US Pharm. 2014;39(9):35-39.
ABSTRACT: Breast cancer is one of the most common cancers, second only to lung cancer, among American women. However, death rates from breast cancer have been declining since 1989 due to earlier detection through screening, increased awareness, and treatment improvement. Besides being costly and toxic, breast cancer treatment is not 100% effective; therefore, clinicians should focus on prevention, such as risk factor reduction and/or use of chemoprevention. Recently, the U.S. Preventive Services Task Force (USPSTF) issued a new guideline about using certain medications (tamoxifen or raloxifene) to prevent breast cancer in women. Since the use of chemoprevention is very low for eligible women, pharmacists can play an important role in educating women about the benefits versus risks of chemoprevention including benefit-risk evaluations, proper medications, dosing, indications, adverse effects, and drug interactions. Contribution to breast cancer prevention for women is a challenge for pharmacists, as it requires significant effort for planning and execution.
Breast cancer is a group of cancer cells (malignant tumor) that develop in the breast and may invade surrounding tissues or spread to distant areas of the woman’s body to become metastatic cancer. Most breast cancers begin in the duct cells (ductal cancer) and can invade the lymphatic vessels and grow in the lymph nodes. Thereafter, cancer cells may get into the bloodstream and spread to other sites of the body. Since the prognosis of metastasis is poor, it is important to discover breast cancer as early as possible so that treatment can be more effective.
Breast cancer is one of the most common cancers, second only to lung cancer, among American women. Death rates from breast cancer have been declining since 1989 due to earlier detection of breast cancer through screening, increased awareness, and treatment improvement.1 However, breast cancer is still a very common threat to women, as it is estimated that more than 230,000 new cases of invasive breast cancer and 62,000 new cases of carcinoma in situ (CIS) will be diagnosed, and about 40,000 women will die from breast cancer in the United States in 2014.1 Per the American Cancer Society (ACS), about 12% of women will likely develop invasive breast cancer during their lifetime.1
Risk Factors
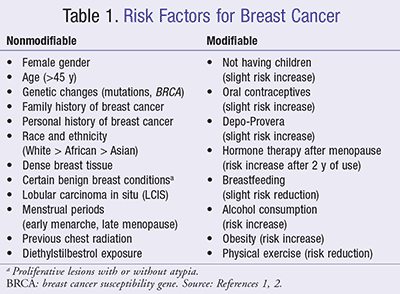
The nonmodifiable risk factors of breast cancer for women and modifiable lifestyle-related risk factors are listed in TABLE 1.1,2 There are also other factors that have been suggested to increase breast cancer but remain controversial due to inconclusive results (e.g., diet and vitamin intake, chemicals in the environment, tobacco smoking, night shift work) or lack of evidence in several different studies (e.g., antiperspirants, bras, induced abortion, breast implants).1 Pharmacists should be knowledgeable about these factors in order to counsel patients on how to reduce breast cancer risk effectively.
![]()
Pathology
How certain factors cause normal cells to become cancerous is not clearly understood. It is believed that gene mutations in DNA alter the gene functions (e.g., oncogenes no longer speed up cell division or tumor suppressor genes no longer suppress abnormal growth), thus resulting in breast cancer. Therefore, most cases of breast cancer are not caused by inherited tumor suppressor (BRCA) genes but by low-penetrance mutations or gene variations.1 Genetic testing can help identify some women with inherited mutations, thus enabling these women to take steps to reduce cancer risk (e.g., taking medications for chemoprevention or having prophylactic surgery). Testing to detect acquired gene changes in women also helps clinicians to predict breast cancer prognosis (e.g., aggressive breast cancer for women with too many copies of the human epidermal growth factor receptor 2 [HER2] oncogene).1
Breast Cancer Prevention
Since in addition to its cost and toxicities, cancer treatment is not 100% effective, clinicians should focus on prevention, and the best way to prevent breast cancer is to reduce risk factors.3 Women may reduce some of the modifiable risk factors shown in TABLE 1 by controlling body weight, exercising regularly (moderate to vigorous physical activity lowers risk of breast cancer in many studies), consuming healthy food (vegetables, fruit, poultry, fish, and low-fat dairy products decrease breast cancer risk per some studies), and avoiding alcohol.1
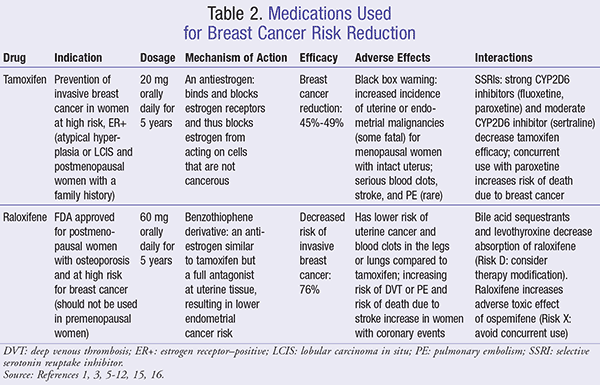
Tamoxifen and Raloxifene: In the 2013 update by the U.S. Preventive Services Task Force (USPSTF), certain medications (known as selective estrogen receptor modulators, or SERMs) are recommended for breast cancer reduction for asymptomatic women aged 35 years without a previous diagnosis of breast cancer, ductal carcinoma in situ (DCIS), or lobular carcinoma in situ (LCIS).4,5 The USPSTF recommends using tamoxifen or raloxifene (TABLE 2) for risk reduction for women with an estimated 5-year breast cancer risk of 3% using the Freeman Risk Assessment Model.4 On the other hand, the American Society of Clinical Oncology (ASCO) recommends a risk cutoff of 1.66% as determined by the Gail Model or study results on women with a history of LCIS.4,6 However, at this lower cutoff, many women will not get a net benefit from using medication for reducing breast cancer risk.4
Clinicians may use a breast cancer risk assessment model to evaluate risk for a woman using different risk factors (age, race or ethnicity, age at menarche, age at first live childbirth, personal history of DCIS or LCIS, number of first-degree relatives with breast cancer, personal history of breast biopsy, body mass index, menopause status or age, breast density, estrogen and progestin use, smoking, alcohol use, physical activity, and diet). Thereafter, risk assessment should be repeated for any changes in risk factors. It is noted that all risk assessment models (e.g., National Cancer Institute, Freeman, Breast Cancer Surveillance Consortium [BCSC], Rosner-Colditz, Chlebowski, Tyrer-Cuzick) should not be used for women with a history of radiation treatment to the chest, or a possible history of mutations in the BRCA1 or BRCA2 genes.4 The USPSTF does not endorse a specific model but does recommend that women with >10% risk probability consult with an experienced genetic counselor regarding potential genetic testing.4
Per the USPSTF, clinicians should discuss and offer risk-reducing medications to women who are at increased risk for breast cancer but at low risk for adverse effects from the medications.4,5 ASCO also recommends that clinicians share and discuss information (preventive medication, benefits, and its adverse drug reactions) to reduce risk for women with an increased risk for breast cancer in the new 2013 guideline (vs. “may be offered” in the 2009 guideline).6-8
To reduce the risk of breast cancer, tamoxifen and raloxifene should be used for 5 years with a daily dose of 20 mg and 60 mg, respectively. A systematic review of seven good and fair-quality trials indicates that tamoxifen reduced incidence of invasive breast cancer by seven cases and raloxifene by nine cases out of 1,000 women over 5 years compared with placebo.9 ASCO also recommends exemestane 25 mg oral daily for 5 years as another option for postmenopausal women even though this drug has not been approved by the FDA for chemoprevention.10
Tamoxifen and raloxifene reduce incidents of bone fracture, but raloxifene is preferred for women with osteoporosis or low bone density.5,6,9 However, tamoxifen and raloxifene should not be used for women who are not at increased risk for breast cancer, have a history of thromboembolic events (e.g., deep venous thrombosis, pulmonary embolus, stroke, or transient ischemic attack), and who are pregnant or breastfeeding, nor in combination with hormone therapy and hormonal contraception.4
Common adverse effects of tamoxifen include venous thromboembolic events, endometrial cancer (only with women having an intact uterus), uterine bleeding, cataract, vasomotor symptoms, vaginal discharge, itching, or dryness.4,11,12 The most common reported adverse effects of raloxifene are venous thromboembolic events, uterine bleeding, cataract, vasomotor symptoms, and leg cramps.4,7
Aromatase Inhibitors: Aromatase inhibitors (e.g., anastrozole, exemestane, letrozole) have been studied for breast cancer prevention in postmenopausal women who are estrogen receptor–positive (ER+). Per the International Breast Cancer Intervention Study II, anastrozole decreased incidence of breast cancer about 50% for high-risk postmenopausal women who were administered the drug for 5 years with no reported increase in endometrial cancer, bleeding, blood clots, or thromboembolic events.13,14 Exemestane blocks the production of a small amount of estrogen in menopausal women, thus lowering the risk of invasive breast cancer by 65% in a recent study.1,14 Common adverse effects of these drugs include joint pain and stiffness, bone loss (resulting in high risk of osteoporosis or even broken bones). However, aromatase inhibitors are not yet approved by the FDA for breast cancer prevention.1,6,8,14
Adverse Reactions and Interactions of Tamoxifen and Raloxifene
Pharmacists may consult with women on the risks and benefits of using chemoprevention for women with high risk of developing breast cancer. Adverse effects of tamoxifen and raloxifene should be discussed with women to ease their concerns and to increase their awareness of monitoring for any side effects while using the medications. In addition, the patient profiles can be reviewed for any drug interactions with tamoxifen or raloxifene; thus, other medications can be modified or changed to compensate for any drug interactions with tamoxifen or raloxifene. Common adverse reactions and interactions of tamoxifen and raloxifene are summarized in TABLE 2.1,3,5-12,15,16
Preventive Surgery for Women With Very High Risk of Breast Cancer
For women with an increased risk of having a BRCA mutation based on a family history of breast cancer, the USPSTF recommends genetic counseling before the related patient decides to have the genetic testing performed (because BRCA mutations are rare and the genetic testing is very expensive). For women with a very high risk for breast cancer (having mutated BRCA genes, strong family history of breast cancer, LCIS, or previous cancer in one breast), preventive surgery (mastectomy, oophorectomy) may be an option.1,4
A preventive mastectomy involves removing both breasts before cancer is diagnosed (applied for some women diagnosed with cancer in one breast). It may or may not apply to women with BRCA mutations. Breast removal does not completely prevent breast cancer, but reduces the risk up to 97%. Per the ACS, it is only applied for strong clinical and/or pathologic indications.1
A preventive oophorectomy involves removal of the ovaries for women with a BRCA mutation before menopause. This procedure reduces the risk of developing breast cancer by 50% or more.1
Screening for Breast Cancer
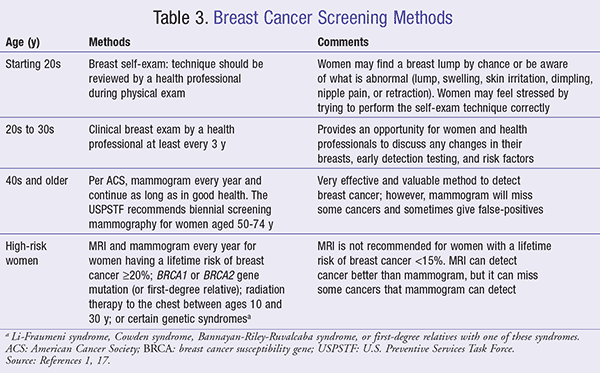
For successful treatment, it is very important for women to detect breast cancer when the cancer is still localized. Consequently, women should follow the ACS guidelines for early detection of breast cancer as strictly as possible. Breast cancer can be screened using breast self-examination, clinical breast examination, mammography, and MRI (TABLE 3).1,4,17
Recently, the benefit of mammography screening has been questioned by the Swiss Academy of Medical Sciences because of false-positive test results and the risk of overdiagnosis.18 Per recently published extended follow-up (25 years) of the Canadian National Breast Screening Study, 21.9% of patients were overdiagnosed (i.e., 106 out of 44,925 healthy women were diagnosed with and treated for breast cancer unnecessarily). In addition, a Cochrane review of 10 trials involving more than 600,000 women revealed that mammography screening did not have an impact on the breast cancer death rate. However, according to a national survey, 71% of U.S. women still believe that mammograms reduce the risk of breast cancer by at least 50%, and 72.1% think that at least 80 deaths would be prevented per 1,000 women having mammography screening. However, available trials show only a relative risk reduction of 20% and a prevention of one breast cancer death per 1,000 women having mammography screening.18
Role of Pharmacists
Pharmacists can play an important role in breast cancer risk reduction, especially for women having increased risk. Since the use of tamoxifen and raloxifene for chemoprevention in eligible women is very low (only 0.2% of women took tamoxifen in 2000 and <15% for high-risk women),10,19 it is an opportunity for pharmacists to collaborate with medical teams and other healthcare professionals in educating women about the benefits of using medications to prevent breast cancer. Pharmacists can provide women with information on the benefits versus risks of chemo-prevention, medications used with appropriate dosage and indication, potential adverse effects, and drug interactions to ease their concerns and increase their confidence in their decision making in this matter. Women should also be provided with information about breast cancer risk factors, breast self-examinations, clinical breast examinations, and methods used for prevention of breast cancers in those with increased risk.
Through public and/or community outreach activities, pharmacists can convince a higher number of women with increased risk to use medications for breast cancer risk reduction effectively, thus contributing significantly to the prevention effort. Certainly, it is a real challenge for pharmacists, as this will require a significant effort involving money, time for planning, communication, advertising, and execution of breast cancer prevention campaigns.
REFERENCES
1. Breast cancer. American Cancer Society. January 31, 2014. www.cancer.org. Accessed February 23, 2014.2. Stopeck AT, Harris JE, Swart R, et al. Breast cancer risk factors. Medscape. August 19, 2013. http://emedicine.medscape.com/article/1945957-overview. Accessed February 23, 2014.
3. Miller KD. Prevention: stop cancer before it starts. Medscape. April 16, 2014. www.medscape.com/viewarticle/823572. Accessed February 23, 2014.
4. Moyer VA. Medications for risk reduction of primary breast cancer in women: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2013;159(10):698-708.
5. Chustecka Z. New guidelines on chemoprevention for breast cancer. Medscape. September 24, 2013. www.medscape.com/viewarticle/811553. Accessed February 23, 2014.
6. Brookes L, Visvanathan K. A pill a day to keep breast cancer away. Medscape. February 14, 2014. www.medscape.com/viewarticle/820541. Assessed February 23, 2014.
7. Thomsen A, Kolesar JM. Chemoprevention of breast cancer. Am J Health Syst Pharm. 2008;65(23):2221-2228.
8. Schapira L, Goss PE. Doc, should I take this pill or NOT? Medscape. February 20, 2014. www.medscape.com/viewarticle/820858. Accessed February 23, 2014.
9. Nelson HD, Smith ME, Griffin JC, Fu R. Use of medications to reduce risk for primary breast cancer: a systematic review for the U.S. Preventive Services Task Force. Ann Intern Med. 2013;158:604-614.
10. Mulcahy N. ASCO adds oomph to breast cancer chemoprevention guide. Medscape. July 8, 2013. www.medscape.com/viewarticle/807489. Accessed February 23, 2014.
11. Radmacher MD, Simon R. Estimation of tamoxifen’s efficacy for preventing the formation and growth of breast tumors. J Natl Cancer Inst. 2000;92(1):48-53.
12. Wax A. Tamoxifen for breast cancer treatment and prevention. WebMD. June 26, 2012. www.webmd.com/breast-cancer/tamoxifen-for-breast-cancer-treatment-and-prevention. Accessed February 23, 2014.
13. Johnson K. Anastrozole halves breast cancer in prevention study. Medscape. December 12, 2013. www.medscape.com/viewarticle/817775. Accessed February 23, 2014.
14. Miller G. Exemestane well-tolerated for breast cancer prevention. Medscape. April 18, 2014. www.medscape.com/viewarticle/823789. Accessed May 20, 2014.
15. Lexi-Drugs Online. Hudson, OH: Lexi-Comp, Inc. www.lexicom/lco/doc/retrieve/docid/patch. Accessed February 23, 2014.
16. Goetz MP, Schaid DJ, Wickenham DL, et al. Evaluation of CYP2D6 and efficacy of tamoxifen and raloxifen in women treated for breast cancer chemoprevention: results from the NSABP P-1 and P-2 clinical trials. Clin Cancer Res. 2011;17(21):6944-6951.
17. Screening for breast cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2009;151:716-726.
18. Biller-Andorno N, Jüni P. Abolishing mammography screening programs? A view from the Swiss Medical Board. N Eng J Med. 2014;370(21):1965-1967.
19. Chustecka Z. Tamoxifen not being used much for prevention of breast cancer. Medscape. February 8, 2010. www.medscape.com/viewarticle/716583. Accessed May 26, 2014.
To comment on this article, contact rdavidson@uspharmacist.com.





