Comorbidities and their associated concomitant medications complicate the use of many classes of pharmacotherapeutic agents. Such is the case with psychotherapeutic medications in the elderly (TABLE 1). Seniors experience more adverse effects with psychoactive medications, with a tendency toward greater seriousness, as compared with younger patients.1 Treating seniors with these agents is also complicated by age-related pharmacokinetic (PK) and pharmacodynamic (PD) changes. Further, these PK and PD changes can be exacerbated by acute illness, the potential for concomitant drug-drug interactions, and poor medication adherence.1
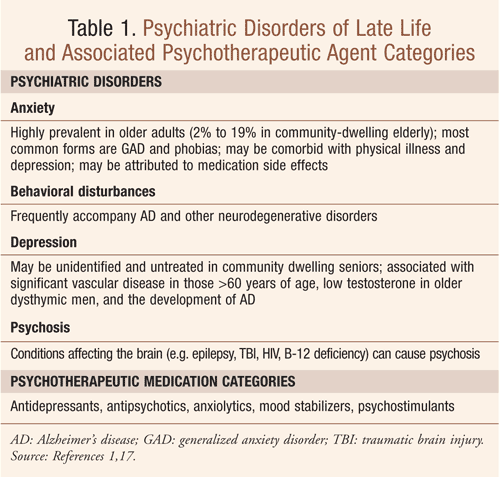
When treating seniors with psychotherapeutic medications, clinicians must conduct an individualized risk analysis based on the strength of data available for each condition and drug; the side effect profile of each drug; and its safety with concomitant medications.1 Quality of life is an important element when formulating a pharmaceutical care plan and should be discussed with the patient, family, and caregivers when possible. The debilitating and detrimental effects of late-life psychiatric illness (TABLE 1) on activities of daily living, cognition, institutionalization, and mortality should also be taken into consideration when formulating the medication's risk-to-benefit ratio.1 Of note, undertreated or undiagnosed psychiatric illness may complicate underlying medical conditions and place additional stress, directly and indirectly, on the health care system.
Antipsychotic Agents
A discussion of both categories of antipsychotic agents (TABLE 2) is beyond the scope of this article; pharmacists are referred to Reference 2 for an overview and detailed discussion of each. For this column, the focus will be on highlights regarding side effects of the atypical (second generation) antipsychotic agents whose major advantage can be their lower risk of neurologic side effects, particularly on movement.2
Antipsychotic Use in Seniors With Dementia
Of note, although antipsychotic drugs are widely used to treat psychosis, aggression, and agitation in patients with Alzheimer's disease, their benefits are uncertain.3 Concerns about safety have not only emerged, but have also been assessed with regard to effectiveness in outpatients with Alzheimer's disease.3 Schneider et al have reported, based on a 42-site, double-blind, placebo-controlled trial, that the adverse effects offset the advantages in the efficacy of atypical antipsychotic drugs for the treatment of psychosis, aggression, or agitation in patients with Alzheimer's disease.3
Both traditional and atypical antipsychotic agents are not FDA approved for the treatment of dementia-related psychosis.4 Use of these agents in geriatric patients with dementia-related psychosis is associated with an increased risk of death.4 It is recommended that prescribers instituting antipsychotic medication in the regimen of a geriatric patient with dementia-related psychosis discuss the risk of increased mortality with the patient, family members, and caregivers if possible.5 Since there is no FDA-approved medication for the treatment of dementia-related psychosis, other management options should be considered by health care providers.5 In dementia, cholinesterase inhibitors (e.g., donepezil, rivastigmine, galantamine) are used for cognitive difficulty and are discussed in Reference 6.
Common Adverse Effects of Antipsychotic Agents
The majority of undesirable effects of the antipsychotic agents are extensions of their pharmacologic actions. Additionally, there are some allergic and idiosyncratic adverse effects.7 In an attempt to limit the emergence of side effects associated with antipsychotic agents, elderly patients should receive lower doses than those used in younger patients. Parenterally administered agents have greater bioavailability as compared with oral dosage forms, and therefore should be dosed accordingly.7
One of the key concepts of appropriate antipsychotic therapy is that side-effect profiles should be used as a basis for selecting antipsychotic agents, since it is challenging to differentiate among antipsychotics based on efficacy alone.2 Using this concept, clinicians should tailor the antipsychotic medication regimen to the individual, incorporating pertinent information to help in selecting an appropriate antipsychotic agent, such as medical history (cardiac or cerebrovascular disease, seizure disorder); medication history (e.g., drug-related orthostatic hypotension); and family history (e.g., diabetes). In patients who complain of poorly tolerated side effects, using an alternative medication should be considered in light of the variety of antipsychotics currently available.2 Patient and family counseling should take place, including education about the illness, symptoms, prognosis, medication, and other psychosocial interventions and adaptive functioning methods.2
Sedation and Cognition: Sedation occurs early in the treatment course and may decrease over time.8 While oversedation may contribute to cognitive, perceptual, and motor dysfunction, positive effects from medication on cognition have been seen with chronic administration.2,8 The agents most frequently implicated in causing sedation are chlorpromazine, thioridazine, mesoridazine, and the atypicals clozapine, olanzapine, and quetiapine.2 Since cognitive impairment renders the senior's disease profile more chronic and treatment resistant,1 any change in cognitive status should be evaluated (e.g., to compare with baseline; to rule out delirium).
Extrapyramidal Symptoms (EPS): EPS include akathisia, a restlessness that may present as anxiety and agitation and result in inappropriate medication therapy; dystonia, an abnormal tonicity featuring prolonged tonic-clonic contractions that may progress and be life threatening; pseudoparkinsonism, including bradykinesia, rigidity, and tremor; and tardive dyskinesia, an abnormal involuntary movement disorder. It has been estimated that half of patients between 60 and 80 years of age taking traditional antipsychotic agents experience EPS.1 Comparator trials have revealed a lower incidence of milder EPS with the atypical agents as compared with the traditional (first generation) antipsychotic agents.1 Olanzapine has a very low incidence of EPS at 10 to 20 mg/day, although many patients receive higher doses in practice.9,10
Anticholinergic: Anticholinergic effects such as constipation, dry mouth, blurred vision, and urinary retention are particularly problematic in the elderly and may contribute to delirium. They are most common with low-potency traditional antipsychotic agents (e.g., chlorpromazine) and clozapine.
Cardiovascular: Cardiovascular effects include electrocardiographic (ECG) changes and orthostatic hypotension (OH).2 ECG changes may include tachycardia from anticholinergic effects or reflex tachycardia from alpha-adrenergic blockade; flattened T waves; ST segment depression; and prolongation of QT and PR intervals.2 OH may result when antipsychotics block beta-adrenergic receptors, and can lead to falls and fractures in the elderly.1 OH is likely to occur with low-potency traditional antipsychotics (e.g., chlorpromazine, thioridazine) and with atypical agents such as clozapine, risperidone, olanzapine, and quetiapine.1 Caution is necessary with use of these agents in seniors with preexisting cardiac or cerebrovascular disease, and in those taking diuretics or concomitant drugs that can prolong the QTc interval.11 A baseline ECG and baseline serum potassium and magnesium levels are recommended in patients >50 years of age.2 Antipsychotics most likely to cause ECG changes are thioridazine and the atypicals clozapine and ziprasidone.2
Weight Gain, Diabetes, and Lipid Abnormalities: Weight gain is a substantially significant side effect of antipsychotic agents and is frequently reported in both adults and children.12,13 Olanzapine and clozapine cause more weight gain than other atypical antipsychotic agents (i.e., >7% of the baseline body weight in 40% or more of patients).2,11,12 Minimal weight gain has been associated with both ziprasidone and aripiprazole.2
Elevations in serum triglycerides (TGs) and cholesterol have been reported with at least some of the atypical antipsychotic agents.2 There is a reported lower risk for change in serum lipid or cholesterol levels with risperidone, ziprasidone, and aripiprazole.14 The risk for the development of metabolic syndrome (i.e., syndrome X: elevation in glucose, TGs, weight/abdominal circumference, blood pressure; low HDL) and diabetes associated with the atypical antipsychotic agents warrants a general health screening and monitoring; if abnormalities occur in patients treated with these agents, intervention should be prompt.
Prolactin: In seniors, an increase in prolactin levels (i.e., due to dopamine blockade) can cause galactorrhea in women and gynecomastia and galactorrhea in men; these effects are more common with the traditional antipsychotic agents and with risperidone and can be dose related.2 Using an alternative agent with no appreciable sustained effect on prolactin (e.g., olanzapine, quetiapine, ziprasidone, aripiprazole) is an option.2
Other Side Effects: Additional side effects and adverse reactions, including the following, are discussed in References 1 and 2: seizures; thermoregulatory problems and neuroleptic malignant syndrome; ophthalmologic effects; psychiatric side effects; and effects on the dermatologic, genitourinary, hematologic, and hepatic systems.
Monitoring
Monitoring for common and potentially disabling side effects of psychotropic medications should be incorporated into the ongoing assessment process. Any unexpected adverse or serious events associated with the use of antipsychotic agents should be reported by health care practitioners, including pharmacists; information about how to report an adverse reaction to the FDA MedWatch Program can be obtained at: www.fda.gov/Safety/MedWatch/Atypical antipsychotic-agent monitoring parameters may include:15,16
* Vital signs
* Fasting lipid profile and fasting blood glucose/HbA1C (prior to treatment, at 3 months, then annually)
* Body mass index, personal/family history of diabetes, waist circumference
* Blood pressure
* Mental status, abnormal involuntary movement scale (AIMS), EPS
* Weight assessment prior to treatment, at 4 weeks, at 8 weeks, at 12 weeks, and then at quarterly intervals
* If a weight gain of ³5% of the initial weight occurs, consider titrating to an alternative antipsychotic agent
* Baseline ECG; baseline serum potassium and magnesium levels
Plasma concentration monitoring of antipsychotic agents is not warranted.7
Conclusion
Seniors have an increased risk of adverse response to side effects, or adverse reactions to antipsychotic agents. In selecting an antipsychotic agent for a geriatric patient, it is recommended to carefully consider the clinical profile of the patient and the side-effect profile of the drug.
REFERENCES
2. Crismon ML, Argo TR, Buckley PF. Schizophrenia. In DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 7th ed. New York, NY: McGraw-Hill Inc; 2008:1099-1122.
3. Schneider LS, Tariot PN Dagerman KS, et al. Effectiveness of atypical antipsychotic drugs in patients with Alzheimer's disease. N Engl J Med. 2006;355(15):1525-1538.
4. Information on antipsychotics. U.S. Food and Drug Administration. U.S. Department of Health and Human Services. www.fda.gov/Drugs/DrugSafety/
5. Zagaria ME. Antipsychotics in seniors: Warnings to prevent misuse. US Pharm. 2008;33(11):20-22.
6. Birks J. Cholinesterase inhibitors for Alzheimer's disease. Cochrane Database Syst Rev. 2006;1: CD005593.
7. Potter WZ, Hollister LE. In: Katzung BG. Basic and Clinical Pharmacology. 9th ed. New York, NY: The McGraw-Hill; 2004:462-481.
8. Tandon R. Safety and tolerability: How do newer generation "atypical" antipsychotics compare? Psychiatr Q. 2002;73:297-311.
9. Jones P, Buckley P. Schizophrenia. London: Mosby; 2006.
10. Lehman AF, Lieberman JA, Dixon LB, et al. American Psychiatric Association Steering Committee on Practice Guidelines. Practice guidelines for the treatment of patients with schizophrenia; 2nd ed. Am J Psychiatry. 2004;161(2 suppl):1-56.
11. Miller AL, Dassori A, Ereshefsky L, et al. Recent issues and developments in antipsychotic use. In: Dunner DL, Rosenbaum JF, eds. Psychiatric Clinics of North America Annual Review of Drug Therapy. 2001. Philadelphia, PA: WB Saunders; 2001;8:209-235.
12. Allison DB, Mentore JL, Heo M, et al. Antipsychotic-induced weight gain: a comprehensive research synthesis. Am J Psychiatry. 1999;156:1686-1696.
13. Patel NC, Kistler JL, James EB, et al. A retrospective analysis of olanzapine and quetiapine on weight and body mass index in children and adolescents. Pharmacotherapy. 2004;24:824-830.
14. Meyer JM. Cardiovascular illness and hyperlipidemia in patients with schizophrenia. In: Meyer JM, Nasarallah HA, eds. Medical Illness and Schizophrenia. Washington, DC: American Psychiatric Press; 2003:53-80.
15. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 14th ed. Hudson, OH: Lexi-Comp, Inc; 2009.
16. Zagaria ME. Atypical antipsychotic agents: monitoring for metabolic syndrome. Amer J Nurse Pract. 2007;11(10):20-26.
17. Lieberman JA. Schizophrenia. Epocrates Mobile Resource Center. www.epocrates.com Accessed
October 25, 2010.
To comment on this article, contact rdavidson@uspharmacist.com






