US Pharm. 2023;48(5):43-47.
ABSTRACT: Medication counseling techniques continue to evolve with the changing needs of diverse patient populations. Equity-based medication counseling supports eliminating health inequities in historically marginalized communities and optimizing health outcomes. Best practices for equity-based medication counseling include setting a culturally respectful counseling environment, using counseling techniques with open dialogue to build patient-provider relationships, and adopting equity-based communication and preferred language.
Counseling patients at the pharmacy counter has been mandated since the Omnibus Budget Reconciliation Act of 1990 (OBRA’90) and has proven to help lessen health risks while allowing patients to have autonomy and informed decision-making in their healthcare.1,2 The discussions between pharmacists and patients on medications can prevent medication-related problems such as polypharmacy, misaligned treatment expectations, misunderstood adverse reactions, and inappropriate medication or prescription abandonment.2-5
The United States has had a history of preventable and quantifiable health inequities over 120 years.6,7 Historically marginalized communities are the populations most susceptible to being underserved in healthcare and living with health disparities.8 These communities include individuals who experience health inequities that relate to disability status, income status, racial and ethnic identity, sexual identity and orientation, language, and geographic location.9
Medication counseling is an essential stage in the continuum of patient care and can provide another stepping-stone to eliminating health inequities. Practicing equity-based communication and using preferred language during patient counseling can improve health outcomes and build stronger patient-practitioner relationships.10
Setting a Culturally Respectful Environment
Cultural Respect
Cultural respect is a concept supported by organizations such as the National Institutes of Health and the CDC. Cultural respect is critical to reducing health disparities by helping pharmacists to understand what influences beliefs surrounding health.11 It helps improve access to high-quality healthcare that is respectful of and responsive to diverse patients’ needs and belief systems. When developed and implemented as a framework, cultural respect enables systems, agencies, and groups of professionals to function effectively to understand the needs of groups accessing health information and healthcare.
To practice cultural respect, a pharmacist must first develop cultural humility. Cultural humility is practicing self-awareness about one’s cultural background, cultural identity, and personal beliefs.12 Self-awareness also includes examining power imbalances, self-critique, and finding solutions that allow pharmacists to connect with their patients and advocate for their best health outcomes. Additionally, pharmacists should dedicate themselves to lifelong learning about their patients’ differing cultures and belief systems. To improve their understanding of different cultures, pharmacists should actively listen to their patients’ stories and experiences, appreciate their motivations, and ask clarifying questions to understand their patients’ health beliefs fully.
First Impressions and Rapport
First impressions are crucial moments that build rapport during a patient’s medication counseling.13 A rapport based on respect and cultural respect is optimal for facilitating information and fostering trust between patients and providers. A neutral-open body language and a positive-neutral facial expression are preferred to convey respect in any setting. Utilizing SURETY can help keep a positive and open body language by Sitting at an angle, Uncrossing legs and arms, using a Relaxed posture, using Eye contact, and using appropriate Touch, all while using Your intuition.14 First impressions and rapport management that foster cultural respect rely on verbal and nonverbal communication.15
Research has shown that over 65% of nonverbal facial expressions are interpreted inaccurately and can be influenced by the social judgment of culture, gender, class, education, and other factors.16 Approaching each patient in the same positive-neutral manner will help quickly set the tone for a more open conversation while avoiding unintentional bias or stigma.17
Body language and facial expression are deeply rooted in most cultures, can be tied to things such as gender roles within those cultures, and result in different interpretations of the same actions. Avoiding gestures with the face, hands, fingers, and arms is a good rule of thumb to prevent unintentional messages in most cultures. When faced with uncertainty, a pharmacist can employ the matching-and-mirroring technique to build patient rapport.18 Matching-and-mirroring aligns or coordinates the pharmacist’s physical body language with the patient’s body language and can help to gauge the best eye contact, personal space, and posture to use with the patient.
Consider Caregivers and Additionally Involved Parties
Another aspect in setting the tone for medication counseling is taking into consideration other parties accompanying, supporting, or assisting the patient. Depending on the counseling setting, these other parties may or may not be directly involved in the patient’s care, and definitions of “caregiver” often vary.19 For many patients, it is common and imperative to have family, friends, neighbors, partners, and loved ones involved in healthcare and medication.
Pharmacists must exercise their professional judgment and adhere to the Health Insurance Portability and Accountability Act of 1996 (HIPAA) by reasonably ensuring that other people are involved in the patient’s care.20 Therefore, to respect the patient’s privacy, be direct when stating that you will be “reviewing the details of their medication.” If a pharmacist is counseling a patient’s agent, asking if and how the agent is involved in the patient’s care is highly recommended. Knowing more about the care being provided can assist you in determining if the agent is simply providing transportation or is more intimately involved in the daily health-related care of the patient. If the relationship or desired inclusion from the patient is unclear, simply asking if the other party “is going to help them with their medication” is also acceptable.
Once you have established that a detailed medication review is taking place and the other party’s role, such as a caregiver or a family member, you can observe whether the patient refers to the other party often for responses. If the other party is often referred to, it may be pertinent to include the other party in your acknowledgments and questions; however, it is important to always address the patient first in the discussion, regardless of age, ability, gender, language preference, and other factors, to maintain an environment of respect.
Counseling Techniques That Support Relationship Building
Medication counseling between a pharmacist and patient has remained the same in foundational methods and legal requirements over the past 30 years.1 However, the historical hierarchal approach to medicine has now evolved to focus on building patient-provider relationships. In today’s pharmacy practice, Indian Health Services is still the cornerstone of patient counseling using the three prime, open-ended questions (FIGURE 1).21

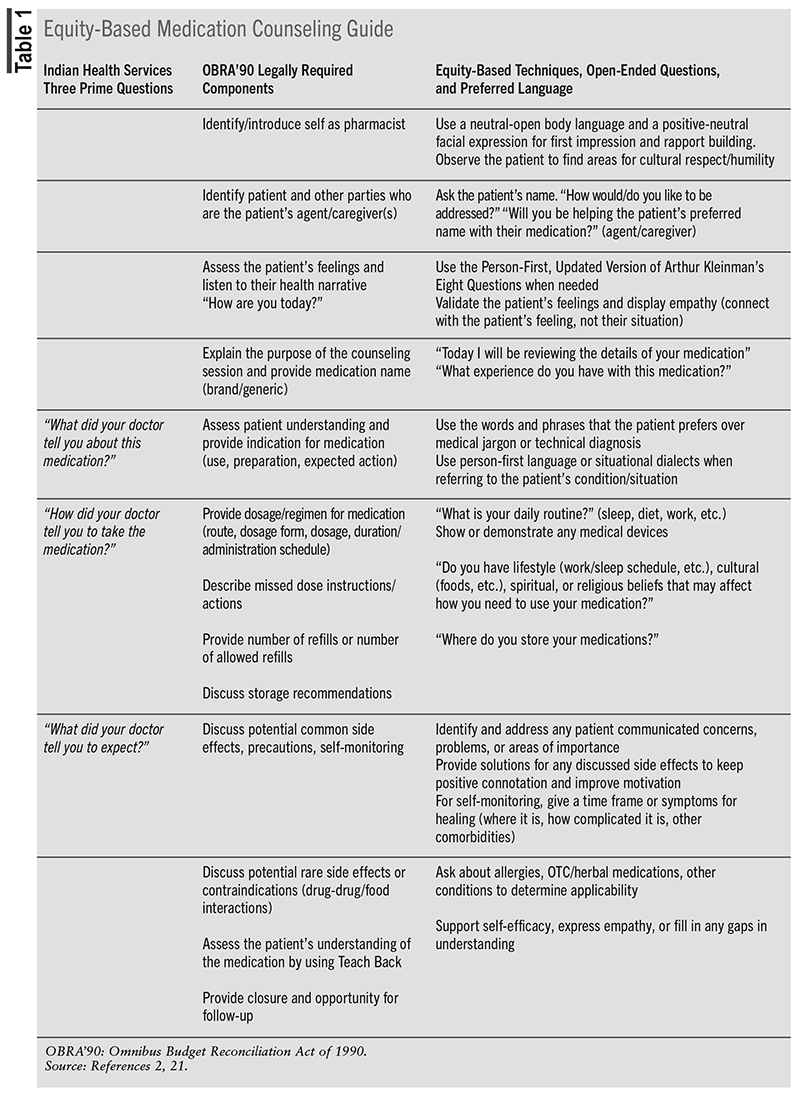
Using open-ended questions avoids automated patient responses such as “yes” and “no,” allowing patients to describe their health and lives in their own words and using their perceptions of the medical information they have been given previously.22 Additional techniques such as AIDET, the QuEST process, and the SCHOLARMAC tool may also be helpful in other situations, such as making patient recommendations and OTC medication counseling.23-25 Open-dialogue techniques, such as the Equity-Based Medication Counseling Guide (TABLE 1), have been shown to assist in conveying empathy, reducing patient anxiety, and improving patient health outcomes.26
Empathy is a mainstay of open dialogue in healthcare; however, it is a commonly miscommunicated concept. Although by definition empathy is the ability to understand and sense other people’s emotions, it is not so straightforward when counseling patients in complex environments and with in-depth medication information.27 The phrase “I understand” is common in practice; however, it can unintentionally dismiss the patient’s situation and feelings. It is rare that anyone truly “understands” precisely what another person is experiencing.
For providers, connecting with the patient’s basic emotions, such as confusion, frustration, fear, and being overwhelmed, is more accurate and sensitive. When verbally expressing this connection with the patient, avoid the phrase “I understand” and opt for validation of the patient’s feelings.28 The patient’s feelings can be validated by reflecting the interpreted feelings to the patient using phrasing like “that sounds very frustrating” or “I can see how that would feel overwhelming.” The use of validation is not easy or natural; it does require active and intentional engagement with the patient and often takes practice on the part of the pharmacist.
Open dialogue between patients and pharmacists allows for a more equity-based conversation that avoids traditionally dominant narratives and assumptions often associated with bias and stereotypes. Using technique-based, open-ended questions can aid pharmacists in obtaining an accurate picture of patients’ beliefs and motivations surrounding their health. The use of empathy and validation further convey respect in equity-based medication counseling (TABLE 1) and helps build a stronger relationship with the patient.
Equity-Based Communication and Preferred Language
Having insight into patients’ perception of their health and medication also provides pharmacists with words and phrases that the patient prefers over medical jargon. A best practice for any patient-counseling technique is to use plain language to provide clear and concise information to the patient.29 Research has shown that patients are more open to discussing sensitive topics when mutual patient-provider relationships replace traditional hierarchal roles in healthcare.10
Along with plain language, other equity-based communications and preferred language practices are recommended for provider adoption. Equity-based communication and preferred language encompass using preferred names, situational dialects, person-first, and positive language. Equity-based communication considers patients’ preferences and conveys connection, understanding, provider humility, and empathy.
Preferred Names
When counseling patients, it is vital to remember the appropriate and inclusive language that respects their preferred identity. When addressing patients, always use their chosen or preferred name. Asking “how would you like to be addressed” is an all-encompassing question that covers title, status, pronouns, and chosen or preferred names. Many situations, such as software limitations and insurance incompatibilities, prevent preferred names from being used on health data. This situation is found especially with transgender patients, and many may not be able to afford, are not of age, or have no access to change their names legally.30
When addressing transgender patients, it is also essential and respectful to align the patient’s pronouns with the preferred or authentic gender, regardless of having undergone gender confirmation surgery (GCS) or having taken hormones.31 The best way to ensure correct pronoun usage is to ask the patient “What pronouns do you use?” If it is impossible to ask which pronouns a patient uses, use the pronoun consistent with the person’s gender expression or use the singular “they” when not assigning a specific gender. Using the singular “they” to describe nonbinary gender is becoming increasingly common and is a respectful manner of addressing those who do not wish to identify as either male or female.
Situational Dialects
Improving sensitivity in terminology and phrasing has become increasingly crucial for stigma and bias reduction in healthcare. It is important for pharmacists to be up-to-date on trends in communication and to start identifying areas of improvement in their daily wording. For instance, in transgender populations undergoing GCS, the phrases “sex change,” “preoperative,” and “postoperative” should be avoided. Terms such as “assigned male at birth” and “assigned female at birth” are considered favorable to use as opposed to “biologically male,” “biologically female,” “genetically male,” “genetically female,” “born a man,” or “born a woman.”32
Areas of healthcare that have historically been shrouded in stigma now have guidelines on sensitive language choices called “situational dialects.” Situational dialects are tools for appropriate word choice with homelessness, bereavement, gender identity and orientation, mental health conditions, substance use disorder, and HIV, among many others.33-36 Pharmacists with patient populations living with or experiencing these situations can significantly improve their patient-provider relationships by utilizing these tools.
Person-First, Positive Language
As pharmacists improve their terminology and wording during patient communications, other aspects can be updated to create a significant impact. Using person-first language is a technique that avoids dehumanizing the patient by always describing the person before the medical condition and avoiding using a diagnosis as a label or descriptor. For example, person-first language, such as “Jorge is living with diabetes,” more accurately describes that the patient is not defined by the diagnosis.37-39
Additionally, person-first language can update other communication techniques, such as Kleinman’s Questions.40 Removing the “you,” “your,” and other languages from these questions can minimize connotations perceived as passing judgment (TABLE 2). These updated questions are helpful to start the conversation, especially when a pharmacist is newly becoming acquainted with the patient or the patient is processing a new diagnosis. A grieving process occurs when patients receive a health diagnosis, regardless of whether they anticipate it. Within this process, attitudes, perceptions, and motivations are formed within the patient’s mind toward the condition. Kleinman’s Questions can help determine how patients feel about their condition so that you can tailor your counseling to optimize their health outcomes.

The final touch to polish any equity-based medication counseling is to keep positive connotations and language throughout the encounter. Positive language is critical to avoid blame, implicit or unaware-type bias, and judgment when discussing health conditions and treatment.41 Avoiding implicit bias is another significant step in minimizing contributions to health inequities. To practice positive language, adopt words that have neutral or positive connotations, such as “adherence” versus “compliance,” “declined” versus “refused,” or “not at goal” versus “failed.” Also, reframing directives into options or choices explained with reasoning can be very successful for a patient’s willingness to accept. An example of positive reframing of a directive is “I would consider taking this with food to avoid upset stomach” versus “take with food.” Polishing equity-based medication counseling with positive language will require some retraining of habitual language; however, a small amount of practice can improve patient relationships and mutual satisfaction during medication counseling.
Conclusion
Medication counseling is a pillar of the pharmacy profession and is vital in closing the equality gaps in healthcare. Communication techniques and language preference change frequently, so pharmacists must keep updated on the latest, most sensitive wording and phrasing. Creating culturally respectful environments, utilizing open-dialogue counseling techniques, and adopting inclusive language can aid in the creation of trusting patient-pharmacist relationships. Health inequities are indicative of poor health outcomes for historically marginalized patients. However, the ability to reduce these disparities exists when pharmacists commit to fully engaging with their patients and utilizing best practices of equity-based medication counseling.
REFERENCES
1. Volino LR, Das RP, Mansukhani RP, Cosler LE. Evaluating the potential impact of pharmacist counseling on medication adherence using a simulation activity. Am J Pharm Educ. 2014;78(9):169.
2. Accessed March 12, 2023. https://www.congress.gov/bill/101st-congress/house-bill/5835/text
3. Tariq RA, Vashisht R, Sinha A, Scherbak Y. Medication dispensing errors and prevention. In: StatPearls. StatPearls Publishing; 2022.
4. Akinbosoye OE, Taitel MS, Grana J, et al. Improving medication adherence and health care outcomes in a commercial population through a community pharmacy. Popul Health Manag. 2016;19(6):454-461.
5. Brown MT, Bussell JK. Medication adherence: WHO cares? Mayo Clin Proc. 2011;86(4):304-314.
6. Whitehead M. The concepts and principles of equity and health. Int J Health Serv. 1992;22(3):429-445.
7. Social determinants of health. Accessed March 12, 2023. www.who.int/topics/health_equity/en/.
8. CDC. Health disparities. 2020. www.cdc gov/healthyyouth/disparities/index.htm. Updated November.
9. Bowleg L, Huang J, Brooks K, et al. Triple jeopardy and beyond: multiple minority stress and resilience among black lesbians. J Lesbian Stud. 2003;7(4):87-108.
10. Haidet P, Paterniti DA. Building a history rather than “taking” one: a perspective on information sharing during the medical interview. Arch Intern Med. 2003;163:1134-1140.
11. Wheeler M. Cultural competence and cultural humility: a literature review for understanding and action. 2018. tripartners.com.
12. Yeager KA, Bauer-Wu S. Cultural humility: essential foundation for clinical researchers. Appl Nurs Res. 2013;26(4):251-256.
13. Bhatt N. Interviewing techniques. In: Guide to Intellectual Disabilities. Springer International Publishing; 2019:57-63.
14. Stickley T. From SOLER to SURETY for effective non-verbal communication. Nurse Educ Pract. 2011;11(6):395-398.
15. Harrison MA, Smith WR, Greenwell MR, Stephens KK. Frontline employees in the health clinic: impression management multiplexing when performing in-the-round. Commun Monogr. 2018;85(3):309-330.
16. Hareli S, Shomrat N, Hess U. Emotional versus neutral expressions and perceptions of social dominance and submissiveness. Emotion. 2009;9(3):378-384.
17. Leppänen JM, Hietanen JK. Positive facial expressions are recognized faster than negative facial expressions, but why? Psychol Res. 2004;69(1-2):22-29.
18. Clabby J, O’Connor R. Teaching learners to use mirroring: rapport lessons from neurolinguistic programming. Fam Med. 2004;36(8):541-543.
19. Kent EE, Rowland JH, Northouse L, et al. Caring for caregivers and patients: research and clinical priorities for informal cancer caregiving. Cancer. 2016;122(13):1987-1995.
20. Covered Entities: Required Disclosures. A Covered Entity Is Required to Disclose Protected Health Information: (I) To an Individual, When Requested under and Required by § 164.524 or § 164.528; and (Ii) When Required by the Secretary under Subpart C of Part 160 of This Subchapter to Investigate or Determine the Covered Entity’s Compliance with This Subchapter.
21. Colvin NN, Mospan CM, Buxton JA, et al. Using Indian Health Service (IHS) counseling techniques in an independent community pharmacy to improve adherence rates among patients with diabetes, hypertension, or hyperlipidemia. J Am Pharm Assoc. 2018;58(4):S59-S63.
22. Hashim MJ. Patient-centered communication: basic skills. Am Fam Physician. 2017;95(1):29-34.
23. http://paetc.org/wp-content/uploads/2014/07/AIDET-Training-Presentation1.pdf. Accessed March 12, 2023.
24. Leibowitz K, Ginsburg D. Counseling self-treating patients quickly and effectively. Proceedings of the APhA Inaugural Self-Care Institute; 2002.
25. Buring SM, Kirby J, Conrad WF. A structured approach for teaching students to counsel self-care patients. Am J Pharm Educ. 2007;71(1):8.
26. Well-being. www.pharmacist.com/Practice/COVID-19/Well-being. Accessed March 12, 2023.
27. Baguley SI, Pavlova A, Consedine NS. More than a feeling? What does compassion in healthcare ‘look like’to patients? Health Expectations. 2022;25(4):1691-1702.
28. Warde F, Papadakos J, Papadakos T, et al. Plain language communication as a priority competency for medical professionals in a globalized world. Can Med Educ J. 2018;9(2):e52-e59.
29. Kate MS. GLAAD media reference guide–transgender people. GLAAD. 2022. www.glaad.org/reference/covering-trans-community. Accessed March 12, 2023.
30. Kate MS. GLAAD media reference guide–transgender people. GLAAD. 2002. www.glaad.org/reference/transgender. Accessed March 12, 2023.
31. Vocabulary T. https://docs.asee.org/public/LGBTQ/Transgender_Vocab_Handout.pdf. Accessed March 12, 2023.
32. www.dbsalliance.org/wp-content/uploads/2019/02/DBSA_language.pdf. Accessed March 12, 2023.
33. www.thementalhealthcoalition.org/wp-content/uploads/2020/05/The-Mental-Health-Coalitions-Language-Guide.pdf. Accessed March 12, 2023.
34. National Institute on Drug Abuse. Words matter–terms to use and avoid when talking about addiction. 2021. https://nida.nih.gov/nidamed-medical-health-professionals/health-professions-education/words-matter-terms-to-use-avoid-when-talking-about-addiction. Accessed March 12, 2023.
35. Stophivtogether C. People/person with HIV preferred word or phrase: person with AIDS, person with HIV, person living with HIV, HIV-positive person preferred word or phrase: HIV-positive people/person, people/person with HIV, people/ person with AIDS. www.cdc.gov/stophivtogether/library/stop-hiv-stigma/fact-sheets/cdc-lsht-stigma-factsheet-language-guide.pdf. Accessed March 12, 2023.
36. Crocker AF, Smith SN. Person-first language: are we practicing what we preach? J Multidiscip Healthc. 2019;12:125-129.
37. Dickinson JK, Guzman SJ, Maryniuk MD, et al. The use of language in diabetes care and education. Diabetes Care. 2017;40(12):1790-1799.
38. Hashim MJ. Patient-centered communication: basic skills. Am Fam Physician. 2017;95(1):29-34.
39. Kleinman A, Eisenberg L, Good B. Culture, illness, and care: clinical lessons from anthropologic and cross-cultural research. Ann Intern Med. 1978;88(2):251-258.
40. FitzGerald C, Hurst S. Implicit bias in healthcare professionals: a systematic review. BMC Med Ethics. 2017;18(1):19.
41. König L, Jucks R. Effects of positive language and profession on trustworthiness and credibility in online health advice: Experimental study. J Med Internet Res. 2020;22(3):e16685.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






