US Pharm.
2008;33(12):24-29.
A
n estimated one of every 100 to 200 people in the United States has celiac disease (also known as gluten-sensitive enteropathy, nontropical sprue, or celiac sprue), an autoimmune inflammatory enteropathy that is triggered by the ingestion of gluten-containing grains in susceptible individuals.1-9 Gluten is the main storage protein of wheat. The alcohol-soluble fraction (prolamin) of gluten is damaging in celiac disease, as are similar proteins in barley (hordein) and rye (secalin).1,6,9,10
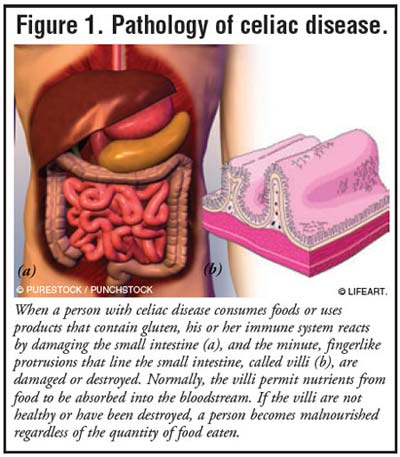
The major site of damage in celiac disease is the proximal small intestine (FIGURE 1).1,5,6,11 This damage can cause a wide variety of consequences, including maldigestion and malabsorption of nutrients, vitamins, and minerals in the digestive tract.1,9 Over time, numerous organ systems--including the skin, liver, nervous system, bones, reproductive system, and endocrine system--can be negatively affected by celiac disease.1-3,6 Treatment of celiac disease consists of the removal of gluten proteins from the diet, which improves and often eliminates the small-intestine pathology.1,3,5
Celiac disease was first described by Samuel Gee in 1888, although a similar description of a chronic malabsorptive disorder by Aretaeus of Cappadocia (now Turkey) dates back to the second century ad.8,9,12,13 Gee described the classic features of celiac disease as diarrhea, lassitude, and failure to thrive; he believed that the regulation of food was the main part of the treatment and noted that the disease was not age-specific.9 Since this time, much has been learned about the diagnosis and treatment of celiac disease.5,8,13 This article examines the pathogenesis, epidemiology, clinical presentation, diagnosis, and treatment of celiac disease and discusses how pharmacists can provide pharmaceutical care to patients with this disorder.
Pathogenesis
Two primary factors are thought to contribute to the development of celiac disease: consumption of gluten proteins and genetic predisposition.3,4,12 It is not completely understood how gluten sensitivity begins or whether early exposure to gluten proteins increases the risk of sensitivity.3 Most experts agree that celiac disease results from an "unchecked" immune reaction to gluten and that this reaction results in inflammation of the proximal small intestine, where the partially digested gluten proteins make contact with the gut's immune system.6,7 This immune response extends beyond just a direct reaction to the exogenous substance, also involving a potent, multifaceted immune response to the exogenous substance that results in substantial damage to the structure and function of the gut and other organs.7
Genetics also appears to play a role in the development of celiac disease. Almost all patients with celiac disease exhibit human leukocyte antigen (HLA)-DQ2 or HLA-DQ8, which facilitate the immune response against gluten proteins; some 40% of the general population also carries these HLA haplotypes, however.3 The presence of these haplotypes is necessary for the development of celiac disease, and their absence virtually excludes the diagnosis. HLA-DQ2 is expressed in more than 90% of patients with celiac disease, and HLA-DQ8 is found in most of the remainder.9
Environmental factors may also affect the risk or the timing of developing celiac disease. The risk of celiac disease appears to increase when large amounts of gluten are incorporated into the diet during the first year of life.10 In contrast, breast-feeding imparts a consistent protective effect; the risk of celiac disease decreases when a child is still being breast-fed at the time dietary gluten is introduced.10 Interestingly, a recent study found that, in children prone to developing celiac disease as result of HLA-DR3 or -DR4 alleles, initial exposure to wheat, barley, and rye in the first three months or from the seventh month onward significantly increased the risk of developing celiac disease–associated autoantibodies compared with exposure at four to six months.10,14
Epidemiology
Celiac disease previously was thought to be extremely rare in the U.S.2,5,6,9 Two epidemiologic studies published prior to 2000 estimated that between one and 4,800 and one in 10,000 people in the U.S. were affected by celiac disease.2,6,15,16 Population studies published in recent years, however, suggest a much higher prevalence, particularly in individuals of European ancestry.2,4,6 One of the largest studies in the U.S. involved 13,145 participants (4,508 first-degree relatives of patients with celiac disease, 1,275 second-degree relatives, 3,236 symptomatic patients, and 4,126 not-at-risk subjects) who underwent screening.2,6,9,12,17 The prevalence of celiac disease was 1:22 in first-degree relatives, 1:39 in second-degree relatives, 1:56 in symptomatic patients, and 1:133 in not-at-risk subjects.2,6,9,12,17
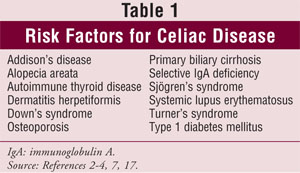
The likelihood of having celiac disease increases to 10% to 20% in persons who have a first-degree relative with the disease, and up to 75% in monozygotic twins.2,3 In addition, patients who have type 1 diabetes mellitus, Down's syndrome, Turner's syndrome, or other disorders are at increased risk for developing celiac disease (TABLE 1).2-4,7,17
Celiac disease also occurs in people not of European descent, although the prevalence is not as great. People from the Punjab and Gujarat regions of India who lived in England developed celiac disease 2.7 times as often as Europeans on a gluten-rich diet; in addition, a disorder termed summer diarrhea has long plagued people of the tropics, especially during the summer months, when wheat commonly replaces maize in the diet.4,12 Furthermore, a very high prevalence rate of 5% has been documented in the Saharawi population of northern Africa.4
Clinical Presentation
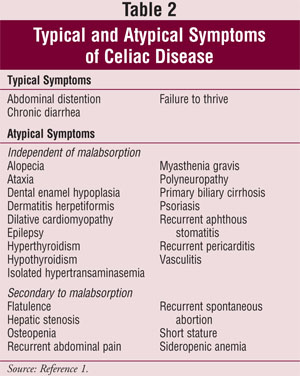
The clinical manifestations of celiac disease vary markedly by the age of the patient, the duration and extent of disease, and the presence of extraintestinal pathology (TABLE 2).1 Depending on the features at the time of presentation and taking into account the histologic and immunologic abnormalities at the time of diagnosis, celiac disease can be divided into the following three clinical forms: classic (typical), atypical, and silent (asymptomatic).1
Classic Celiac Disease:
This form typically presents in infancy (age 6 to 18 months) and manifests as failure to thrive, diarrhea, abdominal distention, muscle-wasting, developmental delay, and (occasionally) severe malnutrition.1,2 Symptoms typically begin weeks to months after the introduction of weaning foods containing prolamines, and soon there is a progressive decrease in weight gain, with a decline in the child's percentile for weight and weight for height.1 In many instances, failure to diagnose the disorder can lead to a true medical emergency.1,2 Beyond infancy, the symptoms of classic celiac disease tend to be less dramatic.2 Older children may present with constitutional short stature or dental enamel defects.2
Women constitute approximately 75% of newly diagnosed adult cases of classic celiac disease, and they typically have more clinically conspicuous disease.2 In adults of both sexes, gastrointestinal (GI)-tract involvement may manifest as diarrhea, constipation, or other symptoms of malabsorption, such as bloating, flatus, or belching.2 These symptoms may be accompanied by consequences of malabsorption, such as weight loss, severe anemia, neurologic disorders from deficiencies of B vitamins, and osteopenia (low bone mass) from vitamin D and calcium deficiency.4
Atypical Celiac Disease:
This type is characterized by few or no GI symptoms, and extraintestinal manifestations predominate.5 Recognition of the atypical features of celiac disease is responsible for much of the increased prevalence, and atypical disease now may be the most common presentation.5 The clinical features of atypical celiac disease (e.g., iron deficiency, osteoporosis, short stature, infertility) typically are milder than those associated with the classic form of the disease.18
Silent Celiac Disease:
This form is found during testing of asymptomatic patients (e.g., because of a family history of celiac disease or during an upper endoscopy performed for another reason).18 It is important to note that asymptomatic patients are still at risk for complications of celiac disease.2
Diagnosis
No single test has been universally accepted as the standard for diagnosing celiac disease. However, serologic testing and small-bowel biopsy are highly sensitive and specific for making the diagnosis, especially in patients with symptoms suggestive of celiac disease and in those at increased risk (e.g., having a family history or an associated autoimmune disorder).3 Diagnostic testing must be performed while the patient is on a diet that includes gluten-containing foods.3
As a general rule, testing for celiac disease should begin with serologic evaluation.18 Immunoglobulin A (IgA) antitissue transglutaminase and IgA endomysial antibody, which have equivalent diagnostic accuracy, are generally considered to be 85% to 100% sensitive and 96% to 100% specific for celiac disease.2,18 Antigliadin antibody tests are no longer used routinely because of their lower sensitivity and specificity.18 Importantly, serologic testing may not be as accurate in children under 5 years of age.18
Patients who have a positive IgA endomysial or transglutaminase antibody test should undergo small-bowel biopsy; patients with biopsy-proven dermatitis herpetiformis in whom the diagnosis can be established without small-bowel biopsy are exceptions, however.3,18 Biopsy also should be considered in patients with negative serologic test results who are at high risk or in whom the clinician strongly suspects celiac disease.3
A diagnosis of celiac disease is presumptively established when there is concordance between the serologic results and the biopsy findings. The diagnosis is confirmed when symptoms resolve subsequently on a gluten-free diet. A demonstration of histologic normalization is not required, however.18
Early diagnosis of celiac disease is extremely important because it can minimize, if not prevent, serious complications. A patient's risk of developing other autoimmune diseases and intestinal lymphomas is proportional to the time of exposure to gluten.1 For this reason, the National Institutes of Health's 2004 consensus statement on celiac disease recommends testing for the disorder in patients at high risk for developing it; patients experiencing GI symptoms (if not otherwise explained) such as chronic diarrhea, malabsorption, weight loss, and abdominal distention; and patients lacking another explanation for signs and symptoms (e.g., persistent elevation of serum aminotransferases, short stature, delayed puberty, iron-deficiency anemia, recurrent fetal loss, and infertility).5,18
Treatment
The cornerstone of treatment for celiac disease is strict lifelong adherence to a gluten-free diet.1,2,5,9 All foods and medications containing gluten (found in wheat, barley, rye, and their derivatives; TABLE 3) should be eliminated from the diet.9 One of the major controversies in the treatment of celiac disease relates to the amount of gluten allowed. The National Food Authority has redefined the term "gluten-free"; previously, less than 0.02% gluten in a product was considered gluten-free, but gluten-free now means no gluten at all, and less than 0.02% gluten is labeled "low-gluten."1

Complete exclusion of dietary gluten generally results in symptomatic, serologic, and histologic remission in the majority of patients.2,9 Growth and development in children typically return to normal with adherence to the gluten-free diet, and many disease complications can be avoided in adults.9 Patients' overall nutritional status should be evaluated so that nutritional and caloric deficiencies can be adequately supplemented.8
Understanding the Gluten-Free Diet:
Gluten is the primary protein in wheat; therefore, wheat and products containing wheat must be avoided--as must barley and rye, which contain similar proteins.2 Oats are a subject of controversy; although oats themselves may not be harmful in limited quantities, commercial oat products are measurably contaminated with wheat.2 Generally speaking, soybean and tapioca flours, rice, corn, maize, buckwheat, potatoes, and other grain substitutes (such as nuts and beans) are gluten-free.2,8 Many commercial gluten-free products, including breads, cookies, chips, and cereals, can be found on store shelves. In addition, meats, vegetables, fruits, and most dairy products are free of gluten as long as they were not contaminated during production.2 Various resources are available for patients with celiac disease, including cookbooks, gluten-free prepared foods, Internet sites, and organizations. See TABLE 4 for some resources.

Correcting Nutritional Deficiencies:
In patients presenting with the classic malabsorption of celiac disease, deficiency in fat-soluble vitamins (vitamins A, D, E, and K) is commonly encountered, and supplementation is required.6 Iron-deficiency anemia is a common manifestation of celiac disease and should be treated with supplemental iron. Osteoporosis should be treated with calcium and vitamin D replacement. Other nutritional deficiencies in celiac disease that frequently require correction involve magnesium, zinc, selenium, copper, and folate.2,6
Since a gluten-free diet can be low in fiber, it may induce constipation. Constipation usually responds to the addition of dietary rice bran or ispaghula husks; psyllium fiber and methylcellulose supplements also are generally gluten-free.8
The Pharmacist's Role
It is not surprising that many pharmacists are unsure about how to support patients with celiac disease, since the cornerstone of treatment does not involve pharmaceutical agents.19 Despite this, pharmacists can play a pivotal role in helping patients with this disorder improve their quality of life.
Pharmacists should encourage patients with celiac disease to seek the advice and guidance of licensed dieticians and explain that many dieticians specifically handle the needs of celiac patients and can instruct them about which foods to avoid, especially foods not inherently known to contain gluten (e.g., sauces, salad dressings, licorice). Trained dieticians also can teach patients key words to look for on food labels (e.g., barley malt extract).8,13
Women make up a majority of newly diagnosed adult cases, so bone loss is of particular concern.6 Pharmacists should ensure that female patients, especially postmenopausal women, consume at least 1,500 mg of elemental calcium per day while being treated with a bisphosphonate agent.6 Bisphosphonates may not be needed if the underlying celiac disease is corrected.
Pharmacists should remind patients with celiac disease of the importance of certain vaccinations. Because celiac disease is associated with hyposplenism, prophylactic administration of the pneumococcal vaccine is reasonable.13 Pharmacists should also encourage patients with celiac disease to receive the influenza vaccine annually.20
Pharmacists should be aware than many medications and vitamin and mineral supplements may contain gluten as inactive ingredients. Information about inactive ingredients is found in the package insert.1 Nebulous inactive ingredients that require further investigation include gums and starches.1,19 Vegetable gums commonly contain gluten.19 If the product lists the starch as "cornstarch" or "starch (corn)," it can be assumed to be gluten-free.19 Pregelatinized starch and sodium starch glycolate, which are derived from corn, wheat, potatoes, or rice, have been chemically treated and may or may not contain gluten.19 A call to the manufacturer is the only way to confirm the source of the starch. Likewise, if simply "starch" is listed, the only way to verify the source of the starch and the gluten status is to contact the manufacturer. Importantly, inactive ingredients may differ between brand and generic products; for this reason, it cannot be assumed that a generic product is gluten-free just because a brand product is gluten-free, or vice versa. Additionally, when a product is reformulated, its gluten status may change. If a product is "new and improved," is a new formulation, has a new appearance, or is being made by a new manufacturer, this is a signal that the gluten status of the product may have been altered.19
Clearly, pharmacists are advocates who can take an active role in improving the lives of patients with celiac disease. The education that pharmacists can provide for these patients has the potential to have wide-reaching effects in raising awareness about this common disorder.
Conclusion
Adherence to a gluten-free diet remains the mainstay of therapy for celiac disease. Although a gluten-free diet seems simple theoretically, the diet can be difficult for some patients to adhere to.6 The most common reasons for lack of response are poor compliance and inadvertent gluten ingestion.8 All patients with celiac disease should be reevaluated periodically. The evaluation should include assessment of growth, assessment of GI and other symptoms associated with celiac disease, and the individual patient's understanding of and compliance with the gluten free-diet.8
REFERENCES
1. Fasano A, Catassi C. Current approaches to diagnosis and treatment of celiac disease: an evolving spectrum. Gastroenterology. 2001;120:636-651.
2. Nelsen DA. Gluten-sensitive enteropathy (celiac disease): more common than you think. Am Fam Physician. 2002;66:2259-2266.
3. Presutti RJ, Cangemi JR, Cassidy HD, Hill DA. Celiac disease. Am Fam Physician. 2007;76:1795-1802.
4. Hill ID. Clinical Manifestations and Diagnosis of Celiac Disease in Children. Waltham, MA: UpToDate; 2008.
5. US Department of Health and Human Services. NIH Consensus Statement on Celiac Disease. NIH Consensus and State-of-the-Science Statements. June 28-30, 2004. http://consensus.nih.gov/2004/2004CeliacDisease118PDF.pdf. Accessed October 31, 2008.
6. Barton SH, Kelly DG, Murray JA. Nutritional deficiencies in celiac disease. Gastroenterol Clin North Am. 2007;36:93-108.
7. Barton SH, Murray JA. Celiac disease and autoimmunity in the gut and elsewhere. Gastroenterol Clin North Am. 2008;37:411-428.
8. Hill ID. Management of Celiac Disease in Children. Waltham, MA: UpToDate; 2007.
9. Niewinski MM. Advances in celiac disease and gluten-free diet. J Am Diet Assoc. 2008;108:661-672.
10. Branski D, Fasano A, Troncone R. Latest developments in the pathogenesis and treatment of celiac disease. J Pediatr. 2006;149:295-300.
11. National Digestive Diseases Information Clearinghouse. Celiac disease. NIH Publication No. 08-4269. http://digestive.niddk.nih.gov/ddiseases/pubs/celiac/. Accessed October 31, 2008.
12. Schuppan D, Dieterich W. Pathogenesis, Epidemiology, and Clinical Manifestations of Celiac Disease in Adults. Waltham, MA: UpToDate; 2008.
13. Ciclitira PJ. Management of Celiac Disease in Adults. Waltham, MA: UpToDate; 2008.
14. Norris J, Barriga K, Hoffenberg E, et al. Risk of celiac disease autoimmunity and timing of gluten introduction in the diet of infants at increased risk of disease. JAMA. 2005;293:2343-2351.
15. Rossi T, Albini C, Kumar V. Incidence of celiac disease identified by the presence of serum endomysial antibodies in children with chronic diarrhea, short stature, or insulin-dependent diabetes mellitus. J Pediatr. 1993;123:262-264.
16. Talley NJ, Valdovinos M, Petterson TM, et al. Epidemiology of celiac sprue: a community-based study. Am J Gastroenterol. 1994;89:843-846.
17. Fasano A, Berti I, Gerarduzzi T, et al. Prevalence of celiac disease in at-risk and not-at-risk groups in the United States: a large multicenter study. Arch Intern Med. 2003;163:286-292.
18. Kelly CP. Diagnosis of Celiac Disease. Waltham, MA: UpToDate; 2008.
19. Plogsted S. Medications and celiac disease--tips from a pharmacist. Pract Gastroenterol. 2007;31:58-64.
20. Grabenstein JD. Pharmacy-Based Immunization Delivery: A National Certificate Program for Pharmacists. Washington, DC: American Pharmacists Association; 2008.
To comment on this article, contact
rdavidson@jobson.com.





