US Pharm. 2021;46(5):28-31.
ABSTRACT: The new, unique challenges directly associated with the COVID-19 pandemic are exacerbating an already stressful work environment in community pharmacy. Initially, with the country on lock-down, prescription volume increased overnight as patients went into panic mode. With social distancing, use of pharmacy drive-through lanes expanded dramatically. Pharmacies were later recognized as an ideal access point to provide COVID-19 testing along with COVID-19 vaccination services. These challenges and increased responsibilities in community pharmacy have created ideal conditions to leave burned-out pharmacy personnel in the aftermath. Pharmacy professional organizations have responded with resources to address and prevent burnout.
The increased demand for medical services during the COVID-19 pandemic has placed an unprecedented strain on the healthcare system. After about a year of working in this high-stress environment, the vital resource that is the healthcare work force is foundering. Healthcare workers are reporting burnout at rates that are cause for concern. A study conducted early in the pandemic (June to September, 2020) that included 1,119 healthcare workers reported burnout at an alarming rate of 76%.1 Burnout is defined by the World Health Organization as chronic workplace stress that has not been successfully managed. It is characterized by three dimensions, including feelings of energy depletion or exhaustion, increased mental distance from one’s job or feelings of negativism or cynicism related to the job, and reduced professional efficacy.2
In a study of physicians, burnout included emotional exhaustion, including feeling “used up” at the end of a workday and having nothing left to offer patients from an emotional standpoint. Burnout included depersonalization, including feelings of treating patients as objects rather than human beings and becoming more callous towards patients. Burnout also related to a reduced sense of personal accomplishment, encompassing feelings of ineffectiveness in helping patients with their problems and a sense of reduced valuing of the results of work-related activities, such as patient care or professional achievements.3
Burnout can lead to negative consequences for patient care, including lower care quality, increased medical errors, and decreased patient satisfaction.3 Burnout can also impact the healthcare system by reducing provider productivity and increasing provider turnover.3 Finally, burnout can lead to negative impacts on providers’ health, including poor self-care, substance abuse, depression, and suicidal ideation.3
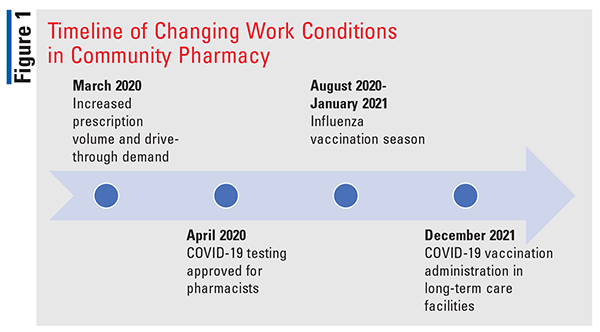
Unfortunately, burnout affects all disciplines of the healthcare work force, and community-pharmacy personnel are no exception. A study conducted in January of 2020, just prior to the start of the pandemic, with the assistance of the American Pharmacists Association (APhA), found pharmacist burnout in 75% of study participants.4 Since the start of the pandemic, prescription volume has fluctuated, drive-through use has increased, COVID-19 testing has been implemented, and vaccination changes have occurred (FIGURE 1). A perfect storm is brewing in community pharmacy owing to the new, unique challenges directly associated with the COVID-19 pandemic that have the potential to leave burned-out pharmacy personnel in the aftermath.
Daily Prescription Volume
Prior to COVID-19, community-pharmacy personnel were working in stressful conditions. An increasing daily prescription volume is associated with increased prevalence of burnout.4 In one study conducted before the pandemic, among pharmacists who filled a daily prescription volume of 200 or less, burnout rates were at 65%; those who filled 201 to 350 prescriptions were at 77%; and those who filled 351 to 500 prescriptions were at 84%.4 In mid-March 2020, COVID-19 stay-at-home orders and state lock-downs started, causing a panic among patients and increasing prescription demand by nearly 15%.5 After an initial jump in demand for prescriptions mitigated by authorization of 90-day fills, stockpiling, and “refill too soon” flexibility, prescription volume stabilized and even decreased as physician visits and surgeries were cancelled.5 However, the initial surge created ideal conditions for burnout.
Drive-Through Window
Pharmacy drive-through services were introduced in the United States in the 1990s by Walgreens community pharmacies.6 Drive-through services offer faster and more convenient dispensing of medication and improved patient satisfaction.6 Though beloved by patients, the presence of a drive-through window is associated with more pharmacist burnout. The rate among community pharmacists is roughly 84% when there is a drive-through compared with 16% when there is not.4 Recently, the CDC has encouraged patients, especially those at increased risk of severe illness, to use the drive-through pharmacy services to pick up medication in order to reduce the risk of COVID-19 infection.7 This recommendation resulted in an uptick in use of drive-through windows. To comply with the CDC recommendations, some pharmacies created a new workflow process to incorporate or expand drive-through services. The advantages of a drive-through window for patients include less virus exposure risk and eliminating crowds while still maintaining access to medication; the disadvantage, however, is the potential risk for increased pharmacy-staff burnout, as the presence of a drive-through window is a clear risk factor.
Implementation of COVID-19 Testing
Pharmacies have always been a critical access point for healthcare information. A pharmacist is ever available to patients and offers free healthcare advice, thereby increasing access to the medical system at a decreased cost. During the COVID-19 pandemic, the federal government has recognized pharmacies as a critical touch point for medical care in the community and has issued a new scope of practice to pharmacists to help their communities during these tough times. On April 8, 2020, the Office of the Assistant Secretary for Health issued guidance under the Public Readiness and Emergency Preparedness Act authorizing licensed pharmacists to order and administer COVID-19 tests.8 Giving pharmacists the authorization to order and administer COVID-19 tests to their patients means easier access to testing for Americans who need it.8 Though this role is critical to stopping the pandemic and allows pharmacists the ability to work to the limits of their license, it increases workload and requires workflow changes, additional training, and increased exposure risk for pharmacy personnel. The additional workload created by the integration of COVID-19 testing into an already stressed work environment creates another risk factor for burnout.
Influenza Vaccinations
For more than 10 years, pharmacists have been vaccinating their local communities. The most common vaccination administered in the community-pharmacy setting is the seasonal influenza vaccine. For the 2020-2021 influenza season, concerns about concurrent circulation of influenza and COVID-19 led to increased emphasis on maximizing influenza vaccination coverage in order to reduce the burden of influenza-related respiratory illnesses on public health and the healthcare system.9 A study was conducted by the CDC to assess early signals regarding influenza vaccination behavior in September of 2020.9 The findings stated that 59% of patients reported an intention to receive the 2020-2021 influenza vaccine. Of the same population, only 52% of patients reported being vaccinated in the previous season.9 Overall, intention to be vaccinated increased by 7%. Among patients who had already received their vaccine, the proportion reporting vaccination at a pharmacy was 53.8%, which was considerably higher than the equivalent proportion for the previous season (34.9%).9 The proportion of patients reporting vaccination at a doctor’s office was 29.7%, which was considerably lower than the previous season (37.3%).9 Overall, influenza vaccination rates are anticipated to be increased for this season. At the time of this study, pharmacies were administering more influenza vaccines than in years past, and conversely, doctor’s offices were administering fewer vaccinations. To reduce the spread of COVID-19, many doctor’s offices have increased telemedicine appointments and decreased face-to-face appointments. Therefore, patient access to influenza vaccinations at the doctor’s office has likely decreased. Access to influenza vaccination services is readily available to patients at their local pharmacy; however, the increased demand for influenza vaccination along with the requirement to maintain all other workflow processes can increase workplace stress and potentially contribute to burnout.
COVID-19 Vaccinations
On December 11, 2020, the FDA issued the first emergency-use authorization (EUA) for a vaccine for the prevention of COVID-19.10 In October, roughly 2 months prior to the EUA and the circulation of any vaccine product in the market, the government partnered with CVS and Walgreens to provide COVID-19 vaccines to patients living in long-term care facilities.11 As of February 16, 2021, there were more than 5.9 million doses of COVID-19 vaccine given to long-term care patients participating in the federal pharmacy partnership program.12
Many of these vaccinations were given by pharmacists traveling to the long-term care facility. Some pharmacists were going to long-term care clinics during their standard workdays, potentially leaving an understaffed store behind. Other pharmacists are going to vaccination clinics on top of their normal work schedule, thereby giving up their personal time.
As the vaccination rollout continues, vaccination administration is moving locally to the pharmacies. However, the demand for vaccination is profuse. Hiring of pharmacists has increased to help support the vaccination effort, but the supply of pharmacists may not meet the demand in all areas of the country, leaving the responsibility of vaccinating on the shoulders of the current staff. Overall, the impact pharmacists and support staff have made on vaccinating Americans during this time of crisis is nothing short of heroic. Without discounting the heroism, this increased vaccination volume has put a tremendous strain on pharmacy personnel. With the timeline of the COVID-19 vaccine administration falling right after the height of the influenza vaccination administration season, pharmacy personnel are exhausted and under more stress than ever, making them more vulnerable to burnout.
Pharmacist Resources for Burnout
To address the unique new environment created by COVID-19, pharmacy professional organizations are providing resources for pharmacy teams specifically to help increase resilience and reduce burnout (TABLE 1). The American Society of Health Systems Pharmacists (ASHP) is an original sponsor of the National Academy of Medicine’s Action Collaborative on Clinical Well-being and Resilience.13 ASHP is representing pharmacy in the interprofessional efforts to address the workforce and patient care issues.13 Their program is entitled “Wellbeing & You” and aims to foster and sustain the well-being, resilience, and professional engagement of pharmacy personnel.13 The website includes various resource modalities, such as a “Share Your Story” feature that allows pharmacists to share tips on what has helped them build resilience, as well as other resources, including webinars that address burnout, to accomplish this mission and aid struggling pharmacy personnel.13
In addition to the program sponsored by ASHP, pharmacy personnel have access to a program sponsored by APhA. One feature of the AphA program is a Well-Being Index, a validated screening tool created by the Mayo Clinic to evaluate fatigue, depression, burnout, anxiety, stress, and mental/physical quality of life.14 Respondents to the anonymous survey will receive immediate individualized feedback including the likelihood of burnout and the likelihood of making a medication error.14 This will allow them to compare themselves with other pharmacists and healthcare professionals and connect with tools that address individual well-being, such as a link to a mindfulness meditation app. Participants will also be able to track their status over time.14 These resources can be invaluable during the pandemic, as workplace stress is not likely to decrease.
Conclusion
Conditions in the community-pharmacy setting have been rapidly changing and expanding since the onset of COVID-19. Increasing prescription rates, use of drive-through services, addition of COVID-19 testing, increased influenza vaccine administration rates, and initiation of COVID-19 vaccination administration programs set the conditions for a potentially unhealthy work environment for pharmacy personnel. The increasing workplace challenges inflicted on community-pharmacy personnel in the wake of COVID-19 places this valuable human resource at increased risk of burnout. Professional pharmacy organizations have acknowledged this risk and have developed resources to improve well-being and resilience during this unprecedented time.
The views expressed herein are those of the author and do not reflect the official policy of the Department of the Army, Department of Defense, or the U.S. Government.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Mental Health America. The mental health of healthcare workers in COVID-19. https://mhanational.org/mental-health-healthcare-workers-covid-19. Accessed February 11, 2021.
2. World Health Organization. Burn-out an “occupational phenomenon”: International Classification of Diseases. www.who.int/news/item/28-05-2019-burn-out-an-occupational-phenomenon-international-classification-of-diseases. Accessed February 11, 2021.
3. West CP, Dyrbye LN, Shanafelt TD. Physician burnout: contributors, consequences and solutions. J Intern Med. 2018;283(6):516-529.
4. Patel SK, Kelm MJ, Bush PW, et al. Prevalence and risk factors of burnout in community pharmacists. J Am Pharm Assoc (2003). 2021;61(2):145-150.
5. PBA Health. Elements. How will COVID-19 change the future of retail pharmacy? Published July 7, 2020. www.pbahealth.com/how-will-covid-19-change-the-future-of-retail-pharmacy/. Accessed February 11, 2021.
6. Farha RA, Hammour AK, Alefishat E, et al. Drive-thru pharmacy service: assessments of awareness, perception and barriers among pharmacists in Jordan. Saudi Pharm J. 2017;25(8):1231-1236.
7. CDC. Guidance for pharmacists and pharmacy technicians in community pharmacies during the COVID-19 response. Published 2020. www.cdc.gov/coronavirus/2019-ncov/hcp/pharmacies.html. Accessed February 17, 2021.
8. U.S. Department of Health and Human Services. HHS statements on authorizing licensed pharmacists to order and administer COVID-19 tests. Published April 8, 2020. www.hhs.gov/about/news/2020/04/08/hhs-statements-on-authorizing-licensed-pharmacists-to-order-and-administer-covid-19-tests.html#:~:text=HHS%20Secretary%20Alex%20Azar%20issued%20the%20following%20statement%3A&text=HHS%20Assistant%20Secretary%20for%20Health,19%20tests%20to%20their%20patients. Accessed February 17, 2021.
9. Lindley MC, Anup A, Hendrich M, et al. Early-season influenza vaccination uptake and intent among adults – United States, September 2020, Seasonal Influenza (Flu). CDC. Published 2020. www.cdc.gov/flu/fluvaxview/nifs-estimates-sept2020.htm. Accessed February 17, 2021.
10. FDA. Pfizer-BioNTech COVID-19 Vaccine. Published 2020. www.fda.gov/emergency-preparedness-and-response/coronavirus-disease-2019-covid-19/pfizer-biontech-covid-19-vaccine. Accessed February 17, 2021.
11. U.S. Department of Health and Human Services. Trump administration partners with CVS and Walgreens to provide COVID-19 vaccine to protect vulnerable Americans in long-term care facilities nationwide. Published October 16, 2020. www.hhs.gov/about/news/2020/10/16/trump-aministration-partners-cvs-walgreens-provide-covid-19-vaccine-protect-vulnerable-americans-long-term-care-facilities-nationwide.html. Accessed February 17, 2021.
12. CDC. COVID data tracker. https://covid.cdc.gov/covid-data-tracker/#vaccinations-ltc. Accessed February 17, 2021.
13. American Society of Health-System Pharmacists. Wellbeing & you. https://wellbeing.ashp.org/. Accessed April 12, 2021.
14. American Pharmacists Association. Well-being during COVID-19. Published 2021. Pharmacist.com. https://pharmacist.com/Practice/COVID-19/Well-being. Accessed April 8, 2021.
To comment on this article, contact rdavidson@uspharmacist.com.







