Assessing and monitoring cardiovascular medication therapy in seniors involves a comprehensive approach. Elements to be considered include the effects of aging on cardiovascular function, identifying seniors at risk for medication-related problems (MRPs), prescribing trends, the concept of “post-hospital syndrome,” and opportunities for traditional and novel pharmacist-delivered medication therapy management (MTM).
Age-Associated Vulnerability
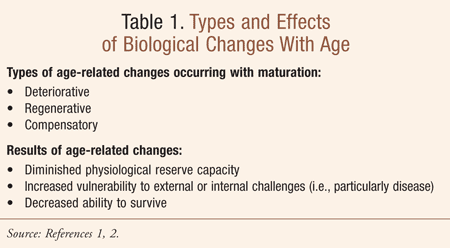
Disease does not result from aging itself, but rather from the vulnerability that aging causes in lowering the threshold for the development of disease (TABLE 1).1 Aging also intensifies and accelerates the effects of disease once a condition or disorder is initiated.1 Overall, physiological deterioration plays an important role in the increase in the age-specific mortality rate associated with aging.2 In older adults, age-associated changes in drug absorption, distribution, metabolism, and elimination are more important predictors of pharmacokinetic alterations than is aging per se.3 Due to age-related physiological changes (e.g., renal impairment), seniors are more vulnerable to adverse drug events (ADEs).4 With this in mind, the practice of considering a newly manifested symptom or sign in an older adult as potentially being caused by a medication until proven otherwise is prudent. Ongoing assessment and monitoring of medication therapy in vulnerable seniors is warranted to ensure safety and optimize therapeutic outcomes.5,6
Effects of Aging on the Cardiovascular System
Aging is accompanied by substantial alterations in anatomy and physiology of the heart and vasculature. Important age-related factors pertinent to the cardiovascular system are outlined in TABLE 2 . A serious disorder that can significantly affect cardiovascular function is coronary atherosclerosis; this condition can be subclinical and is highly prevalent in Western societies.1 Even more common is systemic arterial hypertension. Therefore, in order to separate aging from subclinical and clinical disease, reasonable screening is meaningful.1

The tendency to gain weight increases with age, leading to obesity. Adipose tissue secondary to excess caloric intake imparts a variety of effects involving practically all physiological systems.1 Potential complications of obesity that may affect the cardiovascular system include diabetes mellitus, dyslipidemia, hypertension, coronary artery disease, deep venous thrombosis, and pulmonary embolism.7,8 Medications such as prednisone as well as specific conditions (e.g., hypothyroidism, Cushing’s syndrome, genetic alterations, neurologic disorders) may occasionally cause secondary obesity.9,10
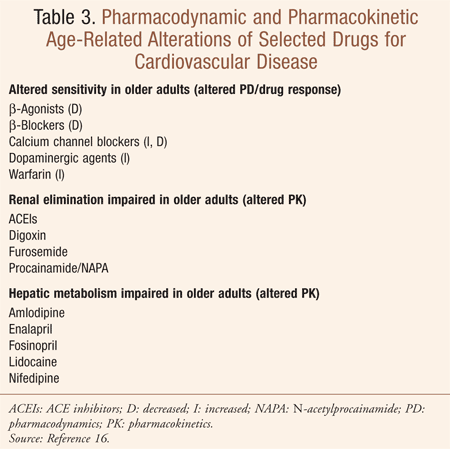
Assessing and monitoring cardiovascular
medication therapy requires addressing factors such as altered
pharmacodynamics, altered pharmacokinetics, renal and hepatic
impairment, overprescribing, and underprescribing. TABLES 2 and 3 can help to identify patients who may be at risk for MRPs and benefit from MTM.
Implications of a Recent Hospitalization
According to meeting highlights of the American Heart Association Scientific Session 2012, an examination of the National Cardiovascular Data Registry ACTION Registry—Get With The Guidelines was conducted looking at myocardial infarction (MI) patients admitted between January 2007 and March 2011, to answer the question, “Is high-dose aspirin being prescribed indiscriminately to patients who have experienced an acute MI?”11
Surprisingly, 44% of individuals receiving triple therapy (aspirin, clopidogrel, and warfarin) were discharged receiving high-dose aspirin (325 mg); 57% of individuals with a major bleeding event (i.e., a 4 mg/dL drop in hemoglobin, intracranial hemorrhage, or red blood cell transfusions) while in the hospital were discharged receiving high-dose aspirin.11 Researcher Hall concluded that high-dose aspirin is overused in the U.S., based on elevated rates of high-dose aspirin use in subgroups with heightened bleeding risk for whom a guideline-based indication was lacking.11
Other study data show that the use of drugs (e.g., aspirin, statin, ACE inhibitor, beta-blocker, diuretic) for secondary prevention of cardiovascular disease in post-MI patients is disappointingly low worldwide, regardless of the income level of the countries surveyed.12 One study found both inappropriate use and underuse of medications to be common in seniors taking five or more medications; often both problems were present in these individuals.13 Researchers point out that while inappropriate medication use is more frequent in patients taking many medications, underuse is also common; they advise attention regardless of the total number of medications in the medication regimen.13
One unique risk factor for ADEs in ambulatory adults is recent hospitalization. 3,14 In light of the Affordable Care Act (ACA) and the financial pressure hospitals face to avoid readmissions, health care stakeholders could flag these vulnerable individuals for MTM by a pharmacist both pre- and postdischarge. Postdischarge MTM would be scheduled as a follow-up appointment so that real-life issues encountered by the patient in the home setting regarding the administration, timing, and monitoring of medication therapy could be addressed and MRPs identified, resolved, and prevented. The following section further supports this suggestion as an appropriate and timely risk-reduction intervention.
Post-Hospital Syndrome
A recent article in the New England Journal of Medicine discusses a con cept in which patients discharged from a hospital after an acute illness experience a condition author Harlan Krumholz, MD, characterizes as a “post-hospital syndrome,” i.e., an acquired transient period of vulnerability (generalized risk for a range of adverse health events).15 Stressors noted during hospitalization included sleep deprivation, poor nourishment, pain and discomfort, mentally challenging situations, medications that alter cognition and physical function, and deconditioning secondary to bed rest or inactivity. Stressors may cause confusion and even delirium, which is associated with increased risk following discharge. Further, upon discharge, the body is unable to defend against health threats due to impaired physiological systems and depleted reserves.15
Dr. Krumholz calls for novel interventions to promote recovery. He indicates that although there is a “need to continue to improve transitional care and ensure that the condition for which a patient was initially admitted is successfully treated, we also need to focus on the factors during the hospitalization and the early recovery period that contribute to the period of vulnerability.”15
Conclusion
Biological age-related changes occurring during postmaturational life underlie an increasing vulnerability to a host of challenges that decrease seniors’ ability to survive. Pharmacists may use this knowledge, and the recent evidence of inappropriate prescribing, to target those at risk during the pre- and postdischarge phase of a hospitalization, so that MRPs may be identified, resolved, and prevented.
REFERENCES
1. Kitzman DW, Taffet G. Effects of aging
on cardiovascular structure and function. In: Halter JB, Ouslander JG,
Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:883-895.
2. Masoro EJ. Physiology of aging. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:51-58.3. Starner CI, Gray SL, Guay DR, et al. Geriatrics. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 7th ed. New York, NY: McGraw-Hill Inc; 2008:57-66.
4. Manton KG. The future of old age. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:11-17.5. Zagaria ME. Medication-related problems in seniors: risk factors and tips for appropriate prescribing. Am J Nurse Pract. 2009;13(3):23-27.
6. Zagaria ME. Assessing and monitoring medication therapy in seniors. Am J Nurse Pract. 2011;15(9/10):48-52.
7. Phelan EA, Paniagua MA, Hazzard WR.
Preventive gerontology: strategies for optimizing health across the life
span. In: Hazzard WR, Blass JP, Halter JB, et al. Principles of Geriatric Medicine and Gerontology. 5th ed. New York, NY: McGraw-Hill; 2003:85-92.
8. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Health & Aging. Whitehouse Station, NJ: Merck Research Laboratories; 2004:40-41,210-213,382-384,415,556-558,660,744.
9. Kissinger JF, Youngkin EQ. Obesity. In: Youngkin EQ, Sawin KJ, Kissinger JF, et al. Pharmacotherapeutics: A Primary Care Guide. Upper Saddle River, NJ: Pearson Prentice Hall; 2005:693-708.
10. Zagaria ME. Obesity: reality and relevance to health. US Pharm. 2009;34(9):20-24.
11. Alexander W. American Heart
Association Scientific Sessions 2012. Meeting Highlights. Aspirin after
acute myocardial infarction.
www.ptcommunity.com/ptjournal/fulltext/38/1/PTJ3801051.pdf. Accessed
February 4, 2012.
12. Yusuf S, Islam S, Chow CK, et al. Use
of secondary prevention drugs for cardiovascular disease in the
community in high-income, middle-income, and low-income countries (the
PURE Study): A prospective epidemiological survey. Lancet. 2011;378:1231-1243.
13. Steinman MA, Landefeld CS, Rosenthal GE, et al. Polypharmacy and prescribing quality in older people. J Am Geriatr Soc. 2006;54:1516-1523.
14. Hajjar E, Artz MB, Lindblad CI, et
al. Risk factors and prevalence for adverse drug reactions in an
ambulatory elderly population. J Am Geriatr Soc. 2004;52:S30-S31.
15. Krumholz HM. Post-hospital syndrome—an acquired, transient condition of generalized risk. N Engl J Med. 2013;368:100-102.
16. Guay D. The pharmacology of aging. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:138-144.
To comment on this article, contact rdavidson@uspharmacist.com.





