US Pharm. 2014;39(7):35-38.
ABSTRACT: Diabetic neuropathy is one of the most common long-term complications of diabetes mellitus, affecting up to 50% of patients. Because hyperglycemia is one of the major risk factors associated with the development and progression of diabetic peripheral neuropathy (DPN), strict glycemic control is imperative. Controlling pain in patients with DPN can greatly improve their quality of life. Antidepressants and anticonvulsants are the medications most commonly used to treat DPN. Duloxetine and pregabalin are the only agents currently FDA-approved and indicated for pain associated with DPN. Pharmacists can educate patients on the essentials of good foot care, as well as discuss the importance of frequent foot examinations, proper glucose control, and smoking cessation.
|
Diabetes mellitus is associated with significant morbidity and mortality, primarily owing to the development of chronic complications affecting major organ systems. Vascular complications are divided into microvascular (retinopathy, neuropathy, and nephropathy) and macrovascular complications (coronary heart disease, peripheral vascular disease, and cerebrovascular disease). The risk of complications increases with the duration and degree of hyperglycemia. Patients with type 2 diabetes mellitus (DM2) are often asymptomatic for a prolonged period before being diagnosed; therefore, many patients will have complications upon diagnosis. |
DIABETIC NEUROPATHY
Diabetic neuropathy is one of the most common long-term complications of diabetes, affecting up to 50% of patients. This condition is defined as the presence of symptoms and/or signs of peripheral nerve dysfunction in an individual with diabetes after other causes have been excluded.1 Diabetic neuropathy can be classified as autonomic, proximal, focal, or peripheral. Autonomic neuropathy results in changes in digestion, bowel and bladder function, sexual response, and perspiration. Proximal neuropathy causes pain in the thighs, hips, or buttocks. Focal neuropathy, which causes sudden weakness of one or more nerves, can result in muscle weakness or pain. Peripheral neuropathy, the most common type, causes pain or loss of feeling in the feet, toes, legs, hands, and arms.2
DIABETIC PERIPHERAL NEUROPATHY
Diabetic peripheral neuropathy (DPN) is present in up to 10% of DM2 patients upon initial diagnosis. Up to 50% of patients with chronic DPN may be asymptomatic; however, 10% to 20% may experience symptoms bothersome enough to require therapeutic intervention.3 Peripheral neuropathy, also referred to as sensorimotor neuropathy, usually affects the legs and feet before the arms and hands. Often, the first clinical manifestation is numbness, tingling, or pain in the feet. Insensitivity to pain or temperature, a burning or prickling sensation, loss of balance and coordination, and extreme sensitivity to even a light touch also may occur.2
Hyperglycemia is one of the major risk factors associated with the development and progression of DPN. Other risk factors include hyperlipidemia, hypertension, cigarette smoking, alcohol consumption, and increased BMI.1,2 Therefore, it is imperative that blood glucose (BG) be monitored and managed appropriately to prevent the development of DPN and its consequences.
CLINICAL MANAGEMENT
Glucose Control
The Diabetes Control and Complications Trial (DCCT) was a multicenter clinical study that enrolled 1,441 type 1 diabetes mellitus (DM1) patients between 1983 and 1989.4 Patients were randomly assigned to either intensive or conventional diabetes management. Conventional therapy consisted of one or two daily injections of insulin, including mixed intermediate and rapid-acting insulins, daily self-monitoring of urine or BG, and education about diet and exercise. Goals of therapy included absence of symptoms attributable to glycosuria or hyperglycemia; absence of ketonuria; maintenance of normal growth, development, and ideal body weight; and freedom from severe or frequent hypoglycemia. Intensive therapy involved administration of insulin three or more times daily by injection or an external pump, with goals of preprandial BG between 70 and 120 mg/ dL, postprandial concentrations <180 mg/ dL, a weekly 3 am measurement >65 mg/ dL, and monthly hemoglobin A1C <6%.4
Microvascular complications, including the development and progression of DPN, were assessed. The DCCT showed a 60% reduction in neuropathy in patients receiving intensive therapy. The observational follow-up study, Epidemiology of Diabetes Interventions and Complications (EDIC), also demonstrated a significantly lower incidence of DPN in the intensive-therapy group at EDIC year 13/14.4
The United Kingdom Prospective Diabetes Study (UKPDS) randomized >5,000 newly diagnosed DM2 patients to intensive management or conventional therapy. Conventional therapy consisted of initial diet therapy followed by pharmacologic intervention, with the goal of keeping patients asymptomatic with fasting plasma glucose levels <270 mg/ dL. Intensive therapy targeted goal fasting BG levels of <108 mg/ dL with a sulfonylurea, metformin, and/or insulin treatment.5 The UKPDS found that for each percentage point the A1C decreased, there was a 25% reduction in microvascular complications.6
The findings of these studies support the notion that chronic hyperglycemia plays a role in DPN development and that strict glycemic control can slow the progression and decrease the incidence of DPN. Observational studies also suggest that avoidance of BG fluctuations can improve neuropathic symptoms.7
Pharmacists can provide patient education concerning self-monitoring BG and the importance of keeping BG in target range. Being aware of the factors that raise or lower BG is key when interpreting BG results and making medication changes and lifestyle modifications. Patient education on proper use of BG meters also plays a role in better diabetes management and prevention of complications.
Pain Management
Controlling pain in patients with DPN can greatly improve quality of life. Antidepressants and anticonvulsants are the medications most commonly used in the treatment of DPN. Currently, duloxetine and pregabalin are the only agents FDA-approved and indicated for DPN-associated pain.8 See TABLE 1 for a list of commonly used medications and recommended dosages.9-11
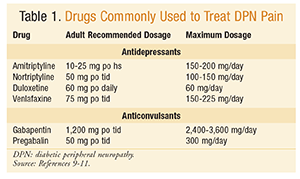
Antidepressants: Low-dose tricyclic antidepressants (TCAs) are recommended as first-line therapy for painful DPN; however, they should be used with caution because of the high incidence of adverse effects (AEs), particularly cardiac and anticholinergic AEs.12 The serotonin-norepinephrine reuptake inhibitors duloxetine and venlafaxine are better tolerated and have fewer drug interactions. There is limited evidence of the efficacy of selective serotonin reuptake inhibitors in treating neuropathic pain.8,12,13
Anticonvulsants: Gabapentin and pregabalin may be used as first-line treatment if there are contraindications or TCA treatment has failed. Pregabalin is well tolerated and causes less sedation than does gabapentin. For both drugs, dosage adjustments should be considered in patients with renal insufficiency. Pregabalin should be avoided in patients with hypertension or heart failure.9,13-15
Topicals : Topical preparations are good options for patients who cannot tolerate oral agents because of their AEs or drug interactions. Lidocaine and capsaicin are among the preferred agents for pain associated with DPN.13
RISK OF FALLS
The normal aging process is associated with an increased risk of falls and fall-related injury. In older adults, the risk increases if they also have DM2 and show evidence of at least mild-to-moderate neuropathy.16,17 Physiologically, older patients undergo age-related changes such as loss of lower-limb muscle strength and alterations in muscle function.16-18 Such patients who also have DPN suffer from confounding factors, such as muscle weakness, that put them at increased risk.19
PREVENTION
Comprehensive Foot Examination
All patients should be screened for DPN starting at diagnosis of DM2 or 5 years after diagnosis of DM1, and annually thereafter.7 An annual comprehensive foot examination by a podiatrist should be recommended. Patients with DPN should have a visual foot inspection at every visit with a healthcare professional. If abnormalities are present, more frequent evaluations are recommended.
There are four key components to a comprehensive foot examination: dermatologic, musculoskeletal, neurologic, and vascular assessment.20 Dermatologic assessment includes a global inspection for the presence of ulceration, areas of abnormal erythema, calluses or blisters, or any change in temperature. In the musculoskeletal assessment, the clinician looks for deformities.20
The neurologic assessment identifies loss of protective sensation (LOPS), rather than early neuropathy. There are five tests that clinicians can use to identify LOPS: 10-g monofilament, 128-Hz tuning fork, pinprick sensation, ankle reflex, and vibration perception threshold (VPT). Often, the performance of two tests during the screening examination—the 10-g monofilament and one other test—is sufficient. One or more abnormal tests suggest LOPS, and two normal tests rule it out.20
The efficacy of the 10-g monofilament test in detecting sensory loss has been confirmed in many trials. The monofilament is applied to certain sites on the plantar surface of the foot, and each time the patient is asked to respond yes or no when asked if the monofilament is applied to the site. Inability to detect the pressure is associated with a loss of large-fiber nerve function.20
The tuning fork test examines vibratory sensation. It should be tested bilaterally over the tip of the great toe. In the pinprick sensation test, a disposable pin is applied with just enough pressure to deform the skin; if the patient cannot feel the pinprick, this is regarded as an abnormal test result. Absence of ankle reflexes has also been associated with an increased risk of foot ulceration.20
VPT testing is performed with a biothesiometer, which is held over the dorsal hallux. The amplitude is increased until the patient can feel the vibration. A VPT >25 V is considered abnormal and is a strong predictor of foot ulceration.20
In addition to these tests, the vascular assessment, which screens for peripheral arterial disease (PAD), should be performed. Diabetes patients who have signs and symptoms of PAD or absent pulses on foot examination should undergo ankle-brachial pressure index testing and be referred to a vascular specialist.19
Patients at risk for developing DPN should understand the significance of the loss of protective sensation and the importance of appropriate footwear, as well as proper foot care (e.g., nail and skin care) and general inspection of the feet on a daily basis. Patients with evidence of plantar pressure, such as erythema, warmth, or calluses, should wear footwear that cushions and redistributes pressure. Patients with bony deformities may need extra-wide shoes, and those with severe bony deformities (Charcot foot) may need custom-molded shoes. Patients should be advised to break in new shoes gradually to avoid blisters.21
Proper Foot Care
Pharmacists can educate patients about the essentials of good foot care, as well as the importance of frequent foot examinations. It is recommended that all patients examine their feet daily for open sores, blisters, and changes in the shape and color of the skin. If they cannot see the soles of their feet, they should use a mirror or ask someone for help. In addition, it is recommended that patients wash their feet daily with warm soap and water and dry them thoroughly with a soft cloth (including between the toes). A thin coat of lotion may be rubbed on the feet to keep the skin soft and smooth and to prevent them from getting dry and cracked; however, lotion should be avoided between the toes.22
Patients should be instructed to wear shoes and socks at all possible times and to refrain from walking barefoot. Comfortable shoes that protect the feet should be worn, and patients should check inside the shoes for stones, buttons, or other loose items that are potentially harmful. Patients should be advised to avoid exposure to hot water and hot pavements. Heating pads and electric blankets should never be used on the feet, as patients may not sense the heat and their feet could get burned.22 Patients should be instructed to put their feet up when sitting, not to sit with legs crossed for a long period, and to wiggle the toes and move the ankles up and down to improve circulation to the feet. See TABLE 2 for a quick guide to prevention for patients.22

Exercise
Moderate-intensity walking may not lead to an increased risk of foot ulceration in patients with DPN. In fact, 150 minutes of moderate exercise per week was reported to improve outcomes in patients with milder forms of neuropathy.7 The presence of DPN may restrict the type of activities patients can perform, but it should not prohibit them from physical activity altogether. Studies have suggested that low-intensity exercise interventions and/or balance or strength training in older adults with diabetes result in a reduction in fall risk by improving balance and lower-limb strength.23,24
Therefore, an exercise program geared toward improving strength, balance, and gait should be recommended to patients with DPN. Improving muscle strength and balance may help patients, especially older ones, more successfully carry out daily activities (e.g., climbing stairs or carrying groceries). Patients should be encouraged to incorporate strength training into their daily routine (e.g., lifting light weights while watching television), since most patients with DPN have a limited sense of balance.19 Patients must be mindful that increased exercise confers the risk of hypoglycemia; accordingly, they should monitor their BG levels and be aware of the signs and symptoms of hypoglycemia and how to treat it.
Smoking Cessation
Cigarette smoking is a risk factor not only for DPN, but also for vascular disease. For these reasons, diabetes patients who smoke should be counseled to quit smoking in order to reduce the risk of these complications.
CONCLUSION
Pharmacists can play a pivotal role in decreasing the risk factors associated with development of DPN. Besides providing education on proper glucose control and foot care, pharmacists can also counsel patients about lifestyle changes such as exercise and smoking cessation. Pharmacists can provide medication therapy management as well as patient education to help control hypertension and hyperlipidemia, which are also risk factors.
REFERENCES
1.
Boulton AJ,
Vinik AI, Arezzo JC, et al. Diabetic neuropathies: a statement by the American Diabetes Association. Diabetes Care. 2005;28:956-962.
2. National Diabetes Information Clearinghouse. Diabetic neuropathies: the nerve damage of diabetes. http://diabetes.niddk.nih.gov/dm/pubs/neuropathies. Accessed February 10, 2014.
3.
Boulton AJ. Management of diabetic peripheral neuropathy.
Clin Diabetes. 2005;23:9-15.
4. Martin CL, Albers JW, Pop-
Busui R; DCCT/EDIC Research Group. Neuropathy and related findings in the Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications study. Diabetes Care. 2014;37:31-38.
5. Turner RC. The U.K. Prospective Diabetes Study. A review. Diabetes Care. 1998;21(
suppl 3):C35-C38.
6. American Diabetes Association. Implications of the United Kingdom Prospective Diabetes Study. Diabetes Care. 2003;25(
suppl 1):S28-S32.
7. American Diabetes Association. Standards of medical care in diabetes—2014. Diabetes Care. 2014;37(
suppl 1):S14-S80.
8. Lindsay TJ, Rodgers BC,
Savath V, Hettinger K. Treating diabetic peripheral neuropathic pain. Am
Fam Physician. 2010;82:151-158.
9. Huizinga MM,
Peltier A. Painful diabetic neuropathy: a management-centered review.
Clin Diabetes. 2007;25:6-15.
10. Micromedex Healthcare Series [online database]. www.micromedexsolutions.com. Accessed February 25, 2014.
11.
Lexicomp Online [online database]. http://online.lexi.com. Accessed February 25, 2014.
12.
Saarto T,
Wiffen PJ. Antidepressants for neuropathic pain. Cochrane Database
Syst Rev. 2007;(4):CD005454.
13. Wong MC, Chung JW, Wong TK. Effects of treatments for symptoms of painful diabetic neuropathy: systematic review. BMJ. 2007;335:87-97.
14.
Wiffen PJ,
McQuay HJ, Edwards J, Moore RA. Gabapentin for acute and chronic pain. Cochrane Database
Syst Rev. 2011;(3):CD005452.
15. Freeman R,
Durso-Decruz E, Emir B. Efficacy, safety, and tolerability of
pregabalin treatment for painful diabetic peripheral neuropathy: findings from seven randomized, controlled trials across a range of doses. Diabetes Care. 2008;31:1448-1154.
16. Maurer MS,
Burcham J, Cheng H. Diabetes mellitus is associated with an increased risk of falls in elderly residents of a long-term care facility. J
Gerontol A
Biol
Sci Med Sci. 2005;60:1157-1162.
17. Patel S,
Hyer S, Tweed K, et al. Risk factors for fractures and falls in older women with type 2 diabetes mellitus.
Calcif Tissue Int. 2008;82:87-91.
18.
MacGilchrist C, Paul L, Ellis BM, et al. Lower-limb risk factors for falls in people with diabetes mellitus.
Diabet Med. 2010;27:162-168.
19.
Mensing C, ed. The Art and Science of Diabetes Self-Management Education Desk Reference. 2nd ed. Chicago, IL: American Association of Diabetes Educators; 2011:737-762.
20.
Boulton AJ, Armstrong DG, Albert SF, et al. Comprehensive foot examination and risk assessment: a report of the task force of the foot care interest group of the American Diabetes Association, with endorsement by the American Association of Clinical Endocrinologists. Diabetes Care. 2008;31:1679-1685.
21. American Diabetes Association. Preventive foot care in diabetes. Diabetes Care. 2004;27(
suppl 1):S63-S64.
22. American Diabetes Association. Foot care. www.diabetes.org/living-with-diabetes/complications/foot-complications/foot-care.html. Accessed February 15, 2014.
23. Morgan RO,
Virnig BA, Duque M, et al. Low-intensity exercise and reduction of the risk for falls among at-risk elders. J
Gerontol A
Biol
Sci Med Sci. 2004;59:1062-1067.
24. Morrison S,
Colberg SR, Mariano M, et al. Balance training reduces falls risk in older individuals with type 2 diabetes. Diabetes Care. 2010;33:748-750.
To comment on this article, contact rdavidson@uspharmacist.com.





