US Pharm. 2019;44(11):23-28.
ABSTRACT: Anxiety disorders are the most common type of psychiatric disorders and are often undertreated and underdiagnosed. Negative patient outcomes can result from poor management of patients after diagnosis. Various pharmacologic and nonpharmacologic therapies are prescribed for these patients. Patients with generalized anxiety disorder are commonly seen in the community pharmacy. By educating patients about their treatment regimens and medication adherence, as well as using Mental Health First Aid training, community pharmacists play a vital role in improving the quality of life in patients with generalized anxiety disorder.
Anxiety disorders are the most common type of psychiatric disorders and are often undertreated and underdiagnosed.1,2 Patients with generalized anxiety disorder (GAD) are frequently seen in the community pharmacy. Pharmacists can have a significant impact on the patient’s quality of life by providing medication-therapy management services including counseling on specific medications, dosing, side effects, and black box warnings, in addition to assessing medication adherence.
In 2017, an estimated 284 million people worldwide had an anxiety disorder. Approximately 2% to 3.1% of adults in the United States suffer from GAD, which involves excessive and persistent worrying that interferes with normal activities and relationships, plus physical symptoms such as restlessness, muscle tension, poor concentration, and sleeplessness.3-5 Yet more than 56% of patients affected with GAD are not receiving treatment.4 Even though patients with GAD tend to use more healthcare resources, fewer than 20% are receiving pharmacotherapy for their symptoms, leading to decreased workplace productivity.6
Treatment Guidelines
The Anxiety and Depression Association of America (ADAA), the National Institute for Health and Care Excellence (NICE), the Canadian Anxiety Guidelines Initiative Group, and the World Federation of Biological Psychiatry (WFSBP) GAD guidelines all emphasize patient preference as the main determinant when choosing among the types of treatment available, which include both psychological and pharmacologic options. In addition, patient motivation, illness severity, treatment-option availability, adverse drug effects, cost, and comorbidities should be considered to guide treatment.2,7-9
The guidelines acknowledge cognitive behavioral therapy (CBT) as first-line psychotherapy and recommend selective serotonin reuptake inhibitors (SSRIs) and selective norepinephrine reuptake inhibitors (SNRIs) for first-line pharmacotherapy.2,7-9 WFSBP specifically states that psychologic and pharmacologic therapies are often concomitant rather than alternative options.9 Commonalities among the guidelines’ recommendations for second-line pharmacotherapy include benzodiazepines, tricyclic antidepressants (TCAs), buspirone, hydroxyzine, and quetiapine; however, these therapies are not universally recommended by the guidelines.2,7-9 Specific psychological and pharmacologic options for each guideline are identified in Table 1. NICE guidelines separate GAD treatment into a stepped-care model. Of note, step 2 offers one or more psychotherapy interventions; step 3 offers either individual high-intensity psychotherapy or pharmacotherapy.8 ADAA and Canadian guidelines discuss natural, complementary remedies used in GAD treatment, although these are not widely recommended.2,7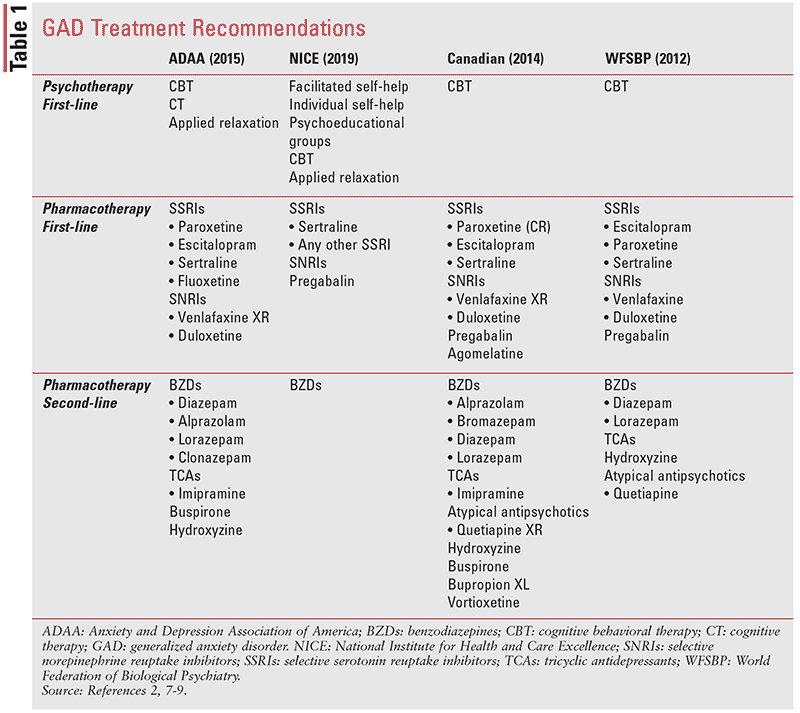
Pharmacologic Therapies
The safety and efficacy of various GAD pharmacologic treatments have been established and validated in many clinical trials.10-14 A brief summary of trials concerning first-line treatment modalities is discussed below.
Escitalopram: Davidson and colleagues performed a flexible-dose study evaluating the safety and efficacy of escitalopram in 315 GAD patients. Greater improvements in the Hamilton Rating Scale for Anxiety (HAM-A) scores that were statistically significant and clinically relevant were noted in the escitalopram group compared with the placebo group at every time point starting at Week 1 through Week 8 of the trial. A significantly greater portion of the escitalopram-treated patients were responders by Week 2 compared with placebo (P <.05). Escitalopram was well tolerated, and the rate of discontinuation was not significantly different compared with placebo.10
Baldwin and colleagues reported on a 12-week parallel-group trial with an active paroxetine reference group to assess the efficacy of fixed doses of escitalopram. The change in HAM-A scores from baseline to 12 weeks was statistically significant in all escitalopram groups compared with placebo. Escitalopram 20 mg was statistically superior to paroxetine 20 mg at Week 12 (P <.05). No statistically significant difference in the number of patients experiencing adverse effects across groups was reported.11
Sertraline: A sertraline flexible-dose 12-week study was conducted by Allgulander and colleagues comparing the efficacy and tolerability of sertraline in 378 patients with GAD. Efficacy was determined based on the decrease in HAM-A scores. Patients in the sertraline group had significantly greater efficacy at week 12 compared with placebo (P <.0001). Patients in the sertraline group had significantly higher responder rates (63% vs. 37%, P <.001).12
Venlafaxine: A 28-week trial to compare the efficacy and safety of a flexible dose of venlafaxine XR in 251 adults with GAD was conducted by Gelenberg and colleagues. Statistically significant reductions in all efficacy measures from baseline were seen in the venlafaxine SR treatment groups (P <.001). No statistically significant differences in adverse effects were seen between groups.13
Duloxetine: Rynn and colleagues studied the efficacy and safety of flexible doses of duloxetine in 327 adults with GAD in a 10-week trial. The results showed a significant decrease in HAM-A total scores in the duloxetine-treated patients as compared with placebo (P <.05). The difference in response rates (40% duloxetine vs. 32% placebo, P <.05) was also statistically significant.14
Pregabalin: The safety and efficacy of pregabalin were demonstrated in a 4-week trial versus either lorazepam or placebo, conducted by Pande and colleagues. The decreases in HAM-A scores from baseline to the study endpoint in the pregabalin treatment groups and the lorazepam treatment group were significantly greater than the decrease in scores in the placebo group. No serious adverse events were reported in the pregabalin treatment group.15
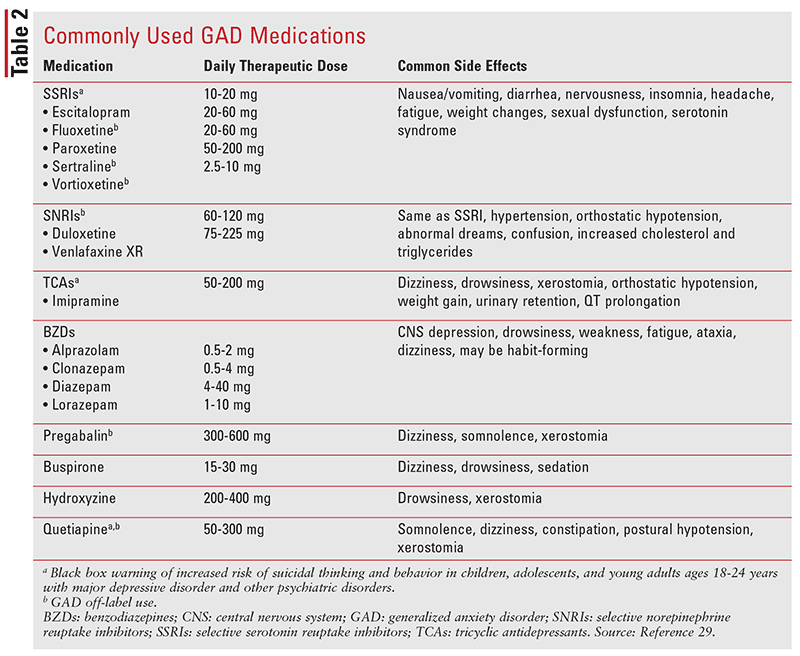
The approach to treatment as highlighted in the NICE guidelines should be patient-centered, with the patient’s preferences playing a key role in selecting pharmacotherapy.8 Patients can be initiated on either an SSRI or SNRI starting at the lowest dose and titrating up to a therapeutic dose incrementally as often as every 2 weeks until either the therapeutic dose is achieved or the highest dose the patient can tolerate is reached. If patients fail to respond after 4 to 6 weeks of therapeutic doses, the medication can be changed to another SSRI or SNRI while tapering the first agent. For patients having minimal response after 4 to 6 weeks of initial therapy, additional medication can be added to the patient’s regimen to augment their response to therapy.6 Augmentation medications include short-term use of benzodiazepines for rapid relief of severe symptoms as needed; buspirone for symptom relief in elderly patients or patients at risk for substance abuse; or pregabalin for symptom relief.2,6 Table 2 highlights dosing, side effects, and black box warnings.
Natural Products
Various natural remedies are used as complementary therapy in patients with GAD; however, most lack significant clinical evidence to support their use.16,17 Lavender oil has been shown to be possibly effective with little concern of toxicity.18,19 German chamomile, passion flower, and lemon balm have also shown benefit in patients with GAD.20,21 These products are available in several forms, and dosages vary depending on the dosage form used. Safety issues may limit their use in patients with GAD.
Nonpharmacologic Therapies
A number of psychological approaches have shown effectiveness in treating GAD. Of these, CBT has the strongest evidence to support its use.22 CBT involves a process of identifying negative thoughts and behaviors that trigger or perpetuate anxiety and replacing them with positive ones. A course of CBT can include therapist involvement, individual or groups sessions, or self-directed strategies. Relaxation techniques including mindfulness and meditation are widely used. Self-help tools—including books, internet programs, videos, podcasts, and smart-phone applications may be helpful, but their efficacy has not been rigorously studied.23
Although CBT may precede or augment medication, the preferences of the patient are still paramount. Some patients do not have the time or the means to see a therapist, may not be motivated to follow-up and keep appointments, or may be concerned about possible stigma associated with seeing a therapist or taking medications. Conversely, some patients only want pharmacologic treatment options.2,7,8,24
Patient Education
Pharmacists can provide education about lifestyle modifications to help patients self-manage anxiety. Patients should be encouraged to participate in regular physical activity, which may have a calming effect, improve sleep and increase in self-confidence.23 Enhanced mood results from endorphins being released during exercise. Focusing on the physical activity itself can replace anxious thoughts even with a simple exercise, such as playing catch. Pharmacists should counsel patients on lifestyle modifications, such as ways to limit caffeine and alcohol. Owing to its stimulant effects, caffeine can precipitate anxiety. In addition, alcohol withdrawal may worsen anxiety in patients who are chronic users. Other medications that can exacerbate or worsen anxiety should be discussed with patients. These medications include, but are not limited to, pseudoephedrine, levothyroxine, prednisone, albuterol, theophylline, clonidine, ibuprofen, amphetamines, and quinolone antibiotics.1,23
Patient medication adherence is key to successful treatment of psychiatric disorders, yet people with these disorders are more likely to be nonadherent.25 Community pharmacists can positively influence adherence through patient education.26 During initial consultation, pharmacists typically explain the use of the medication, teach patients how to take it, and review the most common side effects.26 It is particularly important for GAD patients to understand that it can take several weeks to achieve the full therapeutic effect, so adherence to medications is critical. Patients should also be counseled not to abruptly stop the medication, due to the possibility of discontinuation syndrome; physical effects include gastrointestinal and flu-like symptoms, problems with balance, and sleep disorders.25 Discontinuation syndrome can occur with most SSRIs and SNRIs, with the exception of fluoxetine.1
Although pharmacists often devote more time to counseling a patient during the initial medication fill, it is imperative to continue assessing adherence, efficacy, and side effects with each refill. Asking the patient open-ended questions and using behavioral interventions such as motivational interviewing are two effective counseling strategies. Consistent monitoring and education promotes patient adherence.25
Mental Health First Aid
Community pharmacists are being recognized as essential resources in improving treatment outcomes of mental health disorders such as GAD. The National Council for Behavioral Health and the American Pharmacists Association (APhA) have recently collaborated to provide Mental Health First Aid (MHFA) training to pharmacists.27,28 Participants are taught to identify risk factors and warning signs for mental-health concerns and learn how to help patients in crisis and noncrisis situations. MHFA training may allow more patients with GAD to be identified, referred for appropriate treatment, and monitored. This practice is becoming increasingly implemented in the community setting. All community pharmacists should provide contact information for local mental health services and direct patients to websites and hotlines for additional education and support as listed in Table 3.
Conclusion
Community pharmacists can positively affect mental-health outcomes and play a vital role in the successful management of patients with GAD by educating them about pharmacologic and nonpharmacologic treatments, lifestyle modifications, and medication adherence. Through their frequent interactions with patients, community pharmacists, especially those who have MHFA training, are uniquely positioned to recognize mental illness. Through medication-therapy management, community pharmacists can provide recommendations and direct patients to reliable educational resources.
REFERENCES
1. Melton ST, Kirkwood CK. Anxiety disorders: generalized anxiety, panic, and social anxiety disorders. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: a Pathophysiologic Approach. 10th ed. New York, NY: McGraw-Hill; 2017:1079-1098.
2. Katzman MA, Bleau P, Blier P, et al. Canadian Anxiety Guidelines Initiative Group. Canadian clinical practice guidelines for the management of anxiety, posttraumatic stress and obsessive-compulsive disorders. BMC Psychiatry. 2014;14(suppl 1):S1-S83.
3. National Institute of Mental Health. Anxiety disorders. Updated July 2018. www.nimh.nih.gov/health/topics/anxiety-disorders/index.shtml. Accessed August 27, 2019.
4. Anxiety and Depression Association of America. Facts and statistics. https://adaa.org/about-adaa/press-room/facts-statistics. Accessed August 27, 2019.
5. American Psychiatric Association. What are anxiety disorders? Updated January 2017. www.psychiatry.org/patients-families/anxiety-disorders/what-are-anxiety-disorders. Accessed August 27, 2019.
6. Kehoe WA. Generalized anxiety disorder. In: Dong BJ, Elliott DP, eds. ACSAP 2017 Book 2 Neurologic/Psychiatric Care. Lenexa, KS: ACCP; 2017:7-27.
7. Anxiety and Depression Association of America, ADAA. Clinical practice review for GAD. https://adaa.org/resources-professionals/practice-guidelines-gad. July 2, 2015 (revised). Accessed July 12, 2019.
8. National Institute for Health and Care Excellence. Generalised anxiety disorder and panic disorder in adults: management in primary, secondary, and community care. Last updated July 2019. www.nice.org.uk/Guidance/CG113. Accessed August 26, 2019.
9. Bandelow B, Sher L, Bunevicius R, et al. Guidelines for the pharmacologic treatment of anxiety disorders, obsessive-compulsive disorder and posttraumatic stress disorder in primary care. Int J Psychiatry Clin Pract. 2012;16:77-84.
10. Davidson JRT, Bose A, Korotzer A. Zheng H. Escitalopram in the treatment of generalized anxiety disorder: double-blind, placebo controlled, flexible-dose study. Depress Anxiety. 2004;19(4):234-240.
11. Baldwin DS, Huusom AK, Maehlum E. Escitalopram and paroxetine in the treatment of generalised anxiety disorder: randomised, placebo-controlled, double-blind study. Br J Psychiatry. 2006;189:264-272.
12. Allgulander C, Dahl AA, Austin C, et al. Efficacy of sertraline in a 12-week trial for generalized anxiety disorder. Am J Psychiatry. 2004;161:1642-1649.
13. Gelenberg AJ, Lydiard RB, Rudolph RL, et al. Efficacy of venlafaxine extended-release capsules in nondepressed outpatients with generalized anxiety disorder: a 6-month randomized controlled trial. JAMA. 2000;283:3082-3088.
14. Rynn M, Russell J, Erickson J, et al. Efficacy and safety of duloxetine in the treatment of generalized anxiety disorder: a flexible-dose, progressive-titration, placebo-controlled trial. Depress Anxiety. 2008;25:182-189.
15. Pande AC, Crockatt JG, Feltner DE, et al. Pregabalin in generalized anxiety disorder: a placebo-controlled trial. Am J Psychiatry. 2003;160:533-540.
16. Fedotova J, Kubatka P, Busselberg D, et al. Therapeutical strategies for anxiety and anxiety-like disorders using plant-derived natural compounds and plant extracts. Biomed Pharmacother. 2017;95:437-446.
17. Sibley C. Ten natural remedies to consider for treating anxiety. Pharmacy Times. 2017. www.pharmacytimes.com/contributor/cate-sibley-pharmd/2017/10/10-natural-remedies-to-consider-for-treating-anxiety. Accessed July 12, 2019.
18. Kasper S. An orally administered lavandula oil preparation (Silexan) for anxiety disorder and related conditions: an evidence based review. Int J Psychiatry Clin Pract. 2013;17 Suppl 1:15-22.
19. Generosa MB, Soares A, Tiair, IT, et al. Lavender oil preparation (Silexan) for treating anxiety: an updated meta-analysis. J Clin Psychopharmacol. 2017;37:115-117.
20. Mao JJ, Xie SX, Keefe JR, et al. Long-term chamomile (Matricaria chamomilla L.) treatment for generalized anxiety disorder: a randomized clinical trial. Phytomedicine. 2016;23:1735-1742.
21. Food, Herbs & Supplements Database. Natural medicines. Stockton, CA: Therapeutic Research Center; 2019. naturalmedicines.therapeuticresearch.com. Accessed August 23, 2019.
22. Cuijpers P, Sijbrandij M, Koole S, et al. Psychological treatment of generalized anxiety disorder: a meta-analysis. Clin Psychol Rev. 2014;34:130-140.
23. DeMartini J, Patel G, Fancher TL. Generalized anxiety disorder. Ann Intern Med. 2019;170:ITC49-ITC64.
24. Locke AB, Kirst N, Schultz CG. Diagnosis and management of generalized anxiety and panic disorder in adults. Am Fam Physician. 2015:91:617-624.
25. Semahegn A, Torpey K, Manu A, et al. Psychotropic medication non-adherence and associated factors among adult patients with major psychiatric disorders: a protocol for a systematic review. Syst Rev. 2018;7(1):10.
26. Moore CH, Kyle JA. The role of the community pharmacist in mental health. US Pharm. 2018;43(11):13-20.
27. National Council for Behavioral Health. Pharmacists are untapped resource in treatment of mental illness. www.thenationalcouncil.org. Accessed August 3, 2019.
28. Walgreens forms unique collaboration with National Council for Behavioral Health and American Pharmacists Association to offer mental health first aid training for pharmacists and team members [news release]. Deerfield, IL; May 1, 2019: Walgreens. news.walgreens.com/press-releases/general-news/walgreens-forms-unique-collaboration-with-national-council-for-behavioral-health-and-american-pharmacists-association-to-offer-mental-health-first-aid-training-for-pharmacists-and-team-members.htm. Accessed August 27, 2019.
29. Lexicomp Drug Information Handbook, 28th ed. Hudson, Ohio: Wolters Kluwer Clinical Drug Information, Inc; 2019.
To comment on this article, contact rdavidson@uspharmacist.com.