US Pharm. 2011;36(9)(Oncology suppl):3-7.
ABSTRACT: The choice of treatment for head and neck cancer usually depends on the origin and stage. The majority of patients undergo radiation therapy or surgery, or a combination of both, and caring for individuals undergoing radiotherapy involves multifaceted management. Counseling patients before, during, and after head and neck radiotherapy is important to help them become aware of several oral complications that may be severe and may interfere with everyday living. The pharmacist's role is to help lessen oral discomfort and morbidity in this population.
The three major types of treatment for managing head and neck cancer are radiation therapy, surgery, and chemotherapy.1 The majority of patients undergo radiation therapy or surgery, or a combination of both. Chemotherapy is usually used as a supplement to the above treatments. Combining chemotherapy and radiotherapy does not improve long-term survival rates over those achieved by radiotherapy and surgery.1 The choice of treatment usually depends on the origin and stage of the head and neck cancer. Approximately 50,000 new head and neck cancers are diagnosed annually in the United States, and there are about 350,000 deaths yearly worldwide.2-4Most head and neck cancer starts in the squamous cells of the mucosal tissue that lines the head and neck region, such as the tonsils and tongue. Squamous cell carcinoma represents more than 90% of all head and neck cancers.5 Head and neck cancer can occur anywhere in the head and neck region, and radiation therapy to this area usually results in numerous oral adverse effects that require additional palliative treatment to alleviate these troublesome symptoms.
Radiation Treatment
Radiation therapy, or radiotherapy, is effective in killing tumor cells through nonsurgical methods. High doses of ionizing radiation are aimed directly at the actively dividing tumor cells and are confined to this area as much as possible without going outside the tumor zone. Of major concern is the effect of radiation on normal cells. Since the cells in the oral cavity are also dividing, they too are affected, resulting in the inability of these cells to reproduce and repair damaged tissue. By using a moderate dose of radiation for short periods of time, there is a greater chance of tumor shrinkage with fewer incidences of adverse effects. Management is comprised of about 10 treatments over 2 weeks depending on the type and stage of the cancer. It can take up to 2 to 4 weeks for recuperation; however, many adverse effects from radiation can persist. The major tissues/organs affected by radiation to the head and neck region are the salivary glands, mucous membranes in the oral cavity, taste buds, and bone and teeth.6 Destruction of the tissues/organs results in many oral adverse effects (TABLE 1).

Oral Complications of Head and Neck Radiotherapy
Xerostomia: Ionizing radiation causes normal salivary gland tissue damage, resulting in rapid loss of salivary fluid function.9,10 The salivary glands are especially sensitive to radiation and show acute and chronic responses to radiotherapy.8 Of all of the salivary glands, the parotid gland is mainly affected because the serous cells are most sensitive.11 With a loss of saliva secretion, oral dryness, or xerostomia, is the chief symptom.12 Xerostomia, the most common complication of radiotherapy, occurs due to suppression of salivary function and is usually irreversible because of irreparable damage to the salivary glands (doses greater than 25 Gy).13 If it is temporary, as seen in patients who have received low-dose radiation (less than 25 Gy), treatment is usually palliative with no permanent changes to the oral tissues and complete recovery of salivary function in 12 to 24 months.13,14 The patient can become uncomfortable because there is no salivary lubrication and the mucosal tissues become sticky. Individuals often complain of difficulty in swallowing (dysphagia), food sticking to the teeth, and a burning sensation when eating spicy food and fruit.12 As a result, there may be changes in eating patterns with a decrease in nutritional intake and weight loss. Dry mucosa may also be more prone to bleeding, resulting in bleeding gums. Due to the reduction of salivary flow, there is also an increased incidence of candidiasis, tooth/root decay (caries), and periodontal disease (e.g., gingivitis, periodontitis).13 There is usually a 50% to 60% loss of salivary flow within the first week of radiotherapy.13 Chronically, there is a significant decrease in salivary flow for several months or years following radiotherapy.14
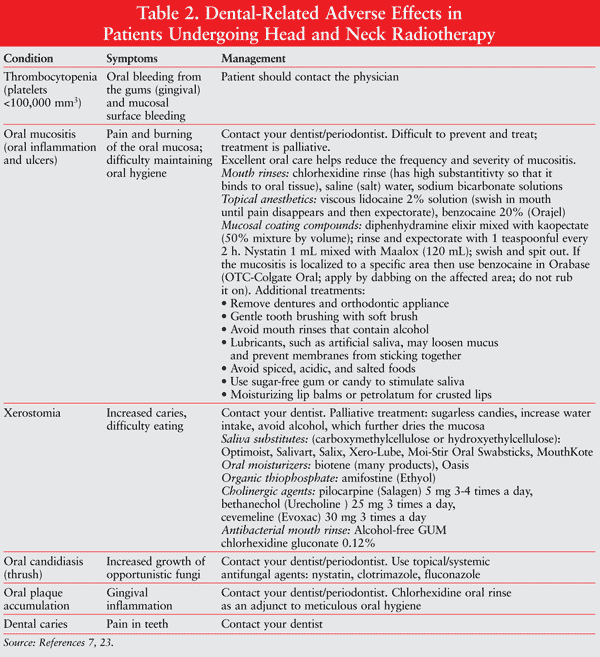
Management of xerostomia involves meticulous oral home care, use of salivary substitutes, and artificial saliva substitutes (TABLE 2).13,15 Since these products do not replace the antibacterial and immunologic properties of saliva, an antibacterial alcohol-free mouth rinse such as GUM chlorhexidine gluconate is recommended. An alcohol-free mouth rinse is recommended because the alcohol can be irritating and dehydrating to the oral mucosa. Sialogogic, cholinergic agents are used to stimulate saliva production from whatever salivary gland tissue remains. Pilocarpine, a muscarinic-cholinergic agonist, is a naturally occurring plant alkaloid that stimulates salivation. Cevimeline induces salivary function with minimal cardiac and pulmonary effects because it has a high affinity for the M3 muscarinic receptors on salivary glands. Bethanechol (Urecholine) is another cholinergic drug.16 Amifostine (Ethyol), an organic thiophosphate chemoprotectant agent, is FDA approved to reduce the incidence of moderate-to-severe xerostomia in patients undergoing postoperative radiation treatment for head and neck cancer. It is recommended for late xerostomia occurring at least 1 year after radiation. At this time there is most likely permanent fibrosis of the salivary glands.17
Oral Mucositis: Mucositis, or oral inflammation, is a common, life-threatening acute adverse effect due to early changes in the oral mucosal tissue, which is extremely sensitive to radiation doses.18 The development of mucositis depends on the dose of radiation, angulation of the beam, location of the tumor, and the degree of oral hygiene.6 Oral mucositis can occur anywhere there is oral mucosa including the oral cavity, esophagus, larynx, and pharynx. Clinically, the oral tissues appear to be red due to epithelial thinning and vasodilation. This can lead to ulcerations or mouth sores, sloughing of the epithelium, and crusting of the lips. Oral mucositis causes severe pain and increases the risk for the development of systemic infection from bacterial, fungal, or viral infections in the mouth.19 Common sites of oral cavity mucositis include the buccal, labial, and soft palate mucosa along with the ventral surface of the tongue and floor of the mouth. If the pharynx is involved, the individual may have a sore throat and difficulties in swallowing and talking. Esophagitis is caused by damage to the mucosal lining and usually presents as dysphagia. A majority of individuals present with mucositis within the first 3 weeks of radiotherapy.7 It peaks at Week 5 and can persist for weeks following the end of therapy.20
Prevention may be the most important factor in the development of oral mucositis; however, it is difficult to prevent as well as treat. Fortunately, it is not permanent. Patients usually also have xerostomia. Maintenance of excellent oral care before and during radiation treatment is important to help reduce the frequency and severity of oral mucositis.21 Ill-fitting dentures can worsen the situation. It usually resolves about 4 weeks after completion of therapy. Refer to TABLE 2 for management of oral mucositis. Clinical studies have not shown any beneficial effects of using chlorhexidine in the treatment of mucositis.7
Fungal/Bacterial/Viral Infections: Due to changes in the saliva, which has antibacterial properties, there are alterations in oral microflora resulting in bacterial and fungal infections. Oral candidiasis (thrush) is common due to an overgrowth of fungi. It is usually found at the corners of the mouth, oropharynx, lateral and posterior boarders of the tongue, and under dentures. It may be more important to prevent rather than treat oral candidiasis.
There are high levels of bacteria such as Lactobacillus species and Streptococcus mutans that cause rampant tooth decay. As discussed earlier, this increased level of cariogenic bacteria is most likely due to the reduced salivary flow (xerostomia).6 For prevention of caries, the patient should be placed on a neutral sodium fluoride rinse such as Prevident rinse or an acidulated phosphate rinse such as Phos-Flur. Chlorhexidine gluconate is a strong antimicrobial oral rinse that is helpful to reduce bacterial levels and help with oral hygiene. Chlorhexidine has high substantivity, which allows it to bind to oral tissues and slowly release over 24 hours in its active form.
Viral infections are often seen in irradiated, immunocompromised patients as oral ulcerations caused by reactivation of latent herpes simplex virus.
Taste Changes: Papillae, which contain taste buds, are present on the tongue, tonsillar pillar, soft palate, laryngeal surface of the epiglottis, and posterior pharyngeal wall.6 It is thought that the loss of taste is due to xerostomia; taste is usually restored 2 to 4 months postradiotherapy.22 Patients lose the ability to differentiate between sweet and salty foods and are also at increased risk for tooth/root caries.Teeth: Generally, the exact effect of radiation on teeth is not known.6 It has been reported that radiation to the head and neck region can cause an increased sensitivity of teeth due to external stimuli.20
Trismus: Another adverse effect of radiotherapy is limited ability to open the jaw or trismus due to fibrosis around the muscles of mastication.7
Alveolar Bone: The bone of the jaw is kept vital by an adequate blood supply. Radiation causes the vascular channels in the bone to narrow, reducing the blood supply.6 This renders the alveolar bone around the teeth and jaw nonvital (no blood supply) and subject to becoming necrotic when traumatized and exposed because it cannot repair itself. This results in a condition called osteoradionecrosis, which usually occurs in the mandible because of poor blood supply and increased bone density.7 Clinical symptoms include infection, swelling, drainage, and pain due to exposed necrotic bone. Any type of trauma to the mandible including dentures with rough edges, tooth extractions, and periodontal surgery can cause osteoradionecrosis in the irradiated individual. It is commonly seen in patients who receive more than 60 Gy of radiation therapy administered to the mandible. Thus, it is important for an individual to have any type of dental procedure performed before radiotherapy begins. There are various treatments for osteoradionecrosis, but it is extremely difficult to treat because it is irreversible. Various treatments include hyperbaric oxygen therapy (raises tissue oxygen levels, which can speed up the healing process), analgesics, and systemic antibiotics; in more advanced cases or when treatments are not effective, surgery is required to remove the necrotic bone. Prevention is the key to avoiding osteoradionecrosis.20
Dental Treatment Before Radiation Therapy
Before an individual starts radiation therapy, a preventive oral health exam should be performed that will identify oral conditions such as mouth sores or infections, tooth decay, gum (periodontal) disease, ill-fitting dentures, infected teeth that require root canal treatment, and salivary gland dysfunction that should be treated before radiotherapy begins. Any extractions and periodontal surgery should be done before radiotherapy. Preferably, extractions for patients undergoing radiation therapy should be performed about 3 weeks before the initiation of therapy, with the minimum being 14 days.21
Starting a routine for oral home care is important before the patient undergoes radiotherapy. An ultrasoft- or soft-bristled toothbrush should be used to avoid soft tissue trauma. A nonabrasive fluoride toothpaste or gel is recommended. An antimicrobial mouth rinse such as chlorhexidine gluconate should be used about 30 minutes after brushing.
Treatment of Oral Complications During and After Radiation Therapy
Routine oral care that was introduced to the patient before radiation therapy should be continued during and after therapy. Individuals should be monitored during radiotherapy. Maintaining low dental plaque levels and oral inflammation can reduce complications such as decay, mouth sores, and infections.
Oral care after radiation therapy consists of the following: using a soft- or ultrasoft-bristled toothbrush or a foam toothbrush or foam oral swab such as Toothettes; using hot water on the bristles immediately before and during brushing will make the bristles even softer and less traumatic to the oral tissues; and brushing at least two to three times a day and after eating. A nonabrasive, unflavored, fluoride-containing toothpaste is recommended. Flossing is important, but may be traumatic to the soft tissues. It is also important to keep lips moist with a moisturizing lip balm. In addition, an antibacterial rinse is recommend; if possible, the patient should use a rinse that does not contain alcohol, which could dry the oral tissues. One example of a nonalcohol rinse is GUM chlorhexidine, and some OTC alcohol-free rinses include Listerine Zero, Crest Pro-Health Complete, Oral-B, and Rembrandt. Finally, patients should remove dentures at night, clean them with a denture brush, and soak them in a cleanser consisting of 8 oz. of water mixed with 1 teaspoon of salt and 1 teaspoon of baking soda.
Conclusion
Caring for individuals undergoing radiation therapy for head and neck cancer involves multifaceted management by many health care professionals such as the head and neck surgeon, radiologist, radiation oncologist, medical oncologist, plastic/reconstructive surgeon, dentist, pharmacist, nurse, nutritionist, and speech therapist. Counseling patients before, during, and after head and neck radiotherapy is important to help them become aware of several oral complications that may be severe and may interfere with everyday living. Introducing good oral home care and more frequent oral prophylaxis visits to the dentist before radiotherapy begins will allow for continuing care during and after therapy. There are several prescription and OTC products that will most likely be used by these patients. The pharmacist's role in the management of the irradiated individual is to help lessen oral discomfort and morbidity stemming from complications of head and neck radiotherapy.
REFERENCES
1. PS Akhtar. Palliative radiotherapy in head and neck cancer. JAFMC Bangladesh. 2010; 6(1):2-3.
2. St John MA, Abemayor E, Wong DT. Recent new approaches to the treatment of head and neck cancer. Anticancer Drugs. 206;17(4):365-375.
3. Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics, 2002. CA Cancer J Clin.
4. Cognetti DM, Weber RS, Lai SY. Head and neck cancer: an evolving treatment paradigm. Cancer. 2008;113(7 suppl):1911-1932.
5. Ridge JA, Glisson BS, Lango MN, et al. Head and neck tumors. In: Pazdur R, Wagman LD, Camphausen KA, Hoskins WJ, eds. Cancer Management: A Multidisiplianary Approach. 11th ed. New York, NY: CMP United Business Media; 2008.
6. Andrews N, Griffiths C. Dental complications of head and neck radiotherapy: part 1. Aust Dent J.
7. Hancock PJ, Epstein JB, Sadler GR. Oral and dental management related to radiation therapy for head and neck cancer. J Can Dent Assoc. 2003;69(9):585-590.
8. Grundmann O, Mitchell GC, Limesand KH. Sensitivity of salivary glands to radiation: from animal models to therapies. J Dent Res. 2009;88(10):894-903.
9. Mossman KL. Quantitative radiation dose-response relationships for normal tissues in man. II. Response of the salivary glands during radiotherapy. Radiat Res. 1983;95:392-298.
10. Brennan NT, Elting LS, Spijkervat RK. Systematic reviews of oral complications from cancer therapies, Oral Care Study Group, MASCC/ISOO: methodology, and quality of the literature.
Support Care Cancer. 2010;18:979-984.
11. Wolff A, Atkinson JC, Macynski AA, Fox PC. Pretherapy interventions to modify salivary dysfunction. NCI Monographs. 1990;9:87-90.
12. Garg AK, Malo M. Manifestations and treatment of xerostomia and associated oral effects secondary to head and neck radiation therapy. JADA. 1997;128:1128-1133.
13. Dirix P, Nuyts S, Van den Bogaert W. Radiation-induced xerostomia in patients with head and neck cancer: a literature review. Cancer. 2006;107(11):2525-2534.
14. Li Y, Taylor JM, Ten Haken RK, Eisbruh A. The impact of dose on parotid salivary recovery in head and neck cancer patients treated with radiation therapy. Int J Radiat Oncol Biol Phys.
15. American Dental Association. Do you have dry mouth? 2002;133:1455.
16. Friedman PK, Isfeld D. Tips for treating xerostomia. Dimens Dent Hyg. 2011;9(1):50,52-53.
17. American Society of Clinical Oncology Clinical Practice Guideline for the Use of Chemotherapy and Radiotherapy Protectans. J Clin Oncol. 1999;17(10):3333-3355.
18. Silverman S, Jr. Diagnosis and management of oral mucositis. J Supp Oncol. 2007;5:13-21.
19. Ankaya H, Güneri P. Importance of a dental approach in head and neck cancer therapy. APJOH.
20. Ballantyne JC, Fishman SM, Rathmell JP. Bonica's Management of Pain. Lippincott, Williams & Wilkins; 2009:621-629.
21. Andrews N, Grittiths C. Dental complications of head and neck radiotherapy: part 2. Aust Dent J.
22. Conger AD. Loss and recovery of taste acuity in patients irradiated to the oral cavity. Rad Res.
23. Barry JM. The dentist's role in managing oral complications of cancer. Dent Today. 2005;24(8):58-61.
To comment on this article, contact rdavidson@uspharmacist.com.





