US Pharm. 2017;42(4):32-36.
ABSTRACT: Less than 50% of the U.S. population obtains the seasonal influenza vaccine, and the vaccine does not confer perfect immunity. There are three types of influenza, plus numerous variations. Practitioners should be confident in the use of antiviral agents in patients with influenza. The most recent guidelines recommend the use of nonpharmacologic management and neuraminidase inhibitors to either prevent the transmission of influenza or treat the infection. Pharmacotherapy is based on an understanding of which patients are at high risk for complications—including immunocompromised persons, those aged 65 years and older, and those younger than 2 years of age—and prompt treatment upon diagnosis.
Influenza viruses remain the most common cause of respiratory infections and result in high morbidity and mortality, especially among young children, the elderly, and immunocompromised persons. The virus consists of three types—influenza A, influenza B, and influenza C—but influenza C is rarely seen. Influenzas B and C are isolated mostly in humans, whereas influenza A, the most common type, infects several mammals, including—but not limited to—birds, swine, and humans.1
Influenza pandemics date back to the 1700s; the deadliest one, which occurred in 1918, was responsible for 675,000 deaths in the United States.1 The most recent pandemic, in 2009, was due to the H1N1 influenza virus (also known as swine flu) and caused 12,469 deaths in the U.S.2 At the end of 2016, the hospitalization rate was 3.1 per 100,000 population, with the greatest percentage of adults aged 65 years and older.3
Prevention is a key component in reducing the rates of influenza-related death and hospitalization. Aggregate data from the CDC, via the National Immunization Survey-Flu and the Behavioral Risk Factor Surveillance System, however, indicate that only 41.7% of the population received seasonal influenza coverage in 2015–2016.4 This leaves more than one-half of the U.S. population without preventive care.
Pathophysiology
Influenza A and B have similar structures: a negative-strand RNA consisting of eight gene segments encapsulated and covered by the proteins hemagglutinin (HA), neuraminidase (NA), and matrix 2.1 The HA protein recognizes and attaches itself to a host cell, where the virus RNA traps itself in an endosome, releasing its viral particles into the nucleus of the host cell for replication.5,6 The influenza A virus first replicates in the nasopharynx and eventually moves replication to the upper and lower respiratory tracts. Infected individuals are contagious for up to a week after symptoms occur; this is because viral replication declines slowly and the virus is shed at least 7 days after illness.1,7
Influenza A is divided into two subgroups based on HA and NA surface proteins. There are 18 different HA proteins and 11 NA proteins, and each influenza A virus consists of one HA surface protein and one NA surface protein.8 The different HA and NA proteins and their combinations are from viral mutations occurring during the replication process by two different mechanisms.8
First, an antigenic drift can occur in which the virus creates small genetic changes during replication. These changes create a virus that is highly similar to its original, since both share the same antigenic properties. Over time, the changes render the virus unrecognizable to human antibodies.9 The second mechanism, known as antigenic shift, causes a pronounced alteration in the influenza A virus.9 The new virus has different antigenic properties and different HA and/or NA proteins.9 Antigenic shift is one of the reasons for the 2009 influenza pandemic.9
After infection, the immune system creates antibodies against the HA and NA surface proteins of the specific virus.1 A vaccine of the attenuated or live virus is introduced into the body for the production of antibodies against the influenza antigens.10,11 The antigenic shift and drift to the RNA virus render the development of the influenza vaccine prognostic.10 Therefore, researchers use data collected from previous years and trends to determine which three or four viral strains should constitute the vaccine’s composition.11,12
The CDC developed a surveillance system to track the progression of the influenza virus each year to aid in vaccine development. Data collected include the location and timing of the viral activity, influenza types and subtypes, any antigenic changes or mutations, reports of influenza-like illnesses, influenza-related hospitalizations, and influenza-related deaths.13 For the 2016–2017 season, influenza A (H3N2) has been reported most commonly, followed by influenza A (H1N1pdm09); however, some influenza B types have also been reported.3
Vaccination is an effective measure of prevention against the influenza virus, having 70% to 90% efficacy against influenza A.1 However, with the continuous small changes caused by antigenic drift, a vaccinated person still could become infected with the influenza virus, and treatment may be deemed appropriate.9
Clinical Course
The symptoms associated with the influenza virus resemble those of bacterial infections and the common cold; the differential diagnosis is an important consideration in caring for patients. Unlike the common cold, influenza symptoms are usually abrupt, with the first signs being a quick-onset fever (100-104°F) and cough.14 The cough is usually dry and severe, causing chest discomfort. Other symptoms include severe myalgia, arthralgia, fatigue, malaise, decreased appetite, and headache. Nasal congestion, sneezing, and sore throat are more prevalent in patients with the common cold, and influenza’s severe dry cough and fatigue typically instigate treatment.14
For influenzas A and B, diagnosis is usually made with a nasopharyngeal or nasal swab. Rapid influenza diagnostic tests (RIDTs) detect viral antigens and are among the most commonly used diagnostic tools because results are available rapidly (<15 minutes). However, the test’s sensitivity of 50% to 70% leads to many false-negatives, and specimens used for RIDTs should be collected within 3 to 4 days (or sooner) of symptom onset.15,16
The reverse transcription polymerase chain reaction (RT-PCR) test remains the gold standard for influenza diagnosis because of its high specificity and sensitivity.16 In addition to nasopharyngeal swabs, several specimens—including throat swabs, bronchial wash, and sputum—may be used. Samples from the lower respiratory tract can detect a positive diagnosis after 4 days post symptom onset; however, it may take 1 to 8 hours to get results.15
Once influenza is diagnosed, nonpharmacologic and pharmacologic treatment options should be considered to manage symptoms and decrease the duration and severity of the virus.
Treatment of Influenza
Nonpharmacologic Treatment: Nonpharmacologic recommendations for influenza are bed rest, avoidance of other persons, and hydration. Fluids should be consumed throughout the illness to prevent complications from dehydration. Acetaminophen or ibuprofen may be used to relieve fever, headache, and muscle aches. However, some patients may benefit from antiviral treatment (see Pharmacotherapy Considerations section).17-19
Pharmacologic Agents: Antiviral medications with activity against influenza viruses are an important adjunct to vaccination for control of the influenza virus. Oseltamivir (Tamiflu), inhaled zanamivir (Relenza), and IV peramivir (Rapivab) are the currently recommended agents for influenza.20-22 These drugs, which are neuraminidase inhibitors with activity against both influenza A and influenza B, work by selectively inhibiting the neuraminidase enzyme, thereby preventing the release of viral particles from infected cells. These medications may be used for treatment, but only oseltamivir and zanamivir may be used for treatment and chemoprophylaxis. The chemoprophylaxis dosages for these drugs are lower than the treatment dosages; however, the therapy duration is longer (TABLE 1).20-23 Oseltamivir and zanamivir are indicated for use in adults and children; peramivir has not been FDA-approved for use in children.19,23
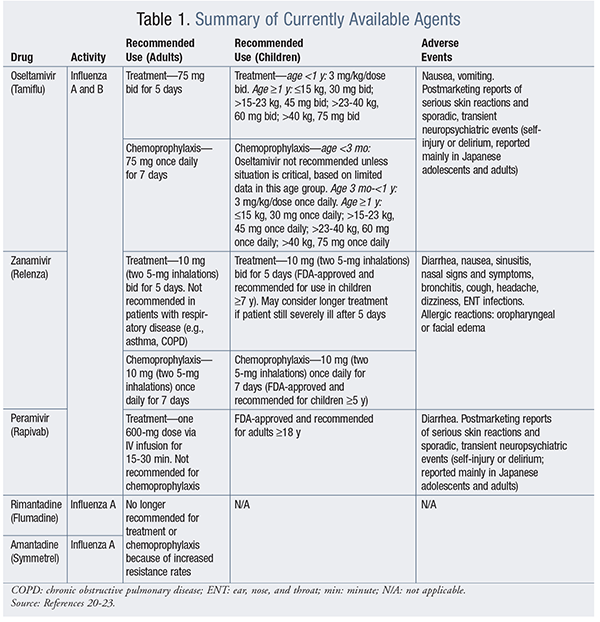
Besides the neuraminidase inhibitors, two other products are available: amantadine (Symmetrel) and rimantadine (Flumadine), both of which are adamantane antiviral agents with activity against influenza A viruses. These agents exert an inhibitory effect on influenza A subtypes (H1N1, H2N2, and H3N2) early in the viral replicative cycle. However, they are no longer recommended for treatment and prevention of influenza because of the increased rates of resistance (>99%) in influenza A types H3N2 and H1N1.19,23
Pharmacotherapy Considerations
Early treatment with the previously mentioned antivirals can shorten the duration of influenza symptoms by 1/2 day to 3 days and may reduce the risk of complications.24 The greatest clinical benefit is seen when antiviral treatment is initiated within 48 hours of illness onset. It is also important to correctly identify patients who meet parameters for either chemoprophylaxis or treatment so that they receive the correct dosage and duration of therapy.19
Chemoprophylaxis should be considered in adults and children aged 1 year and older who are at high risk for developing influenza complications and for whom influenza vaccination is contraindicated, unavailable, or expected to have low effectiveness (e.g., significantly immunocompromised persons).18,19 Chemoprophylaxis should also be considered in this population when the vaccination has not yet been administered and influenza has been detected within the community. Unvaccinated adults—including healthcare workers—and children aged ≥1 year who are in close contact with persons at high risk for developing influenza complications during periods of influenza activity should be considered for chemoprophylaxis, as should all vaccinated and unvaccinated persons in institutions experiencing influenza outbreaks.19
Antiviral treatment should be initiated in all persons with laboratory-confirmed or highly suspected influenza virus infection, including those at high risk for developing complications (TABLE 2).19 Patients who require hospitalization for influenza regardless of vaccination status or underlying illness should also receive treatment. Outpatients at high risk for complications whose illness is not improving and who have a positive influenza test result may be candidates for influenza treatment. The same is true for outpatients who are not at increased risk, but wish to shorten the duration of illness or are in close contact with someone at high risk for complications secondary to influenza infection.19

When the appropriate drug for chemoprophylaxis or treatment is being selected, local patterns of influenza circulation in the community throughout the influenza season should be considered. Oseltamivir (Tamiflu), zanamivir (Relenza), and peramivir (Rapivab) were the antivirals recommended for the 2016–2017 influenza season.19 A generic oseltamivir was approved by the FDA in August 2016, giving patients a less expensive option.25
In patients who are mechanically ventilated or critically ill, oseltamivir may be administered via nasogastric or orogastric (NG/OG) tube. The powder from capsules should be dissolved in 20 mL of Sterile Water and injected down the NG/OG tube, followed by a 10-mL Sterile Water flush.20
Emergent Situations
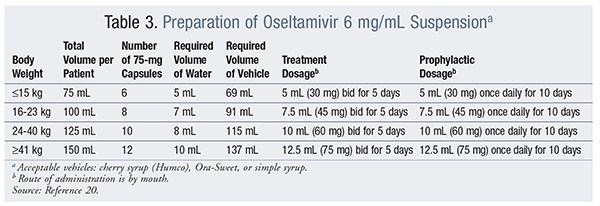
Antiviral therapy may be in short supply during pandemics. If an emerging public-health threat is identified for which no licensed or approved product exists, the Project BioShield Act of 2004 authorizes the FDA Commissioner to issue an Emergency Use Authorization so that appropriate countermeasures can be taken quickly to protect the U.S. population’s safety. However, in certain circumstances in which a commercial oral suspension is not available, the age-appropriate strength is not available, or other antiviral products are not available, oseltamivir (Tamiflu) may be extemporaneously prepared and administered through an NG/OG tube in order to meet the patient’s needs.26 If the commercially prepared oral suspension is not available, the manufacturer recommends compounding a 6 mg/mL suspension in emergency situations. See TABLES 3 and 4 for detailed information.

Conclusion
Despite advances in preventive care, infection with the influenza virus sometimes occurs. In such cases, practitioners must be able to quickly identify patients at high risk for developing complications in order to lessen the morbidity and mortality associated with the influenza virus. Some patients may require chemoprophylaxis to prevent infection. The agents for treatment and chemoprophylaxis are the same, and pharmacists should play an active role in ensuring that the correct dosage is used for the correct indication.
REFERENCES
1. Taubenberger JK, Morens DM. The pathology of influenza virus infections. Annu Rev Pathol. 2008;3:499-522.
2. CDC. CDC estimates of 2009 H1N1 influenza cases, hospitalizations and deaths in the United States. www.cdc.gov/h1n1flu/estimates_2009_h1n1.htm. Accessed December 29, 2016.
3. CDC. Weekly US influenza surveillance report: 2016-2017 season, week 51 ending December 24, 2016. www.cdc.gov/flu/weekly/weeklyarchives2016-2017/Week51.htm. Accessed March 8, 2017.
4. Santibanez TA, Kahn KE, Zhai Y, et al. Flu vaccination coverage, United States, 2015–2016 influenza season. www.cdc.gov/flu/fluvaxview/coverage-1516estimates.htm. Accessed March 3, 2017.
5. Luo M. Influenza virus entry. Adv Exp Med Biol. 2012;726:201-221.
6. Lakadamyali M, Rust MJ, Zhuang X. Endocytosis of influenza viruses. Microbes Infect. 2004;6:929-936.
7. CDC. Influenza (flu): information for schools. www.cdc.gov/flu/school/qa.htm. Accessed December 30, 2016.
8. CDC. Types of influenza viruses. www.cdc.gov/flu/about/viruses/types.htm. Accessed January 14, 2017.
9. CDC. How the flu virus can change: “drift” and “shift.” www.cdc.gov/flu/about/viruses/change.htm. Accessed December 30, 2016.
10. Hunt R. Vaccines: past successes and future prospects. Virology. www.microbiologybook.org/lecture/vaccines.htm. Accessed January 14, 2017.
11. Sedova ES, Shcherbinin DN, Migunov AI, et al. Recombinant influenza vaccines. Acta Naturae. 2012;4:17-27.
12. CDC. Selecting viruses for the seasonal influenza vaccine. www.cdc.gov/flu/about/season/vaccine-selection.htm. Accessed January 14, 2017.
13. Thompson WW, Comanor L, Shay DK. Epidemiology of seasonal influenza: use of surveillance data and statistical models to estimate the burden of disease. J Infect Dis. 2006;194(suppl 2):S82-S91.
14. Montalto NJ. An office-based approach to influenza: clinical diagnosis and laboratory testing. Am Fam Physician. 2003;67:111-118.
15. CDC. Influenza signs and symptoms and the role of laboratory diagnostics. www.cdc.gov/flu/professionals/diagnosis/labrolesprocedures.htm. Accessed January 14, 2017.
16. Vemula SV, Zhao J, Liu J, et al. Current approaches for diagnosis of influenza virus infections in humans. Viruses. 2016;8:96.
17. CDC. Influenza (flu) treatment. www.cdc.gov/flu/consumer/treatment.htm. Accessed December 22, 2016.
18. Fiore AE, Fry A, Shay D, et al. Antiviral agents for the treatment and chemoprophylaxis of influenza—recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2011;60:1-24.
19. Harper SA, Bradley JS, Englund JA, et al. Seasonal influenza in adults and children—diagnosis, treatment, chemoprophylaxis, and institutional outbreak management: clinical practice guidelines of the Infectious Diseases Society of America. Clin Infect Dis. 2009;48:1003-1032.
20. Oseltamivir. Lexi-Comp Online. Hudson, OH: Lexi-Comp, Inc; 2016. https://online.lexi.com. Accessed December 9, 2016.
21. Zanamivir. Lexi-Comp Online. Hudson, OH: Lexi-Comp, Inc; 2016. https://online.lexi.com. Accessed December 9, 2016.
22. Peramivir. Lexi-Comp Online. Hudson, OH: Lexi-Comp, Inc; 2016. https://online.lexi.com. Accessed December 9, 2016.
23. CDC. Influenza antiviral medications: summary for clinicians. www.cdc.gov/flu/professionals/antivirals/summary-clinicians.htm. Accessed March 8, 2017.
24. Cooper NJ, Sutton AJ, Abrams KR, et al. Effectiveness of neuraminidase inhibitors in treatment and prevention of influenza A and B: systematic review and meta-analyses of randomized controlled trials. BMJ. 2003;326:1235.
25. The FDA approves first generic version of widely used influenza drug, Tamiflu. www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformationforPatientsandProviders/ucm514854.htm. Accessed January 13, 2017.
26. CDC. Antiviral emergency use authorization. www.cdc.gov/flu/professionals/antivirals/antiviral-emergency-use.htm. Accessed December 17, 2016.
To comment on this article, contact rdavidson@uspharmacist.com.






