US Pharm. 2015;40(2):40-43.
ABSTRACT: Deferral of blood donors results in the loss of donations in large numbers, greatly affecting the supply of blood in the United States. A donor’s drug profile is one of the reasons for deferral, for either donor or recipient safety concerns. The FDA has developed guidelines on deferrals due to medications. Pharmacists can utilize these guidelines as well as their drug knowledge to both reduce unnecessary deferrals and ensure the safety of donors and recipients.
Blood donation centers in the United States collect over 15.7 million donations annually from a total of 9.2 million donors.1,2 While this may seem excessive, more than 41,000 donations are required daily, a number that translates to about 14.7 million annually. It is estimated that 38% of the U.S. population is eligible to donate blood, even though less than 10% actually donates.1,2
Screening of Donors
The FDA ensures the safety of the entire nation’s blood supply with systems that safeguard against the transmission of infections in particular.3 Out of those who do volunteer to donate, a large number are deferred each year for either donor or recipient safety reasons. Even though the deferral is only temporary in most cases, it discourages volunteers, who often do not return to donate blood. One study found that 12.8% of approximately 48 million donors who presented between 2001 and 2006 in the U.S. were deferred.4 Over those 6 years, deferral due to recipient safety resulted in a temporary and indefinite loss of about 650,000 donors, while deferral due to donor safety led to a loss of over 1 million donors.4
Healthy individuals who are over the age of 17 years (16 years if they have a signed parental consent) and weigh at least 110 lb can be screened further for donation eligibility.5 Screen-ing is usually conducted using the Donor History Questionnaire (DHQ) or its abbreviated version (aDHQ). In addition to checking for recent travel outside the U.S. and reviewing any medical conditions a donor may have, the donor’s drug profile (if any) should also be taken into consideration before blood can be drawn. Blood from donors on medication may contain drugs that could pose a risk for the recipient or affect the quality of the transfusion. Furthermore, a donor’s drug profile may be a sign of a condition that could hinder the individual from donating blood.
The loss of high numbers of donors underscores the need for healthcare professionals to screen donors more comprehensively before deferral. One of the first papers on this issue was published in 1989 and updated in 2001.6,7 The FDA guidelines are based upon the recommendations of the American Association of Blood Banks (AABB), which are the most widely used in the U.S.8
Factors to Consider
Medications can affect an individual’s ability to donate blood, both directly and indirectly. Various factors affect the final decision to defer, including9:
- Type of transfusion that the blood will be used for
- Concentration of the drug in the donor’s plasma
- Pharmacologic properties of the drug
- Presence of any active drug metabolites
- Drug interactions: any medications that the recipient is taking that may interact with traces of drugs in the infused blood.
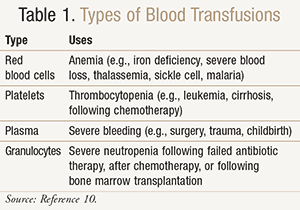
Types of Blood Transfusions: In the early days of medicine, whole blood was used in transfusions. With improvements in medical technology, it is now possible to isolate different components of blood and transfuse only what is required, including red blood cells, platelets, plasma, or granulocytes. Red blood cell transfusions are the most common type used, whereas granulocyte infusions are fairly uncommon. Information on the type of transfusion the blood is being drawn for may affect deferral, since not all drugs affect all types of infusions. For example, the presence of the antiplatelet drug clopidogrel in donor blood will only affect a platelet infusion; therefore, the donor may not have to be deferred if a plasma-only transfusion is required. The different types of blood transfusions are described in TABLE 1.10
Drug Concentrations: The concentration of any drug present in a donor’s plasma will depend upon the amount of drug administered, the time between the drug administration and the blood donation, the route of administration, and the pharmacokinetics of the particular drug.9
Medications Requiring Deferral
The following paragraphs discuss the drugs that may result in deferral of a blood donation. TABLE 2 contains an abbreviated version of the AABB’s Medication Deferral List.8

Teratogenic, Fetotoxic, and Embryotoxic Drugs: Generally, donors taking drugs that may be teratogenic, fetotoxic, or embryotoxic to pregnant women, including retinoids, thalidomide, valproic acid, and vitamin K antagonists, are deferred. However, many reports have shown that concentrations below 3% of the therapeutic level of the teratogen do not seem to cause birth defects.11-13 Moreover, manufacturers of such drugs claim that these agents are not harmful to the unborn child in concentrations below 3% even though their package inserts may not necessarily indicate this for purposes of litigation.9 This means that there is a window of opportunity for individuals taking such medications to donate blood.
It has been suggested that donors who have a concentration of more than 0.000001% of any of the teratogenic drugs should be deferred. It takes 28 plasma elimination half-lives from the last dose for the drug concentration to fall below this level.7
Antiandrogens: Dutasteride and finasteride are 5-reductase inhibitors approved for the management of benign prostatic hyperplasia. They are Pregnancy Category X drugs, and therefore deferral is recommended for blood donors on either of these medications.8,14,15 Finasteride is widely distributed and has a terminal elimination half-life of 4.7 to 7.1 hours.15 The FDA recommends that blood donors taking finasteride be deferred for 1 month, even though one study has calculated that a 3-day deferral period after the last dose should be sufficient.8,9 Dutasteride has a large volume of distribution (300-500 L), is highly bound to plasma albumin (99.0%) and alpha-1 acid glycoprotein (96.6%), and has a terminal elimination half-life of approximately 5 weeks at steady state.14 It is recommended that patients on dutasteride be deferred for 6 months from their last dose.8
Retinoids: Retinoids such as isotretinoin, acitretin, and etretinate are commonly used to manage dermatologic conditions.
Isotretinoin inhibits the function of the sebaceous gland and is indicated for the treatment of severe, recalcitrant cystic acne. It is a Pregnancy Category X drug that can cause neurologic and cardiovascular abnormalities in the unborn fetus.16 Isotretinoin is the most potent teratogen in humans after thalidomide, and its use is regulated through the iPLEDGE system. It is highly bound to plasma protein (~99%) and has been reported to have a plasma half-life of up to 167 hours.17,18 The manufacturer recommends deferring blood donation for 1 month after the last dose.18
Etretinate (Tegison; no longer available in the U.S.) and its metabolite acitretin are both teratogenic drugs used in the management of psoriasis.19 Before its withdrawal from the U.S. market, the FDA recommended that any donor who has taken etretinate be permanently deferred.20
Acitretin (Soriatane) is regulated by the Do Your P.A.R.T. (Pregnancy Prevention Actively Required During and After Treatment) program because of its teratogenic potential.21 It is highly bound to plasma proteins (99.9%), particularly albumin. The manufacturer of acitretin recommends that patients taking the drug wait for 3 years after the last dose before they donate blood.21
Nonteratogenic Drugs: Nonteratogenic drugs with dose-dependent pharmacodynamic concentrations below 3% (which translates to about 5 half-lives) in donor blood are generally considered safe, particularly for infusions containing 250 mL or more of plasma.7,9
Inhibitors of Platelet Aggregation: It has been shown that there are a considerable number of donors who have taken medications that affect platelet activity.22 Donors taking irreversible platelet inhibitors, including acetylsalicylic acid and the thienopyridines (clopidogrel and ticlopidine), need to be deferred, particularly if the blood donation is to be used for a platelet infusion, as the recipient’s blood clotting capacity may be affected. Furthermore, blood containing acetylsalicylic acid must not be infused into children aged <12 years due to the risk of Reye syndrome. Since the life span of human platelets is about 10 days, a deferral period of about 10 days following the last dose of platelet inhibitors should be sufficient.22
Clopidogrel exerts its effect through its active metabolite.23 The metabolite irreversibly binds to the P2Y12 class of adenosine diphosphate (ADP) receptors on platelets. Clopidogrel is used for the management of acute coronary syndrome, recent myocardial infarction, recent stroke, or established peripheral arterial disease. Its half-life is about 6 hours following a dose of 75 mg, and that of the active metabolite is 30 minutes. The manufacturer of clopidogrel (Plavix) indicates that a patient’s bleeding time and platelet aggregation should return to the baseline values in 5 days after the last dose.23
Ticlopidine interferes with platelet membrane function by inhibiting ADP-induced platelet fibrinogen binding and subsequent platelet-platelet interactions.24 It is highly bound to plasma proteins (98%) and has a half-life of 14 to 21 days after steady state concentrations have been achieved.24
Selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) act as reversible platelet inhibitors. Donors taking these drugs also need to be deferred for several days until the levels fall below 3%.9
Poorly Absorbed Drugs: Drugs with low or no systemic effects such as colestipol (a cholesterol-lowering agent) and nystatin (an antifungal) can be overlooked, and donors do not need to be deferred.9
Vitamin or Mineral Supplements: Since most of the preparations for replacement of vitamins or minerals do not normally exceed the endogenous levels of the corresponding compound, in most cases deferral in not necessary. Particular attention, however, should be paid to high-concentrate preparations. Additionally, the levels of fat-soluble vitamins (A, D, E, and K) should be checked in blood that is to be infused into a pregnant woman.9
OTC Products: While OTC preparations are available without a prescription, some products may contain active molecules that might not be suitable for the recipient (e.g., St. John’s wort). Furthermore, traces of these drugs may interact with medications the recipient is already taking.9
Experimental Medications: Donors on experimental medications as part of a clinical trial should be deferred for 12 months unless stated otherwise. Furthermore, it is advisable to contact the research team before blood is withdrawn.8,25
Human Growth Hormone: Growth hormone derived from human pituitary glands is used in the pediatric population to treat short stature due to growth hormone deficiency. The growth hormone has been linked to Creutzfeldt-Jakob disease in a number of studies.26-28 For this reason, the FDA recommends that donors who have taken growth hormone be permanently deferred.8,25
Insulin: Bovine insulin imported from countries where mad cow disease has been found could contain material from the infected cattle. For this reason, the FDA recommends permanently deferring donors who have used bovine insulin.8,25
Hepatitis B Immune Globulin (HBIG): HBIG is indicated for postexposure prophylaxis against hepatitis B infection. The FDA recommends that donors who have had the HBIG injection should be deferred for 12 months to ensure that the injection was effective and the hepatitis has been treated.8,25
Glucocorticoids and Immunosuppressants: While there are no guidelines on deferral for donors on glucocorticoids or immunosuppressants, it is useful to note that these drugs can mask the symptoms of an inflammation or infection. If this is the case, transfusing the blood may in effect transmit the infection to the recipient.29
Illicit Drugs or Anabolic Steroids: Individuals who have used illicit drugs or anabolic steroids should not donate blood due to the risk of transmitting latent blood-borne diseases such as HIV that may not be immediately detected.29
Medications That May Indicate an Underlying Disorder: Certain medications may themselves not pose a risk to the recipient, but may indicate an underlying disorder and thereby pose a risk to the donor. Some examples are:
- Asthma therapy: Asthmatics may experience lower total arterial oxygen-carrying capacity following the withdrawal of blood29
- Cardiovascular drugs: Bleeding is more likely in patients taking anticoagulants29; individuals taking beta-blockers have been shown to experience an increase in vasovagal reactions following blood donations30
- Anticonvulsants: Fainting following blood donation may lead to convulsions in epileptic patients.29
Blood-donation eligibility guidelines may vary between institutions. A more extensive list of what drugs to consider and their deferral periods is available online through the University of North Carolina Blood Donation Center.31
Role of the Pharmacist
Pharmacists can use their drug expertise to avoid any unnecessary deferrals and hence increase the number of blood donors. Furthermore, they can ensure the safety of donors and recipients by reviewing their drug profiles. One study found that 11% of donors did not fully disclose their recent medication history.32 Pharmacists are suitably placed to educate patients on the importance of disclosing their complete medical history, including OTC products, and assist them in doing so by keeping accurate prescription records.
REFERENCES
1. Riley W, Schwei M, McCullough J. The United States’ potential blood donor pool: estimating the prevalence of donor-exclusion factors on the pool of potential donors. Transfusion. 2007;47(7):1180-1188.
2. American Red Cross. Blood facts and statistics. www.redcrossblood.org/learn-about-blood/blood-facts-and-statistics. Accessed August 28, 2014.
3. FDA. Vaccines, blood & biologics. Questions about blood. www.fda.gov/BiologicsBloodVaccines/BloodBloodProducts/QuestionsaboutBlood/default.htm. Accessed August 28, 2014.
4. Zou S, Musavi F, Notari EP, et al. Donor deferral and resulting donor loss at the American Red Cross Blood Services, 2001 through 2006. Transfusion. 2008;48(12):2531-2539.
5. American Red Cross. Eligibility requirements. www.redcrossblood.org/donating-blood/eligibility-requirements. Accessed August 29, 2014.
6. Ferner RE, Dunstan JA, Chaplin S, Baird GM. Drugs in donated blood. Lancet. 1989;2(8654):93-94.
7. Stichtenoth DO, Deicher HR, Frolich JC. Blood donors
on medication. Are deferral periods necessary? Eur J Clin Pharmacol. 2001;57(6-7):433-440.
8. American Association of Blood Banks (AABB). Medication Deferral List. DHQ v1.3. Revised August 2013. www.aabb.org/tm/questionnaires/Documents/adhq/v1-3/aDHQ%20MedicationDeferralList%20v1.3_August2013_Myorisan_Zenatane.pdf. Accessed September 5, 2014.
9. Becker CD, Stichtenoth DO, Wichmann MG, et al. Blood donors on medication—an approach to minimize drug burden for recipients of blood products and to limit deferral of donors. Transfus Med Hemother. 2009;36(2):107-113.
10. American Red Cross. A Compendium of Transfusion Practice Guidelines. 2nd ed. Washington, DC: American National Red Cross; 2013. www.redcrossblood.org/sites/arc/files/59802_compendium_brochure_v_6_10_9_13.pdf. Accessed August 28, 2014.
11. Schaefer C, Hannemann D, Meister R, et al. Vitamin K antagonists and pregnancy outcome. A multi-centre prospective study. Thromb Haemost. 2006;95(6):949-957.
12. Schaefer C, Peters PWJ, Miller RK. Drugs During Pregnancy and Lactation: Treatment Options and Risk Assessment. 2nd ed. New York, NY: Elsevier/Academic Press; 2007.
13. Schardein JL. Chemically Induced Birth Defects. 3rd ed. New York, NY: Marcel Dekker; 2000.
14. Avodart (dutasteride) package insert. Research Triangle Park, NC: GlaxoSmithKline; September 2014. https://www.gsksource.com/gskprm/htdocs/documents/AVODART-PI-PIL.PDF. Accessed September 5, 2014.
15. Proscar (finasteride) patient information. Whitehouse Station, NJ: Merck & Co, Inc; September 2013. www.merck.com/product/usa/pi_circulars/p/proscar/proscar_ppi.pdf. Accessed September 8, 2014.
16. Prahalada S, Tarantal AF, Harris GS, et al. Effects of finasteride, a type 2 5-alpha reductase inhibitor, on fetal development in the rhesus monkey (Macaca mulatta). Teratology. 1997;55(2):119-131.
17. Nulman I, Berkovitch M, Klein J, et al. Steady-state pharmacokinetics of isotretinoin and its 4-oxo metabolite: implications for fetal safety. J Clin Pharmacol. 1998;38(10): 926-930.
18. Accutane (isotretinoin) product monograph. Mississauga ON: Hoffman La Roche; 1982-2014. www.rochecanada.com/fmfiles/re7234008/Research/ClinicalTrialsForms/Products/ConsumerInformation/MonographsandPublicAdvisories/Accutane/Accutane_PM_E.pdf. Accessed September 8, 2014.
19. Geiger JM, Baudin M, Saurat JH. Teratogenic risk with etretinate and acitretin treatment. Dermatology. 1994;189(2): 109-116.
20. FDA. Deferral of blood and plasma donors—medications. July 28, 1993. www.fda.gov/downloads/BiologicsBloodVaccines/.../UCM062813.pdf. Accessed September 8, 2014.
21. Soriatane (acitretin) package insert. Research Triangle Park, NC: Stiefel Laboratories, Inc; May 2014. https://www.gsksource.com/gskprm/htdocs/documents/SORIATANE-PI-MG.PDF. Accessed September 8, 2014.
22. Curvers J, Dielis AW, Heeremans J, van Wersch JW. Platelet function in whole-blood donors is impaired: the effects of painkillers. Transfusion. 2007;47(1):67-73.
23. Plavix (clopidogrel) package insert. Bridgewater, NJ: Bristol-Myers Squibb/Sanofi Pharmaceuticals Partnership; December 2013. http://packageinserts.bms.com/pi/pi_plavix.pdf. Accessed September 8, 2014.
24. Ticlodipine package insert. Toronto, ON: Genpharm Inc; August 1998. www.accessdata.fda.gov/drugsatfda_docs/anda/99/75161_Ticlopidine%20Hydrochloride_Prntlbl.pdf. Accessed September 8, 2014.
25. FDA. Medication Deferral List. DHQ v1.3. Effective May 2008. www.fda.gov/downloads/biologicsbloodvaccines/bloodbloodproducts/approvedproducts/licensedproductsblas/blooddonorscreening/ucm213553.pdf. Accessed August 28, 2014.
26. Lewis AM, Yu M, DeArmond SJ, et al. Human growth hormone-related iatrogenic Creutzfeldt-Jakob disease with abnormal imaging. Arch Neurol. 2006;63(2):288-290.
27. Caboclo LO, Huang N, Lepski GA, et al. Iatrogenic Creutzfeldt-Jakob disease following human growth hormone therapy: case report. Arq Neuropsiquiatr. 2002;60(2-B): 458-461.
28. Croes EA, Roks G, Jansen GH, et al. Creutzfeldt-Jakob disease 38 years after diagnostic use of human growth hormone. J Neurol Neurosurg Psychiatry. 2002;72(6):792-793.
29. Lewis G. Question from practice: do my medicines mean I can’t give blood? Pharm J. 2013;290:679.
30. Pisciotto P, Sataro P, Blumberg N. Incidence of adverse reactions in blood donors taking antihypertensive medications. Transfusion. 1982;22(6):530-531.
31. University of North Carolina Blood Donation Center. Drugs and medication deferral chart. April 2010. https://www.unchealthcare.org/site/blood_donation_center/Drugs%20and%20Medication%20Deferral%20Chart%20April%202010.pdf. Accessed August 28, 2014.
32. Melanson SE, Stowell CP, Flood JG, et al. Does blood donor history accurately reflect the use of prescription medications? A comparison of donor history and serum toxicologic analysis. Transfusion. 2006;46(8):1402-1407.
To comment on this article, contact rdavidson@uspharmacist.com.






