US Pharm. 2022;47(9):6-12.
ABSTRACT: Medical and/or recreational marijuana have been legalized in several states. With this increase in availability, there has been a rise in the number of pediatric exposures, especially for cannabis edibles. Pharmacists should be familiar with the availability of the different forms of cannabis, the issues surrounding the use of cannabis edibles, signs and symptoms of cannabis poisoning, the impact that cannabis edibles have had on pediatric emergency department visits and hospitalizations, and proposed mitigation strategies to reduce risk. Pharmacists need to be at the forefront of educating the public about how to prevent accidental cannabis overdoses in pediatric patients.
The Controlled Substances Act (CSA) of 1970 classified marijuana (or cannabis) as a Schedule I controlled substance, which means that it is considered to have a high abuse potential, is devoid of an accepted medical use, and is not considered safe.1,2 However, under the “Odgen Memo” issued in 2009 by then Deputy Attorney General David Ogden, the federal government indicated that “in prosecutions under the CSA, federal prosecutors are not expected to charge, prove, or otherwise establish any state law violations,” which meant that the federal government would no longer enforce the prosecution of cannabis users or suppliers. However, this ruling did not constitute legalization of cannabis.1,3,4 Although former Attorney General Jeff Sessions rescinded the Ogden Memo, no enforcement has taken place. Further, the CSA states that state drug laws are only preempted if there is an “affirmative conflict” with the CSA, thereby making state law the primary enforcement authority for drug-related offenses.1
The call for legalization of cannabis has largely been based on a concern justice, as proponents state that the burden of enforcing marijuana legal restrictions has fallen more heavily upon disadvantaged minority populations.5 However, how legalization will affect social equity, health, and safety will depend on numerous factors.6
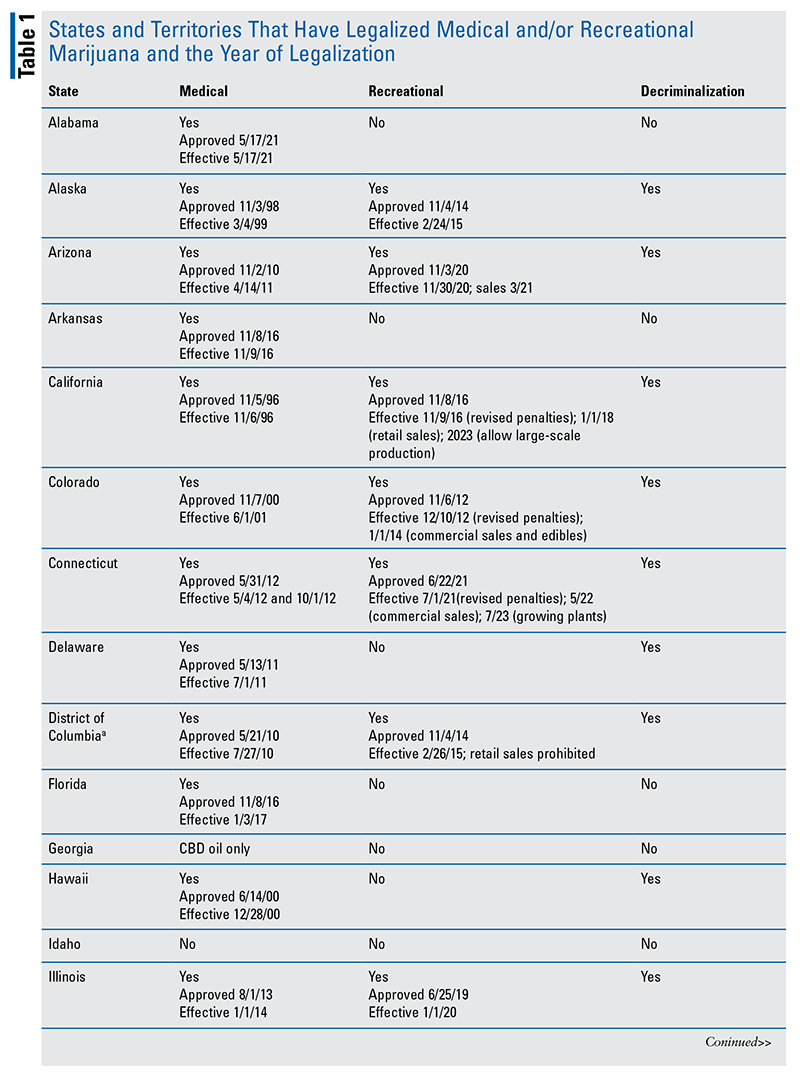
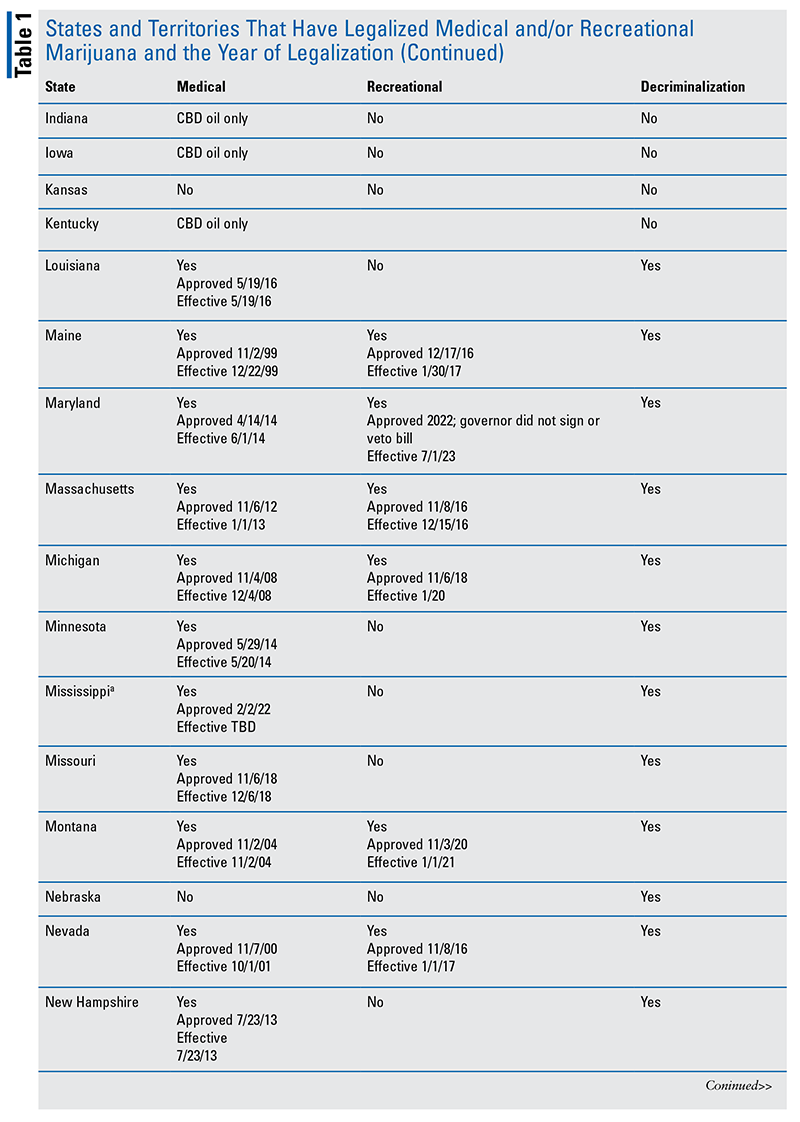
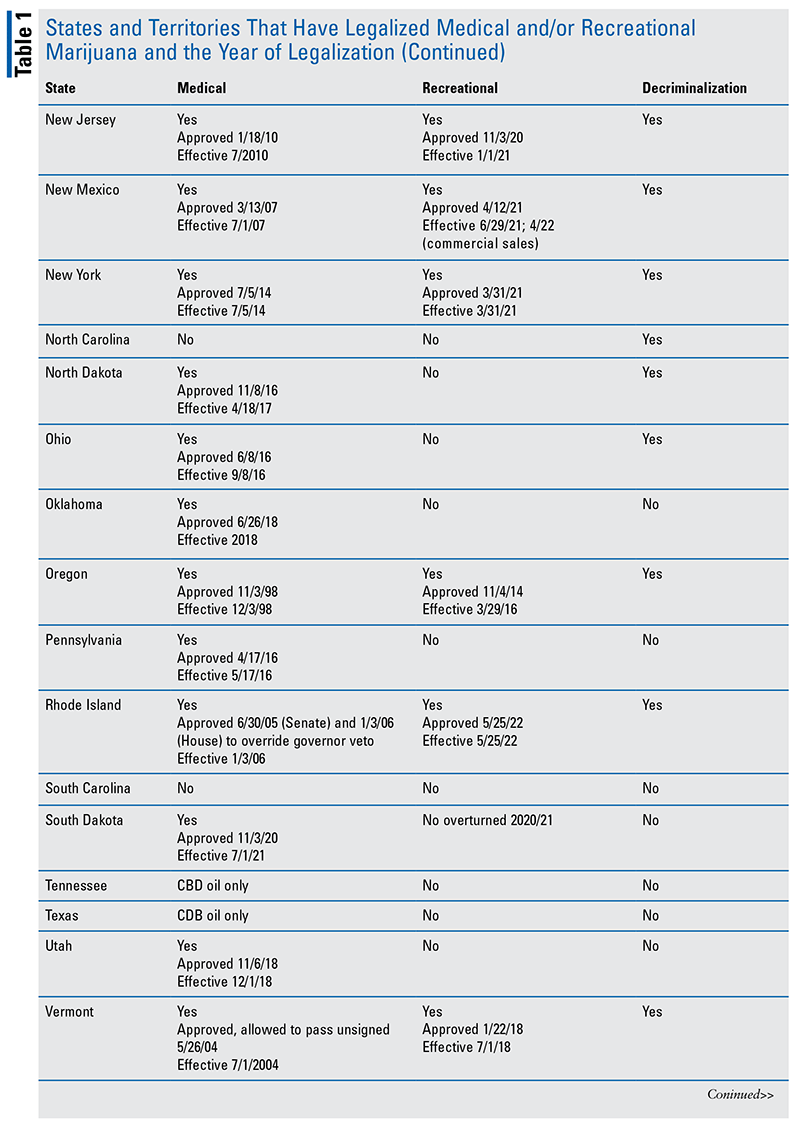
As of June 2022, 37 states (and Washington, DC) have legalized medical marijuana (MM), and 20 states (and DC) have legalized recreational marijuana (RM) (see TABLE 1 in Addendum).7-10
Marijuana is available in numerous forms, but the two primary methods of consumption are inhalation (e.g., joints, blunts, vaping) or ingestion of cannabis edibles (CEs).11 Increased access to cannabis as a result of legalization has resulted in a number of public health concerns, including an uptick in adolescent use and accidental pediatric exposures, which have contributed to emergency department (ED) visits, hospitalizations, and even death.11 The American Academy of Pediatrics favors the decriminalization of marijuana but not its legalization.12
In states that have legalized MM, individuals are 1.78-fold more likely to use CEs than in states that have not legalized MM. This difference is even 2.04-fold greater when vaping is considered.13 Teens aged 14 to 18 years who live in states that have legalized MM and/or RM were 2.24 times more likely to have tried CEs than those in states that have not legalized marijuana. Other factors that were significantly correlated with an increased risk of using CEs include longer duration of legalization (odds ratio [OR] 3.82, 95% CI 2.96-4.94), higher dispensary density (OR 3.31, 95% CI 2.56-4.26), and home cannabis cultivation (OR 1.93, 95% CI 1.50-2.48); the latter factor was also associated with a younger onset of cannabis use.14
Drawing on the experiences of Colorado, one of the first states to legalize both MM and RM, a cautionary warning has been issued about the negative health and safety effects of cannabis on healthcare resources, mental health (i.e., an association with psychosis and schizophrenia, depression, anxiety, suicide, possible link to use of other illicit substances, development of cannabis use disorder); negative social outcomes (e.g., poorer educational outcomes, lower income, unemployment); structural, functional, and chemical brain changes; use during pregnancy and lactation; occurrence of cannabinoid hyperemesis syndrome; increases in pediatric intoxications; increased motor vehicle accidents; adverse cardiovascular and respiratory effects; contamination with mold, heavy metals, and pesticides; suprapotent D9-tetrahydrocannabinol (THC) concentrations; and hash oil burns.15-17
Available Cannabis Forms With a Focus on Edibles
Cannabis is available in numerous forms, including liquid concentrates (e.g., vaping fluids), resins (e.g., dabs), botanicals (e.g., leaves, buds, rosin), wax, shatter, oils (e.g., butane hash oil), or edibles.18 Sales of CEs reached approximately $3.6 billion in the United States in 2021. This is expected to climb to $8.2 billion by 2025.19 Up to 30% of cannabis users have reported consuming a CE or beverage containing cannabis.20 This prevalence of CE use by teens was found to vary from about 21% among 10th-grade students in Los Angeles (polycannabis use was common) to 33% among 9th to 12th grade students in Northern California; 82% of past month cannabis users had consumed CEs.21,22
CEs are available as baked goods (e.g., brownies, cookies, muffins, toaster pastries); gummies and candy (e.g., lollipops, caramels, chocolates, hard candies, gums, rice/marshmallow treats); marijuana-infused drinks (e.g., juices); lozenges; and butter used in the baked goods. These items are enticing to young children and pets.11,20,23-25 A candy bar made with THC may contain four or more times THC than what is considered a “safe adult dose.”
Consumption can result in anxiety and psychotic-like symptoms.2 CEs are indistinguishable from normal food items as they lack the characteristic smell of marijuana that occurs with smoking, further adding to their risk of accidental ingestion.11,24 Since CEs avoid combustion, this form of cannabis is often preferred as a healthier alternative, especially by those who want to avoid inhalation of marijuana and its burn products; who want to use cannabis discreetely (e.g., students); and who use MM.11,20 Some young women/teenage girls have also expressed a preference for the use of CEs to avoid smelling like they have used marijuana, which they feel may make them more vulnerable to a sexual assault.26
Another issue with CEs is that often they lack a homogenous concentration of THC throughout, which can make accurate determinations of exposure difficult following an acute intoxication.20
Over the years, the potency of the THC, the active ingredient that produces the desired psychiatric effect, has markedly increased. In the 1980s, RM was composed of <2% to 4% THC, but by 2012 this increased to 12%.27 Currently, cannabis concentrations are around 20% THC, but THC concentrations may be as high as 80% to 90% in oils, waxes, and dabs.15 Therefore, any ingestion of cannabis by a young child should be considered serious.28 Another issue is that research marijuana available through the National Institutes of Health only contains 3% to 6% THC, not the >20% THC currently in use. Therefore, these substances are being utilized in the absence of scientific data.29
The bioavailability of THC varies by dosage form, preparation, and route of administration. The bioavailability of inhalation cannabis is >2% to 56%, with a peak effect seen in 10 to 30 minutes and a duration of effect of 4 hours. The bioavailability of oral cannabis is in the range of 10% to 20% but may be as low as 6% to 10%.11,20,27,30 Peak effect is delayed for one-half to 3 hours (up to 8 hours) because the drug needs to first be metabolized. Weight, metabolism, gender, and eating habits can impact the onset of effect with CEs.20,27 This delayed effect can lead to overconsumption.11,30 The duration of CEs is longer lasting than for inhalation products, and psychoactive effects can be seen for up to 12 hours.30 One downside of CEs is that the psychiatric effects may be unpredictable.20,31,32
Pharmacokinetics of oral cannabis appears to be dose- and formulation-dependent.31,33 The metabolite, 11-hydroxytetrahydroxycannabinol (11-OH-THC), which is more potent than D9-THC, appears in higher concentrations in blood when cannabis is ingested than when it is inhaled.20 It is estimated that 1 mg of D9-THC in a CE may produce similar behavioral effects as 5.71 mg of D9-THC in inhaled cannabis.20
Data in pediatric cannabis pharmacokinetics are limited to accidental exposures. In one case series involving 10 infants who experienced an accidental oral ingestion of cannabis, there was no correlation between plasma THC concentrations and symptoms. However, a major metabolite of cannabis, tetrahydrocannabinol carboxylic acid (THC-COOH), was found to be >3,000 ng/mL in two infants who experienced seizures.34
Current evidence indicates that THC, cannabidiol (CBD), and cannabinol (CBN), major cannabinoids in marijuana, inhibit CYP2C9 (data are conflicting for THC), and CYP1B. THC and CBD also inhibit CYP2D6, CYP2C19, CYP2B6, CYP2J2, CYP3A4, and carboxylesterase 1 (CES1); CBD may also inhibit CYP3A5/7 and CYP1A1/2. THC induces CYP1A1/2. UGT1A9 is inhibited by CBD and CBN. While UGT2B7 is activated by CBN, it is inhibited by CBD. There are no data on the effects of THC on UGT1A9 or UGT2B7. These effects may vary by cannabis exposure and type, e.g., the induction of CYP1A2 through cannabis smoking.35,36
The Problem With Cannabis Edibles
On May 13, 2022, the FDA issued a consumer warning about the accidental ingestion by children of food products containing THC.37
A study analyzed 256 photos of cannabis-infused edibles packaging sold in 24 states, Washington, DC, and Puerto Rico from May 2020 to August 2021 and found that 15% of the packaging were knockoffs of brand-name products. Features that would appeal to children such as human/nonhuman creatures, flavor images, and flavor text were present on 23%, 35%, and 91% of labels, respectively. Additionally, these packages were brightly colored, with an average of five colors. The authors concluded that existing laws were inadequate in preventing these products from being appealing to youth and could contribute to accidental ingestion or early initiation of cannabis.38
Another study found that of the 731 photos of cannabis products identified from an online survey of cannabis users and through personal contact, 36% were CEs, and of these, 8% were copycat, lookalike products. These packages were found to have high concentrations of THC, with some containing a mean of 459 mg/package or 47.5 mg/dose. Packaging was also attractive to children.39
These packaging concerns regarding CEs invoke the tort-law concept of “attractive nuisance” in which they represent a hazardous condition that foreseeably attracts children too young to fully understand the risk involved with the use of these products (like the Joe Camel ads for cigarettes).2
Some states have limited CEs’ serving size to 5 mg THC and a total package limit of 50 mg to 100 mg THC in an attempt to reduce overconsumption. Alaska does not allow for the sale of edible MM.18
Since cannabis is illegal at the federal level, the Poison Prevention Packaging Act requirements are not binding, and states are responsible for regulating labeling and packaging. Therefore, state requirements for child-resistant packaging (CRP) vary. Further, even in states where child-safe packaging is mandated, once the product is opened at home, pediatric exposures can occur.28
Older children and adolescents may be exposed to social media that condone or normalize use of CEs and even offers advice on recipes for homemade CEs.25,40-42 There is a decreasing perception of risk of harm associated with cannabis products, especially CEs, which can contribute to increased use in adolescents.43,44 See SIDEBAR 1 for take-home points about CEs.45

Recognizing Acute Toxicity From Cannabis in Pediatric Patients
Children are especially vulnerable to cannabis toxicity due to their smaller body size, resulting in higher THC concentrations following the ingestion of even a limited amount of marijuana.30 Clinicians should have a high index of suspicion for cannabis poisoning when treating a young child who presents with altered mental status or an adolescent with behavioral issues. Cannabis toxicity can be mistaken for postictal states, encephalitis, or sepsis. Probing history taking is essential to ascertain the nature of the exposure, to determine the product involved, and to estimate total THC exposure. This may be difficult because parents and caregivers may not be forthcoming because of fear of being charged with child abuse or neglect.27,30
Standard workup should include a urine drug screen, preferably with gas chromatography–mass spectrometry, which is highly specific for cannabis ingestion although it does not provide information on the time frame of exposure. Blood glucose, blood gasses, and electrolytes should also be checked. Testing early upon presentation would help reduce time to diagnosis and unnecessary, costly tests such as brain imaging studies or lumbar puncture.27,30 However, a positive drug screen does not necessarily exclude other possible diagnoses, which may exist concurrently.46
Cannabis toxicity has a variable presentation depending on the age of the patient and route of exposure. Children most often present with central nervous system (CNS) depression (i.e., drowsiness, lethargy, ataxia, coma), whereas adults may exhibit CNS excitation; adolescents display a mixture of CNS depression and excitation. Oral exposure in young children may represent hand-mouth behavior and a predilection for desserts and candy, whereas in older patients, this may be due to intentional overconsumption since the onset of effects of CEs is delayed.18,30
Other common symptoms seen in pediatric cannabis intoxication include tachycardia, confusion, agitation, anxiety, dizziness, irritability, hypotonia, and bilateral reactive mydriasis. Children may also present with nausea, vomiting, bradycardia, bradypnea, hypotension, respiratory depression requiring intubation, tremor, hallucinations, nystagmus, slurred speech, muscle weakness, and seizure.27,30,46-48 In adolescents, 5 mg to 20 mg of THC from an edible can lead to impaired attention, concentration, short-term memory, and executive functioning.27
High-potency cannabis has been linked to an increase in first-episode psychosis.49 Psychosis has also been reported in adolescents and young adults following ingestion of CEs, which can in some cases persist for several days.20,48,50,51 Psychosis may present as dream-like euphoria, delusions, hallucinations, paranoia, and depersonalization and may exacerbate underlying depression or anxiety.48 Panic attacks and hyperemesis syndrome have also been observed with increased use.24 ED visits for acute psychiatric symptoms were more commonly associated with CEs than with inhalation exposure in adults (18.0% vs. 8.4%, P <.001).52
There is growing concern that cannabis may have adverse cardiac effects. Among marijuana’s adverse physiological effects are tachycardia, premature ventricular contractions, atrial fibrillation (AF), and ventricular arrhythmias. CEs appear to be more likely to result in adverse cardiovascular effects due to their increased systemic absorption and their slower onset of action and time to peak effect. In states where cannabis has been legalized, there has been an increase in hospitalizations and ED visits for acute myocardial infarction and arrhythmias, including AF. These cardiac events have been reported in young men who did not have a history of ischemic heart disease and who were heavy and/or frequent users.36,53-55 An increase in cerebrovascular accidents have also been reported. Peripheral arteriopathy and cannabis arteritis has been reported among those who smoke marijuana. These concerns have led the American Heart Association to issue a scientific statement on MM, RM, and cardiovascular health.36
There is also concern that CEs may contribute to the initiation of marijuana use, reduce the average age of initiation since these products are often child-friendly, and increase the frequency and intensity of cannabis use over time.2 Adverse effects of adolescent cannabis use include impaired cognitive functioning, increased risk of developing cannabis use disorder, poor academic performance, elevated risk of developing psychotic behaviors, and increased participation in risky behaviors.56
There is no antidote for cannabis intoxication. Management is symptomatic and includes observation for 8 to 12 hours or until mental status returns to baseline. Gut decontamination with activated charcoal is not effective.30 Respiratory depression, intubation, and ICU admission are more common following the exposure to concentrated cannabis products, especially in young children.18 Cannabinoid receptor antagonists to manage overdoses are currently under investigation.57
D8-THC, an isomer of D9-THC, which exhibits psychoactive properties similar to D9-THC, can also be found in foodstuff and can lead to acute encephalopathy in pediatric patients.15,58,59
Increased ED Visits and Hospitalizations From Pediatric Cannabis Exposure
Since the legalization of RM and/or MM, there has been an increase in pediatric ED due to acute cannabis toxicity. Much of the data that are available has come from Canada, which nationally legalized cannabis in 2018, national U.S. data from poison control centers (PCCs), and data from Colorado, which initially legalized MM in 2000, then RM in 2012, and finally, CEs in 2014 (see TABLE 2 in Addendum). Detailed published data on pediatric cannabis toxic exposures from Canada and the U.S. are found in TABLE 2 in Addendum.4,18, 22,28,29,49,60-96
Mitigating Strategies to Limit Pediatric Exposure to CEs
Cannabis is regulated at the federal level in Canada. Federal Canadian law mandates that CEs be sold in plain, single-colored packaging, with limited brand elements and with rotating health warnings. The plain, single-color packaging requirement is intended to decrease the appeal of edibles to young children. Under Canadian law, a serving size is defined as 10 mg of THC per edible unit or serving. Nutritional information and a list of ingredients must also be provided on CE labeling.97,98 Unit-dose packaging of edible cannabis products eliminates the need for dose calculations and has been found to enhance consumers’ ability to correctly identify a standard serving size. This may prevent overconsumption and toxicity.99
A survey was conducted in Canada to examine the effect of plain labeling measures on consumer appeal. Despite these restrictions, edible gummies were still rated as appealing by teens and young adults and were considered to be more youth-oriented than joints or cannabis oil.100
In the U.S., labeling requirements for both MM and RM products vary from state to state. This has led to a lack of standardization in formulation and quality control in the CE industry, as inaccuracies have been observed when product labeling was compared with product content.20 There is limited research on the labeling requirements for THC products, but what has been found is that consumers have a difficult time understanding THC content expressed in milligrams or as percentages.101 THC content in CEs can range from being negligible to containing several hundred milligrams of the psychoactive compound.102 One proposal has been to standardize a THC unit at 5 mg of THC for all cannabis products and methods of administration.103
In 2016, California Assembly Bill No. 266, which was part of the Medical Marijuana Regulation and Safety Act, delineated requirements for MM labels and packaging, including CEs. An investigation found that while 90% of products were labeled and in a tamper-resistant package, only one out of 20 products were in CRP.104
Colorado requires that cannabis products be sold in CRP that conforms to the federal consumer product safety regulations. Packaging must also be opaque and resealable if not for single use. It also requires that each 10-mg THC serving carry a universal THC symbol and packages to be limited to 10 mg THC, except where labeling individual servings is infeasible.102,104 A survey of CEs consumers in Colorado showed that fewer than 15% were aware of what constituted a standard serving size of THC.102
Michigan law does not allow CEs to be in a shape or labeled in a way that would appeal to minors. It also forbids packaging that can be easily confused with commercially sold candy, and it requires the use of opaque CRPs.92
Another strategy that has been proposed to combat the public health issue of availability of large amounts of THC, which can lead to accidental ingestion by children or to diversion, is to limit sales of cannabis based on total THC content as opposed to product weight. Current laws allow for the sale of >500 THC-standardized doses (up to 2,283 doses per transaction) of THC in a single transaction based on median product potencies.105
A study conducted in 2019 of government websites of states that allow the sale of cannabis for recreational use found that only five states’ product labeling warn about harm to youth or fetuses.106
Regulatory recommendations and model regulations for cannabis packaging and labeling have been proposed by the Council on Responsible Cannabis Regulation and the National Cannabis Industry Association (https://masscannabiscontrol.com/wp-content/uploads/2017/12/111717CannabisPackagingandLabelingRegulatoryRecommendationsforStates.pdf). Among these are CRP, liquid unit measurement, use of opaque packaging, prohibiting packaging that is attractive to minors or resembles certain commercially available products, and requiring packaging to protect contents from contamination.
The American College of Medical Toxicity has developed a position statement on addressing and mitigating pediatric cannabis exposures (see TABLE 3).107

Although published in June 2018 and in need of revisions, a quick reference listing is available on cannabis labeling requirements by state (http://www.weberpackaging.com/pdfs/Cannabis%20Laws%20by%20State.pdf.)
Counseling to Prevent Accidental Pediatric Cannabis Overdose
Pharmacists need to educate parents and pet owners on the safe storage of CEs, which includes keeping these products in a locked and hidden area. This is especially important and urgent given that CE ingestion has been found to be a strong predictor of ICU admission in children.65 In a survey of adult visitors to a pediatric ED who had children younger than age 18 years, it was found that 14.5% reported using cannabis in the home in the past 6 months; 39% of these respondents used CEs. While 55% reported keeping their cannabis locked, only 45% kept their marijuana locked and hidden, and only 16% reported having received safe storage information from the dispensary.108
Pharmacists should discourage the purchase of copycat products that look like foodstuffs that are geared toward children. They should also instruct patients on how to read edible CEs’ labels to determine THC content. Pharmacists need to educate parents and other healthcare professionals on how to recognize the signs and symptoms of cannabis toxicity and should encourage them to have the PCC number readily available. This information should also be relayed to babysitters and other caregivers.11
Cannabis is the most commonly used recreational drug by pregnant and lactating women.109 Pharmacists should also counsel women trying to conceive, expectant mothers, and women who are breastfeeding to refrain from using cannabis.110 There is a paucity of data on the effect of CEs during pregnancy and lactation, and most data (if described) are based on inhalation exposure. However, given that blood THC levels are higher and more sustained with CEs than with inhalation products, one can speculate that the effects may be even greater than what is seen with inhalation exposure.
From 2009 to 2017 both the frequency of cannabis use in the year before pregnancy and during pregnancy were found to increase from 6.8% to 12.5% and from 1.95% to 3.38%, respectively.111 D9-THC is measurable in breast milk for up to 6 days following maternal marijuana use. Sixty-four percent of women in this study were exposed to cannabis via inhalation.112 For women with a cannabis-use disorder, data from Canada revealed that maternal substance use before childbirth increased the risk of future drug poisonings 1.84-fold, especially in the first 2 years of their child’s life (hazard ratio 1.84, 95% CI 1.01-3.34).113
Evidence is also pointing to a bidirectional relationship between prenatal cannabis inhalation exposure and behavioral problems, especially in female children at age 2 years. These behavioral issues were associated with higher maternal cannabis use 1 year later. Additionally, smoking more joints per day during pregnancy was associated with more maternal anxiety and depression and greater attention problems in offspring when assessed at age 3 years.114 Further, maternal cannabis use may be a risk factor for early initiation of cannabis use (i.e., initiation started at age 16 years vs. age 18 years in offspring), and paternal cannabis-use disorder has been associated with an earlier age of a daughter’s initiation of cannabis use, alcohol use, and sexual intercourse.115,116 It is important to keep in mind that these studies offer insight into potential correlations, but they do not establish causality due to their retrospective, often observational nature. Social determinants of health also need to be addressed when attempting to establish causality.
Under the federal Child Abuse Prevention and Treatment Act, pharmacists are mandatory reporters for suspected cases of child abuse and neglect.117 There are penalties, often in the form of a fine or imprisonment, for failing to report suspected cases of child abuse or neglect.118
Conclusion
Due to past federal restrictions, the impact of marijuana on health outcomes has only begun to be evaluated. As evident by real-life experiences, although legalization and decriminalization may have addressed social inequities regarding the judicial system, they have come at the price of increased pediatric cannabis intoxications and earlier adolescent marijuana exposures. CEs have played a major role in both of these negative consequences. Pharmacists need to stay current of the latest high-quality research in the field of cannabinoid science, and they must be at the forefront of educating society about the public health concerns associated with the increased use of cannabis, especially in children.
Table 1 Addendum.
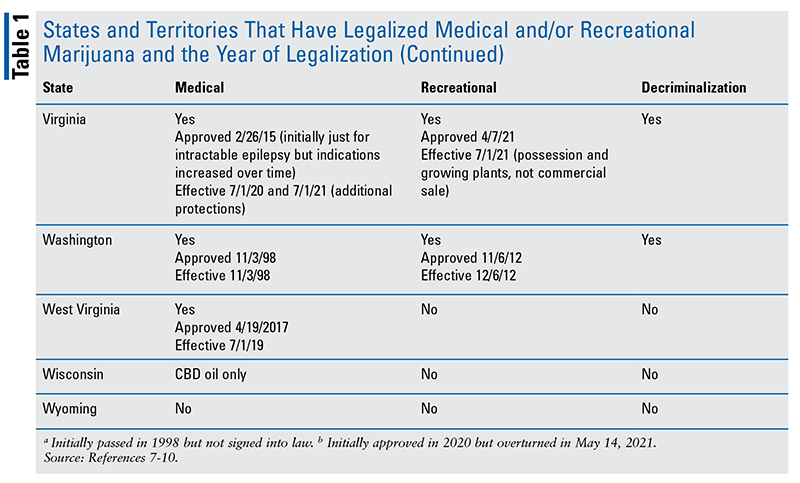
Table 2 Addendum. Published Data on Pediatric Cannabis Toxic Exposures From Canada and the U.S.
Canada
Medical marijuana and recreational marijuana were legalized in Canada in 2001 and 2018, respectively. Canada had a two-step approach to legalization of marijuana: initially flowers, seeds, and oils in 2018 then after 1 year in 2019 they added an expanded selection of products including edibles.60-61
Baseline data from prior to recreational marijuana legalization on cannabis poisonings of those aged <16 years who were treated in the ED at a children’s hospital from January 1, 2016, to December 31, 2018, found that there were 114 poisonings related to cannabis use and fewer than 10 poisonings that were due to the inadvertent ingestion (median age: 3 years).62
As early as 2019, evidence started emerging that cannabis edibles were having a harmful effect on children. Data from the Canadian Paediatric Surveillance Program from September to December 2018 revealed 16 cases of serious adverse events associated with cannabis, with 6 involving young children who accidently ingested cannabis edibles and required hospitalization.63
A search was conducted to establish a temporal pattern for cannabis-related injuries and poisonings between the period of April 1, 2011, and August 9, 2019, of the electronic Canadian Hospitals Injury Reporting and Prevention Program (eCHIRPP) database, which included data from 19 EDs throughout Canada. During this time, there were 2,823 cannabis-related cases, of which 158 cases (5.6%) involved cannabis edibles. Of these 158 cases, 87.3% involved children. The annual percent change in for edible-related cases involving children between 2016 to 2018 rose 35.6%. Children aged <17 years made up 67.8% of all cannabis-related cases. Two-thirds of pediatric exposures were unintentional. While 15.1% of cannabis-related cases were associated with serious injury, proportionally more pediatric patients experienced a serious injury (56% aged <17 years).64
A retrospective cohort study of children aged 0-18 years who presented to a pediatric ED in Toronto, Canada with cannabis toxicity during the periods of January 1, 2008, and December 31, 2019, and January 1, 2008, to April 12, 2017, represented the prelegalization period and April 13, 3017 to December 31, 2019, referred to the peripost–legalization period and showed that there were 298 pediatric ED visits for cannabis exposure. While over three-quarters of exposures took place during the prelegalization period (77.8%) and 22.1% took place in the peripost-legalization period, there was a higher pro-portion of children admitted to the ICU in this latter period (4.7% vs. 13.6%, P = .02). This increase in clinical severity occurred despite no significant difference in the median monthly number of cannabis-related ED visits between the two time periods. Both respiratory involvement (P = .05) and altered mental status (P <.01) were significantly more common in the peri-post period (65.9% vs. 50.9% and 28.8% vs. 14.2%, respectively) as was the use of therapeutic interventions, such as lumbar puncture and IV fluids (P = .02). The peripost saw a much younger population treated in the ED, with 12.1% being aged <12 years compared with only 3.0% in this age group in the prelegalization period. Both unintentional exposure (P = .002) and edible ingestion (P = .01) were more common in the peripost-legalization period (14.4% vs. 2.8% and 19.7% vs. 7.8%, respectively). Edibles were associated with a more than 4-fold increased risk of ICU admission (odds ratio 4.1, 95% CI 1.2-13.7, P = .02) and were considered an independent predictor of this outcome.65
Providing more comprehensive data, a repeated cross-sectional study was conducted in Ontario, Canada, that identified all ED visits and related hospitalizations due to cannabis exposure in children aged 0-9 years over three periods: Prelegalization: January 2016-Sepember 2018; Period 1 (period of legalization of flower products) October 2018-January 2020; and Period 2 (period after commercial edibles became available) February 2020-March 2021. Investigators found that of the 522 ED visits (mean age of patients 3.8 years) that occurred during these periods, 24.7% (20 visits), 23.4% (29 visits), and 38.5% (122 visits) occurred during prelegislation, Period 1 and Period 2, respectively. While there was an increase in pediatric ED visits related to cannabis exposure, there was a decrease in total poisoning-related pediatric ED visits. Of these 522 ED visits, 19 or 3.6% resulted in an intensive care unit admission.66
Administrative data for all (total number: 14,697,778) ED visits in Ontario found a similar trend in older adolescents and young adults aged 10-24 years as evidenced by a 4.8-fold increase for cannabis-related ED visits between 2003 to 2017. Cannabis-related ED visits increased from 3.8/10,000 youth in 2003 to 17.9/10,000 youth in 2017. Both the severity of the intoxication and the rate of hospitalization were increased, as evidenced by 88.2% of cannabis-related visits rated as severe compared to 58.1% of noncannabis-related ED visits and by 19% of cannabis-related exposures versus 5.8% of noncannabis related exposures resulting in a hospital admission in 2017.67
United States
National data
Data from 2004-2011 from DAWN (the Drug Abuse Warning Network) showed a significant increase in ED visits with the largest increase in cannabis-only (vs. cannabis-polysubstance) exposures in the 12-17-year-old range. For all ED visits in those > age 12 years, significant increases were observed for both cannabis-only and cannabis-polysubstance exposures. Non-Hispanic blacks had the highest increase in ED visit rates across racial/ethnic groups. Type of cannabis exposure was not specified.68
According to data from the National Poison Data System (NPDS) from between 2005 to 2011, decriminalization and/or the availability of medical marijuana were found to be associated with an increase of 30% per year nationally for accidental pediatric cannabis exposures compared with states in which cannabis remained illegal. Being in the transitional state from nonlegal to decriminalized status was also associated with increased pediatric exposure. These exposures were not associated with long-term mortality or mortality.69
National poison control center data on single-substance edible cannabis exposure reported to the NPDS from January 2013 to December 2014 showed that of the 438 calls received for cannabis-related exposures, one-quarter (24.9%) occurred in children, with the most common age group being age <5 years. Colorado and Washington had the most cases. Over 90% of calls occurred in states that had decriminalized medical and/or recreational marijuana. Common symptoms seen in those aged years 5 and younger were drowsiness, lethargy, tachycardia, agitation, irritability, and confusion. Although there were no deaths, 3 patients, including two aged <10 years, required intubation.70
A systematic review was conducted of published reports of unintentional cannabis ingestions in children aged <12 years revealed that unintentional pediatric cannabis ingestion is a serious public health issue. Most exposures were secondary to ingestion of resins, cookies, joints, medical cannabis, candies, beverage, hemp oil, and from passive inhalation. Lethargy occurred in almost three-quarters of patients, although tachycardia, mydriasis, and hypotonia were also common. Of the 3,582 children, 18% required admission to the pediatric ICU and 6% were intubated.28
Data from the Agency for Healthcare Research and Quality’s Healthcare Cost and Utilization Project (HCUP) 2016 Nationwide Emergency Department Sample (NEDS) found that among those aged >12 years who were treated in the ED, patients experiencing cannabis poisoning were significantly more likely to meet criteria for a psychotic, anxiety, mood, or behavioral/emotional disorder and that rates of admission for cannabis poisoning were almost 2 times greater among those with psychotic disorders.71
Data from 2015-2018 on noncombustible marijuana use among 9,097 12th graders from Monitoring the Future, a longitudinal study examining issues of substance abuse, found nearly one-third of seniors reported having used marijuana in the past 12 months. Among these students, about 40% were exposed via ingestion. Vaping and edible replaced smoking marijuana between 2015 and 2018. Daily use of cannabis was also more common among those who vaped or consumed edibles compared to those who smoked marijuana.72
A cross-sectional study examining data from the NPDS on cannabis use for January 2017 through December 2019 found that of the 28,630 exposures nationwide, 19.3% were due to edibles. Edibles accounted for almost 37% of exposures in children.73
Data from the NPDS on the impact of COVID-19 on unintentional pediatric cannabis exposure in children aged 6 months to 5 years during the first 9 months of the pandemic (pre-COVID-19 [January 2017-March 2020] to April 2020 to December 2020 [COVID-19 period]) demonstrated that within the 7,679 unintentional pediatric exposures, there was a significant increase of 3.1% per month during the initial COVID-19 stay-at-home orders.74
In another study using data from the NPDS specifically examining cannabis edible-related exposures in children aged 0-9 years reported to U.S. poison centers between January 1, 2017, and December 31, 2019, found that of the 4,172 cannabis exposures, 45.7% were due to edibles. Exposure to edibles rose more sharply than did exposure to nonedibles. Children aged 3-5 years accounted for 43.1% of exposures, and of this group, almost three-quarters (72%) were exposed via ingestion. While 15.4% experienced moderate medical outcomes, 1.4% had major medical outcomes. Not only were pediatric exposures more frequent (8.9 per 100,000 vs. 3.4 per 100,000, respectively), among states that had legalized cannabis use, these exposures more often involved edible products (62% vs. 46%, respectively).75
In one of the most comprehensive studies to date using NPDS data, researchers determined the rate of critical care interventions in children aged 6 months to 12 years who were admitted to pediatric ICUs following an unintentional single-substance cannabis exposure during the period of January 1, 2000, to December 31, 2020. During this period, there were 12,882 cases. Both the percentage of cases seen in the hospital increased over time from 43.8% in 2000 to 54.6% in 2020, as did the severity of these events, with 9.5% admitted to the PICU in 2000 and 14% admitted in 2020. Respiratory depression occurred in 8.3% of children admitted to the PICU, and 4.9% required intubation. Clinically significant effects included respiratory depression, hypotension, and bradycardia. while the most common symptoms included CNS depression, tachycardia, vomiting, and ataxia. Although over 75% were discharged from the PICU in fewer than 24 hours, 1.1% were there for a week. The number of cases increased 89.6% from 2019 to 2020. Ingestion accounted for 92.8% of all pediatric exposures. Of the 875 children who were admitted to the PICU, 35 sustained 1 or more seizures.76
Cannabis-related ED visits were tracked using NEDS data from 2006-2018 and on average increased 12.1% annually from 2006-2014. This rate jumped to 17.3% between 2016-2017 then dropped to 11.1% from 2017 to 2018. These rate changes were all statistically significant. A significant rate increase was observed for those aged 0-14 years during the study period.77
Colorado
As a state, Colorado has generated the most data about trends in cannabis use among youth. Colorado approved the use of medical marijuana in 2000 with the passage of Amendment, 20 but 2009 represents the first year of significant growth in the dispensaries and medical marijuana applications in Colorado as a result of the Ogden Memo. This was followed by the approval of recreational marijuana in 2012 with the passage of Amendment 64, which took effect in 2013 and allowed for personal possession and growth limits for recreational marijuana but not commercial sales. In 2014, recreational and medical marijuana became fully regulated and commercialized and edibles were made available for sale.15,78
Following the legalization of medical marijuana, there was a significant increase in hospitalizations among children aged >9 years, from 15 per 100,000 hospitalizations in 2001-2009 to 28 per 100,000 hospitalizations in 2010-2013. Similarly, cannabis-related ED visits significantly increased from 22 per 100,000 ED visits 2010-2013 to 38 per 100,000 ED visits in January-June 2014.4
Infused edibles made up 40% of legal cannabis sales in 2014. This was the same year that Colorado attempted to ban the sale of edibles following several deaths that were associated with their use.22
One of the most prominent cases to come from Colorado was published in the CDC’s Morbidity and Mortality Weekly Report. This involved the death of a 19-year-old male who jumped to his death following the consumption of a cannabis-infused cookie. Not feeling an expected high 30-60 minutes after consuming a single piece of the cookie (~10 mg), he consumed the rest of the cookie, which contained a total of 65 mg. The youth did not have history of substance use or mental illness. Autopsy results determined that marijuana intoxication was a chief contributing factor to his death.79
Wang et al conducted a retrospective review of charts from a children’s hospital in Colorado and the regional poison center (RPC) during the period of January 1, 2009, to December 31, 2015. The median age of cannabis exposure was around 2 years (hospital: 2.4 years, RPC 2 years). Cannabis edibles (i.e., cookies, brownies, cake, candies, and popcorn) accounted for 48% of exposures seen at the hospital. There was a statistically significant increase in the mean rate of hospital visits when comparing the period prior to legalization and the timeframe postlegalization (1.2/100,000 population vs. 2.3/100,000 population 2 years pre- and postlegalization, respectively) and RPC cases increased more than 5-fold from 9 in 2009 to 47 in 2015. Two children out of the 81 seen at the children’s hospital required respiratory support, including intubation. Among the 163 exposures reported to the RPC, 52% of exposures were due to edibles. An 11-month child died after being found unresponsive with wide complex tachycardia and severe metabolic acidosis; urine drug screen was positive for THC and cause of death was myocarditis. A similar study by the same lead researcher found that rates of cannabis-related hospitalizations increased from 274 per 100,000 hospitalizations in 2000, which was the period prior to legalization in Colorado, to 593 per 100,000 hospitalizations in 2015, 2 years after the legalization of recreational marijuana. There was also an increase in intentional marijuana exposures among those aged >9 years be-tween 2013-2015. Edibles were the most common type of exposure for children aged <8 years. There was also an increase in calls to the RPC regarding cannabis intoxication among those aged >25 years. Adolescent marijuana ED and urgent-care visits increased in states that had legalized medical and recreational marijuana. Marijuana-related visits to the ED or urgent care center of a tertiary care children’s hospital system in Colorado increased from 161 in 2005 to 777 in 2015. Additional data demonstrated an overall rate of cannabis-related visits rising from 1.8 per 1,000 ED/UC visits in 2009 to 4.9 per 1,000 ED/UC visits in 2015. There was also an increase in behavioral health evaluation from 84 to 500 during this same period. The median age of the study population was 16.2 years.29, 49,78
An examination of both children’s hospital and the RPC data from between 2009 and 2017 showed that in 2017, visits to the children’s hospital more than doubled from 16 in 2016 to 36 in 2017 and RPC calls increased by almost 50% to 67%. Twenty-one percent of children were hospitalized with 10% being admitted to the PICU. Similarly to previous data, edibles accounted for 52% of exposures. Social work and child welfare consultations also increased during this time. This study identified additional safety concerns involving the occurrence of nonaccidental traumatic injuries and coexposure to other illicit substances. The median age of this population was 3.0 years.80
Data from the RPC from January 1, 2000, to December 31, 2018, found that there was a 19.4% increase between 2017 and 2018 in cases of pediatric cannabis exposure. The largest increase since 2014 has been in those aged 0-8 years. Edible exposure continues to be problematic and significantly increased by 9.6 exposures per year from 2015 to 2018. Although the number of annual marijuana exposures reported to RPC had been stable through 2017, following the legalization and commercial availability of recreational marijuana products, there was an increase in pediatric exposures in 2018.81
Using data from a children’s hospital in Colorado, researchers conducted a chart review of 76 children aged 31 days to 20 years to determine if there was a dose-response relationship to THC in THC-naïve and nonnaïve children with clinical symptoms and outcomes. Despite uncertainty about the reported dose of the exposure, it appeared that a mean level of exposure of THC of 7.13 mg/kg in cannabis-naïve children had an apparent direct relationship between the dose ingested, level of medical intervention needed, and hospital disposition. Hospitalization was more likely in naïve children when the ingested amount was >5 mg of THC per kilogram of body weight. The highest doses resulted in PICU admissions. Lethargy and somnolence were more common in the cannabis-naïve group compared with the nonnaïve group (84% vs. 26%, P = .01). The opposite association was seen for cognition, perception, and behavioral issues (4% vs. 11%, P = .01). The duration of toxicity also lasted longer in the naïve group. Edibles (mostly cookies) accounted for 66% of exposures in the cannabis-naïve group but only 13% in the nonnaïve group. Both the rate of hospitalization and the length of stay were higher following exposure in cannabis-naïve patients.82
Others have also reported on an increase in the severity of symptoms and ED visits due to the high THC concentration in edibles.83,84
California
California legalized medical marijuana in 1996. Twenty years later in 2016, it also legalized recreational marijuana. In 2018, a case series was published involving the inadvertent exposure of 12 children and 9 adults to cannabis edibles. Although all patients were discharged within 12 hours, the children presented with more severe symptoms including leukocytosis and lactic acidosis.85-87
The authors also described a case of a fatal edible ingestion in a 65-year-old woman with a significant cardiac history who sustained a severe ischemic cardiovascular event following the ingestion of a commercial brownie containing 1,000 mg of THC.85-87
A tertiary hospital in California conducted a descriptive retrospective chart review between March 2013 to June 2020 of pediatric patients aged <18 years with a positive urine drug screen for cannabinoids. Investigators identified 422 cases, of which 71% occurred postlegalization of recreational marijuana. Of these cases, 8 occurred in patients aged <10 years (range: 13 months-10 years). Two of these children were admitted, and 2 were transferred to another hospital. Three of these cases involved ingestion of a cannabis edibles. In children aged 15-17 years, 43% presented with a chief complaint of suicidal ideations. Among this population, over one-quarter were positive for another substance; amphetamine coingestion occurred in 13%.85-87
An observational retrospective study that analyzed trends in cannabis exposure reported to the California Poison Control System from 2010 to 2020 found that edible exposure increased approximately 79% (from ~ 0% to 79%). This increase was due to cannabis-infused chocolate, candy, other edibles, drinks, and gummies. This increase was most obvious following recreational marijuana legalization in 2016 and following the initiation of retail sales in 2018. There were significantly increased cannabis exposures for the two time periods for those aged <13 years.88
Massachusetts
Medical marijuana was legalized in Massachusetts in 2012, and recreational marijuana was legalized in 2016.89
Using data from the Regional Center for Poison Control and Prevention (RPC), investigators tracked pediatric cannabis exposures from 2009 to 2016, which represented time before and after the legalization of medical marijuana. They found that the incidence of single-substance cannabis calls increased from 0.4 per 100,000 prior to legalization of medical marijuana to 1.1 per 100,000 following the passage of the legislation. This represented a 140% increase. While most teen exposure was secondary to inhalation, over 86% of exposures in the 0-4 years age group were due to ingestion. These poisonings occurred despite the presence of child-resistant packaging, nonchild–friendly packaging, and use of warning labels.89
In a retrospective chart review conducted at a single, tertiary-care academic medical center that covered a 28-month period, researchers found that were 32 cases of cannabis edible ingestion. Cannabis-infused chocolates and gummies accounted for almost three-quarters of ingestions, and an additional 22% included copycat sweets. Of these patients, 11 were hospitalized and 5 required respiratory support. Those under age 10 years, who made up 37.5%, were at risk for more severe symptoms and outcomes, including bradypnea, hypertension, and the need for hospitalization and respiratory support. The median dose of THC for those requiring respiratory support was 7.1 mg/kg. Other patient characteristics of those requiring respiratory support included female sex, presence of lethargy/somnolence, seizure activity, hypercarbia, bradypnea, hypoxia, and hypertension. The authors noted that the risk of pediatric cannabis edible exposure increased 5-fold after the opening of recreational cannabis dispensaries.90
Michigan
Michigan legalized medical marijuana in 2008 and recreational marijuana in 2016; however, this latter law did not go into effect until December 2018.91
A retrospective, cohort analysis was performed of consecutive patients diagnosed at 7 EDs in Michigan who were seen for cannabis intoxication secondary to ingestion of a cannabis edible between November 2018 and July 2020. Edibles were responsible for 17.1% visits (N = 155) for 909 patients. Approximately 6% (N = 9) were children aged <12 years. Cannabis edibles consisted mainly of baked goods (44.9%), candies/gum (27.9%), beverages (11.6%), and raw plant matter (7.5%). Presenting symptoms differed between cannabis ingestion and cannabis inhalation with the former being associated with psychiatric, cardiovascular, and neurologic symptoms and the latter being associated more often with hyperemesis and signs of acute intoxication.91
Another study retrospectively examined Michigan PCC data to describe temporal trends in pediatric cannabis exposure in the year of legalization of medical marijuana and 1 year following the legalization of recreational marijuana. Data were gathered from January 1, 2008, to December 31, 2009, for patients aged <18 years who reported a single-substance cannabis exposure to the Michigan PCC. A total of 1,392 cannabis-related calls were received, with the majority involving coexposures, which were excluded. This left 426 patients who had had a single-substance cannabis exposure; median age was 6 years. Of these 426 cases, 76.8% involved cannabis ingestion (69.4% from an edible source and 30.5% from a nonedible source). Children aged 0-5 years had the highest number of ingestions. There was a bimodal distribution, with 49% of total cases aged 0-5 years and 40% in those aged 13-17 years. There was an exponential growth pattern with the number of cases doubling every 2.1 years. Between 2017 and 2018, exposures increased 49 to 86, and this was mainly driven by an increase in edible exposure. In 2008, the year of medical cannabis legalization, there had been only 7 reports.92
Washington State
Data from Washington’s Poison Center data, toxiCALL, were analyzed for unintentional pediatric marijuana exposures prior to and after legalization/availability of recreational marijuana. Researchers found that of the 161 cases that were reported between July 2010 and July 2016, 81% occurred in the 2.5-year period following legalization. The median age of the children exposed to cannabis was 2 years and ranged from 0-9 years. Over 80% of exposures occurred in the child’s home. A spike in cases was seen following legalization in November 2012, and another spike was observed in July 2014 when marijuana became commercially available.93,94
In a subsequent paper, these same re-search group found that among pediatric patients with a median age of 21 months, there was a statistically significant difference between the 1.19 cannabis exposure events per year in the 6.75 years prior to legalization compared with 3.88 events per year in the 2.32 years following legali-zation.93,94
Oregon/Alaska
An observational study of Oregon/Alaska Poison Center (PC) data examining calls from between December 2015 and April 2017, which represented the early legalization period, found that of the 253 patients who presented with an acute cannabis exposure, 28.1% (N = 71) were children aged <12 years. Approximately 99% of children had an unintentional exposure. Almost all exposures were via ingestion (97.2%), with cannabis edibles accounting for over two-thirds (67.6%) of these exposures. The edible was either homemade or grown in over one-third of cases (35.2%). Of these 71 children, 4 (ranging in age from 9 months to 4 years) required admission to the pediatric intensive care unit; 2 experienced respiratory depression/failure resulting intubation. The sources of exposure included a commercial chocolate bar, homemade cookie, homemade butane hash oil, and a commercial concentrate.18
Other
Ireland
While recreational marijuana is illegal in Ireland, on June 26, 2019, the Minister of Health of Ireland signed legislation creating a 5-year pilot program allowing for the use of medical cannabis. During an 8-week period from March 17, 2021, 6 children, of which all except 1 child were younger than age 10 years, presented to an Irish pediatric ED with acute encephalopathy following the accidental ingestion of cannabis edibles. While 2 patients were discharged after 12 hours of observation, 4 children were admitted, including 1 who required management in the PICU.95,96
REFERENCES
1. Mead A. Legal and regulatory issues governing cannabis and cannabis-derived products in the United States. Front Plant Sci. 2019;10:697. Accessed May 14, 2022.
2. MacCoun RJ, Mello MM. Half-baked—the retail promotion of marijuana edibles. N Engl J Med. 2015 Mar 12;372(11):989-991. Accessed May 14, 2022.
3. Odgen DW. Memorandum from Deputy Attorney General David W. Ogden to all United States attorneys regarding investigating and prosecutions in states authorizing the medical use of marijuana. October 19, 2009, www.justice.gov/archives/opa/blog/memorandum-selected-united-state-attorneys-investigations-and-prosecutions-states. Accessed May 14, 2022.
4. Kim HS, Monte AA. Colorado cannabis legalization and its effect on emergency care. Ann Emerg Med. 2016 Jul;68(1):71-5. Accessed May 14, 2022.
5. American Civil Liberties Union. Marijuana legalization is a racial justice issue. April 20, 2019. www.aclu.org/blog/criminal-law-reform/drug-law-reform/marijuana-legalization-racial-justice-issue.
6. Kilmer B. How will cannabis legalization affect health, safety, and social equity outcomes? It largely depends on the 14 Ps. Am J Drug Alcohol Abuse. 2019;45(6):664-672.
7. National Conference of State Legislatures. State medical cannabis laws. www.ncsl.org/research/health/state-medical-marijuana-laws.aspx#4 Accessed May 14, 2022.
8. Defense Information Systems Agency (DISA). Map of marijuana legality by state. https://disa.com/map-of-marijuana-legality-by-state. Accessed May 14, 2022.
9. Brittannica ProCon.org. State-by-state medical marijuana laws. https://medicalmarijuana.procon.org/legal-medical-marijuana-states-and-dc/. Accessed May 14, 2022.
10. Brittannica ProCon.org. State-by-state recreational marijuana laws. https://marijuana.procon.org/legal-recreational-marijuana-states-and-dc/ Accessed May 14, 2022.
11. Lin A, O'Connor M, Behnam R, et al. Edible marijuana products and potential risks for pediatric populations. Curr Opin Pediatr. 2022;34(3):279-287. Accessed May 11, 2022.
12. Ammerman S, Ryan S, Adelman WP. Committee on Substance Abuse, the Committee on Adolescence. The impact of marijuana policies on youth: clinical, research, and legal update. Pediatrics. 2015 Mar;135(3):e769-e785. Accessed May 15, 2022.
13. Borodovsky JT, Crosier BS, Lee DC, et al. Smoking, vaping, eating: is legalization impacting the way people use cannabis? Int J Drug Policy. 2016; Oct(36):141-147. Accessed 5/12/22.
14. Borodovsky JT, Lee DC, Crosier BS, et al. U.S. cannabis legalization and use of vaping and edible products among youth. Drug Alcohol Depend. 2017 Aug 1;177:299-306. Accessed May 11, 2022.
15. Roberts BA. Legalized cannabis in Colorado emergency departments: a cautionary review of negative health and safety effects. West J Emerg Med. 2019;20(4):557-572. Accessed May 11, 2022.
16. Wang GS. Pediatric concerns due to expanded cannabis use: unintended consequences of legalization. J Med Toxicol. 2017;13(1):99-105. Accessed May 12, 2022.
17. Matheson J, Le Foll B. Cannabis legalization and acute harm from high potency cannabis products: a narrative review and recommendations for public health. Front Psychiatry. 2020;23(11):591979. Accessed May 17, 2022.
18. Noble MJ, Hedberg K, Hendrickson RG. Acute cannabis toxicity. Clin Toxicol (Phila). 2019 Aug;57(8):735-742. Accessed May 9, 2022.
19. Statista. Sales of adult-use cannabis edibles in the United States from 2019-2025. www.statista.com/statistics/1244945/cannabis-edibles-sales-us/. Accessed May 15, 2022.
20. Barrus DG, Capogrossi KL, Cates SC, et al. Tasty THC: promises and challenges of cannabis edibles. Methods Rep RTI Press. 2016 Nov;2016:10.3768. Accessed May 15, 2022.
21. Peters EN, Bae D, Barrington-Trimis JL, et al. Prevalence and sociodemographic correlates of adolescent use and polyuse of combustible, vaporized, and edible cannabis products. JAMA Netw Open. 2018;1(5):e182765. Accessed May 11, 2022.
22. Friese B, Slater MD, Battle RS. Use of marijuana edibles by adolescents in California. J Prim Prev. 2017;38(3):279-294. Accessed May 7, 2022.
23. Amissah RQ, Vogt NA, Chen C, et al. Prevalence and characteristics of cannabis-induced toxicoses in pets: Results from a survey of veterinarians in North America. PLoS One. 2022;17(4):e0261909. Accessed May 7, 2022.
24. Grewal JK, Loh LC. Health considerations of the legalization of cannabis edibles. CMAJ. 2020;192(1):E1-E2. Accessed May 7, 2022.
25. Lamy FR, Daniulaityte R, Sheth A, et al. “Those edibles hit hard”: Exploration of Twitter data on cannabis edibles in the U.S. Drug Alcohol Depend. 2016;164:64-70. Accessed May 15, 2022.
26. Friese B, Slater MD, Annechino R, et al. Teen use of marijuana edibles: a focus group study of an emerging issue. J Prim Prev. 2016;37(3):303-309. Accessed May 15, 2022.
27. Wong KU, Baum CR. Acute cannabis toxicity. Pediatr Emerg Care. 2019;35(11):799-804. Accessed May 9, 2022.
28. Richards JR, Smith NE, Moulin AK. Unintentional cannabis ingestion in children: a systematic review. J Pediatr. 2017;190:142-152. Accessed May 9, 2022.
29. Wang GS, Le Lait MC, Deakyne SJ, et al. Unintentional pediatric exposures to marijuana in Colorado, 2009-2015. JAMA Pediatr. 2016;170(9):e160971. Accessed May 11, 2022.
30. Levene RJ, Pollak-Christian E, Wolfram S. A 21st Century problem: cannabis toxicity in a 13-month-old child. J Emerg Med. 2019;56(1):94-96. Accessed May 11, 2022.
31. Spindle TR, Cone EJ, Herrmann ES, et al. Pharmacokinetics of cannabis brownies: a controlled examination of Δ9-tetrahydrocannabinol and metabolites in blood and oral fluid of healthy adult males and females. J Anal Toxicol. 2020;44(7):661-671. Accessed May 11, 2022.
32. Giombi KC, Kosa KM, Rains C, et al. Consumers’ perceptions of edible marijuana products for recreational use: likes, dislikes, and reasons for use. Subst Use Misuse. 2018;53(4):541-547. Accessed May 15, 2022.
33. Poyatos L, Pérez-Acevedo AP, Papaseit E, et al. Oral administration of cannabis and Δ-9-tetrahydrocannabinol (THC) preparations: a systematic review. Medicina (Kaunas). 2020;56(6):309. Accessed May 17, 2022.
34. Guidet C, Gregoire M, Le Dreau A, et al. Cannabis intoxication after accidental ingestion in infants: urine and plasma concentrations of Δ-9-tetrahydrocannabinol (THC), THC-COOH and 11-OH-THC in 10 patients. Clin Toxicol (Phila). 2020;58(5):421-423. Accessed May 15, 2022.
35. Qian Y, Gurley BJ, Markowitz JS. The potential for pharmacokinetic interactions between cannabis products and conventional medications. J Clin Psychopharmacol. 2019;39(5):462-471. Accessed May 17, 2022.
36. Page RL 2nd, Allen LA, Kloner RA, et al. American Heart Association Clinical Pharmacology Committee and Heart Failure and Transplantation Committee of the Council on Clinical Cardiology; Council on Basic Cardiovascular Sciences; Council on Cardiovascular and Stroke Nursing; Council on Epidemiology and Prevention; Council on Lifestyle and Cardiometabolic Health; and Council on Quality of Care and Outcomes Research. Medical Marijuana, Recreational Cannabis, and Cardiovascular Health: A Scientific Statement From the American Heart Association. Circulation. 2020;142(10):e131-e152. Accessed May 17, 2022.
37. FDA. FDA warns consumers about the accidental ingestion by children of food products containing THC. www.fda.gov/food/alerts-advisories-safety-information/fda-warns-consumers-about-accidental-ingestion-children-food-products-containing-thc. May 13, 2022. Accessed May 14, 2022.
38. Tan ASL, Weinreich E, Padon A, et al. Presence of content appealing to youth on cannabis-infused edibles packaging. Substance Use Misuse. 2022;57(8):1215-1219. www.tandfonline.com/doi/abs/10.1080/10826084.2022.2069268 Accessed 5/14/22.
39. Ompad DC, Snyder KM, Sandh S, et al. Copycat and lookalike edible cannabis product packaging in the United States. Drug Alcohol Depend. 2022;235:109409. Assessed May 15, 2022.
40. Cavazos-Rehg PA, Zewdie K, Krauss MJ, et al. “No high like a brownie high”: a content analysis of edible marijuana treats. Am J Health Promot. 2018 May;32(4):880-886. Accessed May 15, 2022.
41. Meacham MC, Paul MJ, Ramo DE. Understanding emerging forms of cannabis use through an online cannabis community: an analysis of relative post volume and subjective highness ratings. Drug Alcohol Depend. 2018;1(188):364-369. Accessed May 12, 2022.
42. Laestadius LI, Guidry JPD, Greskoviak R, et al. Making “weedish fish”: an exploratory analysis of cannabis recipes on Pinterest. Subst Use Misuse. 2019;54(13):2191-2197. Accessed May 9, 2022.
43. Grigsby TM, Hoffmann LM, Moss MJ. Marijuana use and potential implications of marijuana legalization. Pediatr Rev. 2020;41(2):61-72. Accessed May 15, 2022.
44. Reboussin BA, Wagoner KG, Sutfin EL, et al. Trends in marijuana edible consumption and perceptions of harm in a cohort of young adults. Drug Alcohol Depend. 2019;205:107660. Accessed May 17, 2022.
45. Zipursky JS, Bogler OD, Stall NM. Edible cannabis. CMAJ. 2020;192(7):E162. www.cmaj.ca/content/cmaj/192/7/E162.full.pdf. Accessed May 14, 2022.
46. Kam AJ. Grandma's brownies are not what they used to be: acute intoxication from cannabis ingestion. Paediatr Child Health. 2020;25(Suppl 1):S3-S4. Accessed May 14, 2022.
47. Potera C. Kids and marijuana edibles: a worrisome trend emerges. Am J Nurs. 2015;115(9):15. Accessed May 9, 2022.
48. Hamid MA, Shaikh R, Gunaseelan L, et al. Recreational cannabis legalization in Canada: a pediatrics perspective. Subst Use Misuse. 2022;57(3):481-483. Accessed May 17, 2022.
49. Wang GS, Hall K, Vigil D, et al. Marijuana and acute health care contacts in Colorado. Prev Med. 2017;104:24-30. Accessed May 13, 2022.
50. Hudak M, Severn D, Nordstrom K. Edible Cannabis-Induced Psychosis: Intoxication and Beyond. Am J Psychiatry. 2015;172(9):911-912. Accessed May 13, 2022.}
51. Bui QM, Simpson S, Nordstrom K. Psychiatric and medical management of marijuana intoxication in the emergency department. West J Emerg Med. 2015;16(3):414-417. Accessed 5/14/2022.
52. Monte AA, Shelton SK, Mills E, et al. Acute illness associated with cannabis use, by route of exposure: an observational study. Ann Intern Med. 2019;170(8):531-537. Accessed May 15, 2022.
53. Ladha KS, Mistry N, Wijeysundera DN, et al. Recent cannabis use and myocardial infarction in young adults: a cross-sectional study. CMAJ. 2021;193(35):E1377-E1384. Accessed May 15, 2022.
54. Burns MM, Toce MS. Pediatric cannabis use and cardiac complications. CMAJ. 2021;193(45):E1737. Accessed May 11, 2022.
55. O'Keefe EL, Peterson TM, Lavie CJ. Reevaluating America's latest pharmaceutical trend: the cardiovascular risk of cannabis. Curr Opin Psychol. 2021;38:31-37. Accessed May 12, 2022.
56. Hopfer C. Implications of marijuana legalization for adolescent substance use. Subst Abus. 2014;35(4):331-5. Accessed May 11, 2022.
57. Skolnick P, Crystal R. Cannabinoid1 (CB-1) receptor antagonists: a molecular approach to treating acute cannabinoid overdose. J Neural Transm (Vienna). 2020 Feb;127(2):279-286. Accessed May 9, 2022.
58. Akpunonu P, Baum RA, Reckers A, et al. Sedation and acute encephalopathy in a pediatric patient following ingestion of delta-8-tetrahydrocannabinol gummies. Am J Case Rep. 2021;22:e933488. Accessed May 11, 2022.
59. Babalonis S, Raup-Konsavage WM, Akpunonu PD, et al. Δ8-THC: legal status, widespread availability, and safety concerns. Cannabis Cannabinoid Res. 2021 Oct;6(5):362-365. Accessed May 11, 2022.
60. Government of Canada. Cannabis legalization and recreation. www.justice.gc.ca/eng/cj-jp/cannabis/. Accessed May 12, 2022.
61. Weedmaps. Is marijuana legal in Canada? https://weedmaps.com/learn/laws-and-regulations/canada#:~:text=Canada%20first%20legalized%20cannabis%20for,of%20Justin%20Trudeau's%20campaign%20platform. Accessed May 15, 2022.
62. Cheng P, Zagaran A, Rajabali F, et al. Setting the baseline: a description of cannabis poisonings at a Canadian pediatric hospital prior to the legalization of recreational cannabis. Health Promot Chronic Dis Prev Can. 2020;40(5-6):193-200. Accessed May 14, 2022.
63. Vogel L. Cannabis edibles already harming kids, new data show. CMAJ. 2019;191(28):E801. Accessed May 9, 2022,
64. Champagne AS, McFaull SR, Thompson W, et al. Surveillance from the high ground: sentinel surveillance of injuries and poisonings associated with cannabis. Health Promot Chronic Dis Prev Can. 2020;40(5-6):184-192. Accessed May 7, 2022.
65. Cohen N, Galvis Blanco L, Davis A, et al. Pediatric cannabis intoxication trends in the pre and post-legalization era. Clin Toxicol (Phila). 2022;60(1):53-58. Accessed May 14, 2022.
66. Myran DT, Cantor N, Finkelstein Y, et al. Unintentional pediatric cannabis exposures after legalization of recreational cannabis in Canada. JAMA Netw Open. 2022 Jan 4;5(1):e2142521. Accessed May 15, 2022.
67. Bechard M, Cloutier P, Lima I, et al. Cannabis-related emergency department visits by youths and their outcomes in Ontario: a trend analysis. CMAJ Open. 2022;10(1):E100-E108. Accessed May 9, 2022.
68. Zhu H, Wu LT. Trends and correlates of cannabis-involved emergency department visits: 2004 to 2011. J Addict Med. 2016;10(6):429-436. Accessed May 11, 2022.
|69. Wang GS, Roosevelt G, Le Lait MC, et al. Association of unintentional pediatric exposures with decriminalization of marijuana in the United States. Ann Emerg Med. 2014;63(6):684-689. Accessed May 19, 2022.
70. Cao D, Srisuma S, Bronstein AC, et al. Characterization of edible marijuana product exposures reported to United States poison centers. Clin Toxicol (Phila). 2016;54(9):840-846. Accessed May 14, 2022.
71. Salas-Wright CP, Carbone JT, Holzer KJ, et al. Prevalence and correlates of cannabis poisoning diagnosis in a national emergency department sample. Drug Alcohol Depend. 2019;204:107564. Accessed May 4, 2022.
72. Patrick ME, Mice RA, Kloska DD, et al. Trends in marijuana vaping and edible consumption from 2015 to 2018 among adolescents in the U.S. JAMA Pediatr. 2020;174(9):900-902. Accessed May 15, 2022.
73. Dilley JA, Graves JM, Brooks-Russell A, et al. Trends and characteristics of manufactured cannabis product and cannabis plant product exposures reported to US poison control centers, 2017-2019. JAMA Netw Open. 2021;4(5):e2110925. Assessed May 15, 2022.
74. Laudone TW, Leonard JB, Hines EQ, et al. Changes in unintentional cannabis exposures in children 6 months to 5 years reported to United States poison centers during the first nine months of the coronavirus-19 pandemic. Clin Toxicol (Phila). 2022;26:1-3. Accessed May 11, 2022.
75. Whitehill JM, Dilley JA, Brooks-Russell A, et al. Edible cannabis exposures among children: 2017-2019. Pediatrics. 2021 Apr;147(4):e2020019893. Accessed May 15, 2022.
76. Leonard JB, Laudone T, Hines EQ, et al. Critical care interventions in children aged 6 months to 12 years admitted to the pediatric intensive care unit after unintentional cannabis exposures. Clin Toxicol (Phila). 2022;6:1-6. Accessed May 11, 2022.
77. Roehler DR, Hoots BE, Holland KM, et al. Trends and characteristics of cannabis-associated emergency department visits in the United States, 2006-2018. Drug Alcohol Depend. 2022;232:109288. Accessed May 14, 2022.
78. Wang GS, Davies SD, Halmo LS, et al. Impact of marijuana legalization in Colorado on adolescent emergency and urgent care visits. J Adolesc Health. 2018;63(2):239-241. Accessed May 15, 2022.
79. Hancock-Allen JB, Barker L, VanDyke M, et al. Notes from the field: death following ingestion of an edible marijuana product—Colorado, March 2014. MMWR Morb Mortal Wkly Rep. 2015;64(28):771-772. Accessed May 14, 2022.
80. Wang GS, Hoyte C, Roosevelt G, et al. The continued impact of marijuana legalization on unintentional pediatric exposures in Colorado. Clin Pediatr (Phila). 2019;58(1):114-116. Accessed May 17, 2022.
81. Wang GS, Banerji S, Contreras AE, et al. Marijuana exposures in Colorado, reported to regional poison centre, 2000-2018. Inj Prev. 2020 Apr;26(2):184-186. Accessed May 11, 2022.
82. Heizer JW, Borgelt LM, Bashqoy F, et al. Marijuana misadventures in children: exploration of a dose-response relationship and summary of clinical effects and outcomes. Pediatr Emerg Care. 2018;34(7):457-462. Accessed May 14, 2022.
83. Heard K, Marlin MB, Nappe T, et al. Common marijuana-related cases encountered in the emergency department. Am J Health Syst Pharm. 2017 Nov;74(22):1904-1908. Accessed May 17, 2022.
84. Marx GE, Chen Y, Askenazi M, et al. Syndromic surveillance of emergency department visits for acute adverse effects of marijuana, Tri-County Health Department, Colorado, 2016-2017. Public Health Rep. 2019;134(2):132-140. Accessed May 15, 2022.
85. Vo KT, Horng H, Li K, et al. Cannabis intoxication case series: the dangers of edibles containing tetrahydrocannabinol. Ann Emerg Med. 2018;71(3):306-313. Accessed May 17, 2022.
86. Kedzierski N, Hernandez M. Blackout brownie: a final dessert case study. J Anal Toxicol. 2022;46(4):e105-e109. Accessed May 11, 2022.
87. Harvey T, Gomez R, Wolk B, et al. Varied presentations of pediatric patients with positive cannabinoid tests. Cureus. 2022;14(3):e23493. Accessed May 14, 2022.
88. Roth W, Tam M, Bi C, et al. Changes in California cannabis exposures following recreational legalization and the COVID-19 pandemic. Clin Toxicol (Phila). 2022 May;60(5):632-638. Accessed May 15, 2022.
89. Whitehill JM, Harrington C, Lang CJ, et al. Incidence of pediatric cannabis exposure among children and teenagers aged 0 to 19 years before and after medical marijuana legalization in Massachusetts. JAMA Netw Open. 2019;2(8):e199456. Accessed May 9, 2022.
90. Kaczor EE, Mathews B, LaBarge K, et al. Cannabis product ingestions in pediatric patients: ranges of exposure, effects, and outcomes. J Med Toxicol. 2021;17(4):386-396. Accessed May 11, 2022.
91. Lewis B, Fleeger T, Judge B, et al. Acute toxicity associated with cannabis edibles following decriminalization of marijuana in Michigan. Am J Emerg Med. 2021;46:732-735. Accepted May 15, 2022.
92. Dean D, Passalacqua KD, Oh SM, et al. Pediatric cannabis single-substance exposures reported to the Michigan Poison Center from 2008-2019 after medical marijuana legalization. J Emerg Med. 2021;60(6):701-708. Accessed May 15, 2022.
93. Thomas AA, Von Derau K, Bradford MC, et al. Unintentional pediatric marijuana exposures prior to and after legalization and commercial availability of recreational marijuana in Washington State. J Emerg Med. 2019;56(4):398-404. Accessed May 14, 2022.
94. Thomas AA, Dickerson-Young T, Mazor S. Unintentional pediatric marijuana exposures at a tertiary care children’s hospital in Washington State: a retrospective review. Pediatr Emerg Care. 2021;37(10):e594-e598. Accessed May 14, 2022.
95. Department of Heath [Ireland]. Medical cannabis access programme. www.gov.ie/en/publication/90ece9-medical-cannabis-access-programme/. Accessed May 31, 2022.
96. Mattimoe C, Conlon E, Ni Siochain D, et al. Edible cannabis toxicity in young children: an emergent serious public health threat. Irish Med J. 2021;114(8):446. Accessed May 17, 2022.
97. Ventresca M, Elliott C. Cannabis edibles packaging: communicative objects in a growing market. Int J Drug Policy. 2022;103:103645.
98. Government of Canada. Regulations under the Cannabis Act. www.canada.ca/en/health-canada/services/drugs-medication/cannabis/laws-regulations/regulations-support-cannabis-act.html. Accessed May 19, 2022.
99. Goodman S, Hammond D. Does unit-dose packaging influence understanding of serving size information for cannabis edibles? J Stud Alcohol Drugs. 2020;81(2):173-179. Accessed 5/19/22
100. Goodman S, Leos-Toro C, Hammond D. The impact of plain packaging and health warnings on consumer appeal of cannabis products. Drug Alcohol Depend. 2019;205:107633. Accessed May 17, 2022.
101. Hammond D. Communicating THC levels and “dose” to consumers: implications for product labelling and packaging of cannabis products in regulated markets. Int J Drug Policy. 2021;91:102509. Accessed May 17, 2022.
102. Goodman S, Hammond D. THC labeling on cannabis products: an experimental study of approaches for labeling THC servings on cannabis edibles. J Cannabis Res. 2022;4(1):17. Accessed May 14, 2022.
103. Freeman TP, Lorenzetti V. “Standard THC units”: a proposal to standardize dose across all cannabis products and methods of administration. Addiction. 2020;115(7):1207-1216. Accessed May 17, 2022.
104. Tsutaoka B, Araya-Rodríguez G, Durrani T. Edible marijuana labeling and packaging. Clin Pediatr (Phila). 2018;57(2):227-230. Accessed May 17, 2022.
105. Pacula RL, Blanchette JG, Lira MC, et al. Current U.S. state cannabis sales limits allow large doses for use or diversion. Am J Prev Med. 2021;60(5):701-705. Accessed May 17, 2022.
106. Malouff JM, Schutte-Malouff BP. Government-mandated warnings on cannabis legally sold for recreational use. J Cannabis Res. 2020;2(1):22. Accessed May 17, 2022.
107. Amirshahi MM, Moss MJ, Smith SW, et al. ACMT Position Statement: Addressing Pediatric Cannabis Exposure. J Med Toxicol. 2019;15(3):212-214. Accessed May 19, 2022.
108. Gimelli A, Deshpande A, Magana JN, et al. Cannabis in homes with children: a survey on use, storage, and attitudes. West J Emerg Med. 2021;22(5):1146-1149. Accessed May 17, 2022.
109. Ryan SA. A modern conundrum for the pediatrician: the safety of breast milk and the cannabis-using mother. Pediatrics. 2018;142(3):e20181921. Erratum in: Pediatrics. 2019;143(1). Accessed May 19, 2022.
110. CDC. Marijuana and breastfeeding. www.cdc.gov/breastfeeding/breastfeeding-special-circumstances/vaccinations-medications-drugs/marijuana.html. Accessed May 19, 2022.
111. Young-Wolff KC, Sarovar V, Tucker LY, et al. Self-reported daily, weekly, and monthly cannabis use among women before and during pregnancy. JAMA Netw Open. 2019;2(7):e196471. Accessed May 15, 2022.
112. Bertrand KA, Hanan NJ, Honerkamp-Smith G, et al. Marijuana use by breastfeeding mothers and cannabinoid concentrations in breast milk. Pediatrics. 2018;142(3):e20181076. Accessed May 19, 2022.
113. Auger N, Chadi N, Low N, et al. Maternal substance use disorders and accidental drug poisonings in children. Am J Prev Med. 2022;62(3):360-366. Accessed May 14, 2022.
114. Eiden RD, Zhao J, Casey M, et al. Pre- and postnatal tobacco and cannabis exposure and child behavior problems: bidirectional associations, joint effects, and sex differences. Drug Alcohol Depend. 2018;185:82-92. Accessed May 17, 2022.
115. Sokol NA, Okechukwu CA, Chen JT, et al. Maternal cannabis use during a child's lifetime associated with earlier initiation. Am J Prev Med. 2018;55(5):592-602. Accessed May 19, 2022.
116. Cho BY. Associations of Father's Lifetime Cannabis Use Disorder with Child’s Initiation of Cannabis Use, Alcohol Use, and Sexual Intercourse by Child Gender. Subst Use Misuse. 2018;53(14):2330-2338. Accessed May 19, 2022.
117. Child Welfare Information Gateway. Mandatory reporters of child abuse and neglect. www.childwelfare.gov/pubPDFs/manda.pdf. Accessed May 19, 2022.
118. Child Welfare Information Gateway. Penalties for failure to report and false reporting of child abuse and neglect. www.childwelfare.gov/pubPDFs/report.pdf. Accessed May 21, 2022.