US Pharm. 2011;36(2):51-57.
Calcium, a mineral that is found in many foods or added to enhance foods and is commonly prescribed to patients as a dietary supplement, has recently received negative attention in both the medical literature and the lay press. Although 99% of calcium—which is abundant in the human body—is stored in bones and teeth for skeletal integrity, the remainder is stored in soft-tissue cells (0.9%) and in the bloodstream and extracellular fluid (0.1%), where it can influence the function of the cardiovascular, nervous, and muscular systems.1,2 Conflicting evidence has been published to support both the cardiovascular benefits of and the risks associated with calcium intake. This article discusses the common use and recommended intake of calcium; reviews the hypothesized cardiac benefits of this fundamental mineral; and addresses a recently published meta-analysis supporting the argument that calcium supplementation can increase cardiovascular events.
Osteoporosis and Calcium Recommendations
As mentioned above, maintaining an adequate calcium intake is vital for the structural integrity of the skeleton. Recommendations for daily calcium intake differ depending on age. Typically, patients at increased risk for hypocalcemia include those with lactose intolerance, a vegetarian diet, amenorrhea, renal failure, or surgical removal of the stomach, and those who take certain medications, such as diuretics.1 Additionally, as women approach menopause and bone-resorption rates increase, calcium requirements rise to counterbalance the physiologic changes that older women experience, such as reduced efficiency of calcium utilization and decreased intestinal absorption of nutrients.2
Although osteoporosis affects both sexes—with an estimated 10 million U.S. adults diagnosed with the disease—80% of patients are women.1 Since up to 90% of hip and spine fractures occur in osteoporotic bones, the primary treatment goal for osteoporosis is to prevent or reduce risk of fracture.2 Evidence to support the benefits of adequate calcium (and vitamin D, to aid calcium absorption) intake is so compelling that the clinical practice guidelines published by the National Osteoporosis Foundation (NOF) recommend that adults aged 50 years and older consume daily at least 1,200 mg of calcium from all sources—both dietary and supplemental—and 800 IU to 1,000 IU of vitamin D.3 However, to avoid health problems, the NOF advises that daily calcium intake should not exceed 2,000 mg to 2,500 mg.4
Hypertension
The relationship between calcium intake and blood pressure has been analyzed in epidemiologic and clinical trials, with inconsistent results.5-9 Supplemental calcium has been shown to decrease systolic blood pressure (SBP) by 0.15 mmHg to 0.4 mmHg for each 100-mg increase in calcium intake.6 Most trials found a minimal or nonexistent effect on diastolic blood pressure (DBP).5,7,8 A more recent clinical trial focusing on postmenopausal women—the group most likely to supplement with calcium—revealed that high calcium intake had only a minimal effect on SBP and did not alter DBP; additionally, it noted that these findings were transient, subsiding after 6 months of therapy.9 The trial investigators concluded that these results were insufficient to support the routine use of calcium supplementation in hypertensive patients.
The DASH (Dietary Approaches to Stop Hypertension) plan—a common topic in patient education about hypertension—was adopted into clinical practice after a study found that a diet high in fruits, vegetables, and low-fat dairy products (main source of calcium) could decrease SBP by 5 mmHg and DBP by 3 mmHg.10 Despite these positive findings, the specific contribution of increased dietary calcium in this regard has not been evaluated. Furthermore, the data on calcium supplementation and hypertension are limited, and better-quality trials are necessary.
Dyslipidemia and Obesity
A link between increased calcium consumption and lower body weight has been suggested.11-13 Analysis of the National Health and Nutrition Examination Survey III database revealed a stepwise inverse association between dietary calcium intake and risk of obesity.14 Two mechanisms have been proposed to explain this association. First, increased calcium intake potentially results in decreased calcium concentrations in fat cells, leading to slower production of parathyroid hormone and the active form of vitamin D, which results in an increased breakdown of fat.12 Second, human and animal studies suggest that calcium can bind with bile acids and fatty acids in the gut, leading to malabsorption of fat from the digestive tract.15,16 The latter mechanism is also used to support the argument that increased calcium intake has a positive effect on serum lipids.
A clinical trial of healthy postmenopausal women reported that calcium supplementation resulted in a nearly 20% increased ratio of HDL cholesterol to LDL cholesterol.17 However, positive outcomes have mainly been reported in animal studies, and even those results are inconsistent.18 Data supporting the correlation between increased calcium intake and decreased serum lipids in humans are limited. Furthermore, clinical trials are needed to strengthen the theory that additional dietary or supplemental calcium may play a role in weight loss or lack of weight gain.19
Cardiovascular Risk
Despite its role in maintaining bone integrity and the possible improvement in some vascular risk factors discussed above, calcium has been found in atherosclerotic lesions, leading to uncertainty as to whether calcium supplementation increases the risk of cardiovascular disease. Recent reports have found that calcium supplementation may increase the risk of myocardial infarction and cardiovascular events in healthy older women.19,20 These trials led investigators to perform a meta-analysis evaluating the effect of calcium supplementation on cardiovascular risk.21
The main objective of this meta-analysis, published in the British Medical Journal in 2010, was to determine whether calcium supplements increase the risk of cardiovascular disease.21 Patient-level and trial-level data were analyzed, including randomized, placebo-controlled trials of patients older than 40 years who were taking ³500 mg of supplemental calcium daily. Studies had to last more than 1 year and enroll at least 100 patients. Trials were excluded if vitamin D supplementation was given only to the intervention group, or if dietary calcium or calcium in the form of complex nutritional supplements was utilized. Of the 15 studies eligible for inclusion, only 11 provided data on cardiovascular outcomes. Primary endpoints were time to first myocardial infarction, time to first stroke, and time to first event, for a composite endpoint consisting of myocardial infarction, stroke, or sudden death. All-cause mortality was the secondary endpoint.
Five studies provided patient-level data on cardiovascular outcomes.21 These studies had an average duration of 4.1 years and involved a total of more than 8,000 patients aged a mean of 73 years. Calcium supplementation ranged from 600 mg to 1.2 g daily. When a Cox proportional-hazards model adjusted for possible covariates associated with cardiovascular outcomes (age, sex, smoking status, baseline diabetes, dyslipidemia, hypertension, or heart disease) was used, there was a significant increase in myocardial infarction in the calcium-supplementation group versus the placebo group (hazard ratio [HR] 1.31, 95% CI 1.02-1.67, P = .035). The number needed to harm (NNH) with calcium for 5 years to cause one incident of myocardial infarction was 69. Stroke, the composite endpoint, and all-cause mortality were increased, although not significantly.
Eight studies provided trial-level data on cardiovascular outcomes.21 These studies had an average trial duration of 3.8 years and included more than 10,000 patients with a mean age of 68 years. Calcium supplementation ranged from 500 mg to 1.4 g daily. Using the same adjusted Cox proportional-hazards model mentioned above, treatment with calcium supplements was associated with an increased risk of myocardial infarction (relative risk [RR] 1.27, 95% CI 1.01-1.59, P =.038). Again, stroke, the composite endpoint, and death did not increase significantly in relation to calcium supplementation.
In a prespecified subgroup analysis, dietary calcium intake over the median of 805 mg per day was associated with an increased risk of myocardial infarction (HR 1.85, 95% CI 1.28-2.67); this increased risk was not found with calcium intake under 805 mg per day, however.21 Overall, in the analysis of the 11 studies with cardiovascular outcomes, calcium supplementation was associated with about a 30% increase in the incidence of myocardial infarction.
Limitations
Vitamin D supplementation has been documented to decrease mortality.22 The meta-analysis discussed above did not include studies comparing coadministered calcium and vitamin D supplements versus placebo. The results of that meta-analysis, therefore, may not apply to calcium supplements that are used in conjunction with vitamin D supplements. It is possible that the decreased incidence of mortality associated with vitamin D intake may diminish the potential risk associated with calcium intake alone.
The Women’s Health Initiative Calcium/Vitamin D Supplementation Trial, a double-blind, placebo-controlled study, enrolled more than 36,000 postmenopausal women aged 51 to 82 years.23 Subjects were randomized to a treatment group (1,000 mg calcium carbonate and 400 IU vitamin D3 daily in two divided doses) or placebo, with an average follow-up of 7 years. Prespecified outcomes included hip fracture (primary outcome), other fractures, or colorectal cancer. Treatment with calcium and vitamin D supplements caused a nonsignificant reduction in the risk of cardiovascular-related death (HR 0.92, 95% CI 0.77-1.10). Although not a primary endpoint, this reduction provides evidence supporting the notion that vitamin D intake may mitigate the effects of calcium supplementation seen in the meta-analysis.
Application to Clinical Practice
The meta-analysis discussed above suggests that calcium supplementation without the coadministration of vitamin D is associated with an increased incidence of myocardial infarction. Additional studies evaluating the cardiovascular effects of calcium supplementation, with and without vitamin D, are needed to clarify the harm or benefit of these supplements.
The reported NNHs in this meta-analysis are alarming. The concern over increased morbidity and mortality associated with calcium supplementation is counterbalanced by the benefits of calcium supplementation in bone loss. A meta-analysis performed in 2007 revealed that the benefit of calcium on fractures is minimal, with an approximately 10% risk reduction in all fractures.24 Thus, patients with significant fracture risk should be advised to take medications with proven antifracture efficacy, such as bisphosphonates. It is too soon to abolish calcium supplementation altogether. Patients, especially perimenopausal and postmenopausal women, are still encouraged to consume adequate calcium; however, calcium supplementation should be recommended only to patients who consume insufficient calcium from dietary sources.
The Pharmacist’s Role
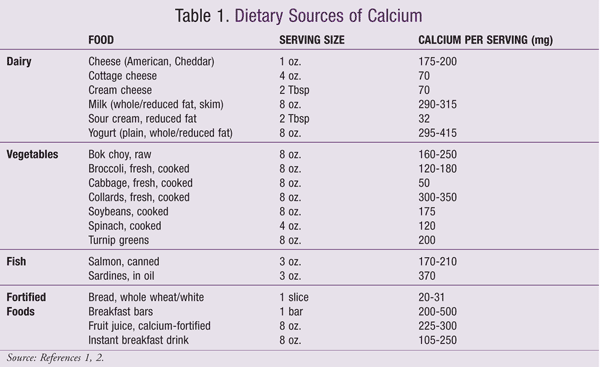
It is important for pharmacists to understand the recently published data and to become knowledgeable about how these findings translate to patient care. Prior to initiating calcium supplementation, it is vital that the patient’s estimated daily calcium intake be assessed by the health care team (TABLE 1). Explain to patients that the findings concerning calcium supplements do not apply to calcium-rich foods, and that there are no reported cases of calcium intoxication from dietary calcium sources.2 Also explain that because the calcium found in food has a much smaller effect on serum calcium, it is preferred to supplements.25 Lactose-intolerant patients and those on a strict vegetarian diet should be encouraged to obtain calcium from nondairy or calcium-fortified products (TABLE 1). A multidisciplinary approach to patient care may help educate patients about appropriate and inappropriate calcium intake by supplementation, as well as prevent them from discontinuing medications owing to misinformation.
REFERENCES
1. National Institute of Health Office of Dietary Supplements. Dietary supplement fact sheet: calcium.
http://ods.od.nih.gov/
2. North American Menopause Society. The role of calcium in peri- and postmenopausal women: 2006 position statement of the North American Menopause Society. Menopause. 2006;13:862-877.
3. National Osteoporosis Foundation. Clinician’s Guide to Prevention and Treatment of Osteoporosis.
4. National Osteoporosis Foundation. Calcium: what you should know.
www.nof.org/node/172. Accessed December 13, 2010.
5. Allender PS, Cutler JA, Follmann D, et al. Dietary calcium and blood pressure: a meta-analysis of randomized clinical trials. Ann Intern Med. 1996;124:825-831.
6. Birkett NJ. Comments on a meta-analysis of the relation between dietary calcium intake and blood pressure. Am J Epidemiol. 1998;148:223-228.
7. Bucher HC, Cook RJ, Guyatt GH, et al. Effects of dietary calcium supplementation on blood pressure. A meta-analysis of randomized controlled trials. JAMA. 1996;275:1016-1022.
8. Griffith LE, Guyatt GH, Cook RJ, et al. The influence of dietary and nondietary calcium supplementation on blood pressure: an updated metaanalysis of randomized controlled trials. Am J Hypertens. 1999;12:84-92.
9. Reid IR, Horne A, Mason B, et al. Effects of calcium supplementation on body weight and blood pressure in normal older women: a randomized controlled trial. J Clin Endocrinol Metab.
10. Appel LJ, Moore TJ, Obarzanek E, et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. N Engl J Med. 1997;336:1117-1124.
11. Davies KM, Heaney RP, Recker RR, et al. Calcium intake and body weight. J Clin Endocrinol Metab.
12. Perikh SJ, Yanovski JA. Calcium intake and adiposity. Am J Clin Nutr. 2003;77:281-287.
13. Zemel MB. Regulation of adiposity and obesity risk by dietary calcium: mechanisms and implications. J Am Coll Nutr. 2002;21:146S-151S.
14. Zemel MB, Shi H, Greer B, et al. Regulation of adiposity by dietary calcium. FASEB J.
15. Govers MJA, Vandermeer R. Effects of dietary calcium and phosphate on the intestinal interactions between calcium, phosphate, fatty acids, and bile acids. Gut. 1993;34:365-370.
16. Denke MA, Fox MM, Schulte MC. Short-term dietary calcium fortification increases fecal saturated fat content and reduces serum lipids in men. J Nutr. 1993;123:1047-1053.
17. Reid IR, Mason B, Horne A, et al. Effects of calcium supplementation on serum lipid concentrations in normal older women: a randomized controlled trial. Am J Med. 2002;112:343-347.
18. Bostick RM, Kushi LH, Wu Y, et al. Relation of calcium, vitamin D, and dairy food intake to ischemic heart disease mortality among postmenopausal women. Am J Epidemiol. 1999;149:151-161.
19. Bolland MJ, Barber PA, Doughty RN, et al. Vascular events in healthy older women receiving calcium supplementation: randomised controlled trial. BMJ. 2008;336:262-266.
20. Reid IR, Mason B, Home A, et al. Randomized controlled trial of calcium in healthy older women. Am J Med. 2006;119:777-785.
21. Bolland MJ, Avenall A, Baron JA, et al. Effect of calcium supplements on risk of myocardial infarction and cardiovascular events: meta-analysis. BMJ. 2010;341:c3691.
22. Autier P, Gandini S. Vitamin D supplementation and total mortality: a meta-analysis of randomized controlled trials. Arch Intern Med. 2007;167:1730-1737.
23. LaCroix AZ, Kotchen J, Anderson G, et al. Calcium plus vitamin D supplementation and mortality in postmenopausal women: the Women’s Health Initiative calcium-vitamin D randomized controlled trial. J Gerontol A Biol Sci Med Sci. 2009;64:559-567.
24. Tang BMP, Eslick GD, Nowson C, et al. Use of calcium or calcium in combination with vitamin D supplementation to prevent fractures and bone loss in people aged 50 years and older: a meta-analysis. Lancet. 2007;370:657-666.
25. Reid IR, Bolland MJ, et al. Does calcium supplementation increase cardiovascular risk? Clin Endocrinol (Oxf). 2010;73:689-695. Washington, DC: National Osteoporosis Foundation; 2010. 2005;90:3824-3829. 2000;85:4635-4638. 2000;14:1132-1138.
To comment on this article, contact rdavidson@uspharmacist.com.





