An age-associated, less-capable immune response to an infectious challenge renders seniors more susceptible to infection. In addition to waning immunity, there are other contributors that predispose the elderly to infection. Among them are malnutrition; comorbidities such as diabetes, lung disease, peripheral vascular disease, renal failure, and Alzheimer’s disease; and medications that suppress inflammation and/or immune responses.1 Cumulative risk factors lead to higher infection risk in the elderly and greater morbidity and mortality associated with infection, particularly pneumococcal pneumonia, influenza virus infections, and urinary tract infections.2-4
Although the mechanism of action of an antibiotic is selectively toxic to an invading organism, the potential for antibiotic-associated adverse effects is not limited by this selectivity.5 For example, the antibiotic may induce an allergic reaction or produce toxicity in a manner unrelated to the agent’s antimicrobial activity, and that effect may be considered a complication of therapy (see below).5 Additionally, some antibiotic-induced adverse reactions occur rarely and appear to be unique to the compound administered.
In order that dosing regimens may be designed with a targeted approach, the study of pharmacodynamics is utilized in distinguishing the relationship between the modifIcation of antimicrobial drug concentrations over time and their therapeutic and toxicologic effects.6 Dosing regimens are not absolute, however, since the safety of a particular antibiotic is related not only to the fundamental nature of the agent but also to patient factors that can predispose an individual to adverse reactions, toxicity, and other complications of therapy ( TABLE 1 ). In seniors, age-related physiological changes and complex medication regimens alter antibiotic pharmacokinetics and require dosage adjustments.
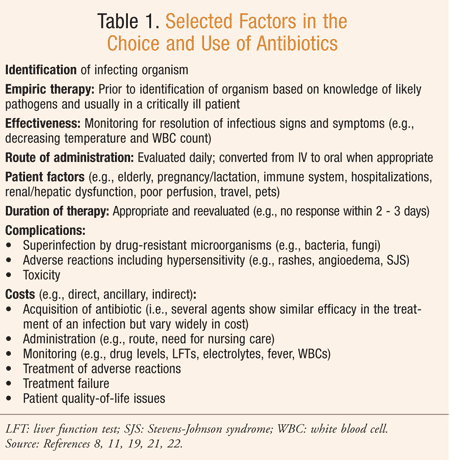
Pharmacists, by using evidence-based data, can help identify, resolve, and prevent adverse reactions and complications of antibiotic therapy. TABLE 1 , and the sections below addressing adverse reactions more commonly seen in seniors and general concepts for the prevention of antibiotic-associated adverse reactions, can assist with medication therapy management (MTM) and the development of pharmaceutical care plans for vulnerable seniors. In addition, TABLE 2 , Selected Adverse Effects and Dosing Considerations of Antibiotics (available at www.uspharmacist.com), and the table noted in RESOURCE , which discusses major drug interactions with antimicrobials, including mechanism of effect and clinical management, are recommended.

Antibiotic-Related Adverse Events in Seniors
Dizziness, the troubling sensation of spinning, unsteadiness, or light-headedness, and vertigo, a false sensation of movement of the body or the environment, can be caused by malfunction of the vestibular labyrinth (inner ear) secondary to certain antibiotics (e.g., aminoglycosides).7 Other symptoms and signs of vestibular damage include nausea, vomiting, nystagmus, and ataxia.8 These disturbances can be especially problematic for an elderly individual in whom balance and stability may already be challenging secondary to vision problems, neuropathy, or arthritis.
A decline in the number of functioning nephrons that, in turn, results in decreased renal function is the major physiological change in persons over the age of 65 years.9 This decline in renal function usually manifests by an increase in adverse effects secondary to antimicrobials that are renally eliminated. For example, aminoglycoside-induced renal toxicity may present earlier in the course of therapy in an older adult than in a younger individual.10
While an adverse reaction frequently requires the discontinuation of the causative agent and the introduction of another organism-susceptible antibiotic, in some cases no alternatives exist.8 Less serious infections may allow antibiotic discontinuation with close monitoring; however, when treatment cannot be discontinued due to a life-threatening infection, an adverse reaction is managed symptomatically.11
Specific examples of some antibiotic-related adverse events that appear to occur more commonly in the elderly include:12,13
Aminoglycoside-induced renal toxicity (often reversible) and vestibular and auditory toxicity (often irreversible): Risk factors for renal, vestibular, and auditory toxicity include older age; frequent or very high dosages; very high drug blood levels; long duration of therapy (e.g., >3 days); preexisting renal disorder; and concomitant administration of amphotericin B, cyclosporine, or vancomycin.8 The coadministration of contrast agents increases the risk for renal toxicity, while coadministration of loop diuretics (e.g., bumetanide, ethacrynic acid, furosemide, torsemide) and preexisting hearing problems increase the risk for auditory toxicity.8
Antibiotic-associated pseudomembranous colitis: Clostridium difficile–associated diarrhea has a disease spectrum ranging from mild diarrhea with little or no inflammation to severe colitis often associated with pseudomembranes, which are adherent to necrotic colonic epithelium (pseudomembranous colitis).10 C difficile occurs most frequently in geriatric patients in hospitals and nursing homes, potentially due to environmental contamination transferred on the hands of facility staff.14
Pseudomembranous colitis may also be caused by an overgrowth of underlying C difficile; overgrowth is referred to as a superinfection by drug-resistant microorganisms and is considered a complication of antibiotic therapy.5 Of note, there is a strong association between fluoroquinolone use and C difficile–associated diarrhea and pseudomembranous colitis, especially due to the hypervirulent C difficile ribotype 027, with outbreaks currently reported in the U.S., Canada, and Europe.8,15,16 Antibiotic-associated diarrhea with no evidence of C difficile infection occurs in a smaller number of patients.10 While virtually all antibiotics have been implicated, the most common are clindamycin, cephalosporins, ampicillin or amoxicillin, and, most recently, fluoroquinolones; the less common are other penicillins and erythromycin.8,17
Trimethoprim (TMP) and sulfamethoxazole (SMX)–induced hyperkalemia and blood dyscrasias: TMP can decrease renal tubular potassium excretion, leading to hyperkalemia. Hyperkalemia can be problematic in patients who have renal impairment or cardiac disease and who may be receiving drugs that increase potassium, such as ACE inhibitors and potassium-sparing diuretics.15 Folic acid deficiency is one of the most common vitamin deficiencies in the U.S.; poor eating habits make this deficiency more common in the elderly. Folic acid deficiency may lead to megaloblastic anemia.18
Fluoroquinolone-related seizures: Fluoroquinolones are associated with central nervous system (CNS) stimulatory effects; the most prominent CNS effects are headache, dizziness, and light-headedness. While seizures are rare, these agents should be used with caution or avoided in patients with CNS disorders, such as epilepsy.5,8 Ciprofloxacin interferes with theophylline metabolism and may evoke seizures.5
Doxycycline-related esophageal ulcerations and strictures: While the esophagus is not easily damaged, the esophageal lining may incur erosion from gradual insult over months to years secondary to gastroesophageal reflux and many drugs, including antibiotics (e.g., doxycycline, clindamycin).7 Since seniors are more likely to have comorbidities involving multiple medication therapy, esophageal damage from medications (e.g., aspirin, bisphosphonates, nonsteroidal anti-inflammatory drugs [NSAIDs]) is more common among these individuals, and the concomitant administration of a potentially offending antibiotic should be considered and avoided if possible. A doxycycline capsule or tablet should be administered orally with at least 8 oz. of water, and the patient should sit up for at least 30 minutes after taking it to reduce the risk of esophageal irritation and ulceration.16
Acute liver injury secondary to prolonged therapy with amoxicillin plus clavulanic acid: Amoxicillin plus clavulanic acid is considered one of the drugs of choice in the outpatient treatment of community-acquired pneumonia in the elderly.16 When prolonged therapy is warranted, periodic monitoring of renal, hepatic, and hematologic function is recommended.16
Complications of Antibiotic Therapy
Complications can occur and may be unrelated to the drug ’ s antimicrobial activity; these include:
Superinfections, resulting from a difficult-to-treat overgrowth of opportunistic organisms (e.g., fungi or resistant bacteria), usually occur with broad-spectrum antimicrobials, prolonged use, or combinations of agents that alter the normal microbial flora of the upper respiratory, intestinal, and genitourinary tracts.5 An example is C difficile–associated diarrhea and pseudomembranous colitis secondary to fluoroquinolone use.
Hypersensitivity adverse reactions to an antibiotic (e.g., penicillin) or its metabolic products can frequently occur, causing serious problems ranging from urticaria (hives) to anaphylactic shock.5 In the case of a delayed dermatologic reaction to penicillin (i.e., rash), the patient can generally receive a cephalosporin.19 Patients with a history of anaphylaxis to penicillin, however, should not be given any beta-lactam again (including for skin testing), except in a very rare situation when no alternative can be found.8 In this case, special precautions and desensitization regimens must be used.8 Alternatives to the cephalosporins include aztreonam, fluoroquinolones, sulfonamide antibiotics, or vancomycin, depending on the type of coverage required.19
Direct toxicity results from high serum levels of certain antibiotics that directly affect cellular processes in the host. An example of the result of direct toxicity is ototoxicity secondary to aminoglycosides.5
Prevention of Antibiotic-Associated Adverse Reactions
Preventing the development of antibiotic-related adverse reactions may be accomplished by 1) judiciously administering antimicrobials and avoiding antibiotic abuse by patients and physicians; 2) attempting to identify the specific etiology of a respiratory tract infection to avoid the excessive prescribing of multiple or empirical antibiotics; 3) modifying empirical treatment upon determining the cause of the infection; and 4) limiting treatment duration to recommended practice guidelines.12Specific recommendations to decrease the toxicity potential of antibiotics consist of: 20,25
• Infusing vancomycin over 2 hours when appropriate
• Administering aminoglycosides once daily when appropriate
• Advising patients to swallow oral doxycycline with copious amounts of water and to avoid taking it at bedtime
• Reviewing drug-allergy history with patients and reviewing the daily medication regimen with a goal of optimum therapeutic benefit and diminished potential for adverse event occurrence.
Conclusion
An age-related decline in the immune system, in conjunction with comorbidities and other factors, increases susceptibility to infection; age-related physiological changes predispose seniors to the risk of antibiotic-related adverse reactions as well. Considering evidence-based data, in conjunction with clinical experience and judgment, is an important aspect of individualizing antibiotic regimens for seniors. With anticipation and prevention of antibiotic-associated adverse reactions, positive therapeutic outcomes in addition to positive pharmacoeconomic and health-related quality-of-life outcomes may be achieved.
REFERENCES
1. Zagaria ME. Predisposition to infection in the elderly. US Pharm. 2011;36(8):28-32.
2. Larbi A, Franceschi C, Mazzatti D, et al. Aging of the immune system as a prognostic factor for human longevity. Physiology (Bethesda) 2008; 23:64-74.
3. Smith PW, Roccaforte JS, Daly PB. Infection and immune response in the elderly. Ann Epidemiol. 1992;2(6):813-822.
4. High KP. Infection in the elderly. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:1508-1515.
5. Harvey RA, Champe PC, eds. Pharmacology. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2009:347-406.
6. Maglio D, Nicolau DP, Nightingale CH. Impact of pharmacodynamics on dosing of macrolides, azalides, and ketolides. Infect Dis Clin North Am. 2003;17(3):563-77, vi.
7. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Health & Aging. Whitehouse Station, NJ: Merck Research Laboratories; 2004:232,738.
8. Beers MH, Porter RS, Jones TV, et al. The Merck Manual of Diagnosis and Therapy. 19th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2011:1180-1225.
9. Stalam M, Kaye D. Antibiotic agents in the elderly. Infect Dis Clin North Am. 2004;18:533-549.
10. Wald A. The large bowel. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010: 661-677.
11. Chin-Hong PV, Guglielmo BJ. Common problems in
infectious diseases & antimicrobial therapy. In: McPhee SJ,
Papadakis MA, Rabow MW, eds. 2013 Current Medical Diagnosis & Treatment. 51st ed. New York, NY: McGraw Hill Medical; 2013:1298-1305.
12. Antibiotic side effects. Medscape News. Pharmacists. www.medscape.com/viewarticle/410873_1. Accessed March 13, 2013.
13. Millan J, Gleckman R. Selecting the right antibiotics for elderly patients. J Crit Illness. 1997;12:590-598.
14. McFarland LV, Mulligan ME, Kwok RY, Stamm, WE. Nosocomial acquisition of Clostridium difficile infection. N Engl J Med.
1989;320:204-210.
15. McDonald LC, Killgore GE, Thompson A, et al. An epidemic toxin gene variant strain of Clostridium difficile. N Engl J Med. 2005;353:2433-2441.
16. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 17th ed. Hudson, OH: Lexi-Comp, Inc; 2012:1069-1072.
17. Settle CD, Wilcox MH. Review article: antibiotic-induced Clostridium difficile infection. Aliment Pharmacol Ther. 1996;10:835-841.
18. Cook K, Ineck BA, Lyons WL. Anemias. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Inc; 2011:1717-1740.
19. Burgess DS. Antimicrobial regimen selection. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Inc; 2011: 1813-1823.
20. Gleckman RA, Borrego F. Adverse reactions to antibiotics: clues for recognizing, understanding, and avoiding them. Postgrad Med. 1997;101:97-108.
21. Boucher HW, Talbot GH, Bradley JS, et al. Bad bugs, no
drugs: no ESKAPE! An update from the Infectious Diseases Society of
America. Clin Infect Dis. 2009;1:1-12.
22. Drusano GL. Antimicrobial pharmacodynamics: critical interactions of ‘bug and drug.’ Nat Rev Microbiol. 2004;2(4):289-300.
23. Sheehan G, Chew NSY. The history of quinolones. In: Ronald AR, Low DE, eds., Fluoroquinolone Antibiotics. Basel, Switzerland: Birkhauser Verlag; 2003:1-10.
24. Zagaria ME. Cutaneous adverse reactions: Stevens-Johnson syndrome. US Pharm. 2008;33(4):20-26.
25. Epocrates Essential and Rx Pro. Version 4.5. Epocrates.com. April 3, 2013.
26. Roujeau JC, Kelly JP, Naldi L, et al. Medication use
and the risk of Stevens-Johnson syndrome or toxic epidermal necrolysis. N Engl J Med. 1995;333:1600-1607.
To comment on this article, contact rdavidson@uspharmacist.com.






