US Pharm. 2015;40(11):37-42.
ABSTRACT: Depression, anxiety, and schizophrenia are some of the mental health comorbidities seen in the diabetic population. Managing diabetes in the context of these mental health disorders can be extremely challenging. Proper control of diabetes requires active patient participation and is dependent upon compliance with lifestyle modifications, self-monitoring, and prescribed medications. Poorly controlled mental health disorders may likely affect patients’ ability to self-manage diabetes. Identifying and treating mental health disorders is an essential component of diabetes management that can be accomplished in an integrated manner by multidisciplinary team members. Pharmacists working with this patient population can provide a number of services—such as individual assessment, collaborative goal setting, skill building, ongoing monitoring, and medication management—to improve patient outcomes.
Diabetic patients may be particularly vulnerable to developing mental health disorders because diabetes is considered one of the most psychologically and behaviorally demanding chronic medical conditions.1 Diabetes is more prevalent in psychiatrically ill patients than in the general population.2 Depression, anxiety, and schizophrenia are a few of the mental health comorbidities seen in the diabetic population. Comorbid psychiatric illness has been linked to worse health outcomes in diabetic patients.2
Comorbid Mental Health Disorders
Even nonclinical levels of depressive symptoms and minor depression have been associated with problems with adherence, risk of complications, functional impairment, higher medical costs, and death.3-5 Increased severity of depressive symptoms has been connected to a greater probability of emergency department, primary care, specialty care, medical inpatient, and mental health costs.3 Depressive symptoms have been found to be more persistent in diabetic subjects compared with nondiabetic subjects (symptom duration 18 months vs. 8-12 weeks).6-8 Relapse of depression is another challenge in the treatment of diabetic patients. Lustman and colleagues demonstrated that 92% of diabetic patients who were successfully treated for major depression experienced at least one relapse in a 5-year period.9
Fear of diabetes complications can lead to anxiety in diabetic patients.10 Anxiety and depression were linked to more perceived symptoms of diabetes, longer anticipated duration of illness, more serious diabetes complications, worse diabetes control, greater healthcare use and costs, decreased medication adherence, and higher mortality rates.11-13 Symptoms of anxiety and depression and negative beliefs relating to diabetes (perceived symptom load, perceived control over diabetes, anticipated outcomes) have been associated with impaired health-related quality of life.13 The reported incidence of depression and anxiety in patients with diabetes is 41% and 49%, respectively, compared with <10% in the general population.14 Diabetic patients who smoke and those who are ex-drinkers or heavy drinkers have higher anxiety and depression scores.15
Rates of diabetes in patients with schizophrenia are approximately double those reported in the general population.16 The prevalence of diabetes is estimated to be 16% to 25% in persons with schizophrenia.17 The greater risk may be attributed to metabolic disturbances and weight gain associated with atypical antipsychotics.18 The use of atypical antipsychotics in patients with mental health disorders has been linked to a two- to threefold increased risk of diabetes.19 In a study by Koller and Doraiswamy, 80% of patients experienced improvements in glycemic control after discontinuing therapy with olanzapine and clozapine.20 However, higher rates of insulin resistance in schizophrenic patients compared with the general population were noted even before the introduction of antipsychotic drugs in the 1950s.21 Patients with schizophrenia also possess other risk factors for the development of diabetes and cardiovascular disease, such as smoking, poor diet, reduced physical activity, and alcohol or drug abuse.22
Impact of Mental Health Disorders on Diabetes Control
The impact of mental health disorders on diabetes care and outcomes is being increasingly recognized. It is believed that psychiatric illness may be a chronic stressor that leads to impaired metabolic control via both direct (increased cortisol levels) and indirect (decreased adherence) pathways.23 Since it is believed that 95% of diabetes management is conducted by the patient, comorbid mental health disorders may lead to poorer outcomes and increased risk of complications by decreasing adherence to glucose monitoring, foot care, exercise, diet, smoking cessation, and medication regimens.2,3,24,25
Depression (even low levels of depressive symptoms) and anxiety have been associated with impaired self-care activities in diabetic patients.5,12 High rates of neglect of proper self-care due to social withdrawal and psychosis are seen in schizophrenic patients.26 Lerman and colleagues noted that diabetic patients who have a history of excessive alcohol intake and are in a depressive state are two to four times more likely not to comply with diabetes self-care recommendations.27 Increasing HANDS (Harvard Department of Psychiatry/National Depression Screening Day Scale) scores have been found to be incrementally associated with poorer self-care behaviors (P <.01).5
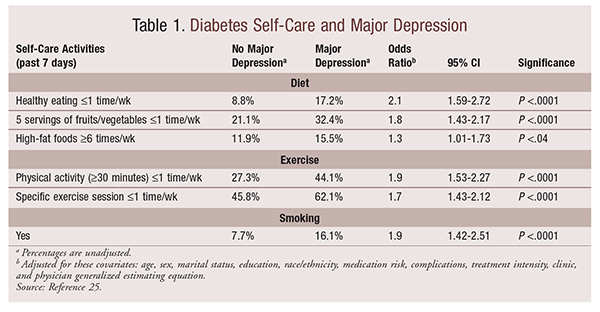
Adherence to Diet: In a study by Gonzalez and colleagues, patients with probable major depression (HANDS score 9) reported significantly fewer days adherent to diet (fruit and vegetable intake, carbohydrate intake spaced over the course of the day), exercise, and glucose self-monitoring (P <.01).5 As detailed in TABLE 1, compared with subjects without major depression, those with major depression were more likely to consume an unhealthy diet (infrequent fruit and vegetable intake and more frequent fat intake) and to be sedentary (exercising 1 time in a given week), and they were twice as likely to smoke.25 These results may be overestimated, since they were based on self-report; actual values may be lower.
Medication Adherence: Gonzalez and colleagues found that major depression was linked to a 2.3-fold increased odds of missed medication doses in the previous week (P <.001).5 Decreased medication compliance was also reported in a study by Lin and colleagues in which pharmacy refill data indicated that, in the prior year, diabetic patients with major depression were nonadherent to their hypoglycemic agents nearly 20 days more than patients without major depression (80 days missed vs. 62 days missed).25 It cannot be assumed, however, that patients consumed all of the refilled medication.25 Depression has been associated with a twofold greater likelihood of poor medication adherence and a shorter time to presence of elevated glycemic values among poorly controlled diabetic patients.24
Glycemic Control: Lustman and colleagues found that the presence of psychiatric illness was associated with worse long-term glucose control in diabetic patients (P <.05).28 The mean glycosylated hemoglobin (HbA1C) of patients with a recent psychiatric illness was higher than that of patients with remote or no psychiatric illness (HbA1C 10.8% vs. 10.1% vs. 9.6%, P <.05). These findings suggest that the more recent the psychiatric illness, the greater the impact on glycemic control.28 In this study, the mean HbA1C of patients who had any depressive episodes in the past was 10.92%, and that of recently depressed patients was 11.35%, compared with a mean of 9.58% in patients who were never psychiatrically ill (both, P <.05).28 The higher levels of HbA1C in these patients suggest that depression, in particular, may contribute to impaired glucose control in diabetes.28
Psychiatrically ill diabetic patients have been found to report more symptoms of poor glycemic control and more symptom-associated distress compared with patients who were never psychiatrically ill (both, P <.001).28 In a study by Lustman and colleagues, overall reports of diabetic symptoms (polydipsia and polyphagia) were not related to HbA1C level and were influenced mostly by a recent psychiatric disorder (P <.001).28 It was concluded, therefore, that psychiatric illness may make symptoms of diabetes less tolerable.28 Hampson and colleagues found that illness beliefs (perceived seriousness of diabetes, beliefs about treatment effectiveness, perceived control over diabetes) were independently associated with HbA1C, eating patterns, physical functioning, and mental health in diabetic patients.29
Lifestyle and Quality of Life: Individuals with depressive symptoms have a 41% to 89% increased risk of developing functional disability, which can be an obstacle for proper diabetes self-care and can impact control.30,31 Studies have shown that depressive symptoms predict the development of limitations in activities of daily living such as eating, drinking, shopping, cooking meals, walking, and doing housework.32 Treating comorbid depression has a direct impact on improvements in functional status.33
Diabetes guidelines strongly suggest that diabetic patients stop smoking, but over a 9-year period, smokers with depression were 40% less likely to quit smoking than nondepressed smokers. Smokers with a history of depression were more likely than nondepressed smokers to develop a major depressive episode. Therefore, improved smoking-cessation rates in diabetic patients may require improved screening and treatment of depression.34,35
Other Factors: Patients with diabetes and depression have been found to miss more medical appointments. This may be because medical appointments with providers require social interaction, which may be difficult in this patient population since mental health disorders are associated with impaired interpersonal behaviors (e.g., social withdrawal, disengagement, avoidance) and, often, a disruption of interpersonal relationships.36 Missed appointments can negatively impact patient-provider communication and continuity of care.37 Therefore, patient care can be compromised.
Individuals with comorbid diabetes and depression worry more about future diabetes complications and the social and vocational impact of diabetes.32 Patients with diabetes and mental health disorders have reported more sick days taken, pain interfering with work, and impaired physical functioning (P <.05).11 In a study by Simon and colleagues, >50% of patients in an HMO population who had comorbid diabetes and depression reported unemployment.38 Loss of income can have a dramatic effect on disease control in terms of adherence to treatment regimens and recommendations. Patients with mental disorders have reported an inability to obtain care or a need to delay care because of the cost.39
Possible causes of poor adherence and diabetes outcomes in patients with schizophrenia include poor integration of medical and psychiatric care, sedentary lifestyle, obesity, poor diet, nicotine use, cognitive impairment, psychosocial deficits, and limited family and social supports.40 One study of 200 randomly selected outpatients with severe mental illness found a high rate of perceived barriers to receipt of medical care in schizophrenic patients.40
Importance of Integrated Care
Strategies to improve the detection and treatment of mental health disorders in patients with diabetes are critical in order to improve function and decrease disability.41 Evidence from several controlled trials suggests that the detection and treatment of depression improves glycemic control.42 In addition, better quality-of-life ratings are associated with lower HbA1C levels.43 However, depression and anxiety are underdetected and undertreated in diabetic patients; these conditions are recognized in <50% of diabetic patients who have them.44 Diabetic patients should be regularly screened for symptoms of anxiety and depression since they are at higher risk for these conditions, and symptoms often are overlooked when they recur.12,15
In the study by Gonzalez and colleagues, only 59.4% of subjects with probable major depression had depression listed in their medical records, and an antidepressant had been prescribed for only 48.8% of them.5 Reports also indicate that only one-third of depressed patients with diabetes on antidepressant therapy are receiving an adequate dosage and only 6.7% are getting an adequate number of psychotherapy sessions.45 According to the National Institute of Diabetes and Digestive and Kidney Diseases, people with mental health disorders are less likely to be offered diabetes screening, education, and examination for complications.46 Dixon and colleagues found that patients with schizophrenia were less likely than those without a mental illness to receive diabetes education.40 In the study by Lin and colleagues, only 50% of patients received annual microalbuminuria screening.25 In addition, a slightly higher proportion of patients with major depression received no HbA1C test in the prior year, compared with diabetic patients without major depression (6.3% vs. 4%; P <.005). Even among patients with poor control (HbA1C ≥8%), the mean number of HbA1C tests per year was low (2.4).25
The American Diabetes Association has recommended integrated delivery of behavioral health with diabetes care.47 Concurrent management by multiple clinicians with poor coordination can impact patients’ therapeutic alliance with their providers, a factor that has been found to affect patient adherence to medications.48 Open communication between healthcare providers and patients reduces barriers to care. Efficient communication and referral protocols between primary care, mental health, and endocrinology departments are needed. Alerts and constant monitoring by healthcare teams for poor diabetes and/or mental health control, medication noncompliance, and clinical inertia (failure to intensify or initiate treatment) in those with poor disease control are necessary.24
Role of the Pharmacist
Pharmacists are highly trusted medical professionals, placing second among the professions listed in a 2014 Gallup poll.49 Individual assessment, collaborative goal setting, skill building, follow-up, and support are needed for the effective treatment of diabetic patients with comorbid mental health disorders, and they represent areas of patient care within the realm of pharmacist capabilities.47 Most reviews of evidence-based interventions to improve patient outcomes suggest that increasing the frequency of contacts, monitoring disease outcomes and adherence, and facilitating return appointments for patients with persistently poor disease control are beneficial.50 Pharmacists can work with collaborating psychiatrists, primary care physicians, and endocrinologists to enhance patient education, provide more frequent follow-up, and monitor for side effects, adherence to medication, and the need for dose titrations. Pharmacists can help patients understand and react to fingerstick readings, a skill that can be used every day. Patients have better outcomes when provided with disease-specific knowledge and skills.51 Pharmacists can also facilitate return appointments to primary care physicians or specialists for patients with persistent symptoms or lack of improvement despite interventions.
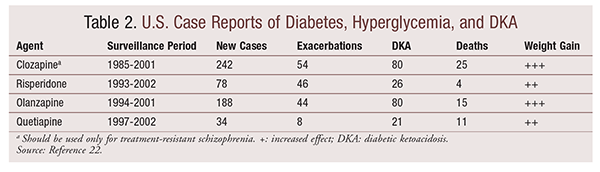
Medication management is extremely important in the schizophrenic population. The pharmacist can help ensure that the patient is screened for undiagnosed diabetes or impaired glucose tolerance (regardless of risk factors and presence of symptoms) prior to initiation of a second-generation antipsychotic.22 The relative risks of diabetes and weight gain should be considered when an antipsychotic is being selected for a patient who has diabetes or is at significant risk for developing it.22 TABLE 2 compares several second-generation antipsychotics.22 The pharmacist should counsel patients on the risks of metabolic side effects and weight gain associated with their medication and should provide diet and exercise guidance to help manage these side effects. The pharmacist can consult with the patient’s psychiatrist if the patient is experiencing worsening glycemic control or if an alternative antipsychotic may be necessary.22
Pharmacists can also work with providers and patients to overcome barriers to medication adherence. In a study by Piette and colleagues, medication regimens with an average supply of ≤30 days were associated with a 3.3-fold increase in relative odds of nonadherence, compared with a supply of ≥60 days.52 Dispensing medications in a supply of ≤30 days enables faster detection of adverse effects and more frequent follow-up, but shorter refill intervals can increase medication nonadherence because of the effort involved with frequent refilling. Pharmacists can review medication regimens and work collaboratively with prescribing providers and patients to promote adherence, patient safety, and proper follow-up.53 The financial impact of copays for larger supplies must also be considered, especially in patients with multiple prescriptions.
The choice of diabetes and mental health medications should be made jointly with the patient (or caregiver, if appropriate) based on an open discussion of side-effect profiles, risk-benefit analyses, and patient preferences. To optimize health outcomes, the patient and his or her loved ones should be involved in shared decision making; they are core members of the care team, not just passive recipients of care.53 In developing a care plan, the unique needs, culture, values, and preferences of the patient should be understood and respected. Shared decision making fosters improved provider-patient relationships and increased adherence.
Clinical outcomes also improve when patients are involved in clinical decisions.54 In an intervention study, patients who were encouraged to participate more actively in the clinic visit reduced their HbA1C from 10.6% to 9.1%, whereas HbA1C increased from 10.3% to 10.6% in controls (P <.01).55 Shared decision making and realistic goals are considered the basis of behavior-change action plans or goal setting.54 In a randomized, controlled trial, patients were assigned to traditional patient education or goal setting with an action plan. The action-plan group had a significant reduction in HbA1C compared with the patient-education group, whose HbA1C did not change (P = .03).56
Health coaching affords interested pharmacists the opportunity to provide ongoing support and care to diabetic patients with mental health disorders. TABLE 3 lists the principal roles of a health coach.53 Health coaches offer patients assistance in five core areas: understanding, knowing their numbers and goals, shared decision making, behavior change, and medication adherence.54

Conclusion
Pharmacists should be aware of the possible coexistence of diabetes and mental health disorders and should always encourage patients to report changes in mood to facilitate necessary mental health care. Pharmacists should also consider the impact of different medications on glycemic control. Pharmacists are a valuable healthcare resource, and with adequate time and training, they can provide regular monitoring and management of both diabetes and mental health disorders to improve care in this patient population.
REFERENCES
1. Cox DJ, Gonder-Frederick L. Major developments in behavioral diabetes research. J Consult Clin Psychol. 1992;60:628-638.
2. Lisi DM. Diabetes and the psychiatric patient. US Pharm. 2010;35(11):62-79.
3. Ciechanowski P, Katon WJ, Russo JE. Depression and diabetes: impact of depressive symptoms on adherence, function, and costs. Arch Intern Med. 2000;160:3278-3285.
4. Black SA, Markides KS, Ray LA. Depression predicts increased incidence of adverse health outcomes in older Mexican Americans with type 2 diabetes. Diabetes Care. 2003;26:2822-2888.
5. Gonzalez JS, Safren SA, Cagliero E, et al. Depression, self-care, and medication adherence in type 2 diabetes: relationships across the full range of symptom severity. Diabetes Care. 2007;30:2222-2227.
6. Peyrot M, Rubin RR. Persistence of depressive symptoms in diabetic adults. Diabetes Care. 1999;22:448-452.
7. de Groot M, Risaliti C, Doyle T, et al. Persistence of depression among type 2 diabetes Appalachians. Ann Behav Med. 2007;33(suppl):S178.
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed, text rev. Washington, DC: American Psychiatric Association; 2000.
9. Lustman PJ, Griffith LS, Freedland KE, Clouse RE. The course of major depression in diabetes. Gen Hosp Psychiatry. 1997;19:138-143.
10. Hampson SE, Glasgow RE, Foster LS. Personal models of diabetes among older adults: relationship to self-management and other variables. Diabetes Educ. 1995;21:300-307.
11. Das-Munshi J, Stewart R, Ismail K, et al. Diabetes, common mental disorders, and disability: findings from the UK National Psychiatric Morbidity Survey. Psychosom Med. 2007;69:543-550.
12. Stoop CH, Spek VR, Pop VJ, Pouwer F. Disease management for co-morbid depression and anxiety in diabetes mellitus: design of a randomised controlled trial in primary care. BMC Fam Pract. 2011;12:139.
13. Paschalides C, Wearden AJ, Dunkerley R, et al. The associations of anxiety, depression and personal illness representations with glycaemic control and health-related quality of life in patients with type 2 diabetes mellitus. J Psychosom Res. 2004;57:557-564.
14. Peyrot M, Rubin RR. Levels and risks of depression and anxiety symptomatology among diabetic adults. Diabetes Care. 1997;20:585-590.
15. Collins MM, Corcoran P, Perry IJ. Anxiety and depression symptoms in patients with diabetes. Diabet Med. 2009;26:153-161.
16. Casey DE. Metabolic issues and cardiovascular disease in patients with psychiatric disorders. Am J Med. 2005;118(suppl 2):15S-22S.
17. Dixon L, Weiden P, Delahanty J, et al. Prevalence and correlates of diabetes in national schizophrenia samples. Schizophr Bull. 2000;26:903-912.
18. American Diabetes Association, American Psychiatric Association, American Association of Clinical Endocrinologists, North American Association for the Study of Obesity. Consensus development conference on antipsychotic drugs and obesity and diabetes. Diabetes Care. 2004;27:596-601.
19. Holt RI, Peveler RC. Antipsychotic drugs and diabetes—an application of the Austin Bradford Hill criteria. Diabetologia. 2006;49:1467-1476.
20. Koller EA, Doraiswamy PM. Olanzapine-associated diabetes mellitus. Pharmacotherapy. 2002;22:841-852.
21. Meduna LJ, Gerty FJ, Urse VG. Biochemical disturbances in mental disorders. Arch Neurol Psychiatry. 1942;47:38-52.
22. Barnett AH, Mackin P, Chaudhry I, et al. Minimising metabolic and cardiovascular risk in schizophrenia: diabetes, obesity and dyslipidaemia. J Psychopharmacol. 2007;21:357-373.
23. Levy MI, Davis KL. The neuroendocrinology of depression. In: Rifkin A, ed. Schizophrenia and Affective Disorders: Biology and Drug Treatment. Boston, MA: John Wright;1983:1-17.
24. Katon W, Russo J, Lin EH, et al. Diabetes and poor disease control: is comorbid depression associated with poor medication adherence or lack of treatment intensification? Psychosom Med. 2009;71:965-972.
25. Lin EH, Katon W, Von Korff M, et al. Relationship of depression and diabetes self-care, medication adherence, and preventive care. Diabetes Care. 2004;27:2154-2160.
26. Goldman LS. Medical illness in patients with schizophrenia. J Clin Psychiatry. 1999;60(suppl 21):10-15.
27. Lerman I, Lozano L, Villa AR, et al. Psychosocial factors associated with poor diabetes self-care management in a specialized center in Mexico City. Biomed Pharmacother. 2004;58:566-570.
28. Lustman PJ, Griffith LS, Clouse RE, Cryer PE. Psychiatric illness in diabetes mellitus. Relationship to symptoms and glucose control. J Nerv Ment Dis. 1986;174:736-742.
29. Hampson SE, Glasgow RE, Strycker LA. Beliefs versus feelings: a comparison of personal models and depression for predicting multiple outcomes in diabetes. Br J Health Psychol. 2000;5:27-40.
30. Gregg EW, Mangione CM, Cauley JA, et al. Diabetes and incidence of functional disability in older women. Diabetes Care. 2002;25:61-67.
31. Bruce DG, Davis WA, Davis TM. Longitudinal predictors of reduced mobility and physical disability in patients with type 2 diabetes: the Fremantle Diabetes Study. Diabetes Care. 2005;28:2441-2447.
32. Schram MT, Baan CA, Pouwer F. Depression and quality of life in patients with diabetes: a systemic review from the European Depression in Diabetes (EDID) research consortium. Curr Diabetes Rev. 2009:112-119.
33. Williams JW Jr, Katon W, Lin EH, et al. The effectiveness of depression care management on diabetes-related outcomes in older patients. Ann Intern Med. 2004;140:1015-1024.
34. Katon W, von Korff M, Ciechanowski P, et al. Behavioral and clinical factors associated with depression among individuals with diabetes. Diabetes Care. 2004;27:914-920.
35. Dierker L, Avenevoli S, Stolar M, Merikangas KR. Smoking and depression: an examination of mechanisms of comorbidity. Am J Psychiatry. 2002;159:947-953.
36. Gonzalez JS, Peyrot M, McCarl LA, et al. Depression and diabetes treatment nonadherence: a meta-analysis. Diabetes Care. 2008;31:2398-2403.
37. Pesata V, Pallija G, Webb AA. A descriptive study of missed appointments: families’ perceptions of barriers to care. J Pediatr Health Care. 1999;13:178-182.
38. Simon GE, Von Korff M, Lin E. Clinical and functional outcomes of depression treatment in patients with and without chronic medical illness. Psychol Med. 2005;35:271-279.
39. Druss BG, Rosenheck RA. Mental disorders and access to medical care in the United States. Am J Psychiatry. 1998;155:1175-1177.
40. Dixon LB, Kreyenbuhl JA, Dickerson FB, et al. A comparison of type 2 diabetes outcomes among persons with and without severe mental illnesses. Psychiatr Serv. 2004;55:892-900.
41. Egede LE. Diabetes, major depression, and functional disability among U.S. adults. Diabetes Care. 2004;27:421-428.
42. Lustman PJ, Clouse RE, Freedland KE. Management of major depression in adults with diabetes: implications of recent clinical trials. Semin Clin Neuropsychiatry. 1998;3:102-114.
43. Rubin RR, Peyrot M. Quality of life and diabetes. Diabetes Metab Res Rev. 1999;15:205-218.
44. Rubin RR, Ciechanowski P, Egede LE, et al. Recognizing and treating depression in patients with diabetes. Curr Diab Rep. 2004;4:119-125.
45. Katon WJ, Simon G, Russo J, et al. Quality of depression care in a population-based sample of patients with diabetes and major depression. Med Care. 2004;42:1222-1229.
46. Holt RI, de Groot M, Lucki I, et al. NIDDK International Conference Report on Diabetes and Depression: current understanding and future directions. Diabetes Care. 2014;37:2067-2077.
47. Anderson D, Horton C, O’Toole ML, et al. Integrating depression care with diabetes care in real-world settings: lessons from the Robert Wood Johnson Foundation Diabetes Initiative. Diabetes Spectr. 2007;20:10-16.
48. Lacro JP, Dunn LB, Dolder CR, et al. Prevalence of and risk factors for medication non-adherence in patients with schizophrenia: a comprehensive review of recent literature. J Clin Psychiatry. 2002;63:892-909.
49. Gallup. Honesty/ethics in professions. www.gallup.com/poll/1654/honesty-ethics-professions.aspx. Accessed June 8, 2015.
50. Renders CM, Valk GD, Griffin SJ, et al. Interventions to improve the management of diabetes in primary care, outpatient, and community settings: a systematic review. Diabetes Care. 2001;24:1821-1833.
51. Bodenheimer T, Lorig K, Holman H, Grumbach K. Patient self-management of chronic disease in primary care. JAMA. 2002;288:2469-2475.
52. Piette JD, Heisler M, Ganoczy D, et al. Differential medication adherence among patients with schizophrenia and comorbid diabetes and hypertension. Psychiatr Serv. 2007;58:207-212.
53. Bennett HD, Coleman EA, Parry C, et al. Health coaching for patients with chronic illness. Fam Pract Manag. 2010;17:24-29.
54. Ghorob A, Willard-Grace R, Bodenheimer T. Health coaching. Virtual Mentor. 2013;15:319-326.
55. Greenfield S, Kaplan SH, Ware JE Jr, et al. Patients’ participation in medical care: effects on blood sugar control and quality of life in diabetes. J Gen Intern Med. 1988;3:448-457.
56. Naik AD, Palmer N, Petersen NJ, et al. Comparative effectiveness of goal setting in diabetes mellitus group clinics: randomized clinical trial. Arch Intern Med. 2011;171:453-459.
To comment on this article, contact rdavidson@uspharmacist.com.





