Asthma and chronic obstructive pulmonary disease (COPD) are common disorders associated with significant morbidity and mortality in the elderly. COPD, diagnosed in the sixth decade in most patients, continues to be underrecognized despite its status as an important chronic disease and a leading cause of disability in seniors.1 Whether asthma or COPD, a number of studies have shown that symptoms of obstructive lung disease are underreported by the elderly and under- or misdiagnosed by physicians.2
Today, the prevalence of COPD is greater in women, and since the year 2000, the mortality rate of this disease has been higher in women than in men.2 Experts estimate that worldwide, by the year 2020, COPD will rank as the third-leading cause of death and as the fifth-leading cause of disability—even though it is largely a preventable disease.1,2 Almost all patients with COPD are current or former smokers.3 The smoking epidemic of the twentieth century has greatly contributed to COPD and cardiovascular disease, both of which may cause symptoms that mimic asthma.1,4 Cardiovascular disease and cancer are considered significant comorbidities associated with COPD.
In the elderly, symptoms and signs of airway disease can be nonspecific; further, they may overlap with other common disorders in this population.2 The classic symptoms of asthma and COPD, including dyspnea (shortness of breath), wheezing, and cough are indistinct in the elderly and may be attributed to other conditions such as gastroesophageal reflux disease (GERD), chronic aspiration, congestive heart failure, and upper airway obstruction. For example, coughing may be the only symptom in some patients with asthma (cough-variant asthma),5 and may be totally overlooked or underreported by patients and under- or misdiagnosed by physicians.
Further, dyspnea and reduced functional ability are frequently attributed to the aging process by both patients and health care practitioners, resulting in a delayed or missed opportunity for diagnosis in seniors. Due to the higher prevalence of comorbidity in the elderly, the differential diagnosis of asthma and COPD in older adults is often more difficult than in younger adults.4
Asthma and COPD in the Elderly
The Global Initiative for Chronic Obstructive Lung Disease (GOLD) has defined COPD as a partially reversible or nonreversible airway limitation that is progressive and cannot be reversed by current therapies; asthma, by contrast, is defined as a syndrome characterized by reversible airflow limitation (see Resources for classification of asthma control and recommended action).6,7 While there are prominent differences between COPD and asthma in older adults (Table 1), they may become indistinct clinically in some elderly individuals.2


COPD is considered a systemic disease associated with extrapulmonary manifestations, including muscle wasting and systemic inflammatory response.2 It is important in the management of both disorders, however, to recognize the role of inflammation in the pathogenesis of asthma and COPD.2
Of note, although the incidence of upper airway obstruction in the elderly is unknown, it can mimic asthma and COPD; therefore, special vigilance is necessary to diagnose upper airway obstruction in this patient population.2 Typical causes of upper airway obstruction include infection, malignancy, trauma, extrinsic compression (e.g., enlarged or pathologic adjacent structures) and benign strictures secondary to airway interventions, which are becoming more prevalent.2
Objective Pulmonary Function Tests: Spirometry
The difficulty of differential diagnosis of asthma and COPD supports the value of objective measurement of lung function in the elderly. Asthma is suspected largely on a person’s report of characteristic symptoms; the diagnosis is confirmed by doing pulmonary function tests.5 The initial (and least expensive) pulmonary function test is spirometry, particularly if the patient is experiencing dyspnea and wheezing.
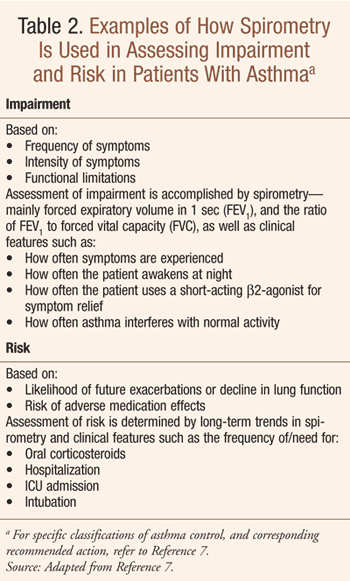
Spirometry should be conducted prior to and after inhalation of a short-acting bronchodilator; flow-volume loops are reviewed to diagnose vocal cord dysfunction (typically a cause of upper airway obstruction that mimics asthma).7 In patients with asthma, spirometry should be repeated at least every 1 to 2 years to monitor disease progression.7 Spirometry can help in the assessment of impairment from airway obstruction, assessment of risk for likelihood of future exacerbations or decline in lung function; it can also be helpful in assessment of risk of adverse medication effects (Table 2) and in monitoring effectiveness of treatment.5 In patients suspected of having asthma who have normal findings on spirometry and flow-volume testing, inhaled methacholine (or alternatives, such as inhaled histamine, adenosine, or bradykinin, or exercise testing) is used to provoke bronchoconstriction; this test is also used for patients suspected of having cough-variant asthma, as long as there are no contraindications.7
Spirometry should also be performed when COPD is suspected.1 Earlier diagnosis could markedly reduce morbidity and improve quality of life.8 Decrease in the forced expiratory volume in 1 second (FEV1) and the ratio of the FEV1 to the forced vital capacity (FVC) are required to demonstrate airflow obstruction and to make the diagnosis.9 A series of tests, comprising a full pulmonary function test (FEV1, FVC, lung volumes, and diffusion capacity), may be performed in selected patients.1 It may also be helpful to use additional tests and tools in the differential diagnosis, including questionnaires specifically developed to discriminate between COPD and asthma and, in special cases, imaging studies.8
According to Price et al, key areas for improvement in the differential diagnosis of COPD include enhanced case identification, improved quality and interpretation of findings on spirometry, and increased use of tools, such as differential diagnosis questionnaires and algorithms, to guide the diagnostic and monitoring process.8 For an algorithm outlining the role of pulmonary function tests in making a differential diagnosis of asthma versus COPD in a patient with chronic or intermittent dyspnea, refer to Reference 4. Price et al note that to achieve optimal outcomes, the primary care team should make every effort to establish a firm diagnosis. For a comprehensive overview of pulmonary function testing, including spirometry, refer to References 7 and 9, available online. For a patient-friendly explanation that may be used in patient counseling, refer to Reference 5, also available online.
Concerns Regarding Pharmacologic Therapy
Medication Delivery: In the elderly, it should be recognized that poor inhaler technique is common.2 One small study conducted by Allen et al assessed the metered-dose inhaler (MDI) technique of 30 elderly patients (mean age 79.9 years).10 The researchers found that while 60% of participants were classified as competent, a mere 10% had an ideal technique; 40% of participants were classified as incompetent. The most frequent error made was inadequate timing of actuation and inhalation.10 The study indicated competence was significantly related to mental status; competence was not related to age, underlying diagnosis, or duration of MDI therapy.10 The researchers recommend that elderly patients requiring MDI therapy should be carefully selected and properly instructed by the prescribing physician. Patients were significantly more likely to be competent if they were first prescribed an MDI in a hospital, rather than prescribed an MDI by a general practitioner.10
Appropriate inhalation technique is essential to achieve optimal drug delivery and therapeutic effect of aerosol inhalant medications.11,12 Educating patients on the role and proper use of inhaled medications while determining which patients would benefit from the use of simple spacers or valved holding chambers is encouraged by evidence-based guidelines for disease management.13 Clinicians, at every opportunity, should re-educate the patient about their tailored and evolving pharmaceutical care plan and encourage patients to become active participants in their own care (see Resources for educational counseling opportunities).13
Medication Effectiveness: Pharmacodynamic and pharmacokinetic differences, as compared with younger patients, may cause a diminished response to b2-agonists, while comorbidities, such as cardiovascular disease, may increase the risk for medication adverse effects.2
Medication Adherence: Factors leading to poor adherence to recommendations and inadequate response include: 1) complex medication regimens, 2) prohibitive cost, 3) cognitive impairment, and 4) poor medication delivery technique.2
Medication Safety: Ongoing monitoring should address increased risk from comorbidities and drug–drug interactions.2 For example, a recent population-based study by Stephenson et al observed senior men and women aged 66 years and older with COPD.14 The researchers found that men who initiated therapy with an inhaled anticholinergic were at increased risk of acute urinary retention; men with benign prostatic hyperplasia were at even higher risk, as were men taking both short- and long-acting inhaled anticholinergics.14
Conclusion
In the elderly, asthma and COPD are common and are associated with significant morbidity and mortality. The differential diagnosis of asthma and COPD in older adults is often more difficult than in younger adults. Objective measurement of lung function in these individuals is of value in striving for earlier diagnosis that could considerably reduce morbidity and improve quality of life.
REFERENCES
1. Yende S, Newman AB, Sin D. Chronic obstructive pulmonary disease. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:987-1001.
2. Braman SS, Abu-Hijleh M. Asthma and chronic obstructive pulmonary disease. In: Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. Philadelphia, PA: Saunders Elsevier; 2010:362-375.
3. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Health & Aging. Whitehouse Station, NJ: Merck Research Laboratories; 2004:725-734.
4. Enright PL. Aging of the respiratory system. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:983-986
5. Asthma. The Merck Manual Home Edition for Patients and Caregivers. Merck Sharp & Dohme Corp., Whitehouse Station, NJ. Revised April 2008.
www.merckmanuals.com/home/
6. Global strategy for diagnosis, management, and prevention of COPD. Updated 2010. Global Initiative for Chronic Obstructive Lung Disease (GOLD).
www.goldcopd.org/Guidelines/
guidelines-resources.html. Accessed June 16, 2011.
7. Asthma. In: Porter RS, Kaplan JL, eds. The Merck Manual Online. Merck Sharp & Dohme Corp., Whitehouse Station, NJ. 2004-2010.
www.merckmanuals.com/
8. Price DB, Yawn BP, Jones RCM, et al. Improving the differential diagnosis of chronic obstructive pulmonary disease in primary care. Mayo Clin Proc. 2010;85:1122-1129.
9. Chronic obstructive pulmonary disease. The Merck Manual Online. Merck Sharp & Dohme Corp., Whitehouse Station, NJ. Revised April 2007.
www.merckmanuals.com/home/
10. Allen SC, Prior A. What determines whether an elderly patient can use a metered dose inhaler correctly? Br J Dis Chest. 1986;80:45-49.
11. Kelly HW, Sorkness CA. Asthma. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 6th ed. New York, NY: McGraw-Hill Inc; 2005:503-535.
12. Expert Panel Report 3 (EPR3): Guidelines for the Diagnosis and Management of Asthma. National Heart, Lung and Blood Institute. National Institutes of Health.
www.nhlbi.nih.gov/guidelines/
13. Zagaria ME. Inhalant agents for asthma, bronchospasm, and COPD: Focus on delivery devices and inhalation technique. The American Journal for Nurse Practitioners. 14:21-25.
14. Stephenson A, Seitz D, Bell CM, et al. Inhaled anticholinergic drug therapy and the risk of acute urinary retention in chronic obstructive pulmonary disease. Arch Intern Med. 2011; 171:914-920.
15. How to use a metered-dose inhaler the right way. Asthma Initiative of Michigan (AIM). For Healthy Lungs. Updated September 18, 2009.
www.getasthmahelp.org/
To comment on this article, contact rdavidson@uspharmacist.com






