefit from the use of a TCA.13
Bupropion is another nonstimulant option that addresses many of the conditions coexisting with ADHD. According to observational research, bupropion may increase cognitive functioning and reduce depression, aggression, and hyperactivity in adults with ADHD, but the drug is not indicated for these uses.14 Bupropion is, however, approved as a smoking-cessation agent, which can be an advantage given that adults with ADHD are significantly more likely than their non-ADHD counterparts to smoke.15 Drawbacks to bupropion include its unpredictable effects on anxiety, its tendency to exacerbate tics, and its known lowering of seizure threshold. Therefore, bupropion should not be used in patients with a history of tic disorders or seizures, and it should be used with caution in patients with anxiety. Given its more tolerable side-effect profile compared with TCAs, bupropion has potential as a primary agent of choice for adult ADHD when its use is not contraindicated. Stimulants may be used in conjunction with bupropion, but extra care should be taken to use the lowest possible dosage.
Alpha2 agonists such as clonidine and guanfacine are indicated for the treatment of ADHD in children and adolescents as monotherapy or as adjunctive therapy to a psychostimulant. Since these agents stimulate alpha2 receptors in the prefrontal cortex, NE flow and synaptic connectivity are enhanced. Low tolerability, hypotension, and sudden death have been reported in children and adolescents taking clonidine, although these effects are less certain in adults.5 In addition, the safety and efficacy of alpha2 agonists have not been established in adults. As such, these agents are last-step alternatives in the management of ADHD.
Nonpharmacologic Therapy: Cognitive behavioral therapy (CBT), the mainstay of nonpharmacologic treatment for ADHD, involves working with a qualified professional to create coping mechanisms and behavioral adaptations for the cognitive processes that cause issues for the patient.16 Large studies examinining the effects of CBT with and without stimulants in children have concluded that CBT significantly improves ADHD symptoms, but no more than stimulant medication alone. CBT and stimulants used together were equally as efficacious as stimulants used alone in some studies, whereas CBT plus stimulant use spurred significant improvements in subsets with co-occurring anxiety, depression, and conduct disorder.5,7,9 In an effort to replicate this finding in adults, Weiss and colleagues performed a small study in which one group was assigned to CBT therapy plus dextroamphetamine and the other group was assigned to CBT plus placebo. Both groups showed improvement, although there was no significant between-group difference. The small study population and incomplete optimization of stimulant therapy could be factors in the failure to show a significant difference. However, the results indicate the need for further research into the use of CBT with and without a variety of ADHD medications in adults, especially adults with coexisting conditions.17
A lot of media attention has focused on dietary causes of hyperactivity in children. To date, no known food products or food additives have been shown to correlate consistently with abnormal hyperactivity or ADHD in adults.7 One popular diet, the Feingold diet, is postulated to be beneficial for hyperactivity and ADHD symptoms, as well as for myriad other ailments. The main focus of the diet is to limit food dyes and additives.6 This diet, however, when properly striated and compared with placebo, shows no significant ability to alleviate ADHD symptoms.7 In general, well-balanced nutrition and regular meals help ensure that ADHD therapy works optimally and side effects are properly managed.
As with many disorders and illnesses, there are times when a simple sense of community and understanding go a long way toward improving treatment outcomes. TABLE 3 lists some common organizations and associations that seek to improve awareness of ADHD and further increase the quality of life of people living with attention deficits.

Drugs on the Horizon: Nicotinic agonists are being studied as a new treatment for ADHD. While the behavioral response to developing nicotinic agonist drugs does not seem significant, the cognitive response seems positive. The hypothesis for this treatment route resulted from observational studies that found that smoking and nicotine exposure tended to improve cognition in subjects with ADHD.15 Worthy of note is the fact that the ADHD population has a significantly higher degree of smokers than the non-ADHD population. Naturally, the negative health outcomes and addictive properties of smoking and nicotine deter its use as an acceptable form of treatment, but research is being conducted to find nicotinic acetylcholine agonists with a more acceptable side-effect profile in order to improve cognitive deficits in ADHD.15
Pharmacist Involvement
Pharmacists can play an important role in the management of medications for the adult ADHD patient. Often, adult ADHD patients either are switching medications that have stopped working for them or are receiving for the first time medications for a problem that has caused them difficulties for years. Both situations warrant a thorough understanding and explanation of what to expect, when patience is necessary, and when to contact the prescriber. Also, the newness of adult ADHD as a recognized disorder has left many primary care physicians and psychiatric professionals uninformed as to proper management of the adult situation. A pharmacist who has a thorough understanding of the pharmacology and efficacy of the available options can be a vital component of a healthcare team that provides effective treatment for the adult ADHD patient.
REFERENCES
1. Greydanus DE, Pratt HD, Patel DR. Attention deficit hyperactivity
disorder across the lifespan: the child, adolescent, and adult. Dis Mon. 2007;53:70-131.
2. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Washington, DC: American Psychiatric Association; 2013.
3. Grohol JM. DSM-5 changes: attention deficit hyperactivity disorder
(ADHD).
http://pro.psychcentral.com/2013/dsm-5-changes-attention-deficit-hyperactivity-disorder-adhd/004321.html.
Accessed July 10, 2013.
4. Faraone SV, Biederman J, Spencer T, et al. Attention-deficit/hyperactivity disorder in adults: an overview. Biol Psychiatry. 2000;48:9-20.
5. Evidence-based practice and attention deficit hyperactivity disorder (ADHD). In: Glicken MD. Evidence-Based Practice With Emotionally Troubled Children and Adolescents. San Diego, CA: Academic Press; 2009:217-228.
6. Zhang L, Chang S, Li Z, et al. ADHD gene: a genetic database for attention deficit hyperactivity disorder. Nucleic Acids Res. 2012;40:D1003-D1009.
7. Faraone SV, Biederman J. Pathophysiology of attention
deficit/hyperactivity disorder. In: Davis KL, Charney D, Coyle JT,
Nemeroff C, eds. Neuropsychopharmacology: The Fifth Generation of Progress. Philadelphia, PA: Lippincott Williams & Wilkins; 2002:577-596.
8. Increasing prevalence of parent-reported attention
deficit/hyperactivity disorder among children—United States, 2003 and
2007. MMWR Morb Mortal Wkly Rep. 2010;59:1439-1443.
9. Adler LA, Spencer TJ, Stein MA, Newcorn JH. Best practices in
adult ADHD: epidemiology, impairments, and differential diagnosis. CNS Spectrums. 2008;13(suppl 12):8.
10. WebMD. 10 problems that could mean adult ADHD. www.webmd.com/add-adhd/10-symptoms-adult-adhd. Accessed October 31, 2013.
11. Lensing MB, Zeiner P, Sandvik L, Opjordsmoen S. Four-year outcome
in psychopharmcologically treated adults with
attention-deficit/hyperactivity disorder: a questionnaire survey. J Clin Psychiatry. 2013;74;e87-e93.
12. Caballero J, Nahata MC. Atomoxetine hydrochloride for the treatment of attention-deficit/hyperactivity disorder. Clin Ther. 2003;25(12):3065-3083.
13. Benkert D, Krause KH, Wasem J, Aidelsburger P. Effectiveness of
pharmaceutical therapy of ADHD (attention-deficit/hyperactivity
disorder) in adults. GMS Health Technol Assess. 2010;6:1-12.
14. Newcorn J, Weiss M, Biederman J. Nonstimulant medications. Medscape Education. www.medscape.org/viewarticle/531493_3. Accessed July 10, 2013.
15. Wilens TE, Decker MW. Neuronal nicotinic receptor agonists for
the treatment of attention-deficit/hyperactivity disorder: focus on
cognition. Biochem Pharmacol. 2007;74:1212-1223.
16. National Alliance on Mental Illness. Cognitive behavioral therapy
(CBT).
www.nami.org/Content/NavigationMenu/Inform_Yourself/About_Mental_Illness/About_Treatments_and_Supports/Cognitive_Behavioral_Therapy1.htm.
Accessed July 10, 2013.
17. Weiss M, Murray C, Wasdell M, et al. A randomized controlled
trial of CBT therapy for adults with ADHD with and without medication. BMC Psychiatry. 2012;12:30. http://www.biomedcentral.com/1471-244X/12/30. Accessed July 10, 2013.
18. Clinical Pharmacology [subscription database]. www.clinicalpharmacology.com. Accessed October 31, 2013.
To comment on this article, contact rdavidson@uspharmacist.com.





