US Pharm. 2020;45(2):8-12.
Known to be common among older adults, delirium is an often underrecognized and preventable acute clinical syndrome of cognition and attention. While delirium has the potential to cause serious adverse effects on function and quality of life, it is often fatal among older patients, as well as associated with substantial health care costs.1 In the United States, more than 2.6 million adults aged 65 years and older develop delirium each year and account for approximately $164 billion in annual healthcare expenditures.2
Currently, rather than considering delirium a primary disorder of arousal alone (i.e., a “mental status” problem), more sophisticated observations and advances in the field have brought forth the consideration of delirium as primarily a disorder of cognition, with impairment of attention and global cognition the typical features.3,4 It is challenging to distinguish an oversedated patient (i.e., unable to arouse) from a patient with delirium (i.e., with impairments in both cognition and arousal in many cases); however, this distinction is clinically relevant since delirium lasting 2 to 3 days or longer has been associated with poorer outcomes versus more transient episodes, which are often secondary to psychoactive medications.1,5
Delirium is difficult to distinguish from dementia. In general, delirium commonly presents with a sudden onset (e.g., hours to days), with an altered level of consciousness and clouded sensorium of relatively short duration; it usually reflects a toxic state that is acute and reversible.6 It is marked by disorganized thinking, with rambling, irrelevant, or incoherent speech; there may also be sensory misperceptions, disturbance of sleep-wake cycle and level of psychomotor activity; disorientation to time, place, and person; and memory impairment.7 In comparison, dementia more commonly presents gradually with a level of consciousness that is unimpaired.8
In alcohol-withdrawal delirium secondary to a reduction or cessation of alcohol consumption—typical in patients with a history of many years of heavy drinking—autonomic hyperactivity is characteristic (e.g., tachycardia, sweating, hypertension). Patients with alcohol-withdrawal delirium also pre-sent with a coarse, irregular tremor; delusions, vivid hallucinations, and wild, agitated behavior; and potentially, seizures.7
Delirium often occurs following an acute illness, surgery, or hospitalization.1 The etiology of postoperative delirium is multifactorial, resulting from a combination of patient risk factors at admission and perioperative insults.9 Many elderly patients present with depleted cholinergic reserves and respond abnormally to anticholinergic medications commonly used in the perioperative period and during general anesthesia.10 Postoperative delirium is easier to diagnose if there is a preoperative baseline.
Delirium Following Cardiac Surgery
Postoperative delirium is a common complication of cardiac surgery and is associated with increased mortality, morbidity, and long-term cognitive dysfunction.11 Delirium following cardiac surgery is estimated to have an incidence (using rigorous methodology) likely between 26% and 52%.12-15 Advanced age is a known predictor of delirium occurrence after cardiac surgery, and in the general population.16,17 Independent risk factors for the development of delirium following cardiac surgery are outlined in TABLE 1.
A recent study has found ICU stay, hospital stay, and intubation time were significantly longer in patients aged 65 years and older with delirium following cardiac surgery.11 Using the Diagnostic snd Statistical Manual of Mental Disorders, fifth edition (DSM-5), criteria for delirium (a gold standard diagnostic criteria in research studies; see RESOURCE and Reference 18), all patients were screened for the presence of delirium by ICU physicians, attending cardiac surgeons, and nurses during the postoperative course, with data regarding the first 5 days after the operation included in the analysis.11
With regard to postoperative outcome, both elderly and very elderly patients had longer hospital length of stay (LOS) if they developed postoperative delirium. The LOS in the cardiac surgery ICU was longer for elderly patients with delirium; intubation time was longer in patients older than age 65 years with delirium.11
Kotfis and colleagues analyzed 1,797 patients aged 65 years and older, including 230 (7.24%) patients aged 80 years and older. Delirium was diagnosed in 21.4% of patients older than age 65 years, and in 33.5% of octogenarians. Early mortality did not differ between patients with and without delirium. ICU stay, hospital stay, and intubation time were significantly longer in patients undergoing cardiac surgery who were aged 65 years and older and had delirium.11
Preoperatively, the most common comorbid conditions were hypertension, diabetes, congestive heart failure, and extracardiac arteriopathy. Compared with their counterparts without delirium, patients aged 65 years or more with delirium were older, more often diabetic, and more often presented with internal carotid artery stenosis, chronic renal failure, ejection fraction <30%, and extracardiac arteriopathy. There were no statistically significant differences between patients aged 80 years and older in groups with and without delirium.11
Kotfis and colleagues concluded that ICU delirium complicates the postoperative course of a significant number of elderly patients undergoing cardiac surgery.11 They found patients older than age 65 years who experience postoperative delirium have poorer outcomes and are more likely to have prolonged hospitalization, a prolonged ICU stay, and longer intubation times, but their 30-day mortality is not increased. The eight independent risk factors for development of postcardiac surgery delirium in elderly patients in their study are outlined in TABLE 1.
Delirium in the Critically Ill and ICU
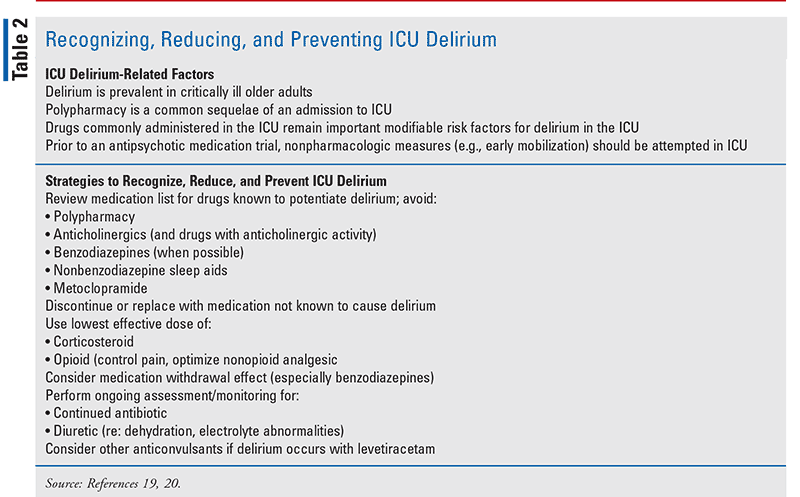
Delirium is prevalent in critically ill older adults, and medications continue to be an underappreciated risk for delirium in this population; many of these agents are commonly administered in the ICU.19 Data from Devlin and colleagues provide strategies to reduce medication-related delirium in the ICU (TABLE 2).20
Delirium at End of Life
Delirium is also common in hospice, in which 80% of terminally ill patients experience delirium in the last few days of life.21 In addition to the clouding of consciousness (inability to either maintain or shift attention) and impaired cognitive functioning (with or without memory disturbances), sundowning (daytime drowsiness and nighttime agitation and restlessness) is a common phenomenon at the end of life, especially in the presence of delirium.6
Potential causes of delirium in the hospice setting are outlined in TABLE 3 and include metabolic disturbances, sleep deprivation, uncontrolled pain, and adverse drug effects of a number of medications, including anticholinergic agents, benzodiazepines, opioids, corticosteroids, and tricyclic antidepressants. Notably, the administration of benzodiazepine monotherapy in a patient with delirium may exacerbate the delirium and confusion. However, while the addition of a benzodiazepine with antipsychotics is not routinely recommended, delirium induced by withdrawal or untreated anxiety may benefit from the addition of a benzodiazepine for symptom management in the terminally ill patient.22
With advances in the diagnosis of delirium, improvement in recognition and risk stratification can be achieved.1 While the prevention of delirium using nonpharmacologic approaches is documented to be effective, pharmacologic prevention and treatment of delirium remains controversial.1 Nonpharmacologic approaches focused on risk factors such as functional decline, immobility, visual or hearing impairment, dehydration, and sleep deprivation are effective for delirium prevention and are also recommended for delirium treatment.1 Based on recent evidence reviews, pharmacologic treatment of delirium involves reserving use of antipsychotics and other sedating medications for treatment of severe agitation that poses a risk to the safety of patient or staff or threatens the interruption of essential medical therapies.1 For further discussion on the evaluation and management of suspected delirium, see Reference 2. Delirium education may have to address both teaching of clinical skills and enhancing the ability to question stereotypes.23
Hospital Elder Life Program and Other Advocacy
Inouye and colleagues indicate that 20% to 30% of patients older than age 70 years who have undergone major surgery will experience subsequent delirium with long-term cognitive decline; these individuals will have an increased risk for developing Alzheimer’s disease or dementia subsequently.2,24 Currently, over 200 hospitals have introduced a program called the Hospital Elder Life Program that incorporates measures after surgery such as making patients move as soon as possible, giving them their glasses and hearing aids soon after surgery, and encouraging proper sleep without the use of sedative hypnotics. Another advocacy group is planning to begin a “prehab” program with recommendations for preparing for surgery which may include measures associated with exercise, healthy diet, hydration, and evaluating medications and supplements; caregiver guidance on providing assistance during the perioperative period—before, during and after surgery—is also planned by some.24 Furthermore, experts indicate that keeping exposure to anesthesia as short as possible and reducing the number of psychoactive drugs used can be helpful.2,24
Conclusion
Delirium, a common and acute disorder of cognition and attention, is often fatal among older adults. Although often underrecognized or confused with dementia, pharmacists can contribute to the identification of conditions that may increase risk, and drugs that may potentiate delirium, in order to decrease the risk of serious adverse effects on a patient’s function and quality of life and reduce healthcare costs.
REFERENCES
1. Oh ES, Fong TG, Hshieh TT, et al. Delirium in older persons: advances in diagnosis and treatment. JAMA. 2017; 318(12):1161-1174.
2. Inouye SK, Westendorp RG, Saczynski JS. Delirium in elderly people. Lancet. 2014;383(9920):911-922.
3. Inouye SK, van Dyck CH, Alessi CA, et al. Clarifying confusion: the confusion assessment method: a new method for detection of delirium. Ann Intern Med. 1990;113(12):941-948.
4. Cunningham C. Systemic inflammation and delirium: important co-factors in the progression of dementia. Biochem Soc Trans. 2011:39(4):945-953.
5. Chedru F, Geschwind N. Disorders of higher cortical functions in acute confusional states. Cortex. 1972;8(4):395-411.
6. Kroustos KR, Sweeney MA. Palliative care. In: Chisholm-Burns MA, Schwinghammer TL, Malone PM, et al, eds. Pharmacotherapy: Principles & Practice, 5th ed. New York, NY: McGraw Hill Education; 2019:31-42.
7. Dorlands Illustrated Medical Dictionary, 32nd ed. Philadelphia, PA: Elsevier Saunders; 2012.
8. Bush SH, Leonard MM, Agar M, et al. End-of-life delirium: issues regarding recognition, optimal management, and the role of sedation in the dying phase. J Pain Symptom Manage. 2014;48(2):215-230.
9. Inouye SK, Charpentier PA. Precipitating factors for delirium in hospitalized elderly persons. Predictive model and interrelationship with baseline vulnerability. JAMA. 1996;275:852-857.
10. Rudolph J, Ramlawi B, Kuchel G, et al. Chemokines are associated with delirium after cardiac surgery. J Gerontol A Biol Sci Med Sci. 2008;63:184-189.
11. Kotfis K, Szylinska A, Listewnik M, et al. Early delirium after cardiac surgery: an analysis of incidence and risk factors in elderly (≥65 years) and very elderly (≥80 years) patients. Clin Interv Aging. 2018;13:1061-1070.
12. Rudolph JL, Inouye SK, Jones RN, et al. Delirium: an independent predictor of functional decline after cardiac surgery. J Am Geriatr Soc. 2010;58:643-649.
13. Rudolph JL, Jones RN, Levkoff SE, et al. Derivation and validation of a preoperative prediction rule for delirium after cardiac surgery. Circulation. 2009;119(2):229-236.
14. Schoen J, Meyerrose J, Paarmann H, et al. Preoperative regional
cerebral oxygen saturation is a predictor of postoperative delirium in
on-pump cardiac surgery patients: a prospective observational trial. Crit Care. 2011;15(5):R218.
15. Plaschke K, Fichtenkamm P, Schramm C, et al. Early postoperative delirium after open-heart cardiac surgery is associated with decreased bispectral EEG and increased cortisol and interleukin-6. Intensive Care Med. 2010;36(12):2081-2089.
16. Tan M, Felde A, Kuskowski M, et al. Incidence and predictors of post-cardiotomy delirium. Am J Geriatr Psychiatry. 2008;16:575-583.
17. Koster S, Hensens AG, van der Palen J. The long-term cognitive and functional outcomes of postoperative delirium after cardiac surgery. Ann Thorac Surg. 2009;87:1469-1474.
18. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-5. 5th ed. Arlington, VA: American Psychiatric Association; 2013.
19. Garpestad E, Devlin JW. Polypharmacy and delirium in critically ill older adults: recognition and prevention. In: Zagaria MA, ed. Polypharmacy. Clin Geriatr Med. 2017;33(2):189-203.
20. Devlin JW, Fraser GL, Riker RR. Drug-induced coma and delirium. In: Papadopoulos J, Cooper B, Kane-Gill S, et al, editors. Drug-Induced Complications in the Critically Ill Patient: a Guide For Recognition and Treatment. Chicago: Society of Critical Care Medicine. 2011:107-116.
21. Temel JS, Greer JA, Muzikansky A, et al. Early palliative care for patients with metastatic non-small-cell lung cancer. N Engl J Med. 2010;36(8):733-742.
22. Bush SH, Kanji S, Pereira JL, et al. Treating an established episode of delirium in palliative care: expert opinion and review of the current evidence base with recommendations for future development. J Pain Symptom Manage. 2014;48(2):231-248.
23. Eeles E, Bhat RS. Delirium. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:903-908.
24. Reddy S. The surgical complication that can damage your brain. The Wall Street Journal. Updated Dec. 9, 2019. www.wsj.com/articles/the-surgical-complication-that-can-damage-your-brain-11575916977. Accessed January 13, 2020.
25. Protus BM, Kimbrel J, Grauer P. Palliative Care Consultant: a Reference Guide for Palliative Care. 4th ed. Hospiscript Services, a Catamaran Company, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.