US Pharm. 2016;41(3):8-15.
Diabetes is one of the most common medical conditions globally. In the United States, the prevalence of diabetes has been steadily increasing; from 1980 to 2014 the number of Americans diagnosed increased fourfold, from 5.5 million to 22 million.1 It is estimated that 1 in 3 adult Americans will have diabetes by 2050.2 If left untreated or poorly controlled, diabetes can lead to significant morbidity and mortality, mostly attributed to the associated long-term microvascular and macrovascular complications.
Neuropathies are a common long-term complication of diabetes, affecting up to 50% of all patients with diabetes.3 Diabetic sensorimotor polyneuropathy is one type of neuropathy described as a diffuse symmetrical and length-dependent injury to peripheral nerve fibers.4 This condition, most often referred to as diabetic peripheral neuropathy (DPN), is the most common diabetic neuropathy, accounting for up to 75% of cases.3,5,6 It is defined as “the presence of symptoms and/or signs of peripheral nerve dysfunction in people with diabetes after the exclusion of other causes.” DPN causes pain or loss of feeling in the toes, feet, legs, hands, and arms. It is the leading cause of lower-extremity amputations, accounting for approximately 60% of nontraumatic lower-limb amputations.1,7
Etiology
The exact mechanism for the development of diabetic neuropathies is not fully understood; however, studies have demonstrated that various metabolic changes and vascular factors are involved in all stages of DPN.8 Impaired blood flow and endoneurial hypoxia play a major role in the development of DPN.8 Metabolic changes, such as hyperglycemia and dyslipidemia, contribute to reduced nerve perfusion.
Hyperglycemia is the major risk factor for the development of DPN. Additional risk factors include older age, male sex, hypertension, duration of diabetes, dyslipidemia, alcohol consumption, smoking, and height.9-14
Clinical Manifestation
Most patients with chronic DPN will be asymptomatic, with 10% to 20% of patients experiencing troublesome symptoms that will require intervention.3 The onset of DPN is usually insidious and typically presents as a painless loss or change of sensation detected by clinical tests; almost 10% of patients newly diagnosed with type 2 diabetes will present with DPN at time of diagnosis.3,15 Patients will typically experience numbness, tingling, pain, and/or weakness. These symptoms begin in the lower limbs symmetrically and may eventually spread to the fingers and hands in more severe cases, described as a “stocking-glove” distribution.3,16
Sensory symptomatology appears to be more prominent than motor involvement, although unsteadiness is increasingly being recognized as a manifestation of chronic DPN, most likely due to numbness and abnormal muscle sensory function.3,16 This unsteadiness leads to balance problems, increasing the risk of falls. Neuropathy has been identified as one of the three main risk factors for falls in patients with diabetes; diabetic patients with DPN are three times more likely to fall than those with no evidence of neuropathy.17
Neuropathic pain is probably the most debilitating symptom, greatly affecting quality of life. It is frequently unreported and more frequently untreated.4 This pain is characterized by burning, electric, and stabbing sensations with or without numbness.16 Patients can develop allodynia and hyperalgesia, which can significantly affect daily activities.16 The pain usually worsens at night, causing sleep disturbances.18
Clinical Management
Management of DPN can be classified into two strategies: treating the underlying cause and targeting the relief of symptoms. The former is more challenging because the only known method for treating the underlying cause is tight glycemic control. The Diabetes Control and Complications Trial (DCCT) demonstrated that tight glycemic control in type 1 diabetes patients reduced the incidence of neuropathy by approximately 69% over a 5-year period in those patients who did not have neuropathy at baseline, and this effect was reconfirmed 16 years later.19,20 The effect of glycemic control in patients with type 2 diabetes is not as clear; studies demonstrated a small reduction in the development of neuropathy with intensive treatment but these results were not statistically significant.21 However, the United Kingdom Prospective Diabetes Study (UKPDS) did demonstrate a statistically significant reduction in the development of DPN with intensive treatment, but only after 15 years.14 Despite these findings, controlling as well as stabilizing blood glucose levels will help lessen the severity of DPN and prevent further neurologic damage in both type 1 and type 2 diabetes.22
Many patients will require pharmacologic intervention for the management of pain symptoms. There are various treatment options available, but many of them have adverse effects or limited evidence regarding their effectiveness. The American Academy of Neurology (AAN) released guidelines in 2011 identifying agents that may have some benefit in managing painful DPN.23 Pharmacologic agents that were recommended include anticonvulsants, antidepressants, and opioids (TABLE 1).23
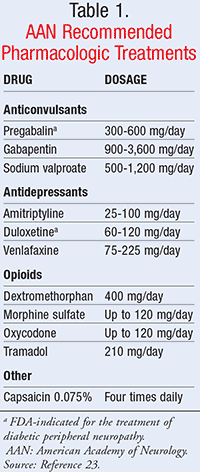
Anticonvulsants: These agents have been used in the management of DPN for years. Pregabalin is the only agent that is recommended by the AAN as first-line treatment; its use is associated with up to a 50% decrease in pain associated with DPN.23 Gabapentin and sodium valproate are recommended as second-line agents. These medications are associated with somnolence, especially pregabalin and gabapentin. Slow titration of these two agents may reduce the incidence. Sodium valproate is teratogenic and should be avoided in pregnant women.23
Antidepressants: There are three classes of antidepressants that are most commonly used to relieve painful DPN—tricyclic antidepressants (TCAs), selective serotonin reuptake inhibitors (SSRIs), and serotonin-norepinephrine reuptake inhibitors (SNRIs). For years, the TCAs have been considered first-line treatment options for painful DPN; however, because of their adverse-effect profiles and the introduction of pregabalin onto the market, they are now considered second-line therapy.23 The severity of their adverse effects is associated with their affinity for muscarinic, histaminic, and alpha-adrenergic receptors. The common adverse effects are therefore anticholinergic in nature and include constipation, dry mouth, blurred vision, urinary retention, and postural hypotension. They should be used with caution, especially in geriatric patients and in patients with glaucoma, benign prostatic hypertrophy, orthostasis, urinary retention, and thyroid disease.
The SNRIs and SSRIs offer another option for DPN pain relief. They are better tolerated and have fewer associated adverse effects. Duloxetine and venlafaxine are both SNRIs that have displayed effectiveness in relieving pain associated with DPN. Duloxetine was the first FDA-approved agent indicated for the treatment of painful DPN. The most common adverse effect is nausea, which can be reduced by slowly titrating the dose.24 Cardiac abnormalities, including blood pressure increases, have been associated with the use of venlafaxine; it should be used with caution in patients with cardiac disease.24 Although SSRIs have been used to treat painful DPN, there are limited data to support their use.3,23,25
Opioids: Opioids and opioid-related agents should be reserved for patients who have not responded to other treatment options. They have a high abuse potential, which limits their use. Dextromethorphan, morphine, tramadol, and oxycodone have all shown some effectiveness in relieving pain associated with DPN.23 Adverse effects commonly associated with their use include sedation, nausea, and constipation; their use can also lead to rebound headaches.23
Capsaicin: Capsaicin, available as an OTC topical cream, has demonstrated up to a 40% improvement in pain symptoms when compared to placebo.26 One study has shown capsaicin application to be equally as effective as amitriptyline for relief of painful DPN.27 It is recommended to be applied three to four times a day. Patients should wear gloves when applying it and wash their hands immediately after application. Although several trials have shown capsaicin to be somewhat effective, its use should be reserved for patients with localized discomfort rather than recommended to those with a more generalized, widespread neuropathic pain.28
Role of the Pharmacist
The loss of sensation in the lower limbs can lead to foot ulcerations and other serious injuries due to unintentional puncture or friction wounds. Patients who have loss sensitivity in their hands cannot sense temperature, leaving them at an increased risk for burns. Pharmacists are most often the healthcare professional patients will encounter initially to inquire about treatment options regarding these issues. It is important for pharmacists to provide education on appropriate foot care as well as the importance of regular foot examinations (TABLE 2).29

In addition, pharmacists should stress the importance of regular exercise. Not only will this help improve glucose control, reduce low-density lipoprotein (LDL) levels, and lower blood pressure, but regular aerobic exercise has been shown to prevent the progression, or even the onset, of DPN.30 Individuals who spent as little as 4 hours per week performing mild-intensity aerobic exercise had a lower incidence of developing motor and sensory neuropathies compared to those who did not exercise.30 Routine aerobic exercise can improve a patient’s quality of life.31 When it is combined with strength training, significant reductions in pain and neuropathic symptoms are observed.32
Conclusion
DPN is one of the most common complications of diabetes, which is often asymptomatic. Pharmacists can help patients decrease their risk of developing DPN or prevent the progression of the disease by helping them understand more about this condition and explaining the importance of proper foot care and routine foot examinations.
PATIENT INFORMATION
Causes and Risk Factors
Patients with uncontrolled diabetes generally have elevated blood glucose, which can cause nerve damage and lead to DPN. There are also a variety of other factors that may contribute to worsening DPN, including duration of diabetes, alcohol consumption, smoking, high cholesterol, hypertension, and older age.
Signs and Symptoms
When diagnosed with diabetes, you may initially appear asymptomatic, but it is imperative that you check for signs and symptoms of DPN. These may include pain, tingling, “pins and needles,” burning, numbness, sensitivity to light touch, muscle weakness, sharp pains, and issues with balance and reflexes, particularly affecting the feet and legs. These symptoms are often worse during moments of rest, such as at bedtime, and may improve with activity and exercise.
Complications
DPN can lead to a loss of sensation in your extremities, including the inability to sense pain or hot and cold temperatures. When this occurs, unintentional injury to your feet, including cuts, scrapes, bruises, splinters, burns, and ingrown toenails, may go unnoticed. That can lead to foot ulcers, infections, and muscle, bone, and joint disease. Muscles, bones, and joints may break down, leading to strength imbalance within different regions of your feet, which may ultimately cause foot deformities. Long-standing ulcers and infections may not heal, even with antibiotics. If infected ulcers do not heal, the affected region must be amputated to prevent the infection from spreading to the rest of your body.
Treatment and Prevention
Unfortunately, there is no known cure for DPN, although various approaches to treat the disease exist. Treatment of DPN generally focuses on slowing or preventing its progression by optimizing blood glucose control, actively caring for your feet, managing any complications, and alleviating pain.
It is imperative that you actively care for your feet on a daily basis, as this can prevent many complications associated with DPN.
- Gently clean your feet daily using lukewarm water and mild soap.
- Pat your feet to dry them, and immediately apply moisturizer.
- Inspect your feet for dry skin, breaks or wounds, calluses, and signs of infection.
- Avoid activities that may injure your feet, including walking barefoot and exposing your feet to hot temperatures.
- When wearing socks, choose cotton ones that fit loosely and change them daily.
- When wearing shoes, ensure that they are not too tight.
- When trimming your toenails, be careful not to cut the cuticles, and file the nails to remove any sharp edges.
- Have your feet comprehensively examined by a podiatrist at least once a year.
When to Seek Medical Attention
It is important to seek medical attention if you experience worsening symptoms of DPN or any complications of diabetes. This includes a cut that does not heal or appears infected; severe symptoms of burning, tingling, pain, or weakness that affect your daily activities; or indications of worsening diabetes, including constant lightheadedness or variations in digestion, urination, or sexual function.
REFERENCES
1. CDC. Number (in millions) of civilian, non-institutionalized persons with diagnosed diabetes, United States, 1980-2014. December 1, 2015. www.cdc.gov/diabetes/statistics/prev/national/figpersons.htm. Accessed January 25, 2016.
2. CDC. Number of Americans with diabetes projected to double or triple by 2050. October 22, 2010. www.cdc.gov/media/pressrel/2010/r101022.html. Accessed January 25, 2016
3. Boulton AJ. Management of diabetic peripheral neuropathy. Clin Diabetes. 2005;23(1):9-15.
4. Bril V, England J, Franklin GM, et al. Evidence-based guideline: treatment of painful diabetic neuropathy. Neurology. 2011;76(20):1758-1765.
5. Boulton AJ, Gries FA, Jervell JA. Guidelines for the diagnosis and outpatient management of diabetic peripheral neuropathy. Diabet Med J Br Diabet Assoc. 1998;15(6):508-514.
6. Smith HS, Argoff CE. Pharmacological treatment of diabetic neuropathic pain. Drugs. 2011;71(5):557-589.
7. Moxey PW, Gogalniceanu P, Hinchliffe RJ, et al. Lower extremity amputations—a review of global variability in incidence. Diabet Med. 2011;28(10): 1144-1153.
8. Cameron NE, Eaton SE, Cotter MA, Tesfaye S. Vascular factors and metabolic interactions in the pathogenesis of diabetic neuropathy. Diabetologia. 2001;44(11):1973-1988.
9. Clair C, Cohen MJ, Eichler F, et al. The effect of cigarette smoking on diabetic peripheral neuropathy: a systematic review and meta-analysis. J Gen Intern Med. 2015;30(8):1193-1203.
10. Adler AI, Boyko EJ, Ahroni JH, Stensel V, et al. Risk factors for diabetic peripheral sensory neuropathy: results of the Seattle Prospective Diabetic Foot Study. Diabetes Care. 1997;20(7):1162-1167.
11. Forrest KY, Maser RE, Pambianco G, et al. Hypertension as a risk factor for diabetic neuropathy: a prospective study. Diabetes. 1997;46(4):665-670.
12. Cheng YJ, Gregg EW, Kahn HS, et al. Peripheral insensate neuropathy—a tall problem for US adults? Am J Epidemiol. 2006;164(9):873-880.
13. Wiggin TD, Sullivan KA, Pop-Busui R, et al. Elevated triglycerides correlate with progression of diabetic neuropathy. Diabetes. 2009;58(7):1634-1640.
14. UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352(9131):837-853.
15. Duby JJ, Campbell RK, Setter SM, et al. Diabetic neuropathy: an intensive review. Am J Health Syst Pharm. 2004;61(2):160-173.
16. Callaghan BC, Cheng H, Stables CL, et al. Diabetic neuropathy: clinical manifestations and current treatments. Lancet Neurol. 2012;11(6):521-534.
17. Agrawal Y, Carey JP, Della Santina CC, et al. Diabetes, vestibular dysfunction, and falls: analyses from the National Health and Nutrition Examination Survey. Otol Neurotol. 2010;31(9):1445-1450.
18. Quattrini C, Tesfaye S. Understanding the impact of painful diabetic neuropathy. Diabetes Metab Res Rev. 2003;19(suppl 1):S2-S8.
19. The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329(14):977-986.
20. lbers JW, Herman WH, Pop-Busui R, et al. Effect of prior intensive insulin treatment during the Diabetes Control and Complications Trial (DCCT) on peripheral neuropathy in type 1 diabetes during the Epidemiology of Diabetes Interventions and Complications (EDIC) study. Diabetes Care. 2010;33(5):1090-1096.
21. Callaghan BC, Little AA, Feldman EL, Hughes RA. Enhanced glucose control for preventing and treating diabetic neuropathy. Cochrane Database Syst Rev. 2012;6:CD007543.
22. Oyibo SO, Prasad YD, Jackson NJ, et al. The relationship between blood glucose excursions and painful diabetic peripheral neuropathy: a pilot study. Diabet Med J Br Diabet Assoc. 2002;19(10):870-873.
23. Bril V, England J, Franklin GM, et al. Evidence-based guideline: treatment of painful diabetic neuropathy; report of the American Academy of Neurology, the American Association of Neuromuscular and Electrodiagnostic Medicine, and the American Academy of Physical Medicine and Rehabilitation. Neurology. 2011;76(20):1758-1765.
24. Dworkin RH, O’Connor AB, Audette J, et al. Recommendations for the pharmacological management of neuropathic pain: an overview and literature update. Mayo Clin Proc. 2010;85(3 suppl):S3-S14.
25. Saarto T, Wiffen PJ. Antidepressants for neuropathic pain. Cochrane Database Syst Rev. 2007;(4):CD005454.
26. Tandan R, Lewis GA, Krusinski PB, et al. Topical capsaicin in painful diabetic neuropathy: controlled study with long-term follow-up. Diabetes Care. 1992;15(1):8-14.
27. Biesbroeck R, Bril V, Hollander P, et al. A double-blind comparison of topical capsaicin and oral amitriptyline in painful diabetic neuropathy. Adv Ther. 1995;12(2):111-120.
28. Zhang WY, Wan Po A. The effectiveness of topically applied capsaicin. A meta-analysis. Eur J Clin Pharmacol. 1994;46(6):517-522.
29. American Diabetes Association. Foot care. www.diabetes.org/living-with-diabetes/complications/foot-complications/foot-care.html. Accessed February 1, 2016.
30. Balducci S, Iacobellis G, Parisi L, et al. Exercise training can modify the natural history of diabetic peripheral neuropathy. J Diabetes Complications. 2006;20(4):216-223.
31. Yoo M, D’Silva LJ, Martin K, et al. Pilot study of exercise therapy on painful diabetic peripheral neuropathy. Pain Med. 2015;16(8):1482-1489.
32. Kluding PM, Pasnoor M, Singh R, et al. The effect of exercise on neuropathic symptoms, nerve function, and cutaneous innervation in people with diabetic peripheral neuropathy. J Diabetes Complications. 2012;26(5):424-429.
To comment on this article, contact rdavidson@uspharmacist.com.





